Category: HIDA scan
Gastroesophageal Reflux: Bile Vs. Acid
May 14, 2019 12:52 pm
Gastroesophageal (GE) reflux is the condition when the stomach content are able to “reflux” back thru an incompetent lower esophageal sphincter (LES) into the esophagus.
Gastroesophageal reflux Disease (GERD) is the clinical condition which is the result of long standing reflux and results in microscopic and visible changes to the inner lining of the esophagus, esophageal mucosa.
GERD is a non descriptive as to the cause of the condition. It only states that the content of the stomach have been irritating the lining of the esophagus on chronic bases. This can be caused by an anatomical abnormality fo the GE junction (Hiatal Hernia), or may be related to disfunction the LES. Other possible causes of the GERD may be infection (H.Pylori) environmental (stress) and dietary (nicotine, alcohol, caffeine, spicy food) in origin.
So far we have not clarified the chemical nature of the the refluxed content.
In Acid Reflux, the relative acid overproduction of acidic secretion and the exposure of the esophageal mucosa is what needs to be addressed. This is accomplished by acid suppression medications, Anti Histamine (H2 blockers) Proton pump inhibitors (PPI) for example. The physiology, and the mechanism involving this condition is well understood. As a surgeon, we do however see patients who should have had surgical intervention. The initial mode of therapy for a patient with documented acid reflux, and or symptomatic hiatal hernia is placing them on medication. These patients are then recommended to have related upper endoscopy. Patients who do not improve or where deterioration of the esophageal mucosa, presence of precancerous cells, then the patients are referred for surgical intervention.
Bile Reflux, contrary to acid reflux may have very little if anything with the LES. The symptoms experienced by the patient may be as ofter related to the excessive bile in the stomach seen frequently
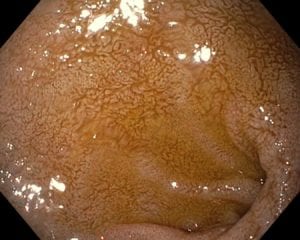
after cholecystectomy, or in those patients with dysfunctional gallbladder (low EF on HIDA scan).
The treatment of Bile reflux, is Duodenal Switch with without the associated sleeve gastrectomy component in addition to repair of hiatal hernia if present Ann Surg. 2007 Feb; 245(2): 247–253.
Evaluations of Gallbladder Disease And Function
April 11, 2015 7:03 am
Gallbladder disease can include both anatomical and functional condition. We are familiar with gallstones. Bile acids, Lecithin (a phospholipid), and cholesterol are present in the Bile. When the proportional percentage of each one of them is outside a very narrow range, gallstones are formed. Approximately 75% of the gallstones are formed because of the supersaturation of the content of the gallbladder with cholesterol which results in cholesterol stone formation. The rest are pigmented stones.
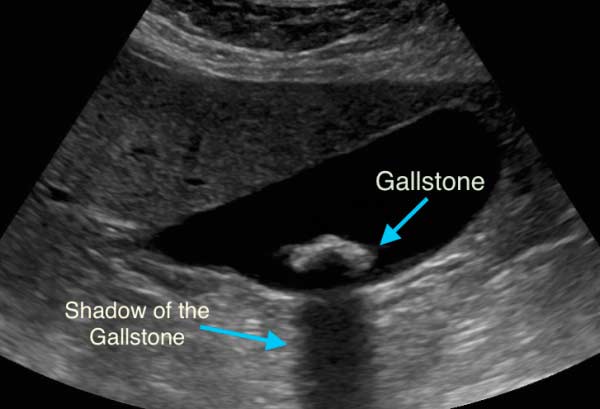
Gallstones are usually identified by ultrasound and they are seen as shadows.
There are patients that have a normal gallbladder ultrasound result that continue to have signs and symptoms of gallbladder disease, such as abdominal pain in the right upper quadrant, nausea and vomiting with fatty meals, and bloating to name a few. These patients should be evaluated by a dynamic HIDA scan.
A dynamic HIDA scan study evaluates the function of the gallbladder, by creating a movie of the gallbladder, where as an ultrasound takes pictures of the gallbladder.
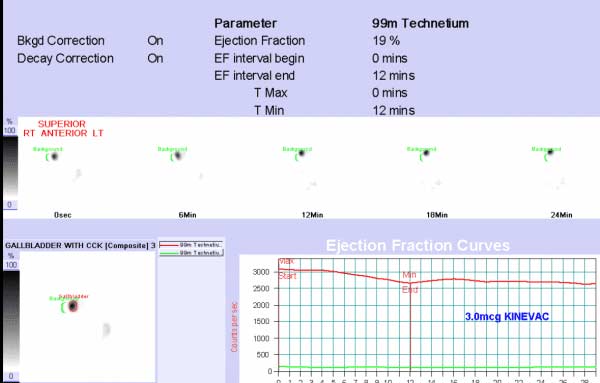
In a dynamic HIDA scan, and contractility of the gallbladder is reported in form of ejection fraction (%EF). This represent the amount of gallbladder contraction in response to the stimulation by a fatty meal mediated thru cholecystokinin (CCK). A normal EF is greater that 35%. Anything less than than with the sign and symptoms of gallstones, should be highly suspect for acalculous cholecystitis. Calculus because there is no stone.
(The bright white collection represents the filling of the gallbladder)
This short movie represents the uptake of the radio nuclear material in the gallbladder and its normal secretion in the small bowel.
These are the static images before the injection of CCK.
Following the injection, digital subsection of the images measure the amount of nuclear activity of the gallbladder before and after contraction and an Ejection Fraction is calculated.
- Weight loss Medications compared to surgery February 20, 2024
- SIPS-SADI and ASMBS December 31, 2023
- Survey December 16, 2023
- Long Term Outcome Survey December 1, 2023
- Weight Loss Injection May 10, 2023