Category: Obesity
Survey
December 16, 2023 9:54 am
Overfed But Undernourished
October 01, 2019 11:27 am
Obesity is related to as many as 400,000 deaths each year in the US and it has increasingly been recognized as a risk factor for several nutrient deficiencies. This may seem surprising given the likelihood of over consumption of calories, however these additional calories are not from nutritious sources. One of the main reason for these nutritional deficits is the greater availability of inexpensive foods that are rich in calories and are nutrient deficient. This has led some medical professional to conclude that there is a certain group of people who are overfed but undernourished. Even with the epidemic of the obesity, there is significant nutritional deficiencies noted.
Obese subjects have increased blood volume, cardiac output, adiposity, lean mass and organ size all of which can influence volume of distribution, in addition, treatment for severe obesity involving surgical procedures can worsen these nutrient deficiencies and in some cases may cause new ones to develop.
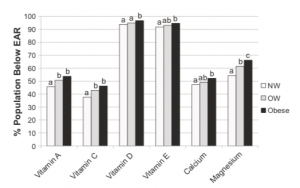
This table shows the percentage of population below the estimated average requirement (EAR) by body weight status in adults more tan 19 years old, showing that almost 90 to 100 percent of people including normal weight (NW) are below the EAR of vitamin D and Vitamin E.
 Nutritional deficiencies in obese patients may promote the development of chronic diseases including increased insulin resistance, pancreatic B-cell disfunction and diabetes, this is because specific micronutrients are involved in glucose metabolic pathways; There are other chronic diseases related to obesity that are being investigated such as decrease in focal grey matter volume and cognitive impairment or inadequate sleep due to low intake of antioxidant vitamins.
Nutritional deficiencies in obese patients may promote the development of chronic diseases including increased insulin resistance, pancreatic B-cell disfunction and diabetes, this is because specific micronutrients are involved in glucose metabolic pathways; There are other chronic diseases related to obesity that are being investigated such as decrease in focal grey matter volume and cognitive impairment or inadequate sleep due to low intake of antioxidant vitamins.
We would like to thank Miguel Rosado, MD for his significant contribution provided for this Blog.
Sleeve And Weight Regain
July 22, 2019 9:50 am
 Felsernreich et.al. demonstrated that 10 years after sleeve gastrectomy 33% were requiring revisions of their sleeve due to weight regain or reflux. 66% needed revision for weight loss and only 34% for reflux. Those patients who have revision to gastric bypass (in their practice all being revised with two exception) had resolution of their reflux however had no sustained weight loss after the revisions. This supports our position that we have had for years that the those patient who had the sleeve and are experiencing weight regain, recurrence of comorbidities inadequate weight loss ahould all be revised to the duodenal switch operation.
Felsernreich et.al. demonstrated that 10 years after sleeve gastrectomy 33% were requiring revisions of their sleeve due to weight regain or reflux. 66% needed revision for weight loss and only 34% for reflux. Those patients who have revision to gastric bypass (in their practice all being revised with two exception) had resolution of their reflux however had no sustained weight loss after the revisions. This supports our position that we have had for years that the those patient who had the sleeve and are experiencing weight regain, recurrence of comorbidities inadequate weight loss ahould all be revised to the duodenal switch operation. 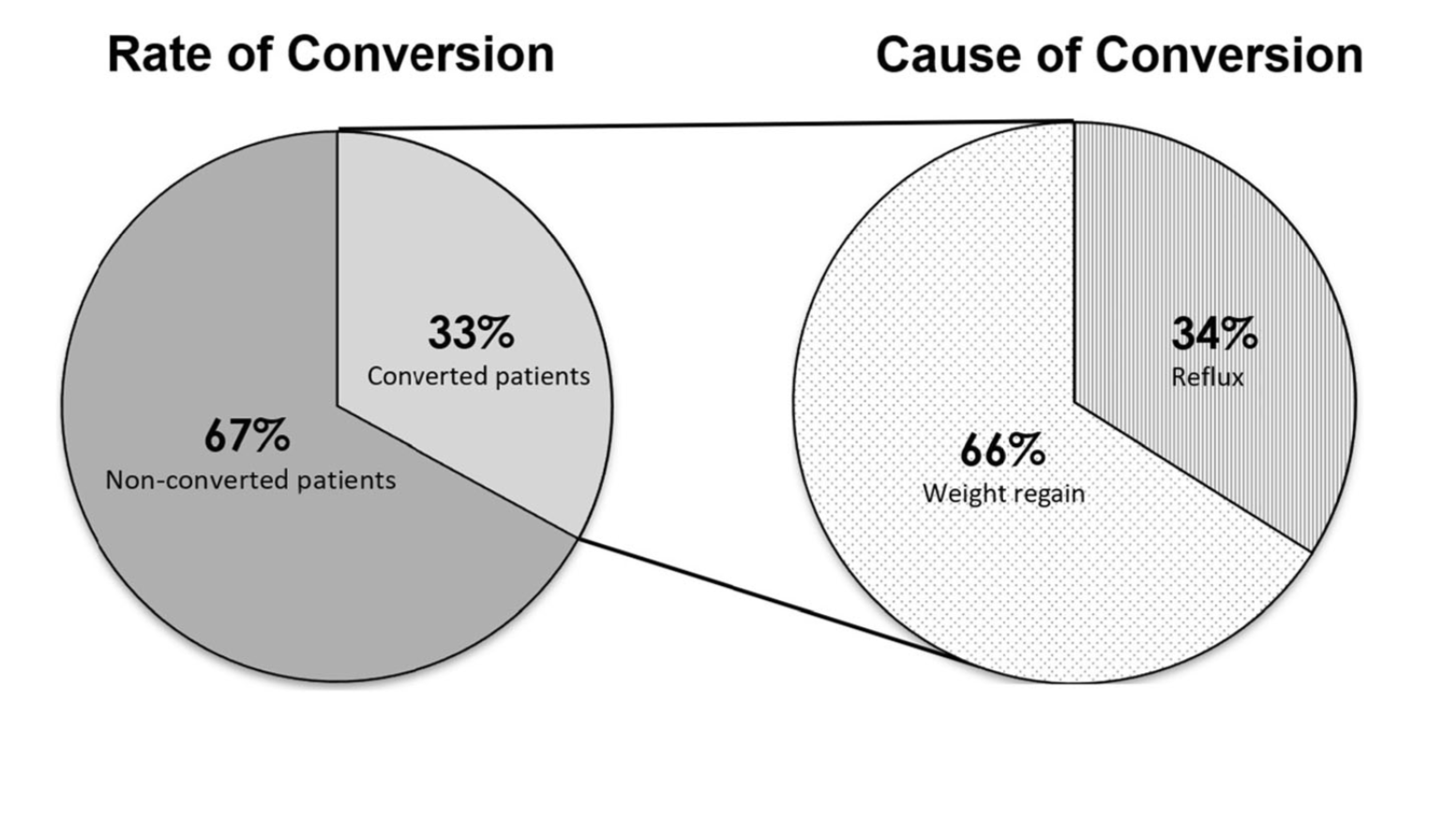
Gastroesophageal Reflux: Bile Vs. Acid
May 14, 2019 12:52 pm
Gastroesophageal (GE) reflux is the condition when the stomach content are able to “reflux” back thru an incompetent lower esophageal sphincter (LES) into the esophagus.
Gastroesophageal reflux Disease (GERD) is the clinical condition which is the result of long standing reflux and results in microscopic and visible changes to the inner lining of the esophagus, esophageal mucosa.
GERD is a non descriptive as to the cause of the condition. It only states that the content of the stomach have been irritating the lining of the esophagus on chronic bases. This can be caused by an anatomical abnormality fo the GE junction (Hiatal Hernia), or may be related to disfunction the LES. Other possible causes of the GERD may be infection (H.Pylori) environmental (stress) and dietary (nicotine, alcohol, caffeine, spicy food) in origin.
So far we have not clarified the chemical nature of the the refluxed content.
In Acid Reflux, the relative acid overproduction of acidic secretion and the exposure of the esophageal mucosa is what needs to be addressed. This is accomplished by acid suppression medications, Anti Histamine (H2 blockers) Proton pump inhibitors (PPI) for example. The physiology, and the mechanism involving this condition is well understood. As a surgeon, we do however see patients who should have had surgical intervention. The initial mode of therapy for a patient with documented acid reflux, and or symptomatic hiatal hernia is placing them on medication. These patients are then recommended to have related upper endoscopy. Patients who do not improve or where deterioration of the esophageal mucosa, presence of precancerous cells, then the patients are referred for surgical intervention.
Bile Reflux, contrary to acid reflux may have very little if anything with the LES. The symptoms experienced by the patient may be as ofter related to the excessive bile in the stomach seen frequently
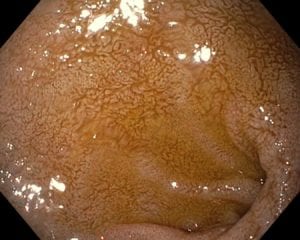
after cholecystectomy, or in those patients with dysfunctional gallbladder (low EF on HIDA scan).
The treatment of Bile reflux, is Duodenal Switch with without the associated sleeve gastrectomy component in addition to repair of hiatal hernia if present Ann Surg. 2007 Feb; 245(2): 247–253.
Sleeve Gastrectomy Failure
May 07, 2019 12:53 pm
Sleeve gastrectomy (SG) is the most commons performed weight loss surgery in the US. There is a subset of patients for which Sleeve Gastrectomy will be inefficient/ineffective. Sleeve Gastrectomy failure may be defined as inadequate weight loss or weight regain. However, in some cases this may also include non resolution of some of the co-morbidities of obesity, and/or recurrence of others.
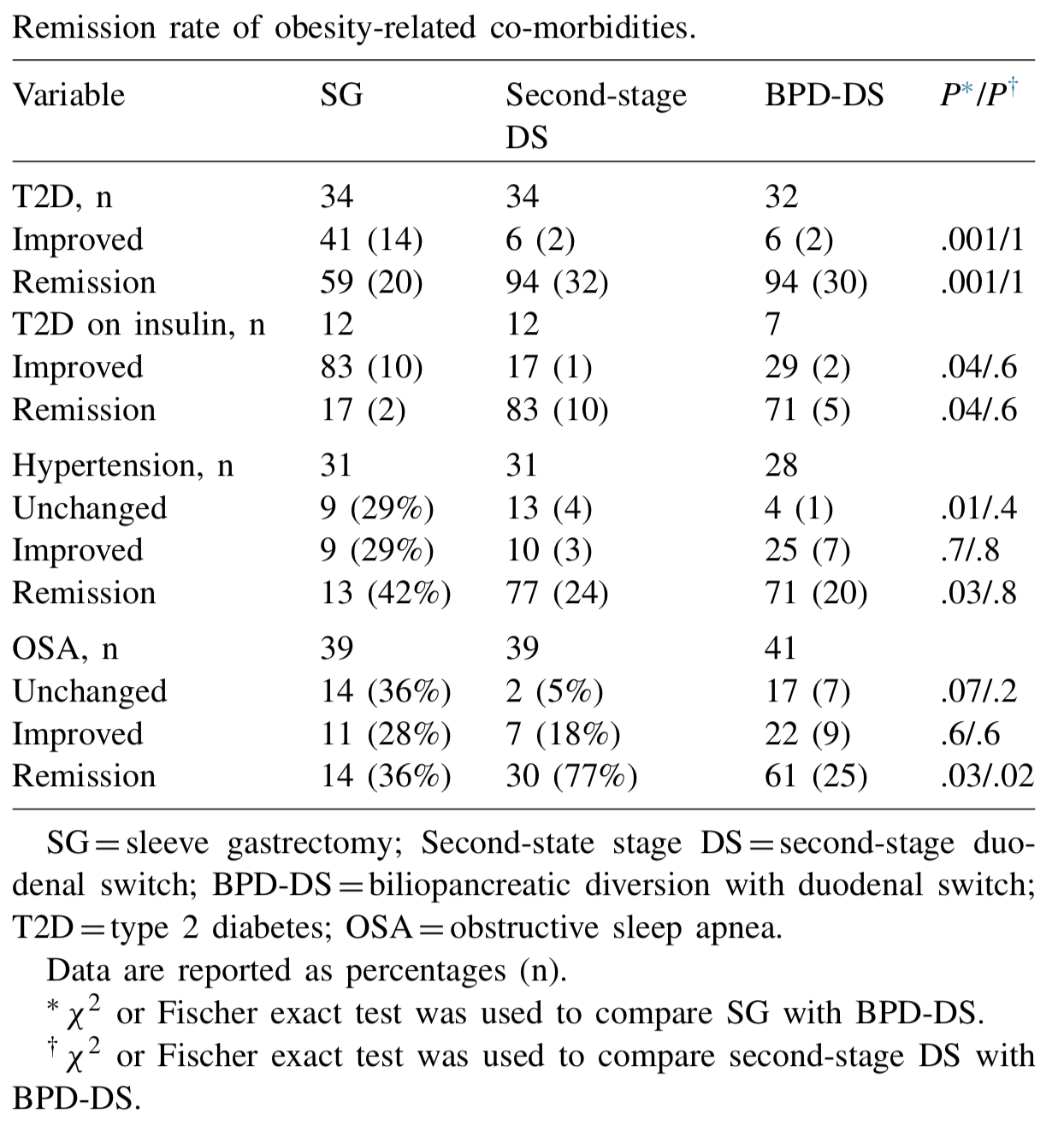
Biertho, et. al, (Surgery for Obesity and Related Diseases 14 (2018) 1570–1580) Published a study titled “Second-stage duodenal switch for sleeve gastrectomy failure: A matched controlled trial” where 118 patients were decided in two groups. One group had the duodenal switch as a singe procedure, and the second group had the sleeve gastrectomy followup by the second stage duodenal switch. They concluded that “Second-stage DS is an effective option for the management of suboptimal outcomes of SG, with an additional 41% excess weight loss and 35% remission rate for type 2 diabetes. At 3 years, the global outcomes of staged approach did not significantly differ from single-stage BPD-DS; however, longer-term outcomes are still needed.”
They showed that the remission rate of the obesity related co-morbidities were improved.
The weight loss rate that had stopped, or in some cases where weight gain had been noted, were both reversed where by at at average of 24 months after addition of the DS to the SG patients would experience additional 39% Mean excess weight loss. 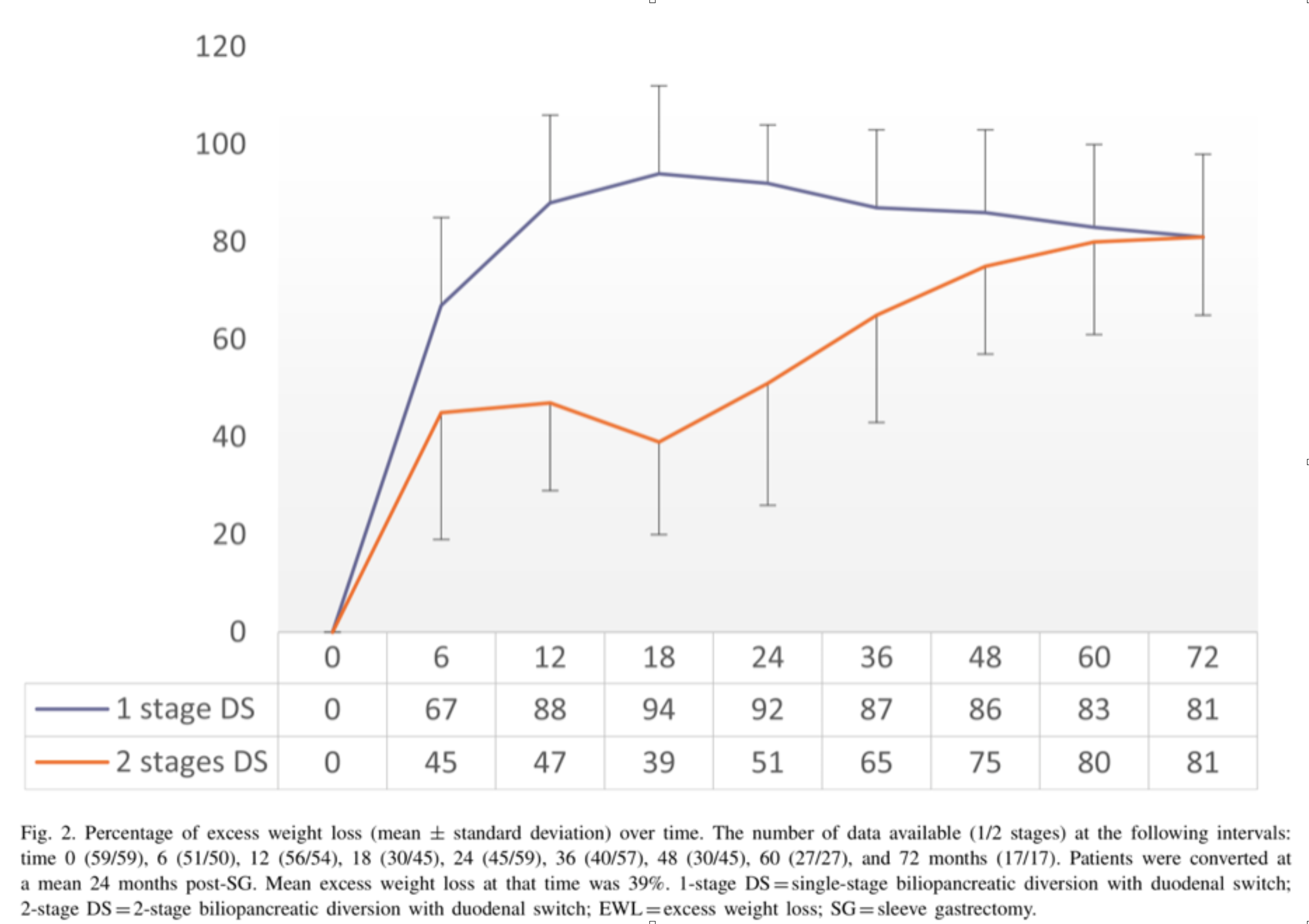
With regards to alternative approaches they indicate “ Other forms of revisions have been described, (i.e., adjustable or nonadjustable gastric band, plication, endoscopic balloon), with limited scientific evidence on their efficacy or safety. These procedures are mostly considered investigational and should be performed under Ethical Review Board approved protocols.”
In summary, patients may be offered a number of alternative if they are experiencing weight regain, inadequate weight loss, or return of co-morbidities after sleeve gastrectomy failure. We have seen a variety of them in our office. Patients who have had band placed on the sleeve, or are scheduled to have gastric balloons placed. As I have always said, buyers beware and know your outcomes and resolution of co-morbities.
Duodenal switch operation, (not the single anastomosis look alike) results in sustained weight loss and resolution of the co-morbidities. A second stage Duodenal Switch can mean adding the intestinal procedure to an existing Sleeve Gastrectomy. Some patients have required an adjustment to their Sleeve Gastrectomy in addition to adding the Duodenal Switch intestinal portion. Finding the right balance for each patient is a crucial part of our practice.
Gastric Balloon
March 12, 2019 9:10 am
Here we go again…. There is a new cure for obesity, Gastric Balloon, with minimal to no risk, is an outpatient procedure and/or can be done in the surgeons office with no anesthesia. Have we not similar claimed like this before (Adjustable gastric band) ?
Randomized sham-controlled trial of the 6-month swallowable gas-filled intragastric balloon system for weight loss published in Surgery for Obesity and Related Diseases 14 (2018) 1876–1889, by Sullivan et. al reports
“Conclusions: Treatment with lifestyle therapy and the 6-month swallowable gas-filled intragastric balloon system was safe and resulted in twice as much weight loss compared with a sham control, with high weight loss maintenance at 48 weeks.”
This sound very promising, however is very vague and leaves out significant, critical, and pertinent information.
The outcome of weight loss at 24 weeks was reported in Total Body weight loss % (TBWL%), Excess weight % (EWL), weight loss, and BMI change. Of those, the last three were statistically significant changes.
The outcome the weight loss was reported to be at 7% TBWL% at 24 weeks with some weight regain, with the patient employing post REMOVAL life style changes. 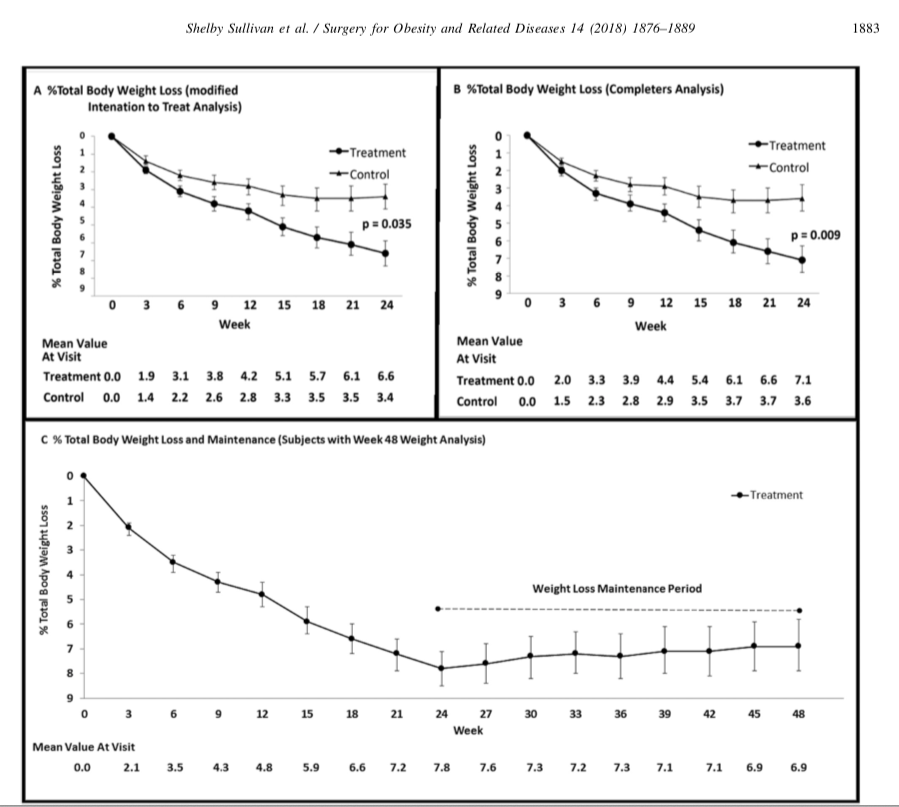
It is stated that the Gastric Balloon is temporary device that needs to be removed in 6 months and should be considered in low BMI patients (<35kg/m2). It is is important for those patients who are considering this temporary expensive measure for minimal weight loss to entertain the alternative of the same temporary results that may be obtained by lifestyle changes. These results may be maintained by a healthy lifestyle, exercise, and eating without the need for a device.
PolyCystic Ovarian Syndrome PCOS
September 04, 2018 9:58 am
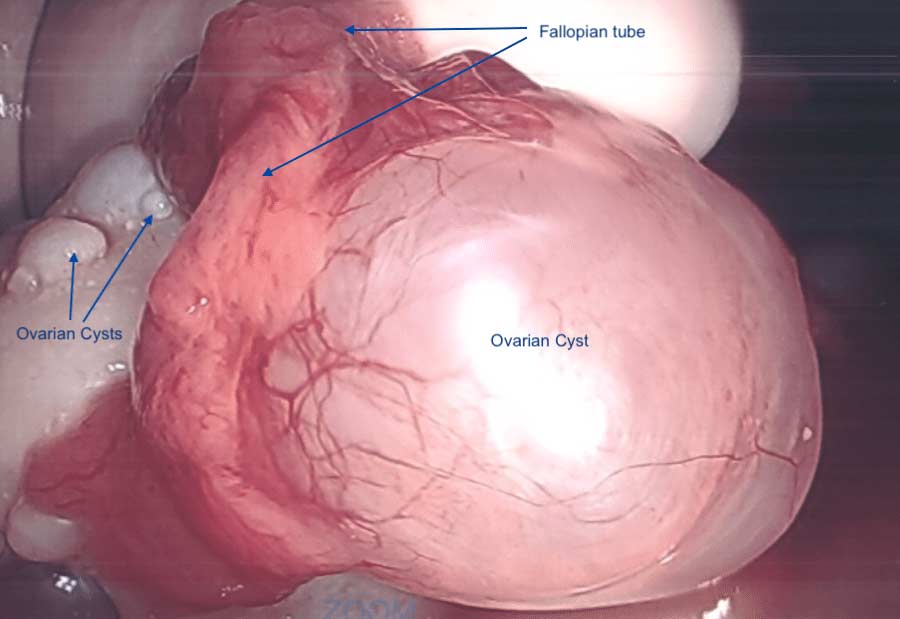
PolyCystic Ovarian Syndrome PCOS is a complex condition. The exact cause of PCOS is unknown however, it involves hormones imbalance and multiple ovarian cysts, irregular menses, and infertility. In some cases, PCOS can be compounded by diabetes, hypertension and other metabolic conditions. PCOS has been shown to effect approximately 10% of women of childbearing age with symptoms of menstrual abnormalities, poly cystic ovaries, and excess androgen (male sex hormone). PCOS should be diagnosed by ensuring there are no other underlying endocrine issues. There are several associated disease processes that seem to be related to PCOS. These related disease processes are Type 2 Diabetes, higher depression and anxiety, increased cardiovascular risks, stroke, hyperlipidemia, sleep apnea, overall inflammation, and endometrial cancer.
Anatomically, numerous cysts are found on the ovaries. These are usually diagnosed by ultrasound, blood levels of hormones, and symptoms described above.
Bariatric Surgery and PolyCystic Ovarian Syndrome PCOS
Bariatric Surgery can improve PCOS in those individuals with Type 2 Diabetes Mellitus. Further information on weight loss surgery and its effect on PCOS here.
Insurance Appeals And Denials
August 07, 2017 7:08 am
Whenever you are dealing with insurance issues it is important to have a general understanding of insurance ins and outs. The Obesity Action Coalition has a good general guide to the insurance process here. If you are having issues with out of network, out of area, or insurance appeals and denials for Duodenal Switch, there may be some additional assistance from two individuals who have had the Duodenal Switch procedure themselves. We are grateful that they have provided assistance throughout the years to the Duodenal Switch community. The following is their statement on insurance.
The majority of insurance companies are in the business of making money (for profit). They can deny requests for preauthorization with impunity. These denials are often complexly worded and difficult to comply with and overcome, and are definitely overwhelming to the patient, and the busy surgeon’s office. The vast majority of patients faced with demanding if not impossible to achieve prerequisites, or denial of the request for preauthorization simply give up, and the insurance companies pocket the savings.
If you find yourself facing impossible pre-op hurdles, or a denial, we urge you to appeal, and to seek assistance in preparing the appeal. You can hire an attorney, of course, but there is an informal and free resource we suggest that you investigate as well.
If you go to BariatricFacts.org (a non-profit, patient-run site), you will find individuals who are long-term DS postops, and patient advocates. They have been helping patients, pro bono (for free), for over 10 years. They will help you draft your appeal letters, provide supporting medical and legal documentation, and prepare draft letters of medical necessity to be reviewed and signed by your surgeon supporting your appeal. They will not represent you directly, but they will help you best represent yourself. in many cases it is necessary to exhaust all internal appeals (because the insurance companies are unlikely to overrule themselves), and then file for external review, where independent reviewers often overrule improper denials. If you join and then post on BariatricFacts.org asking for help, you will be connected with them and you can decide if you want their help.
Please note that this is just a suggestion. It is neither legal nor medical advice, nor a guaranty regarding their services, and you should always consider getting legal advice and assistance from an attorney who will represent you directly. The members at BariatricsFacts.org will help you draft your own letters, but will not be your legal or medical representatives; you will be required to do a fair amount of your own work on your appeals, and to sign them yourself.
It is suggested that before or at the same time as you contact the resources suggested at the site, you gather as much of the following information as you can:
- A copy of your Evidence of Coverage, which is the usually 100+ page insurance contract between your employer and the insurance company, which you can obtain it from your HR department. If you are self-insured, it will be available directly from your insurance company. Note: it is NOT the Summary of Benefits – it needs to be the contract itself.
- If your insurance is through an employer, you need to determine whether your plan is self-funded or fully-funded. Your rights are significantly different under the two types of plans.
- If your insurance company has a separate bariatric surgery policy, provide a copy of that, too.
- A copy of your surgeon’s request for preauthorization, which provides the ICD-10 and CPT codes submitted.
- A copy of your denial letter, including the section regarding your appeal rights.
* It is strongly recommended that you obtain a copy of your surgeon’s LOMN (letter of medical necessity) before it is submitted to your insurer or for external review, so we can assist your busy surgeon in making the strongest possible case for you.
Don’t be deterred by a denial. It is unfortunately more common than it should be, but it can often be overcome if you meet the requirements for bariatric surgery, if you get help navigating the process.
Shared Success Story- Theresa & Rodney (Duodenal Switch)
August 05, 2017 8:41 am
Life before surgery seems like a lifetime ago for both my wife and I. Being extremely overweight is not only a burden on your general health but a burden on your lifestyle in general. You have the awful label of being called obese, or morbidly obese. This is such a wonderful word that makes you feel as if you have been judged a misfit in society. We were both overweight all of our lives and had done all of the diets known on the planet throughout the years. Some worked a little some not at all and we always found ourselves back to where we were before and usually larger than that. The main focus though as we were getting older was our health. For Theresa it was very difficult. Along with being over 400 pounds she had a severe case of asthma which caused her episodes where she felt she was going to suffocate. She also had very little muscle mass which made it very difficult to get up and down from seating or lying positions. Theresa had her surgery in February of 2014 and not a moment too soon. If she had done nothing it is a good chance that she was facing a horribly short future. She also has a slight heart murmur which did not bode well for a person with her weight. She did not have diabetes thank goodness but her A1C was on the rise as was her BP. She did have sleep apnea as well and had to have a CPAP machine.
I was also severely overweight, my highest weight was nearly 400 pounds and on surgery day I was 355 pounds. I was also under the illusion that I had more control over my weight and that once Theresa had her surgery I would just be able to diet and exercise my way to a healthy weight. I was able to do this in my younger years to a certain extent and I was naive enough to think I could continue to do so. How wrong I was. I had found that no matter how much diet and exercise I did my weight would drop a bit at first but then stall and I would have to essentially starve to lose any more and of course that just makes for a bad outcome. My A1C shot up to 7.6 and this was with 1000mg of metformin a day! My BP was very high with both numbers over 100, well over. This is with a high dose of BP meds. I had a severe case of sleep apnea and could not even consider sleeping without a CPAP machine with a high pressure. I have an artificial hip that was being burdened by my 350 pound plus frame and would probably need to be replaced sooner rather than later. My future was not looking good. Dying before I was 60 seemed like a reality for me and that is not the future I was hoping for. The decision to have weight loss surgery for the both of us was tough. You of course hear the nay sayers spout what a cop out it is and it’s the easy way out! You are just weak and just simply need to not eat hamburgers, French fries and donuts. Just stick with non-fat and low calories and you will reach the promised land. What a load of BS.
Once you wrap your head around the fact that your body is wired in such a way that it will always seek a higher weight every time you lose weight, it’s time to consider the type of surgery. Everyone has heard of the Gastric bypass and that seemed to be the path at the time of Theresa’s surgery. The thing about Theresa and what I admire very much is her persistence and her ability to research to the point where a decision is spot on. She looked at all of the four possible surgeries and quickly realized that the Duodenal Switch was a no brainer. It had the greatest measure of success in the long term as well as short term. Reading about the process and talking to others who have had the surgery it became clear that it was the right choice. Finding out where to go and have the surgery was a real challenge. We were lucky to find Dr. Ara Keshishian and have the ability to travel to his location to have the surgery.
Theresa’s Stats Rodney’s Stats
Surgery Weight: 410 Surgery Weight: 355 Pounds
Total Weight Loss: 215 pounds Total Weight Loss: 170 Pounds
Surgery Type: Duodenal Switch Surgery Type: Duodenal Switch
Surgery Date: February 2014 Surgery Data: May 2016
Surgeon: Dr. Ara Keshishian Surgeon: Dr. Ara Keshishian
Life after surgery is an amazing series of challenges, changes, and a journey that transforms your life in a huge way. For Theresa, it was freedom. Freedom from the overbearing weight she was carrying that kept her from essentially moving or doing anything but staying at home. We did very little outside of the house before surgery. Only the necessities of shopping and keeping up the house on the inside and out. Even that was difficult and went by the wayside all too often. Of course eating out was easier than going to the grocery store and that made the scale just go higher. After surgery, Theresa began to lose weight and you could see day by day the changes. After the first month, you could see a dramatic change not only in her look but the fact that she was moving again! She had dropped 35 pounds in that first month and it made a huge difference. As the weight kept coming off over the next few months we began doing things we have not done before. We started to do a lot of walking and a lot more things around the house that needed to be done. Shopping became a breeze and we ate out a lot less. The dramatic change was in her health. A number of changes for the better were happening on that front. The main one and a huge relief was the asthma. It simply was no longer there. She was no longer short on breath and was simply out moving me! I could barely keep up with her. She also had a bad case of psoriasis which before surgery she could do nothing about. Since the surgery it has disappeared. It might be due to the increased in vitamins, particularly the D vitamin. Her sleep apnea went away and now she is healthy and happy. It is almost difficult to describe the changes until you see them for yourself. For Theresa it has been a life changing experience that has transformed the both of us in ways we never imagined. Theresa eats a normal diet and after 3 ½ years post op she fluctuates about 5 pounds either way. It is amazing.
For me it was not what I expected. What I mean by that is, learning to eat is a challenge. With the Duodenal Switch you are not only eating less, but what you eat is tremendously important to the success of the transformation. With the other surgeries, Lap Band, Bypass and Sleeve you do not have the degree of malabsorption. You simply eat less and you lose weight, but you are still essentially “on a diet”. With the Duodenal Switch you have to consider the malabsorption and think protein first and for most. Once you get past the first month of eating small amounts and what you can while your innards heal you need to learn what to eat and is it enough protein. You may also have to contending with the fact that you have an aversion to foods you ate before. I, for one, could not even eat cheese, and chicken. I pretty much lived on scallops, crab, shrimp and protein drinks for the first three months. Nuts were also a good source of the protein when you get to that stage. This does change and things do go back to normal as far as the taste changes, but it takes a few months. The weight in that first month pretty much peeled off. I was dropping like a pound a day. It was incredible. You think that this is going to be a breeze and you will drop it all in no time! Then that 4 week somewhat of a stall occurs. From what I can tell, everyone experiences it in one form or another. It freaks you out because you start to think about the past where you would work your butt off and either gain or drop and ounce or two. But I was lucky, my wife had gone though it two years before me so she was there to explain that it was normal. The whole “this is a journey thing”, and she was right! At the time though I was listening to the negative voice in my head from the past. That is where the support from the many groups come in. You see that pretty much everyone has the same ups and downs and then your body gives up the farm and you drop a bunch of weight in a weeks’ time. There is really a lot of science behind it. Researching and reading about this particular surgery and how it works will benefit you while you go through the process. Another important thing we face with this surgery is the necessity of Vitamins. Thank goodness for my wife and the DS groups and of course my surgeon. You will not be without knowledge if you actively join the different groups and do your research on the vitamins. I am still learning about what my body needs and am looking forward to my labs in the next month to see where I may be deficient. I have also come to realize the importance of drinking water and avoiding dehydration. I never used to drink it much before the Duodenal Switch, but since the surgery I find it aids heavily in the success if you drink it and drink a lot of it.
To conclude this has been a journey and one I wish I could have done a lot sooner in life, but it is never too late. Today Theresa and I are at weights that we are happy with and our bodies are happy with. We are more active then we have ever been before together. No more days idle in front of the television with large amounts of fast food and drinks. That is what we used to look forward too. Now we cannot wait until we go out and do something. We are not running marathons or anything but we are active and enjoy being so. We no longer have the ailments we had before surgery. Theresa’s asthma is practically nonexistent, living in the northwest with fires in the summer she may have a bout or two. Nothing even close to what she has before and a simple inhale and its gone. Both of us no longer need a CPAP! The freedom to simply lay your head on the pillow and sleep is amazing and wonderful. All of the medication we had prescribed for us are gone as well. My A1C was 5 on my last set of labs and 5.3 on the one before that. Theresa’s is the same and has been for three years. BP is normal and my hip is holding steady. Oh, and another cool thing about it is you can actually shop for clothes anywhere! Your sizes will shrink but we have found we have become quite the clothes horses since losing all this weight. It makes it fun to be able to fit into a size you haven’t seen since who knows when.
Life is always a challenge for many reasons but to remove the burden of the weight simplifies things just a bit. It is a decision we will never regret and wished we had made a long time ago. We both owe our lives firstly, to having Duodenal Switch surgery. Secondly, and most important – was in seeking out the best surgeon we could find, and that was without a doubt, Dr. Ara Keshishian. As a surgeon he is thorough, meticulous, constantly learning and keeping up on the latest research;as a person he is easy to talk to, very approachable, and genuinely cares about his patients before, during and after the surgery process. We could not imagine choosing anyone else.
Resistance Exercise BandsExclusive Member Content
July 19, 2017 12:47 pm