Category: Lap Band Removal
A patient story: Lap Band complication and Wegovy
October 24, 2024 4:30 pm
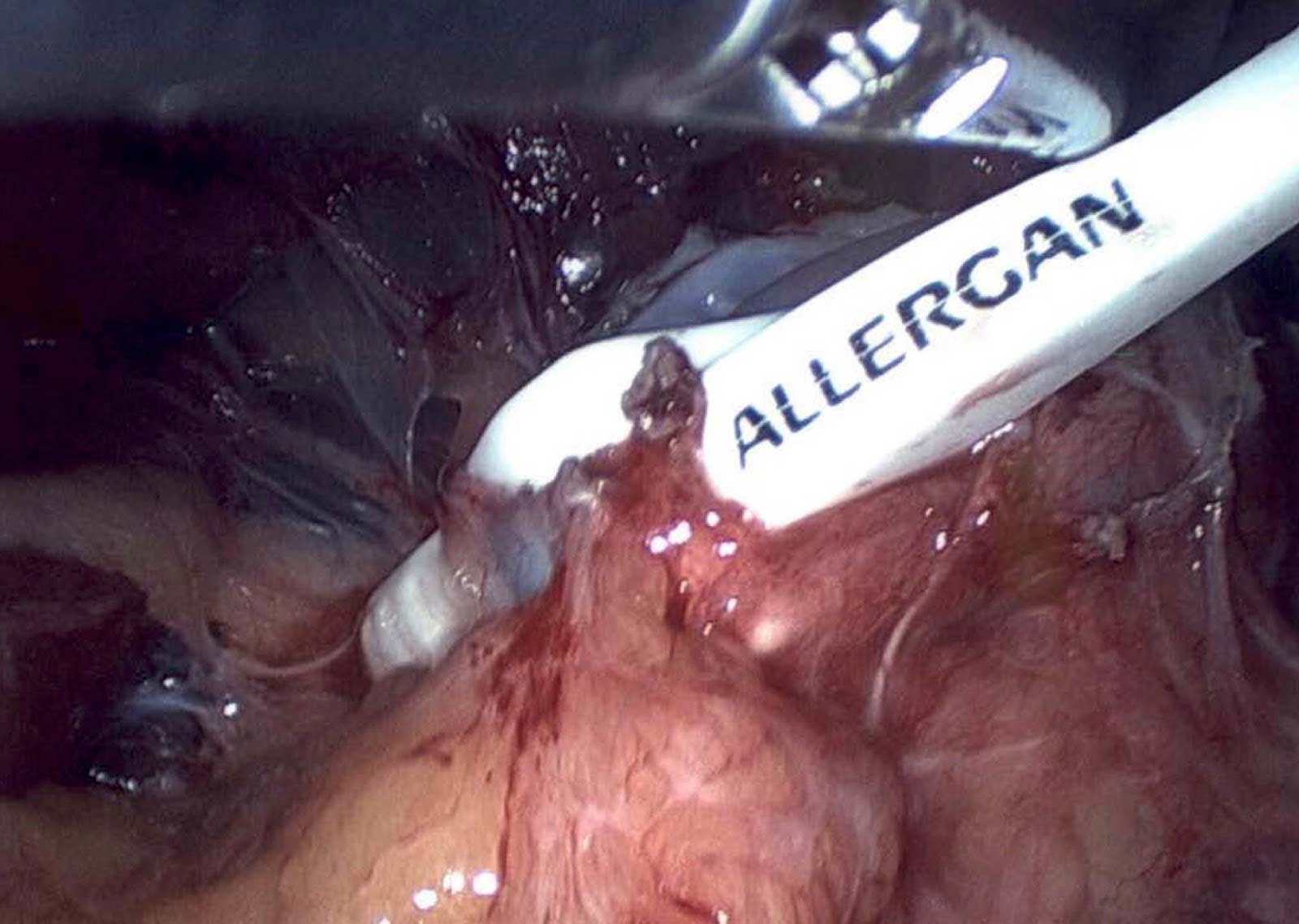
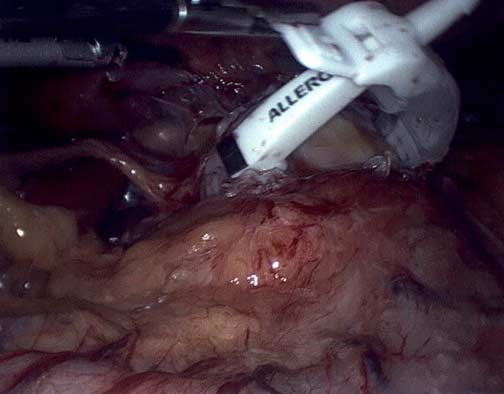
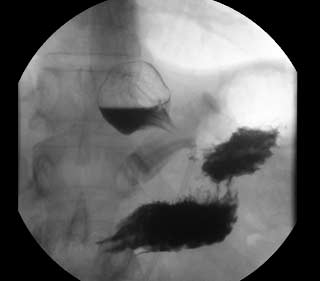
Not too long ago, I saw an old patient who had seen me years ago after having had a lap band placed for weight loss. At the time, I recommended that the lap band be removed and that alternative plans be made. I suspected a slipped band. We discussed the reality that after the band removal, weight gain is to be expected. Several surgical options were discussed, and the patient dismissed them as “too radical.” The patient decided to “deal” with the ongoing nausea and vomiting since it was a small price to pay for the weight loss. I warned the patient that elective removal of the band is much safer than an emergency procedure in the middle of the night when it is least convenient. The patient did end up with an emergency lap band removal and was started on GLP-1 Agonists (Wegovy) because of the weight gain that followed the band removal. The side effects of the medication were debilitating, with nausea, dizziness, and fainting due to low blood sugar. The drug has all been stopped, and most, not all, of the side effects are resolved. The plan is to get this patient in a better shape and, reevaluate the esophagus and the stomach, and formulate a strategy based on the blood work, upper endoscopy, upper GI study findings and decide if the patient will be a good candidate for the Laparoscopic sleeve or the duodenal switch operation.
Here are my recommendations:
- Patients should avoid lap bands. Those with lap bands, regardless of how they feel and whether they are having issues with them, should have the lap band removed immediately before they end up in the emergency room or have irreversible changes to the cells or function of the stomach and esophagus.
- Patients who have the lap band removed will have less weight loss with the sleeve than those who have the sleeve as the primary procedure (the lesson here is that a less invasive, seemingly easy solution is much worse long term; more on this below). Lap Band patients should be revised to the duodenal switch, SPIS, SADI, or Gastric bypass if they have substantial weight to lose.
- GLP-1 agonist medication should be avoided. It is not a solution to the underlying problem but a band-aid covering the metabolic derangement.
- GLP-1 agonist medication needs to be taken long term, and there is no exit strategy– when the patients stop taking the drug, the weight comes back, in addition to the complication associated with it.
- I have also heard that “if it were bad, then the FDA would not approve it.” well, let’s think about it: the FDA approved the Lap band and Phen-Fen, and we all know how these worked out.
- There are no shortcuts, simple injections, or a pill for the complex, multifaceted condition of obesity. Advocating solutions with no long-term outcome, significant complications, and safety concerns is irresponsible.
- A diabetic patient should take the medication LIFELONG to control their blood sugars, including the GLP-1 agonist class of drugs. The concerns are for these medications being used for the treatment of obesity
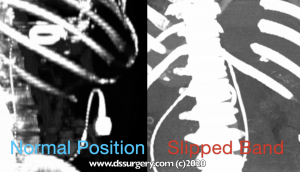
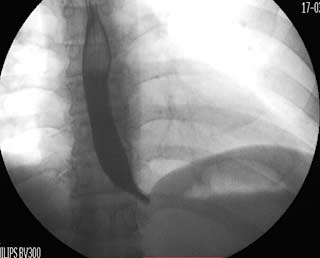
Radiology film of normal position and a slipped LapBand
SUMMARY: Buyers beware- those who choose to embark on the dangerous load of GLP-1 agonist medications should be prepared to deal with the short and long-term complications of the medication and its withdrawal. This is like the problems that are being seen with patients who choose to have a lap band because it was advocated as simple, reversible, and the Phen fen medication for weight loss with the associated cardiac complication.
https://www.dssurgery.com/wp-content/uploads/2024/09/P000008S017b.pdf
https://www.dssurgery.com/wp-content/uploads/2024/09/20-year-all-procdure-metaanalysis.pdf
https://www.dssurgery.com/weight-loss-injection/
https://www.dssurgery.com/glp-1/
https://www.dssurgery.com/weight-loss-medications-compared-to-surgery/
https://www.dssurgery.com/articles/glp-1-agonists-a…agency-clinicians/
https://www.dssurgery.com/articles/managing-the-gas…clinical-practice/Survey
December 16, 2023 9:54 am
Revision from failed AGB to Duodenal Switch
January 10, 2018 2:10 pm
A few times a month during consultation for weight loss surgery , I’m ask as to why I do not offer the adjustable gastric banding as an alternative to the patients. As I have said over the years when a patient considers an weight loss surgery the totality of the risk should be considered. This includes the operative, immediate postoperative course, the maintenance and the follow-ups needed. The potential complications of the procedure in addition to the long-term success off each operation should also be taken into account.
Unfortunately, some patients are led to believe that any perceived benefit in the short operative time and the ease of the adjustable gastric banding also translates to a better outcome. This is in fact the opposite of what the published data have shown, a recent study published in April 2017 by Vinzes et.al, shows that 71% of patient lost their band by 10 years out.
What is also interesting that more patients underwent revision from failed AGB to the duodenal switch than the sleeve gastrectomy (Fig 1.). This is what I also recommend.
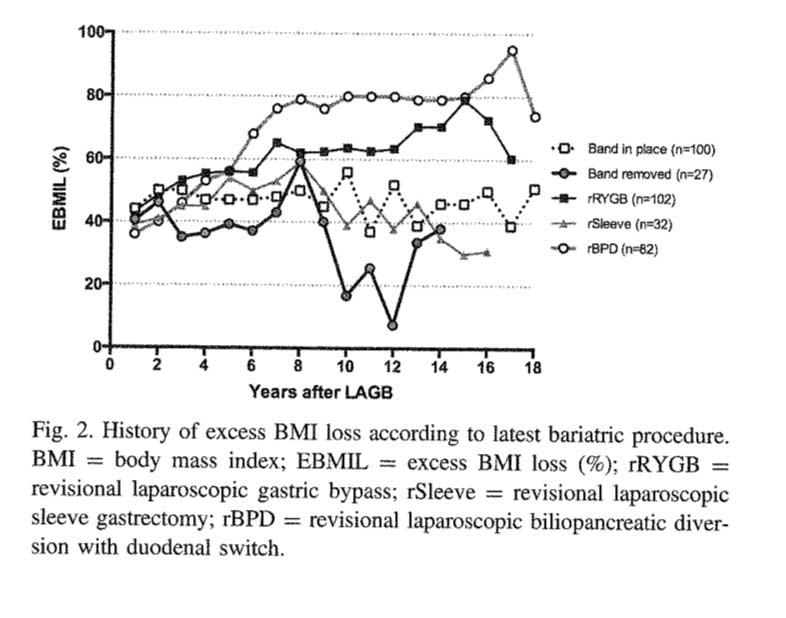
More importantly, The patients who underwent a revision from failed AGB to the duodenal switch operation had the best long term results of all patients (Fig 2.) note the “rBPD” line that is the highest of %EBMIL.
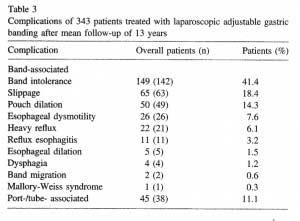
Complication’s were broad and frequent (Table 3.)
Further information on revision from failed AGB to Duodenal Switch or other failed weight loss surgeries can be found here.
Rebanding- A Bad Idea In My Opinion
May 12, 2015 3:42 pm
There is a wide discrepancy of outcomes for patients who have decided to have weight loss surgery and are experiencing different weight loss, regain and complications primary related to their choice of the procedure. In our practice we see quite a few revisions cases on weekly basis. More recently there have been a few “Rebanding” patients seeking revision to the Duodenal Switch.
The typical scenario is of a patient who had an adjustable gastric band placed, and after the initial weight loss (mostly because of the persistent nausea and vomiting) the weight stabilized. The weight loss was never close to a healthy weight and in most cases their co-morbidities did not resolve but now have added complications of reflux and abdominal pain developed. These patients were then recommended to have the band repositioned to resolve a slipped band causing the above complications.
The scientific evidence for rebranding is not justifiable. I think there continues to be an element of denial that the adjustable gastric banding procedures do not work for the vast majority of the people. In fact, AGB in the long term will result in some complications that may not be revisable. The scientific literature shows that there is no benefit to rebranding when it comes to weight loss.
In my opinion when a patient encounters problem with the adjustable gastric band, Duodenal Switch operation represent the best option because it has the best long term outcome of all weight loss surgical procedures.
Erosion of Gastric Band
November 30, 2014 5:03 pm
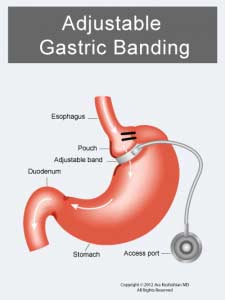
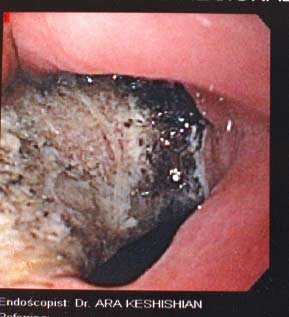
Gastric bands are restrictive rings placed around the top part of the stomach, close to the junction of the esophagus. Their mechanism of action is to create a small tight band to restrict the flow of the food into the stomach. The theory has been that the band will decrease the time food travels down past the narrowing thereby eating less with the end result of weight loss. One of the many complications from the band is erosion of the band into the lumen of the stomach. This results in the patient presenting with nausea, vomiting and some patients develop abdominal accesses. This may present itself with symptoms of abdominal pain, fever, and redness at the port site under the skin.
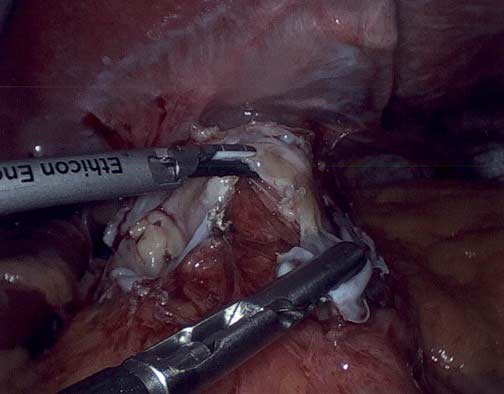
The treatment for this is urgent removal of the band and repair of the erosion/ulceration. Patients who are contemplating a revision to another weight loss surgical procedure are best advised to stage the procedure because of the potential for leak from the repair site. Almost all of these procedures can be done laparoscopically.
Adjustable Gastric Band Easily Reversible?
November 24, 2014 3:25 pm
The Adjustable Gastric Band (AGB) procedures have been advertised as “easily reversible” minimally invasive procedures. A point of interest is why doesn’t anyone ask the question, “Why would a successful device and/or procedure need to be revised or removed?”
The long term success data shows that the AGB procedure is the most inferior of all bariatric procedures. It is important, that when looking at the published data, special attention is given to the definitions in that particular study. An example would be that if a study defines “successful outcomes as weight loss for 30 days!” then all procedure will be successful.
The following is an example of a patient who had the Lap Band (R) a several years ago in another institution. She was seen for surgical follow up with minimal weight loss over a short period of time. She then developed the typical complications of the band, namely the upper abdominal pain, reflux, inability to swallow solids, persistent nausea and vomiting. Her symptoms were all “worked up” and was told that all the studies were normal. All of her symptoms were contributed to her eating habits, even though they persisted after the Lap Band (R) was completely empty.
The patient then presented n our office for a second opinion. After being seen in our office and having a full work up, she had the Lap Band removed and was revised to a Laparoscopic Sleeve Gastrectomy. She had complete resolution of all of her prior presenting symptoms.
Shared Success Story: Krystal U. Had a LapBand to Duodenal Switch Revsion
November 13, 2014 6:23 pm
Another amazing and emotional success story by Krystal Unruh. Krystal we celebrate you and your successful LapBand to Duodenal Switch revision. Thank you for sharing with us all.
Shared Success Story: Patricia Y. Had a LapBand to Duodenal Switch revision
November 04, 2014 3:16 am
Patricia’s success story is truly inspiring and emotional. Please take a moment to celebrate her success by watching video about her journey and revision from LapBand to Duodenal Switch. Thank you Patricia for sharing you journey with us.
“Normal” Lap Band placement!
April 23, 2013 9:39 pm
One of the most common problems that we see are patients who have been told that their band is in correct placement, and yet they are still having nausea, vomiting, reflux etc. These patients are frequently blamed for their symptoms as if properly placed band completely eliminates the problems being associated with the band.
Slipped Band
November 02, 2012 10:40 pm