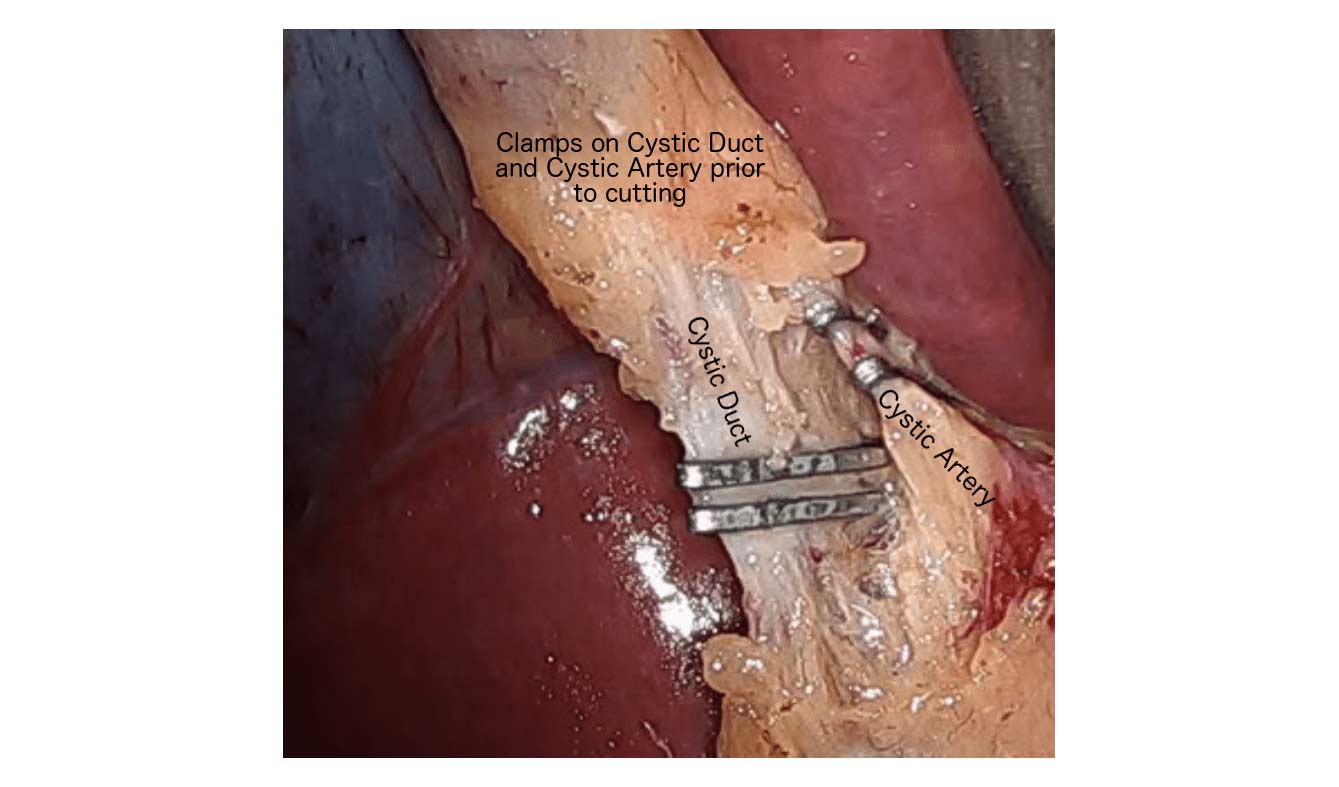
Category: Lap Sleeve Gastretomy
Survey
December 16, 2023 9:54 am
Pictures For Anesthesia
February 02, 2022 11:57 am
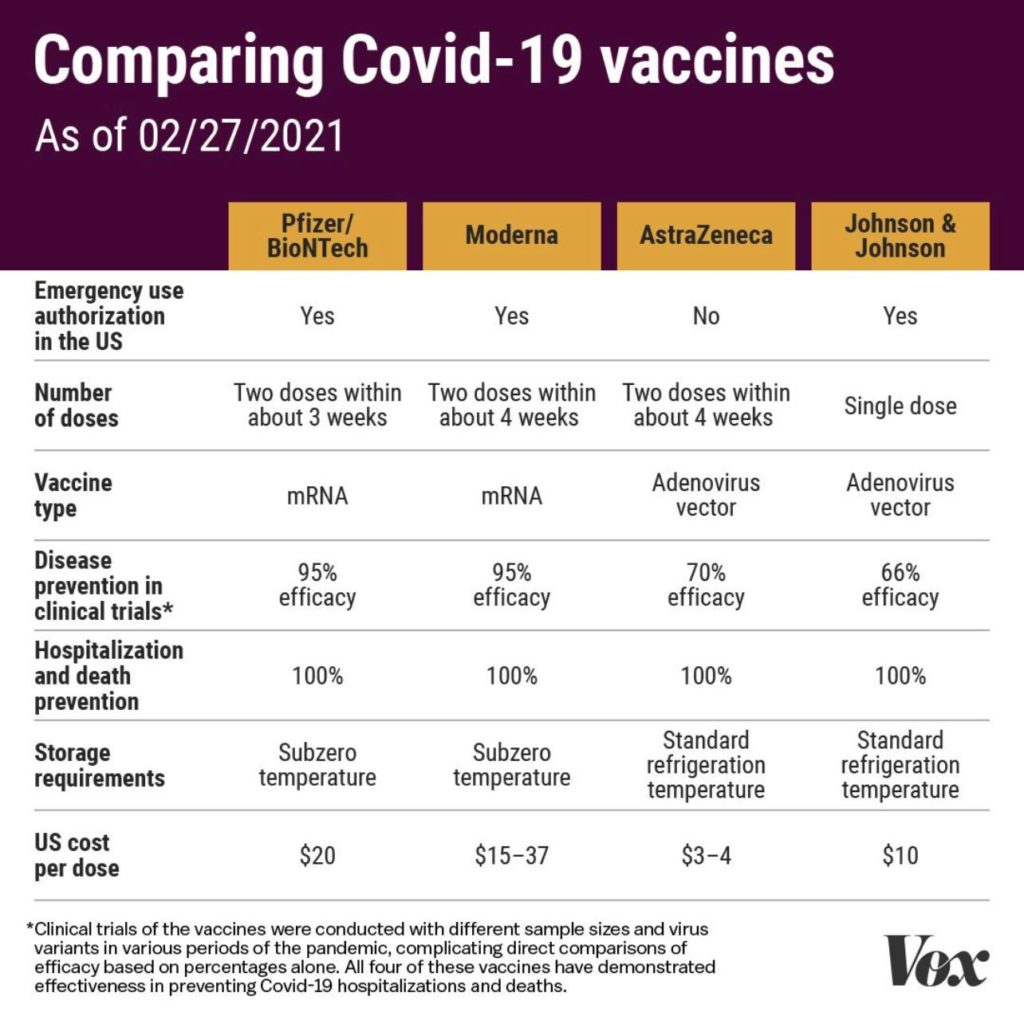
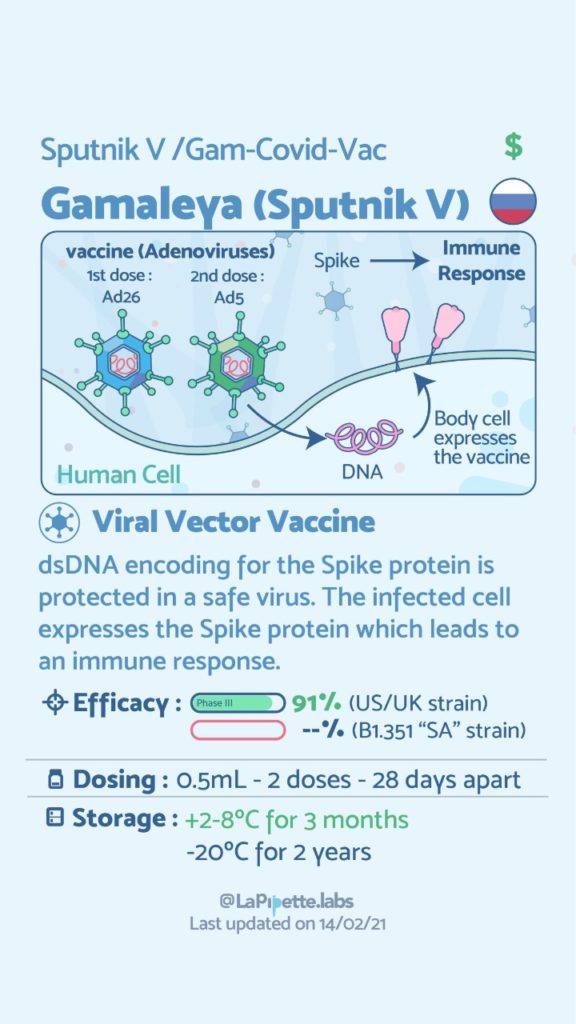
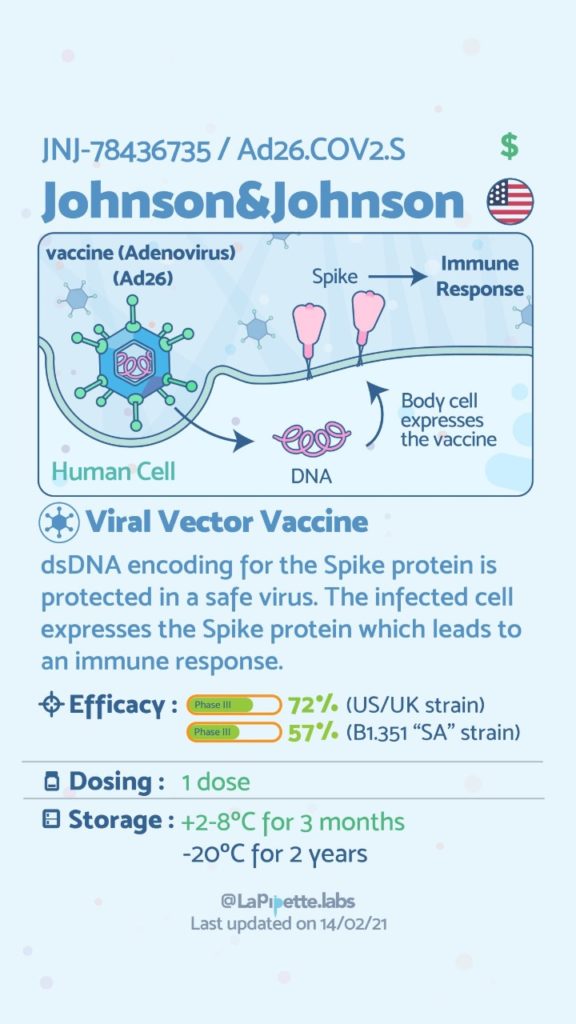
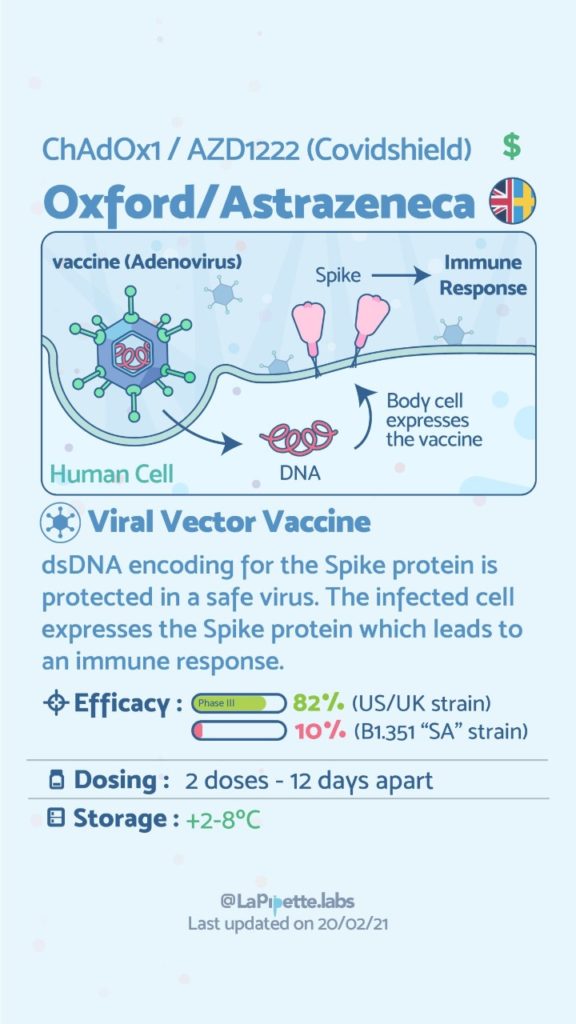
COVID Vaccines
March 05, 2021 3:50 pm
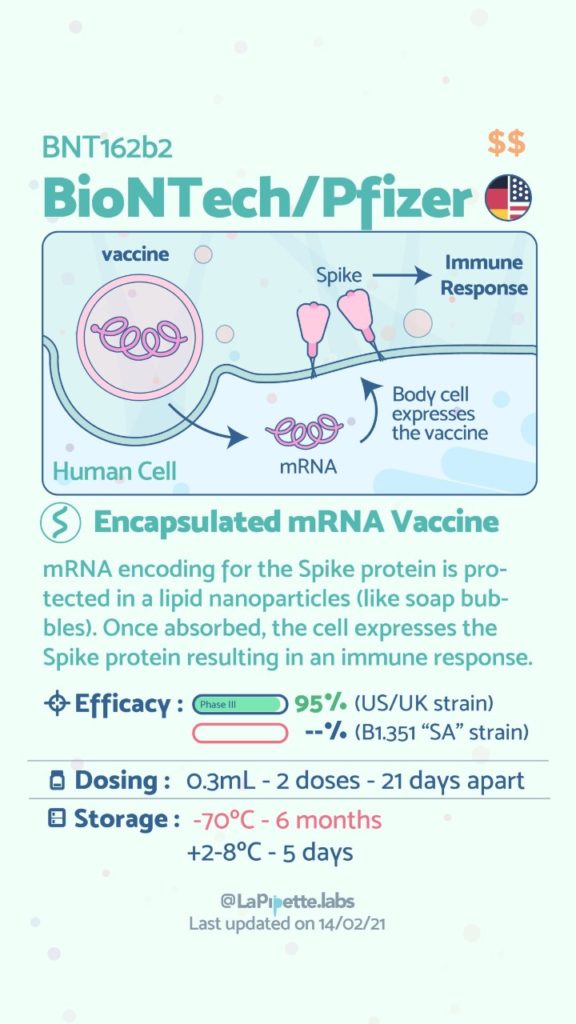
There are no known contraindications from a weight-loss surgical perspective to prevent a post-surgical patient from getting the COVID vaccines.
A patient who has had a Duodenal Switch, Lap Sleeve Gastrectomy, RNY Gastric Bypass, or revisions to Weight Loss Surgery should have the COVID vaccine. The vaccination should be avoided for a few weeks after surgery. For other possible contraindications, please consult your PCP.
Here is a summary of the vaccines and the details of each one approved as of the publication date.
Protein Intake
October 14, 2019 7:08 am
Protein intake requirements change over time following weight loss surgery. This is based on the requirements imposed on our body by a number of variables. These include, activity level, muscle mass, over all health condition to name a few.
A very young muscular athletic male with a BMI or 30 will require much higher protein intake (and absorption) that an inactive older Female with the same BMI. The same young athletic male will require much higher protein intake is he is recovering from a surgery than his baseline.
As we have stated in the past, the protein intake, should be adequate and not excessive. High level of protein intake that are not accounted for based on muscle mass and activity level, will eventually result in weight gain. The best measure of protein intake in a stable weight patient over 3-4 years post op is their albumin and protein level. Following your yearly laboratory values at a minimum is an important part of weight loss surgery follow up care.
You also need to adjust protein intake when necessary. Protein needs increase depending on physical needs, infection, healing, pregnancy, surgery, age, injury, etc. Plastic surgery requires higher protein needs for appropriate healing.
Information on protein sources and quality here.
The basic formula for protein intake is 1gm/kg of ideal body weight. The calculator below will provide a guide for the protein into based on your stable weight in lbs.
Sunscreen
June 27, 2019 3:03 am
Recently there has been some research and concern regarding sunscreen and the chemicals within them. This has led to findings that can be concerning but that need further research.
Post weight loss surgical patients, and in general patients who suffer with obesity, before or after weight loss surgery, have low vitamin D level. This may be caused by a number of factors. One such factor may be the reluctance to get skin exposed to sunlight in order for the bodies natural Vitamin D pathways functioning.
The recommendations are for daily exposure to sun. This not only is critical to the vitamin D metabolic pathways, but also help with bone health, immune function, mood, counteracting depression.
In a recently published online article, concerns were raised that some of the ingredients of some of few sunscreens are absorbed in the blood stream. This is a small study, and as the results indicates, it is not recommending to stop using the sun screens. Be aware of your sun exposure, timing exposure, and the ingredients in your sunscreen.
You can find past blog posts on Vitamin D, Bone health, etc here
Thyroid Medication Absorption And Weight Loss Surgery
June 10, 2019 8:59 am
Question : “Do I have to take higher dose of thyroid medication after the duodenal switch? ”
Answer : “Maybe”
With all weight loss surgical procedures, there may be changes to absorption of medications. It is easily understood why duodenal switch may results in decreased absorption of fat-soluble medication. What is not as clear is the reduction in absorption of other medication with procedures that do not explicitly change the absorption at the level of the small bowel directly.
The research data is all over on this topic. There is published literature that shows improvement in the thyroid function after gastric bypass and the sleeve gastrectomy. However, the exact mechanism is not completely understood.
There is research that reports “…decreased postoperative levothyroxine requirements.” Other have shows no correlation between the length of the bowel distal to duodenum to absorption of thyroid medication.
With all this confusing data, the best course would be to always “treat the patient and not the lab results.”
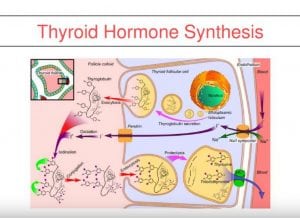 If a patients who has been on medications with stable number and symptoms, suddenly presents with complaints of hypothyroidism after weight loss surgery, it’s possible the medications should be up adjusted even if the thyroid lab values may not be as defining.
If a patients who has been on medications with stable number and symptoms, suddenly presents with complaints of hypothyroidism after weight loss surgery, it’s possible the medications should be up adjusted even if the thyroid lab values may not be as defining.
Sleeve Gastrectomy Failure
May 07, 2019 12:53 pm
Sleeve gastrectomy (SG) is the most commons performed weight loss surgery in the US. There is a subset of patients for which Sleeve Gastrectomy will be inefficient/ineffective. Sleeve Gastrectomy failure may be defined as inadequate weight loss or weight regain. However, in some cases this may also include non resolution of some of the co-morbidities of obesity, and/or recurrence of others.
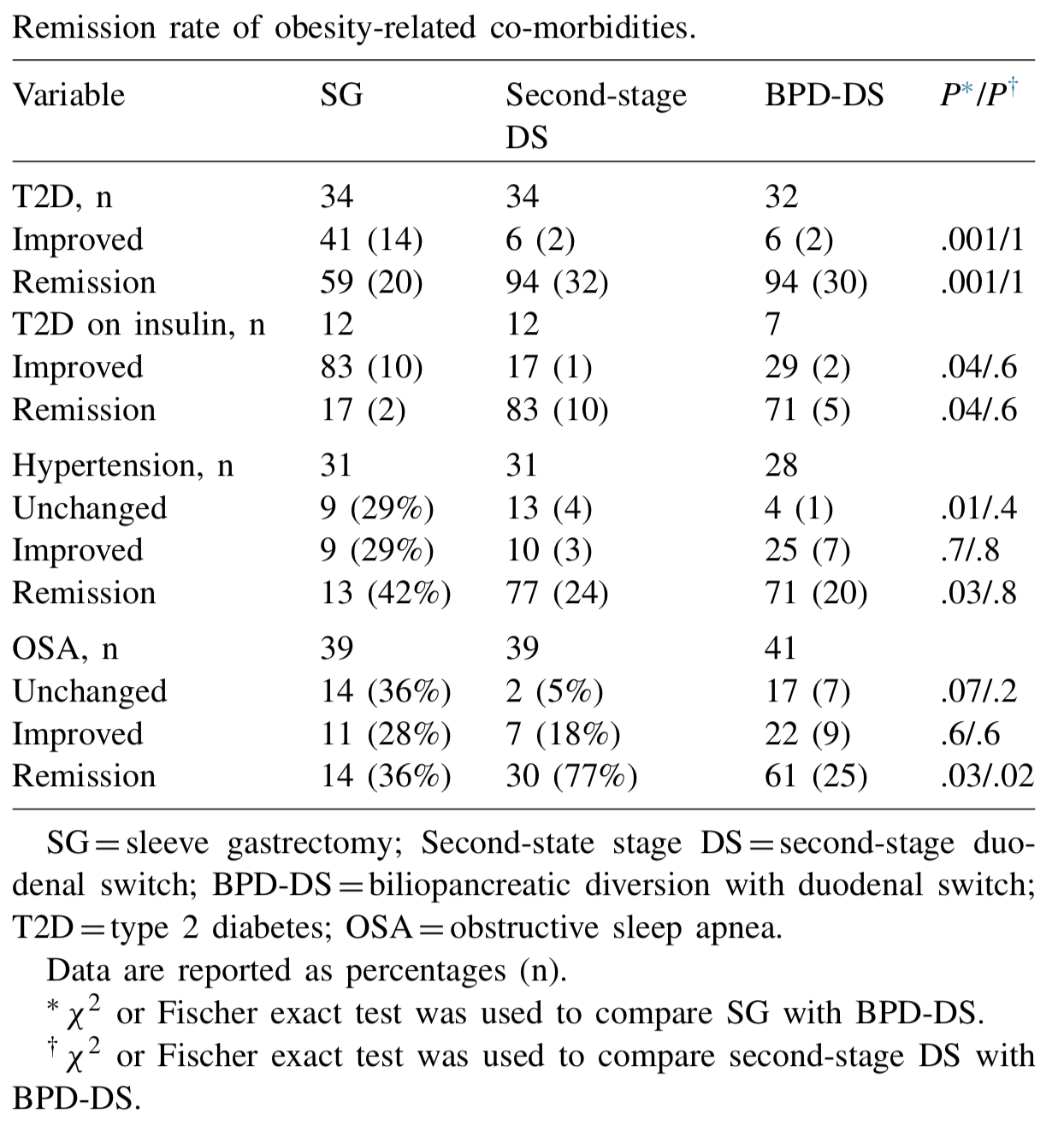
Biertho, et. al, (Surgery for Obesity and Related Diseases 14 (2018) 1570–1580) Published a study titled “Second-stage duodenal switch for sleeve gastrectomy failure: A matched controlled trial” where 118 patients were decided in two groups. One group had the duodenal switch as a singe procedure, and the second group had the sleeve gastrectomy followup by the second stage duodenal switch. They concluded that “Second-stage DS is an effective option for the management of suboptimal outcomes of SG, with an additional 41% excess weight loss and 35% remission rate for type 2 diabetes. At 3 years, the global outcomes of staged approach did not significantly differ from single-stage BPD-DS; however, longer-term outcomes are still needed.”
They showed that the remission rate of the obesity related co-morbidities were improved.
The weight loss rate that had stopped, or in some cases where weight gain had been noted, were both reversed where by at at average of 24 months after addition of the DS to the SG patients would experience additional 39% Mean excess weight loss. 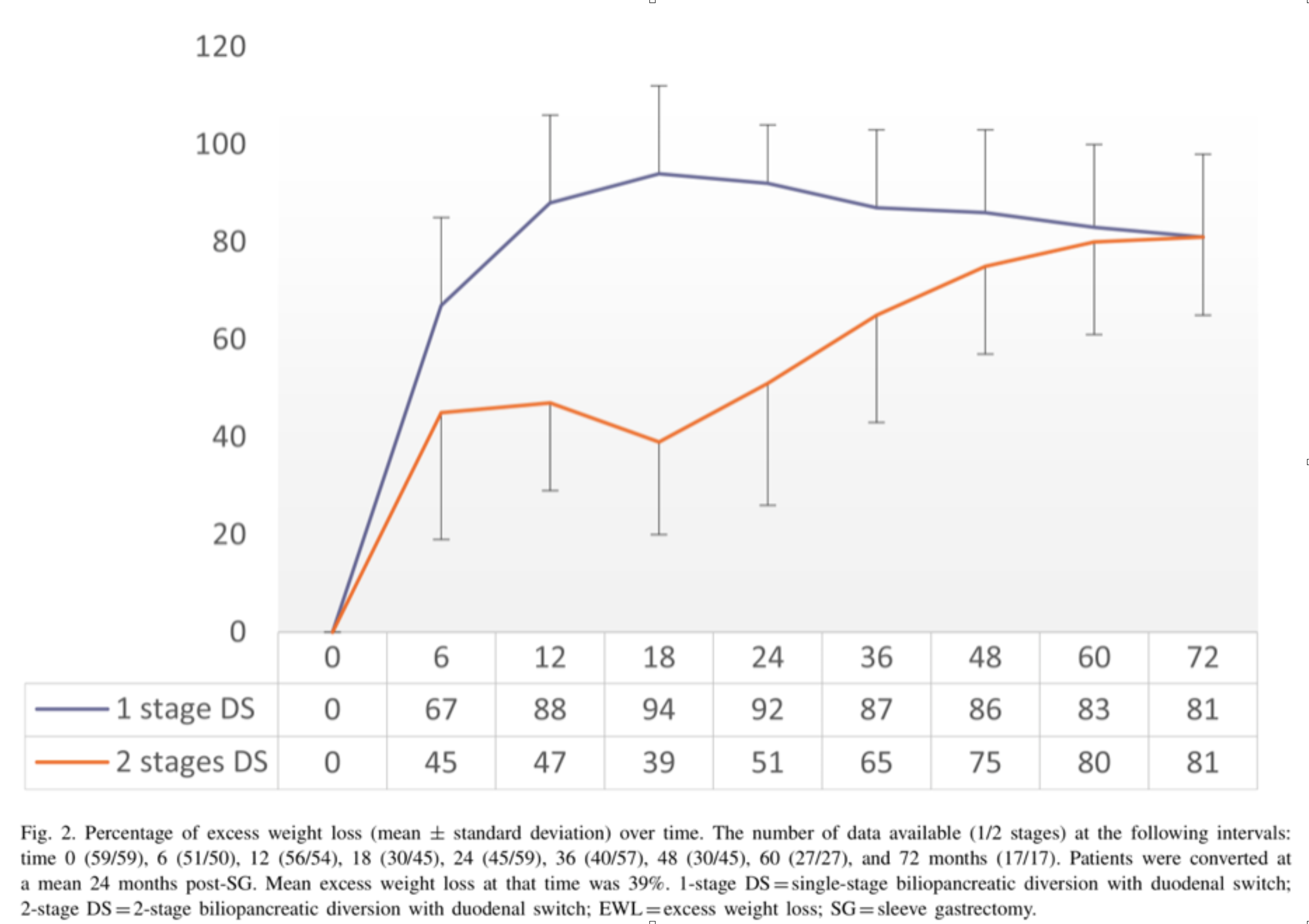
With regards to alternative approaches they indicate “ Other forms of revisions have been described, (i.e., adjustable or nonadjustable gastric band, plication, endoscopic balloon), with limited scientific evidence on their efficacy or safety. These procedures are mostly considered investigational and should be performed under Ethical Review Board approved protocols.”
In summary, patients may be offered a number of alternative if they are experiencing weight regain, inadequate weight loss, or return of co-morbidities after sleeve gastrectomy failure. We have seen a variety of them in our office. Patients who have had band placed on the sleeve, or are scheduled to have gastric balloons placed. As I have always said, buyers beware and know your outcomes and resolution of co-morbities.
Duodenal switch operation, (not the single anastomosis look alike) results in sustained weight loss and resolution of the co-morbidities. A second stage Duodenal Switch can mean adding the intestinal procedure to an existing Sleeve Gastrectomy. Some patients have required an adjustment to their Sleeve Gastrectomy in addition to adding the Duodenal Switch intestinal portion. Finding the right balance for each patient is a crucial part of our practice.
SIPS, SADI-S, Loop DS
May 01, 2019 9:03 am
The American Society for Metabolic and Bariatric Surgery (ASMBS) and MBSAQUIP-A on March of 2019, published and updated list of “Endorsed Procedures and Devices”
Endorsed Procedures and Devices | American Society for Metabolic and Bariatric Surgery
Note that any surgical procedures that does not employ two anastomosis, are not endorsed and are only recommended to be performed with an IRB (Institutional Review Board) or an IRB exemption. Duodenal Switch, Sleeve Gastrectomy, Roux en Y Gastric Bypass, Gastric Balloon, Adjustable Gastric Banding, and Nerve Blocking which are endorsed procedures.
SIPS, SADI-S, SIPS, Loop DS are all in the category of the “Non-Endorsed Procedures and Devices”. To see an anatomical comparison of these procedures to the Duodenal Switch procedure.
Patients should request that their consent be clearly defined and should explicitly outline the procedure that is being proposed to them. This is to avoid a patient having a procedure that they assumed, or are led to believe to be a Duodenal Switch operation with two anastomosis. Do your due diligence and know the procedure you want. Investigate if the surgeon you are working with performs the procedure you are interested in. Have them draw a picture of the procedure or give you a diagram of the procedure.
Cholecystectomy-Gallbladder Removal
September 10, 2018 9:44 am
There are differing opinions, based on a broad set of scientific publication, wether or not gallbladder should be removed at the time of weight loss surgery. Obviously, Cholecystectomy is a stand alone general surgical procedure that is often performed due to gallstones and/or gallbladder disease with a variety of symptoms. However, the focus of this blog will deal with Bariatric Surgery and Cholecystectomy.
Rapid weight loss can increase a patients chance of forming gallstones. This rapid weight loss can be as little as 3-5 pounds per week. Weight loss surgery can increase your risk for gallstone formation. Several of the common thought processes the mechanism of this is, obesity may be linked to higher cholesterol in the bile, larger gallbladders, high fat diet and larger abdominal girth.
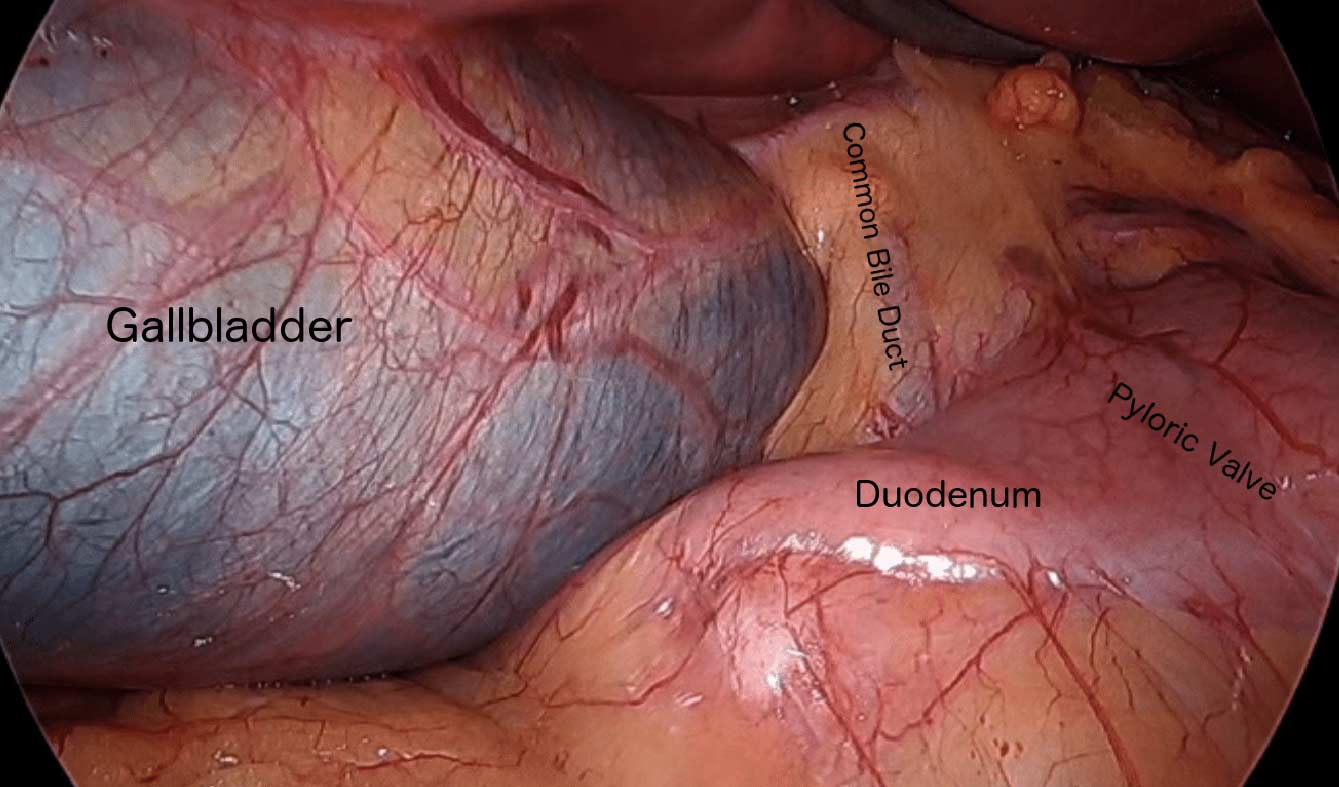
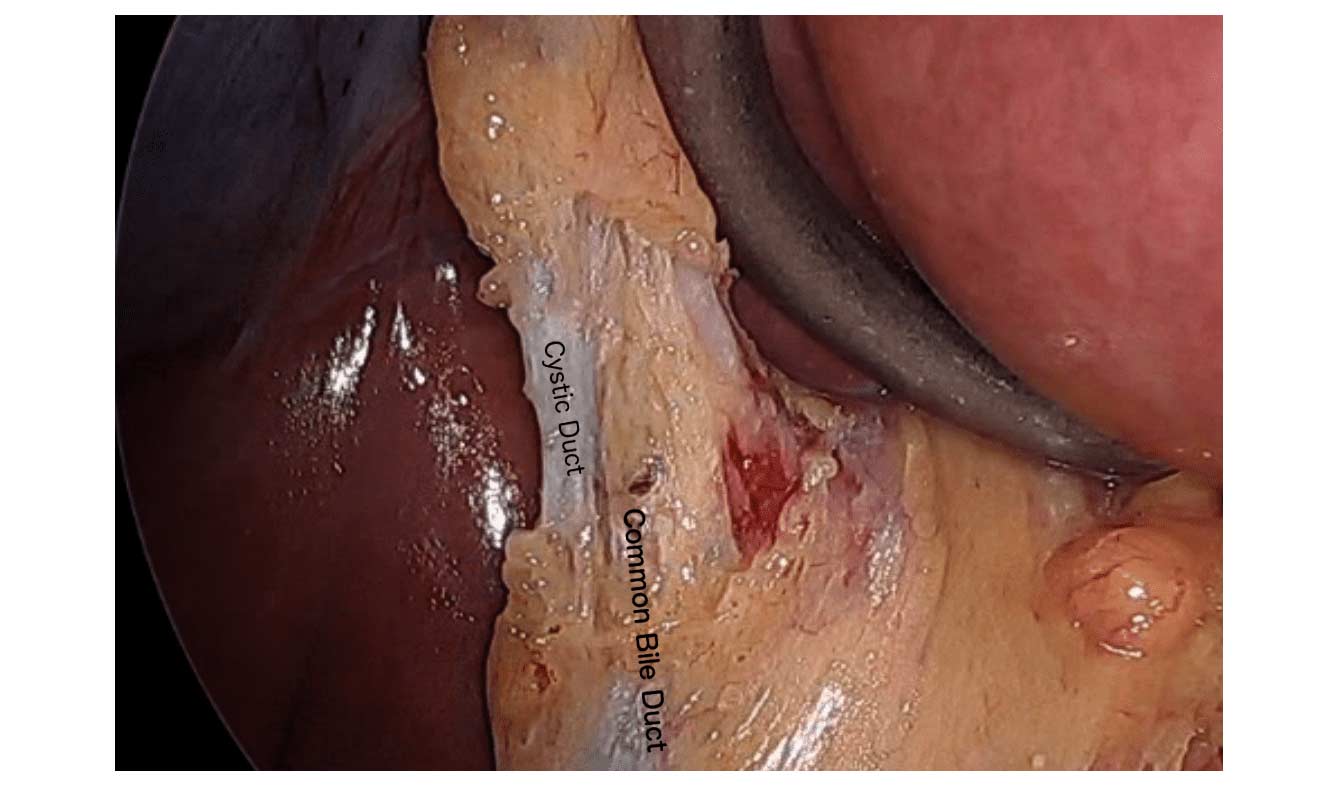
When a patient is having the Duodenal Switch (DS) Bariatric operation, or having a revision of a failed gastric bypass to the DS, I always remove the gallbladder. This is because there isn’t an anatomical route to utilize endoscopic procedure for an ERCP should the need rise.
In the case of a patient undergoing Vertical Sleeve Gastrectomy, if there are any indications or complaints of abdominal pain then an ultrasound is done. If there are findings of gallstones or other disease of the gallbladder, then a cholecystectomy is performed at the same time as the Sleeve Gastrectomy.
In my opinion, every patient having the Gastric Bypass (RNY) should also have the gallbladder removed because of the anatomical limitations after surgery that prevents the use of ERCP if needed. Some clinicians will place the patient on a long term medications to reduce the chance of gladstone formation after surgery, which themselves have side effects limiting the compliance in most patients.
Further information on Common Bile Duct Dilatation and ERCP
Review & Update Giveaway!
August 31, 2016 6:27 pm
The Prize winners are Jo and Kimberly! Congratulations ladies and enjoy the Obesity Help National Conference! Thank you to all that participated in the Giveaway!
We are holding a review and update giveaway for two different prizes! Thank you for your
participation!
One Prize and One Grand Prize
Prize: two tickets to Obestiy Help National Conference Sept. 30-Oct 1, 2016
Grand Prize: two tickets to Obesity Help National Conference and one night
hotel stay October 1, 2016
Conference: 11999 Harbor Boulevard Garden Grove, California 92840 Event link here
Hotel Prize: SHERATON GARDEN GROVE – ANAHEIM SOUTH HOTEL
12221 Harbor Boulevard
Garden Grove, California
Official Rules:
How to Enter and eligibility: All entrants and winners must be 18 years of age or older at the time of entry. Up to 5 entries per person.
- Write a review of Dr. Ara Keshishian on one or all of the sites below or do an update on your profile on Obesity Help between now and Sept. 8, 2016 at 5:00 PM
2. Take a screen shot of the review or update with your username and date.
3. E-mail the screenshot to contact@dssurgery.com with your contact information (name, phone number, e-mail, and mailing address )
4. Entries must be a verifiable patient of Dr. Ara Keshishian in Glendale, CA.
Promotion Timing:
The Review & Update Giveaway begins September 1, 2016 and ends September 8, 2016 at 5:00pm PST
How Winners are Chosen:
Winners will be chosen by random draw. Odds of winning vary upon the number of entries received for the giveaway.
Winner Notification and the Claiming of Prizes:
Winners will be notified via the email provided at time of entry and also published on our blog comments www.dssurgery.com/blog and on our FaceBook page. The winner will have 72 hours to respond to the winning notification email or the prize will be forfeited. The prizes have no cash value. The prizes are non-transferable and must be accepted as awarded. No changes may be made to the prizes. There is no cash value for the prizes.
General Conditions:
By entering the Giveaway, entrants agree to abide by and be bound by these Official Rules and the decisions of the Sponsor, which are final and binding in all matters relating to the Giveaway, and release and hold harmless Sponsor and its affiliates, directors, officers, employees and assigns from and against any liability, claims, lawsuits, judgments, losses, damages of any kind, injuries, death, property damage, costs and expenses, arising from, resulting from or in connection with the Giveaway, the participation in the Giveaway, or the receipt, possession, use or misuse of any prize. Sponsor is not responsible for lost, late, incomplete, inaccurate, stolen, delayed, misdirected, undelivered or illegible entries or for lost or stolen entry boxes or other errors or difficulties of any kind whether human, mechanical, electronic, typographical, printing or otherwise relating to or in connection with the Giveaway, including, without limitation, errors or difficulties which may occur in connection with the administration of the Giveaway, the processing of entries, the announcement of the prizes, or in any Giveaway-related materials. Sponsor is not responsible for technical, hardware, software or telephone malfunctions of any kind, lost or unavailable network connections, or failed, incorrect, incomplete, inaccurate, garbled or delayed electronic communications caused by the user or by any of the equipment or programming associated with or utilized in the Giveaway. Persons who tamper with or abuse any aspect of the Giveaway or who are in violation of these Official Rules, as solely determined by Sponsor, will be disqualified and all associated entries will be void. The Sponsor reserves the right, at its sole discretion, to cancel, terminate, modify or suspend the Giveaway if, in Sponsor’s opinion, it is not capable of running as planned, including, but not limited to, due to tampering, unauthorized intervention, fraud, technical or phone line failures or any other problems beyond the control of the Sponsor, and select the winners for affected drawing(s) from among all eligible entries timely received for such affected drawing(s) prior to cancellation.