Category: esophagus
Three Different Problems: Gastritis, Gastroesophageal Reflux, and Bile reflux Gastritis
June 05, 2025 4:52 am
Gastritis is a general term used for the description of symptoms associated with several very different physical conditions and require different treatments based on their ideology . Gastritis, gastroesophageal reflux, and bile reflux gastritis
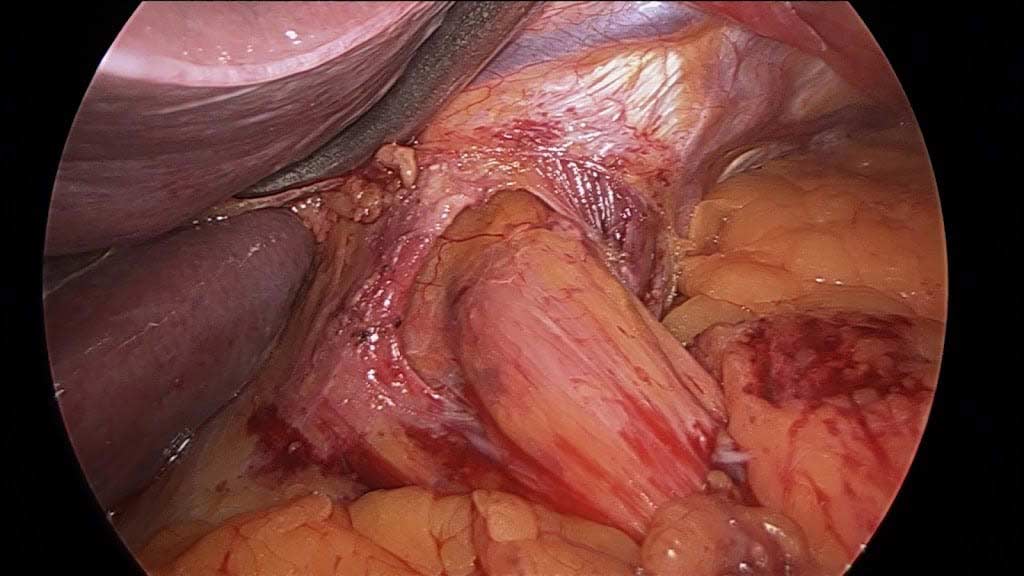
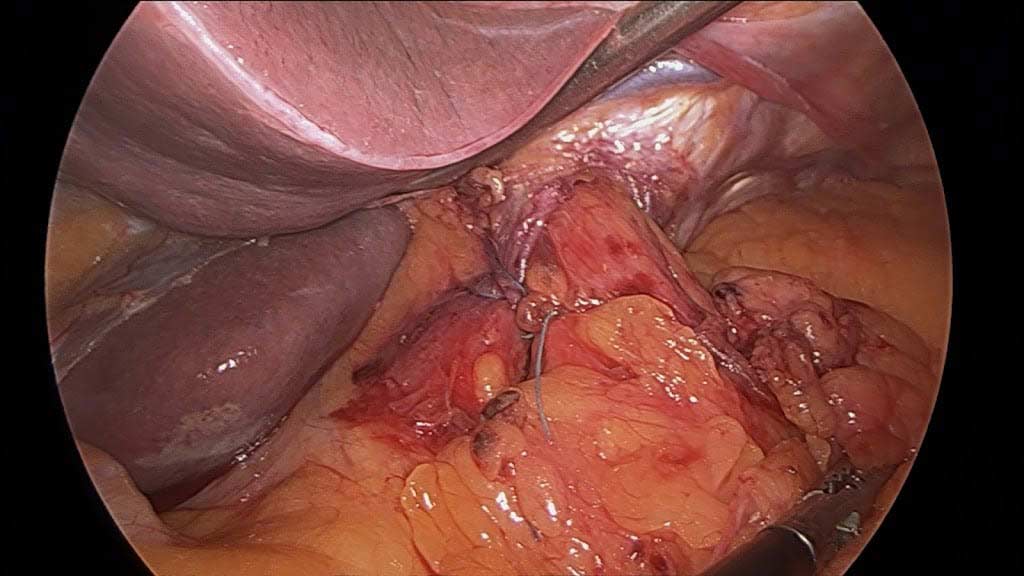
Gastritis may be caused by excess acid or bile in the stomach. Some patients may have gastroesophageal reflux due to a hiatal hernia, which needs to be treated surgically with Nissen fundoplication, regardless of the size of the hernia, contrary to what gastroenterologists recommend by prescribing antacids for an extended period. I have seen patients who have had one cm hiatal hernia and have been very symptomatic, and others who have had larger hiatal hernias and have been asymptomatic. Size should not be a determinant of whether the patient has had or will have a hernia repair or not.
Billiary Diversion is the definitive surgical procedure for Bile Reflux Gastritis.
Gastroesophageal Reflux: Bile Vs. Acid
May 14, 2019 12:52 pm
Gastroesophageal (GE) reflux is the condition when the stomach contents are able to “reflux” back through an incompetent lower esophageal sphincter (LES) into the esophagus.
Gastroesophageal reflux Disease (GERD) is a clinical condition caused by long-standing reflux that results in microscopic and visible changes to the inner lining of the esophagus and esophageal mucosa.
GERD is nondescript as to the cause of the condition. It only states that the stomach contents have been irritating the lining of the esophagus on a chronic basis. This can be caused by an anatomical abnormality of the GE junction (hiatal hernia) or may be related to dysfunction of the LES. Other possible causes of GERD may be infection (H. Pylori), environmental (stress), and dietary (nicotine, alcohol, caffeine, spicy food) in origin.
So far, we have not clarified the chemical nature of the refluxed content.
In Acid Reflux, the relative acid overproduction of acidic secretion and the exposure of the esophageal mucosa need to be addressed. This is accomplished by acid suppression medications, anti-histamine (H2 blockers), and Proton pump inhibitors (PPIs). The physiology and the mechanism involving this condition are well understood. As a surgeon, however, I do see patients who should have had surgical intervention. The initial mode of therapy for a patient with documented acid reflux and or symptomatic hiatal hernia is placing them on medication. These patients are then recommended to have a related upper endoscopy. Patients who do not improve or where deterioration of the esophageal mucosa and the presence of precancerous cells are referred for surgical intervention.
Bile Reflux, contrary to acid reflux, may have tiny, if anything, to do with the LES. The symptoms experienced by the patient may be as after related to the excessive bile in the stomach, which is seen frequently
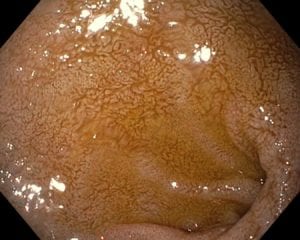
after cholecystectomy, or in those patients with a dysfunctional gallbladder (low EF on HIDA scan).
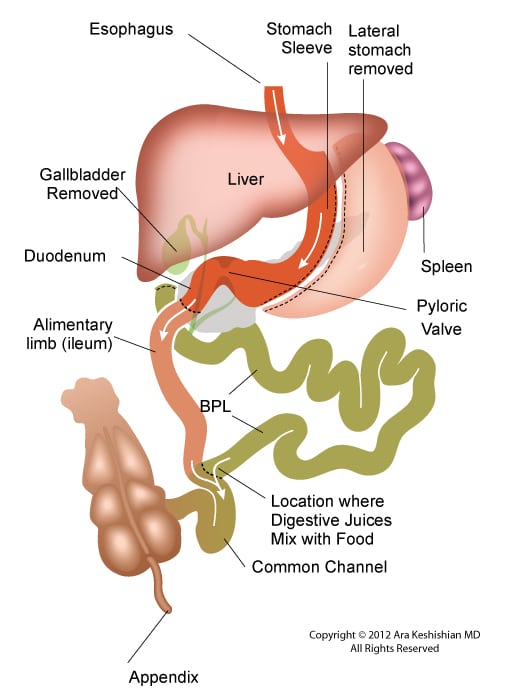
The treatment of Bile reflux is Duodenal Switch without the associated sleeve gastrectomy component in addition to repair of hiatal hernia if present. Ann Surg. 2007 Feb; 245(2): 247–253.
GI Bleed following Weight Loss Surgery
September 17, 2018 10:28 am
Gastrointestinal (GI) Bleed following weight loss surgery is rare but does require knowledge of the particular bariatric surgical procedure the patients has and how to proceed with diagnostics to fully evaluate the situation. Acute or chronic gastrointestinal bleeding can cause anemia in patients. However, Anemia may also be caused by nutritional deficiencies (iron, vitamin , minerals), Kidney disease, bone marrow disease and others. The work-up for anemia following weight loss surgery follows a routine protocol. If there is an evidence of bleeding from intestine (bloody emesis, bloody bowel movement, “tar” like black bowel movements) then the diagnostic work up would include an upper and lower endoscopy.
Endoscopic Procedures:
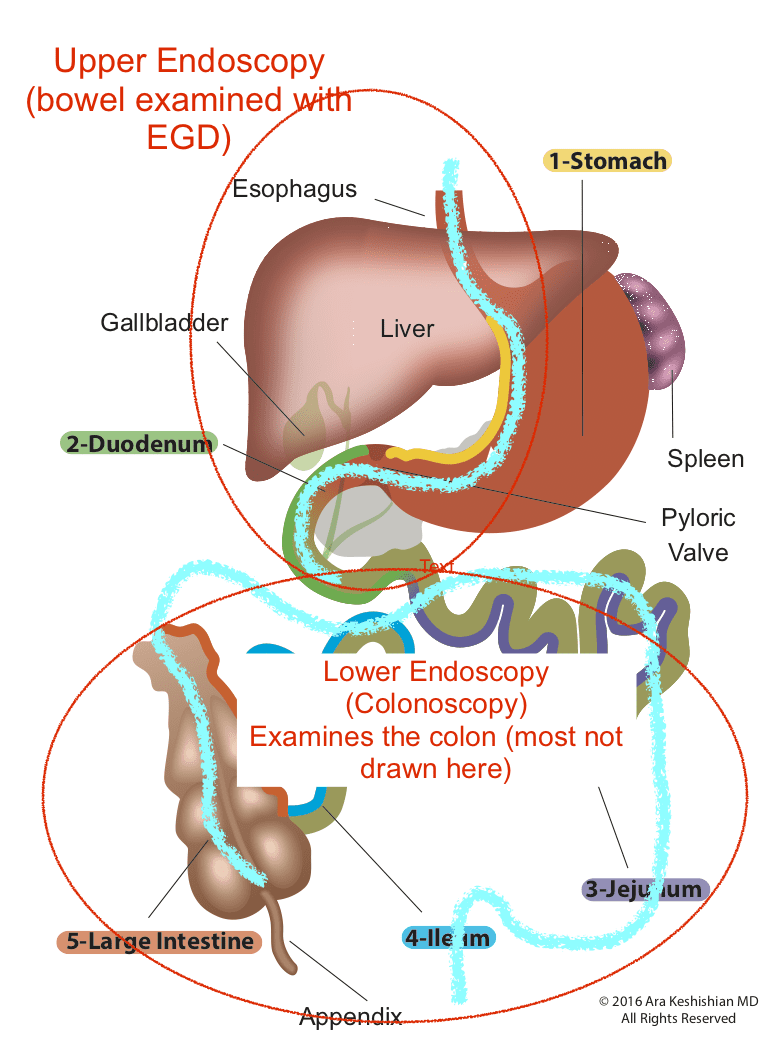
Upper endoscopy Esophagogastroduodenoscopy (EGD): evaluates the esophagus, stomach and a limited area of the duodenum past pyloric valve.
Lower endoscopy Colonoscopy or coloscopy: evaluates the rectus and the entire colon.
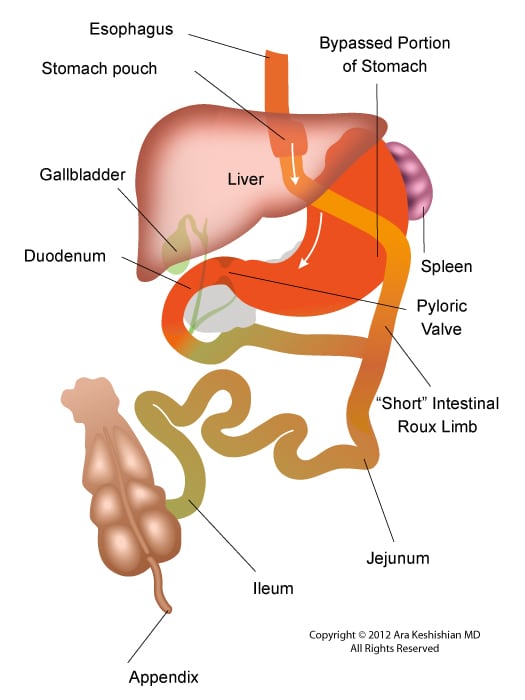
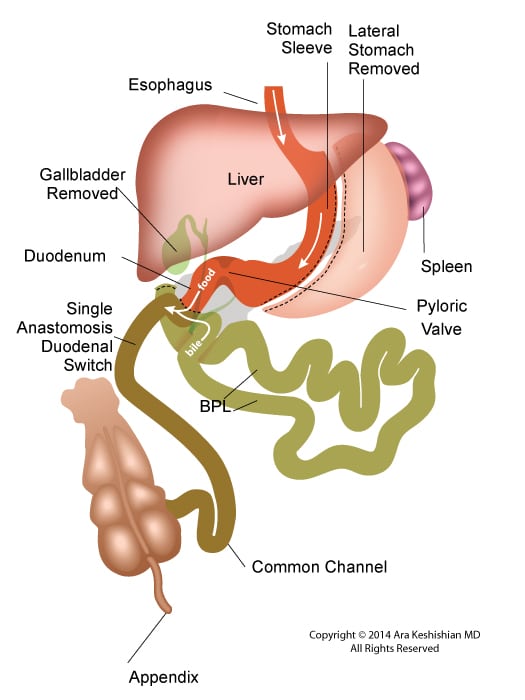
Between these two tests, there is still a considerable amount of the small bowel that is not accessible or visualized with endoscopic procedures. For the small bowel, examination Capsule endoscopy is an option in an intact GI tract. Patients who have had Gastric bypass RNY or the Duodenal Switch, the large segments of the small bowel can not be visualized or examined with capsule endoscopy.
Patients who have had Duodenal Switch, Gastric Bypass and SADI – S would need a tagged red cell scan or CT angiography if GI bleed is suspected in areas of the small intestine that are inaccessible by endoscopic procedures.
Hiatal Hernia Treatment
February 13, 2016 4:45 pm
Hiatal Hernia may be one reason for developing symptoms of GERD (Gastroesophageal reflux disease). As we have discussed previously, the treatment for reflux should not be long-term use of the “purple pill”, or all PPI’s, as advertised on TV. There is a large population who are delaying definitive care and probably increasing their chance of esophageal cancer by taming the symptoms of the reflux with over the counter or prescription medication. However, it is important to note that taming the symptoms isn’t necessarily stopping the effects. Be proactive and request to be sent to a surgeon to fix any issues if you are being recommended to “….take the medication and come back again for another endoscopy again ….”
Types of Hiatal Hernia:
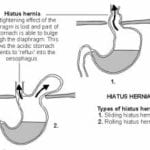
This is an example of a patient who had been told to take the medication and just keep and eye on it with repetitive endoscopies. He had to have hiatal hernia repair with Nissen fundoplication for progressively worsening symptoms even on maximum treatment.
This is another example of a hiatal hernia repair procedure of a patient with a previous history of sleeve gastrectomy. In this patient, mesh had to be placed in order to fix the hiatal hernia.
GERD, Nausea and Vomiting- Don’t ignore it!
April 28, 2015 11:30 am
Gastroesophageal Reflux Disease is a serious matter and should not be left untreated. It is know as heartburn or reflux and if you are experiencing more than twice a week you should be evaluated by a physician to investigate the cause. Listed below are some of the causes and end results of not treating GERD.
Esophagitis – An irritant that can be acid, bile, food and digestive enzymes coming back up the esophagus can cause irritation and swelling in the esophagus. If left untreated, it can damage the lining of the esophagus to the point of erosion and scarring. Bile Reflux may also be a cause of esophagitis and Duodenogastroesphogeal reflux (DGER). Bile Reflux information here.
Esophageal Stricture – Scar tissue can cause the lumen of the esophagus to become smaller and narrow. This stricture makes it difficult or painful to swallow foods. If a stricture is narrow enough food may become stuck and require intervention for removal and treatment. This can also put a person at risk for choking. The treatment includes ballon dilation with an endoscope and in cases where it recurs surgery may be required.
Esophageal Ulceration– If GERD is left untreated it can progress to actual ulcerations in the esophagus. Patients may cough up or vomit blood or see it in their stool as dark tarry or coffee ground type stool.
Gastric Stricture– After weight loss surgery such as sleeve gastrectomy, RNY Gastric Bypass, Duodenal Switch, SADI/Loop, Adjustable Gastric Banding, or other gastric surgeries a narrowing of the inner opening of the stomach can result from scar tissue forming. This will require a surgical procedure to rectify. The symptoms can be food intolerance, full feeling, nausea and/or vomiting. (See pictures below)
Hiatal Hernia– An anatomical weakening or enlargement of the opening of the diaphragm muscle where the esophagus meets the stomach. This defect can allow a portion of the stomach to slide or roll into the chest cavity. This then causes reflux of gastric juice and content. Hiatal Hernia’s can also form on weight loss surgical patients. There are several examples within this blog here.
Breathing Difficulties– The acid aspiration while sleeping can make asthma and other breathing difficulties worst and can cause coughing and other issues.
Dental Issues – The acid, food, digestive enzymes backing up into the esophagus and mouth can cause dental issues such as erosion and tooth decay. In regards to dental issues after weight loss surgery there are also other vitamin and mineral deficiencies that can cause oral health issues. Dental Issues after WLS here.
Lower Quality of Life– GERD can affect a person’s quality of life. If you are in discomfort from acid reflux or having food intolerance it can make life difficult. It can also alter food choices and impact nutrition.
Barrets Esophagus– Pre-cancerous changes in the bottom portion of the esophagus due to long term acid exposure from gastric reflux. Diagnosis requires and endoscopic procedure (EGD) and biopsy.
Esophageal Cancer– There is a significant rise in the western world in esophageal adenocarcinoma. The main risk factors are alcohol use, smoking, untreated GERD, and poor diet.
Reflux and difficulty with swallowing caused by stricture is not normal. These problems are quite frequently encountered as complication of Adjustable gastric banding, with slipped band or a band that is too tight and scarred in placed resulting is belt effect. This results in the esophagus not being able to empty and propel the food down. The end result is significant reflux, with difficulty swallowing, nausea, vomiting etc. Similar problems are seen with Gastric bypass where the anastomosis between the stomach pouch and the small bowel RNY limb is too narrow. In Gastric Sleeve and Duodenal Switch operations, is the sleeve is made too narrow, or misshaped (hour glass, funnel, cork screw) it will result in the patient having reflux and symptoms of stricture. One specific problem with the new operation of SADI is the concern for risk of bile reflux, similar to the BillRoth I procedure.
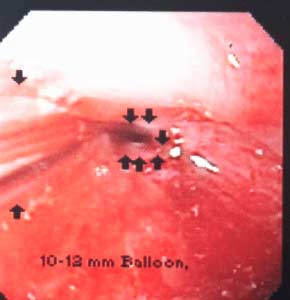
Gastric bypass patient with stricture at the gastro-jejunostomy before and after balloon dilation. Fig A
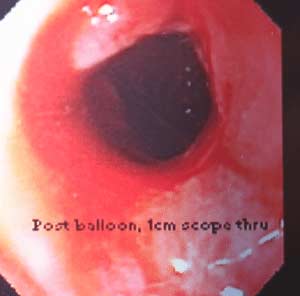
After balloon dilation. Fig B
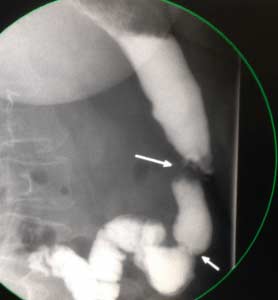
Fig. C : Lap band Patient with stricture where the band as removed at another facility and the scar tissue formed around the GE junction was not taken down. The patient had to be taken back to the operation room after his symptoms persisted even though the band had been removed 3 months prior.
A corkscrew stomach of a Duodenal Switch done at another facility, with the patient presented with persistent reflux, nausea and vomiting for years after surgery. Fig. D
This is not an inclusive discussion of GERD and the treatment. Please see your healthcare providers if you are experiencing any symptoms pertaining to GERD or any other health care issue.
Surgical Treatment of Esophageal Achalasia (Esophageal Motility Issue)
January 23, 2015 6:50 pm
Hiatal Hernia Repair- Reflux and Adjustable Gastric Band Revision
January 14, 2015 3:47 pm
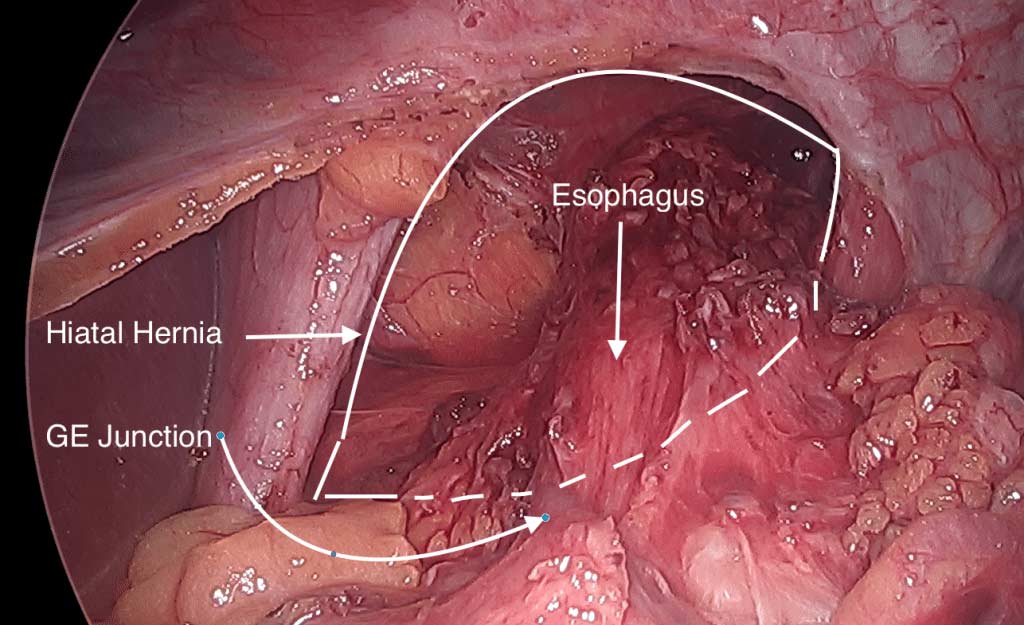
Hiatal Hernia is an anatomical weakening or enlargement of the opening in the diaphragm where the esophagus meets the stomach. The defect can allow a section of stomach to slide or roll into the chest cavity. This causes the reflux of stomach content back to the esophagus. Esophageal Reflux may also be occur without the presences of a Hiatal hernia. It is reported that approximately 60% of people over 50 have a Hiatal hernia with about 9% being symptomatic.
However, over the years we have also noticed a significant increase in reflux disease in patients who have had adjustable gastric band placed. Quite frequently the reflux symptoms after the band is ” blamed” on the patient’s eating habit. Most of the time all studies are reported as “normal” and the complaints are discounted. Other symptoms of Hiatal hernia may or may not include shortness of breath, heart palpitations, or a feeling of food being stuck.
It is important to confirm the presence or absence of a hiatal hernia when considering revision from an adjustable gastric band procedure. Any hiatal hernia identified either before surgery or at the time of the operation will need to be repaired surgically.
With a hiatal hernia repair, the opening is made smaller, and the esophagus, stomach and the junction between them is returned to the proper location to minimize-eliminate reflux.