Category: diabetes
Sleeve Gastrectomy in Adolescent patients
September 23, 2020 5:44 am
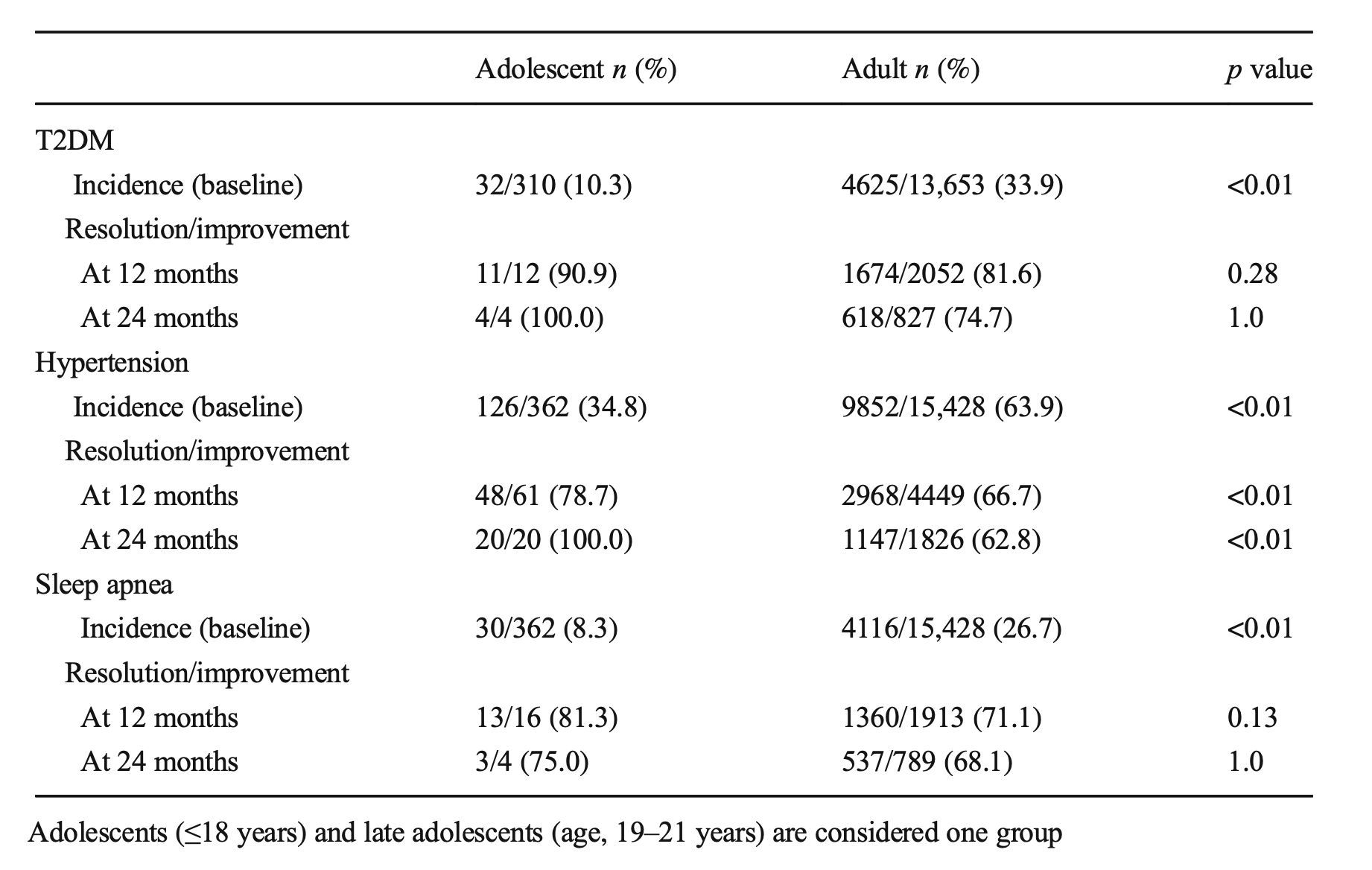 Sleep apnea resolved at the same rate. These early interventions can mean there may be lower long-term risk and associated conditions for these teens as they age.
A recent article was written from several adolescent weight loss surgical patients’ perspectives: This included their feelings of hope for their futures and health.
Sleep apnea resolved at the same rate. These early interventions can mean there may be lower long-term risk and associated conditions for these teens as they age.
A recent article was written from several adolescent weight loss surgical patients’ perspectives: This included their feelings of hope for their futures and health.
100% Fruit Juices and Risk of Cancer
April 16, 2020 8:54 pm
We have talked about the excess free calorie that is present with fruit juices. Now there is proven research article demonstrating the connection between surgary drinks and the increased risk of cancer. This study 
This study is significant for a number of reasons: It is a very large study with over a 100,000 subjects studied. Furthermore, it was specifically looking for association between nutrition and health.
The conclusion of this research article is self explanatory. Eliminating or cutting down high sugary drinks is an easy way of reducing cancer risk factors. The study also states that there were no identifiable association between the artificial sweeteners and cancer risks. However, this conclusion was not statistically significant. The relationship between sweeteners and cancer have been studied extensively in the past and we’ve shared several of them.
Covid-19 Pandemic and Obesity
April 12, 2020 7:44 pm
We have now seen several articles with data collection regarding patients with obesity and COVID-19 being at greater risk of hospitalization. We can look at metabolic syndrome associated with obesity as a risk factor also.
We have all been in physical isolation due to Covid-19 pandemic. The strategy of minimizing contact has worked. The data is clear when comparing information from states that instituted an aggressive containment plans compared to those who have not. This shows a sigifnicat flattening of the curve in California for example.
The CDC publishes the Morbidity and Mortality Weekle Report (MMWR) . The latest publushed summary (as of date of publucation of this blog) provides an insight to the risk factors of hospitalization.
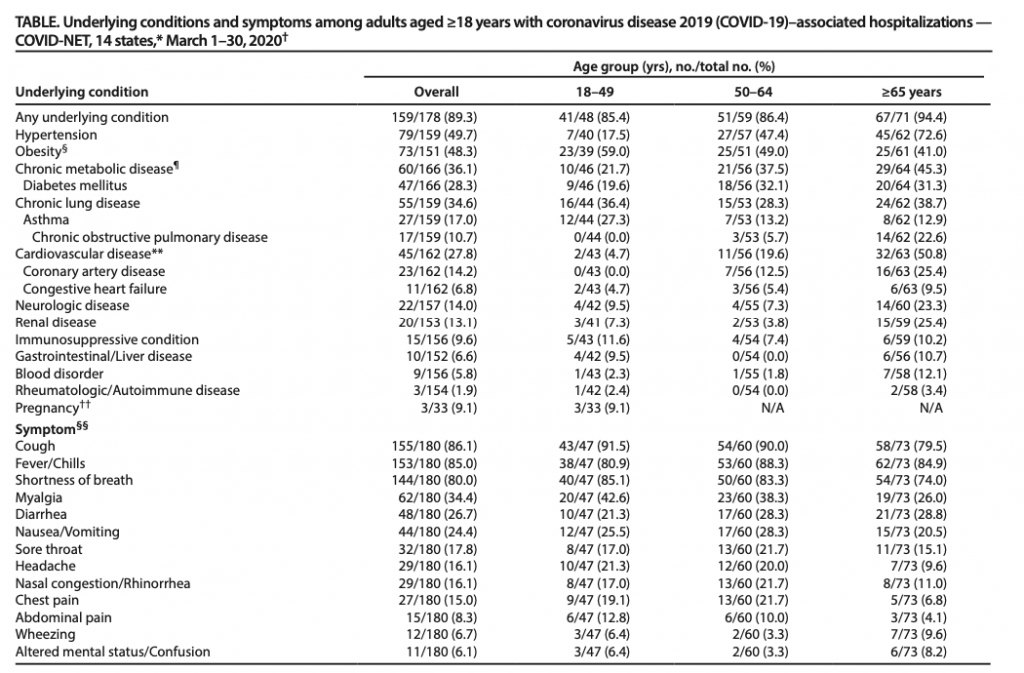 The above table outlines the underlying conditions of those hospitalized with Covid-19.
The above table outlines the underlying conditions of those hospitalized with Covid-19.
Concerning to see that a respiratory virus is more likely to hospitalize those with Obesity, Diabetes and hypertension at a higher rate than lung and pulmonary related conditions.
Let us recognize that this is only a summary collected data. Therefore, there are limitatation to making any assumption of conclusion based on this information.
With those limitation aknowldged, and relying on our obesity related comobidities, we can make a few conclusions:
Not surprising, Obesity as with other diseases, compounds Covid-19 exposure and infection. Diabates is also a risk factor. There are no indepth information available on the diabetic patients. There is now data showing superior outcome of diabetes resoultion with weight loss surgery compared ro medical treatment.
Diabetes and Weight Loss Surgery
April 06, 2020 5:51 am
The scientific literature is riddled with evidence pointing to the benefit of early metabolic surgery as a superior treatment, remission and possible cure option for diabetes. Unfortunately, the medical education, pharmaceutical companies, primary care healthcare delivery systems and third party payers (health insurance companies) have not caught up with the published data. The American Diabetes Association has changed their guidelines to reflected the benefit for combating diabetes with weight loss surgery.
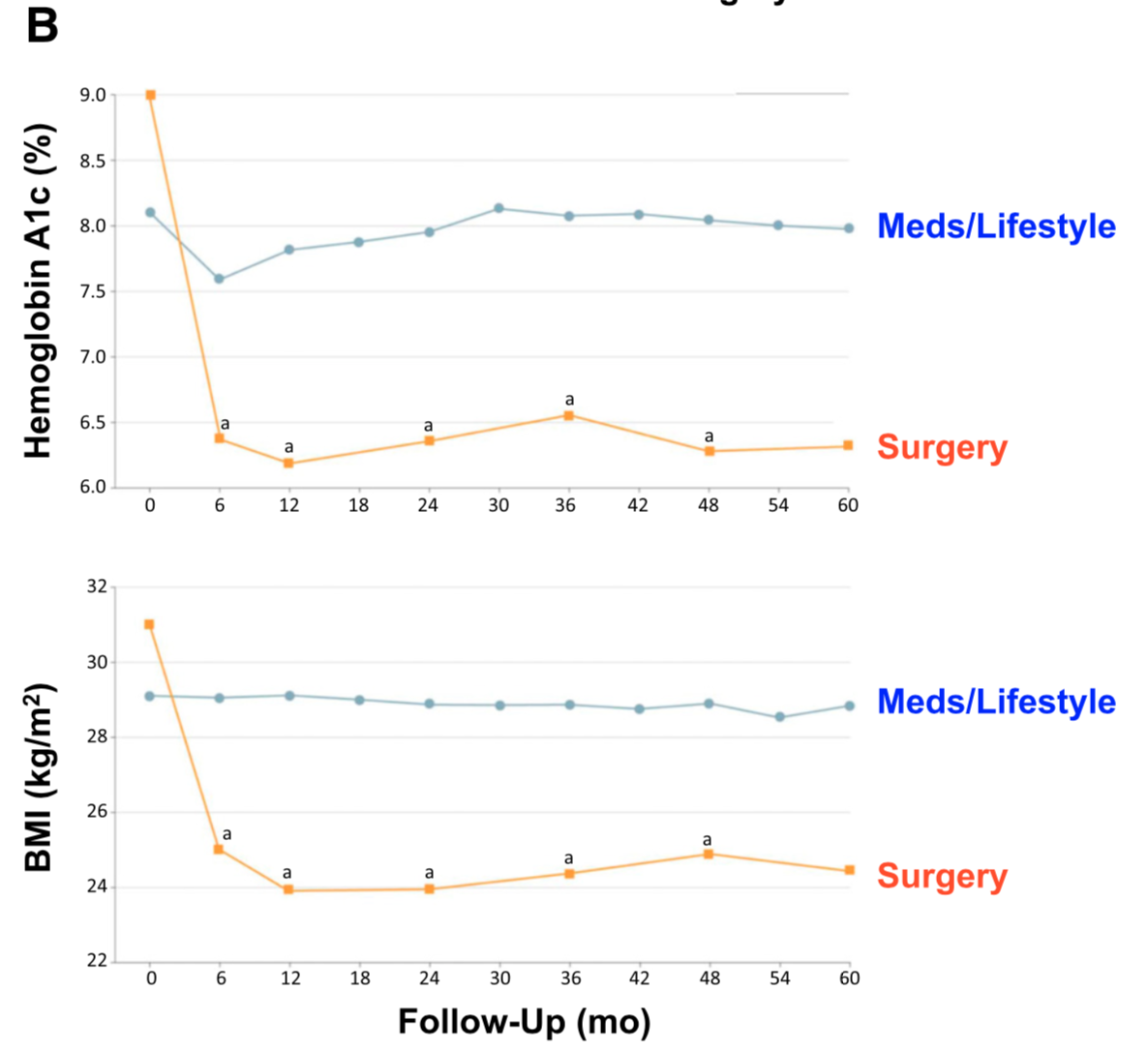
There is ample evidence of the superior outcome of surgery as a treatment option for diabetes when compared to medical managment. Cummings et.al, in a published article in Diabetes Care, showed sustained stabilization of the Hemoglobin A1C six years after surgery. In contrast, there was no significant changes noted in the non-surgical group.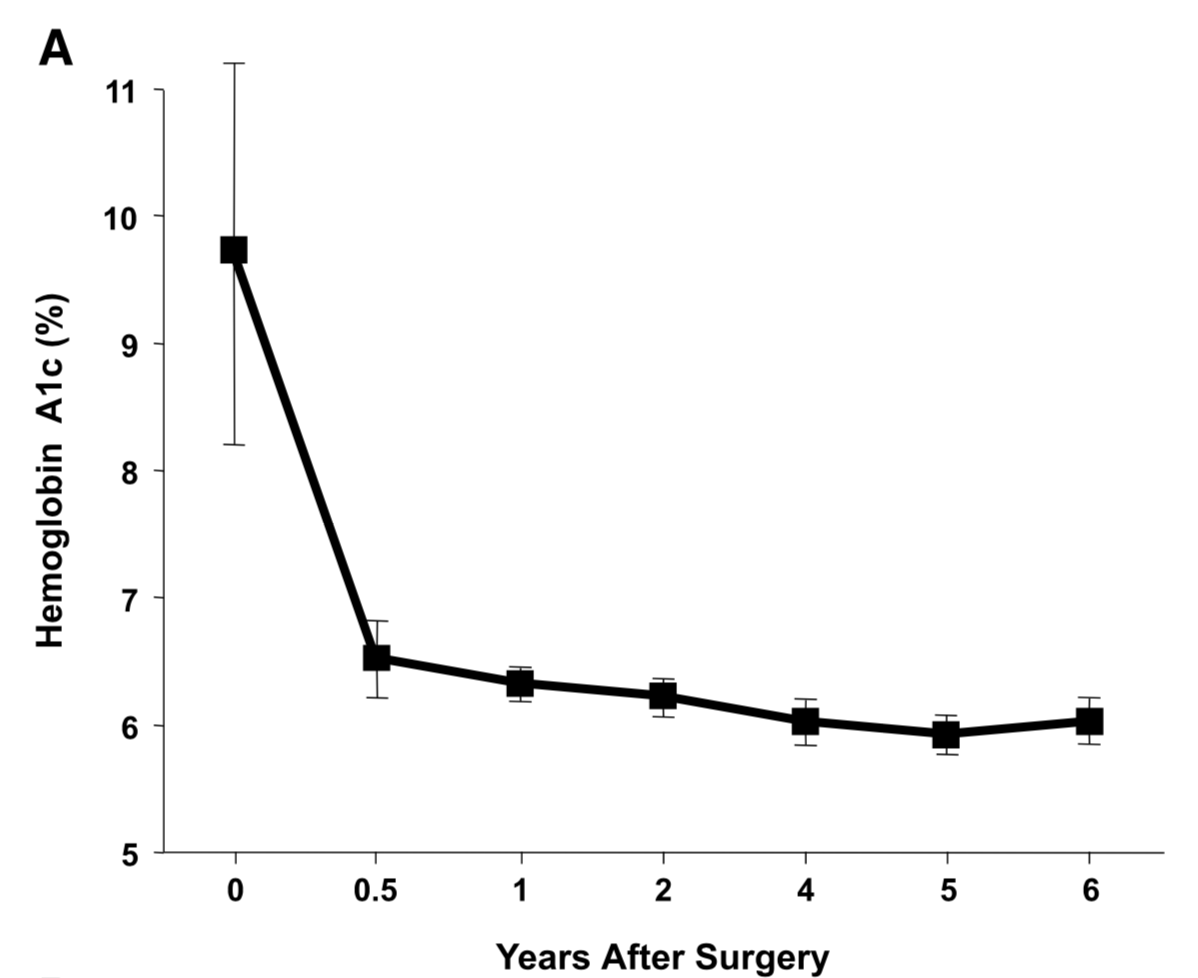
Jans et.al. , in November of 2019 showed that the patients who had NOT been on Insulin, and had metabolic surgery had the highest long term success for resolution and remission of the diabetes. This identifies that having a patient be proactive in their care by having metabolic surgery improves success rates.
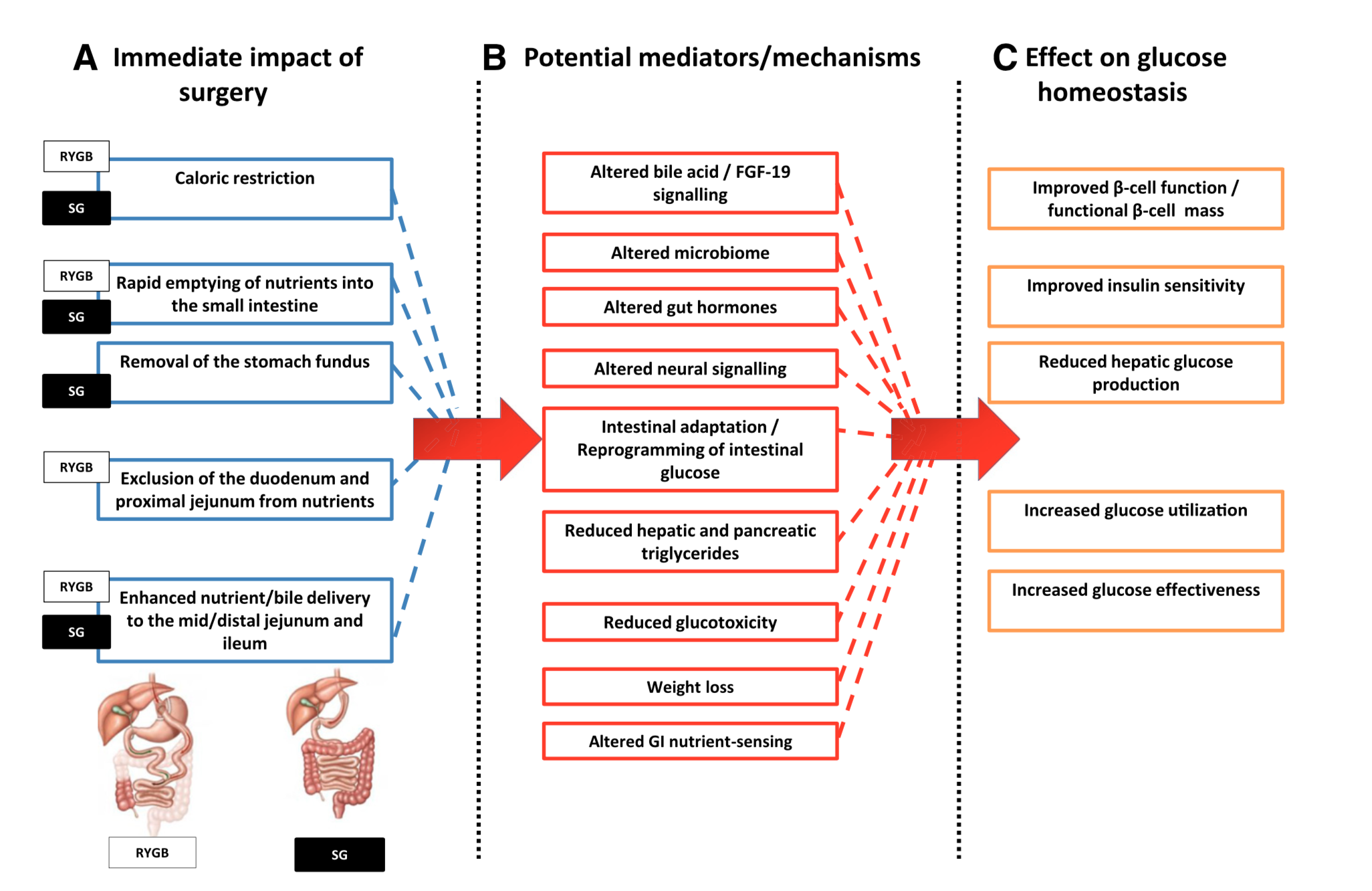
The exact mechanism by which the diabetes is resolved is unclear. The weight loss may play a role. There are numerous hormones and neuroendocrine modulators which control the complex metabolic pathways. Batterham et.al., in Diabetes Care (2016), published a summary overview of the possible mechanism involved in diabetes improvement following metabolic surgery.

There are a number of overlapping and sequential layers for possible reasons why diabetes resolves after weight loss/metabolic surgery. These may be directly related to surgery and the reduction of the calorie intake or absorption. It may also involve the neuroendocrine modulators.
What can be said definitively is that early surgical intervention is best and most likely the only permanent solution to type II diabetic resolution. There is no medical justification in not considering metabolic surgery in diabetic patients who may also have difficulty with meaning a BMI< 35.
PolyCystic Ovarian Syndrome PCOS
September 04, 2018 9:58 am
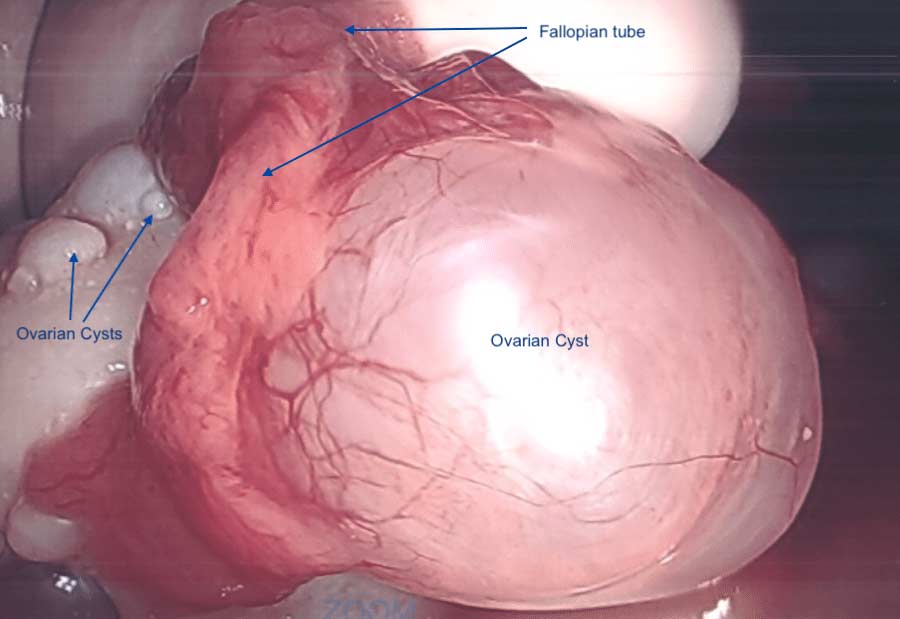
PolyCystic Ovarian Syndrome PCOS is a complex condition. The exact cause of PCOS is unknown however, it involves hormones imbalance and multiple ovarian cysts, irregular menses, and infertility. In some cases, PCOS can be compounded by diabetes, hypertension and other metabolic conditions. PCOS has been shown to effect approximately 10% of women of childbearing age with symptoms of menstrual abnormalities, poly cystic ovaries, and excess androgen (male sex hormone). PCOS should be diagnosed by ensuring there are no other underlying endocrine issues. There are several associated disease processes that seem to be related to PCOS. These related disease processes are Type 2 Diabetes, higher depression and anxiety, increased cardiovascular risks, stroke, hyperlipidemia, sleep apnea, overall inflammation, and endometrial cancer.
Anatomically, numerous cysts are found on the ovaries. These are usually diagnosed by ultrasound, blood levels of hormones, and symptoms described above.
Bariatric Surgery and PolyCystic Ovarian Syndrome PCOS
Bariatric Surgery can improve PCOS in those individuals with Type 2 Diabetes Mellitus. Further information on weight loss surgery and its effect on PCOS here.
Resistance Exercise BandsExclusive Member Content
July 19, 2017 12:47 pm
Less Invasive, Easier?
July 20, 2016 11:02 am
There is a continuous desire for a “less invasive”, “easier” procedure for the treatment of obesity and its associated co-morbidities. We have been very clear when discussing the benefits and long term outcome of the procedures. Let’s remind ourselves that “less invasive” does not mean a better option. In almost all cases a less invasive weight loss surgery means less weight loss, lower incidence of resolution of co-morbidities, and in some cases higher complications rate. Have we forgotten the adjustable gastric banding that was advocated to be the cure all for all obesity? All we hear now are the complications, the long term sequel of the reflux, hiatal hernia, irreversible esophageal injury, in addition to inadequate weight loss or weight regain.
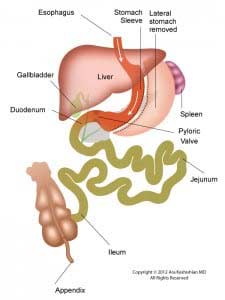
Unfortunately, the same is to be said about the Sleeve Gastrectomy. We have said, as supported by the scientific literature, that the long term outcome of the sleeve gastrectomy is not as good as that of the Duodenal Switch procedure. This is true for the amount of weight loss as well as the resolution of the co-morbidities. We see quite a few patients who have gained their weight back after sleeve, never lost enough weight, and/or did not achieve resolution of their co-morbidities, such as diabetes, and are having their procedure revised to Duodenal Switch procedure.
Here is a recent publication that discusses this.
Along with the same argument, this is why I caution patients when having the SIPS or SADI procedures. There is a chance that when the long term data for SIPS/SADI is available there may be some benefits procedure. However, as it stands at this point in time, these procedures are not the same as the Duodenal Switch procedure. So in short, less invasive, easier isn’t better.
Weight loss Surgery for Treatment of Diabetes
May 25, 2016 7:21 am
New guidelines and recommendation are coming out of the second Diabetes Surgery Summit in the Fall of 2015. One major change is Metabolic or Weight Loss Surgery for the treatment of Diabetes. With all the advances made in newer classes of medication for treatment of diabetes, the majority of patients who are being treated fail to get to achieve the desired results of lowered blood glucose level. This is in contrast where weight loss surgical procedures such as Duodenal Switch can results in >95% cure rate of type II diabetes.
The American Diabetes Association has made the recommendation for weight loss surgical procedures be considered as a treatment option for type II diabetes.
Summarizing their criteria “According to the new Guidelines, metabolic surgery should be recommended to treat type 2 diabetes in patients with Class III obesity (BMI greater than or equal to 40 kg/m2), as well as in those with Class II obesity (BMI between 35 and 39.9 kg/m2) when hyperglycemia is inadequately controlled by lifestyle and medical therapy. It should also be considered for patients with type 2 diabetes who have a BMI between 30 and 34.9 kg/m2 if hyperglycemia is inadequately controlled, the authors agreed. The Consensus S
tatement also recognizes that BMI thresholds in Asian patients, who develop type 2 diabetes at lower BMI than other populations, should be lowered 2.5 kg/m2 for each of these categories. ”
This is a remarkable change in thought and policy on diabetic treatment and long term strategies that can only improve patient outcomes. Stabilization and blood glucose hemostasis can only improve patient health, health care utilization and health care costs.
Diabetes and Weight loss Surgery
June 30, 2014 5:44 pm
Diabetes should be considered as a family of diseases sharing a common name. They are different diseases because the cause, pathophysiology, and the treatment options are different for each diseases. This is not to say that there are not commonalities between them.
- Type I (Insulin deficiency, Juvenile onset)
- Type II (Insulin Resistance, Adult onset)
- Latent Autoimmune diabetes (LADA)
- Gestational
Type I diabetic patients requires insulin for control of their blood sugar. Insulin deficiency is the underlying problem with type I diabetes. The causes of type I diabetes are many and some are poorly understood. It is presumed that viral infections, genetics, infections, chronic pancreatitis and autoimmune conditions may all be potential causes of type I diabetes.
Type II diabetes is an insulin resistance state. This means that the patients’ body may be making adequate level of insulin however, for a number of reasons, the insulin is not able to normalize the blood sugars. Some Type II diabetic patients may also require insulin during advanced stages, but in most cases the initial treatment is oral medications.
| Diabetes Type | Blood Sugar | Blood Insulin |
| Type I | High | Low-absent |
| Type II | High | High(early disease state) |
The table above summarizes the laboratory findings in a patient who is diagnosed with diabetes. The measured insulin can be distinguished in the labs as being injected or patients own.
LADA is probably a subtype of Type I, with a delayed presentation. It behaves like Type I, with insulin deficiency, yet it is adult onset.
Gestational is more of a high blood glucose state during the pregnancy.
The goal of medical treatment for diabetes has been to normalize the blood sugars. There are no medical treatments regimens that correct any of the underlying causes of the Type I, or Type II.
In the case of Type I, the underlying case is Insulin deficiency. The definitive treatments may include Pancreatic transplantation, and intelligent Insulin pumps.
Surgical treatment of Type II, by some know and unknown mechanisms, corrects the underlying resistance to the insulin.
Weight loss surgical procedures have been shown to “cure” Type II”. The “remission” or “cure” rate of diabetes is really different between surgical procedures. Duodenal switch operation has been shown to have the highest remission-cure rate of all surgical procedures for the Type II diabetes. The references are available on our website. By definition, Type I can not be corrected-cured with weight loss surgery, since the underlying problem is insulin deficiency. What we have experienced however is that the Insulin requirements significantly decreases and blood glucose control is much easier after weight loss surgery.
There have been a number of articles reporting high relapse rate of Type II in gastric bypass patients. This is why I have always advocated that the patients with metabolic conditions, including diabetes should only consider the duodenal switch as their only surgical option.
The one study of 4434 patients, 68.2% of those patients who had Type II had remission within 5 years after the gastric bypass procedure. 35% of those patients, however, had a redevelopment of Type II after 5 years. “When the patients that never remitted and those that relapsed were added together, more than half of the patients (56%) did not have durable remission of diabetes.” (Obes Surg 2012 Nov 18:doi 10.1007/s11695-012-0802-1).
An article published in May 2010, reported 24% recurrence or worsening of the diabetes in patients who have had gastric bypass operation. (SOARD Volume 6, issue 3, May 201 249-253).