Tag: PCOS
PolyCystic Ovarian Syndrome PCOS
September 04, 2018 9:58 am
PolyCystic Ovarian Syndrome PCOS is a complex condition. The exact cause of PCOS is unknown however, it involves hormones imbalance and multiple ovarian cysts, irregular menses, and infertility. In some cases, PCOS can be compounded by diabetes, hypertension and other metabolic conditions. PCOS has been shown to effect approximately 10% of women of childbearing age with symptoms of menstrual abnormalities, poly cystic ovaries, and excess androgen (male sex hormone). PCOS should be diagnosed by ensuring there are no other underlying endocrine issues. There are several associated disease processes that seem to be related to PCOS. These related disease processes are Type 2 Diabetes, higher depression and anxiety, increased cardiovascular risks, stroke, hyperlipidemia, sleep apnea, overall inflammation, and endometrial cancer.
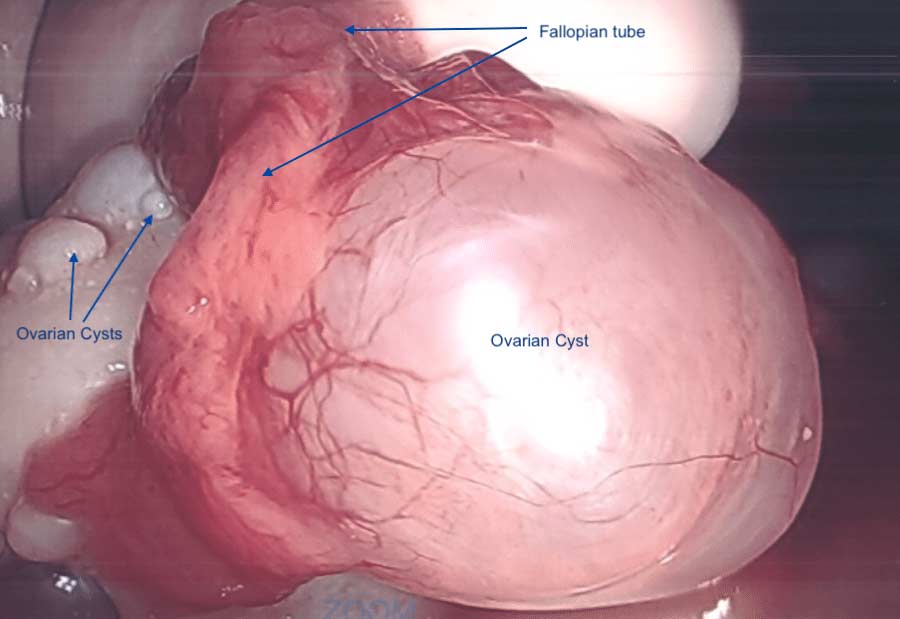
Anatomically, numerous cysts are found on the ovaries. These are usually diagnosed by ultrasound, blood levels of hormones, and symptoms described above.
Bariatric Surgery and PolyCystic Ovarian Syndrome PCOS
Bariatric Surgery can improve PCOS in those individuals with Type 2 Diabetes Mellitus. Further information on weight loss surgery and its effect on PCOS here.
Bariatric Surgery effects on PCOS
May 17, 2017 11:02 am
Women with Polycystic Ovary Syndrome (PCOS) often feel hopeless and depressed with their diagnosis. Bariatric Surgery improves metabolic syndrome, diabetes resolution, cardiac improvement, quality of life, and increased life expectancy. Bariatric Surgery effects on PCOS are positive in many aspects. However, there isn’t a consensus regarding recommendation for bariatric surgery for PCOS other than morbidly obesity with co-morbities.
PCOS has been shown to effect approximately 10% of women of childbearing age with symptoms of menstrual abnormalities, poly cystic ovaries, and excess androgen (male sex hormone). PCOS should be diagnosed by ensuring there are no other underlying endocrine issues. There are several associated disease processes that seem to be related to PCOS, such as Type 2 Diabetes, higher depression and anxiety, increased cardiovascular risks, stroke, hyperlipidemia, sleep apnea, overall inflammation, and endometrial cancer.
Bariatric surgery can improve several issues related to PCOS such are Type 2 Diabetes, lower weight, sleep apnea, infertility, and hyperlipidemia. Duodenal Switch has the highest rate of Type 2 Diabetes resolution of all weight loss surgeries available at this time. Duodenal Switch also significantly improves hyperlipidemia.Weight loss surgery has been shown to improve and in some cases resolved PCOS in general. A recent meta-analysis of the effects of bariatric surgery in more than 22,000 procedures found an average weight loss of 61%, associated with the complete resolution or improvement of diabetes, hyperlipidemia, hypertension, and obstructive sleep apnea in more than 60% of the patients. Another study looked just at PCOS patients and their metabolic improvement from 47% of the PCOS population to only 21% post Bariatric Surgery.
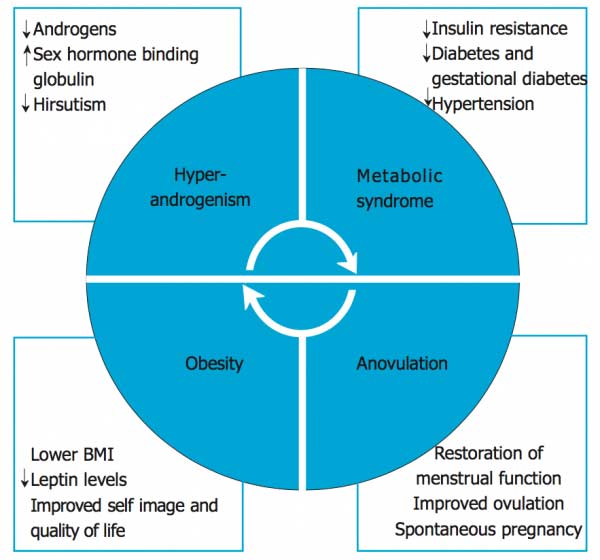
Several recent article have described how Bariatric Surgery effects PCOS with positive aspects related to fertility. The range of improved fertility in post Bariatric PCOS patients is a wide range of 33-100% with in the literature. It is thought that the loss of fat mass improves hormone levels and insulin resistance in PCOS and has a positive effect on fertility. One study of only 6 omen had a 100% improvement of infertility. American Society of Metabolic and Bariatric Surgery as well as the American College of Obstetricians and Gynecologist have a statement that bariatric surgery is should not be considered a treatment for infertility. The graphic below demonstrates the overlap of some of the symptomatology between PCOS, obesity and metabolic syndrome.
There are several documented positive effects and improvement in co-morbidilties related to PCOS post Bariatric Surgery. These include lipid profile, lower weight, cardiovascular risk, hypertension, and fertility. It is important to note that certain bariatric surgeries have better resolution of these co-morbidities or symptoms of PCOS. Always discuss with your physicians and surgeon what your options are and which treatments may work best for you.
In Summary, PCOS is a metabolic disease condition affecting different organ systems. Weight loss surgery should be considered as a viable treatment option and should be discussed with your OB/GYN and Infertility specialist.
Acanthosis Nigricans
November 16, 2015 9:28 am
There are a a number of skin conditions that are associated with the disease of obesity. Acanthosis Nigricans is characterized as areas of thickened, dark, velvety discoloration in body folds and creases. Usually seen in the armpits, neck, under the breasts, in the skin folds of the abdomen and groin. The exact cause of it at the molecular level is not clear other than seen frequently with insulin excess in the case of benign conditions. This symptom can give a warning about health conditions that require further investigation.
Patients may assume excessive sweating and poor hygiene are the causes of this condition- both of which are incorrect.
Acanthuses Nigerians is caused by acanthosis and papillomatosis of the epidermis (the outer most layer of the skin) pigmentation is usually not in this area, rather than pigment-producing cells. The skin proliferation abnormalities in acanthosis nigrcans are frequently associated with hyperinsulinemia and insulin resistance. This probably presents the best understanding of the pathology behind it. It suggests that the layer of skin gets thicker probably caused by some stimuli- as indicated above seen with insulin excess.
There are two forms of this condition: Benign and Malignant.
Benign forms are associated with obesity, insulin resistance, and type II diabetes.
Insulin resistance: Insulin is a hormone secreted by the pancreas that allows your body to process sugar. Resistance predisposes to type II diabetes.
Hormonal disorders: Hypothyroidism, Polycystic Ovarian Disease, and other endocrine disorders of adrenal glands are ovaries
Drugs: Certain drugs and supplements such as high-dose niacin, birth control pills, steroids, may cause acanthosis nigricans.
Malignant forms may be an indication of Gastro-intestinal cancer such as stomach, colon, or liver cancer.
Treatment: No specific treatment is available for acanthosis nigricans. Treating the underlying conditions may restore some of the normal color and texture to affected areas of skin.
- Weight loss Medications compared to surgery February 20, 2024
- SIPS-SADI and ASMBS December 31, 2023
- Survey December 16, 2023
- Long Term Outcome Survey December 1, 2023
- Weight Loss Injection May 10, 2023