Tag: obesity
COVID Vaccines
March 05, 2021 3:50 pm
There are no known contraindications from a weight-loss surgical perspective to prevent a post-surgical patient from getting the COVID vaccines.
A patient who has had a Duodenal Switch, Lap Sleeve Gastrectomy, RNY Gastric Bypass, or revisions to Weight Loss Surgery should have the COVID vaccine. The vaccination should be avoided for a few weeks after surgery. For other possible contraindications, please consult your PCP.
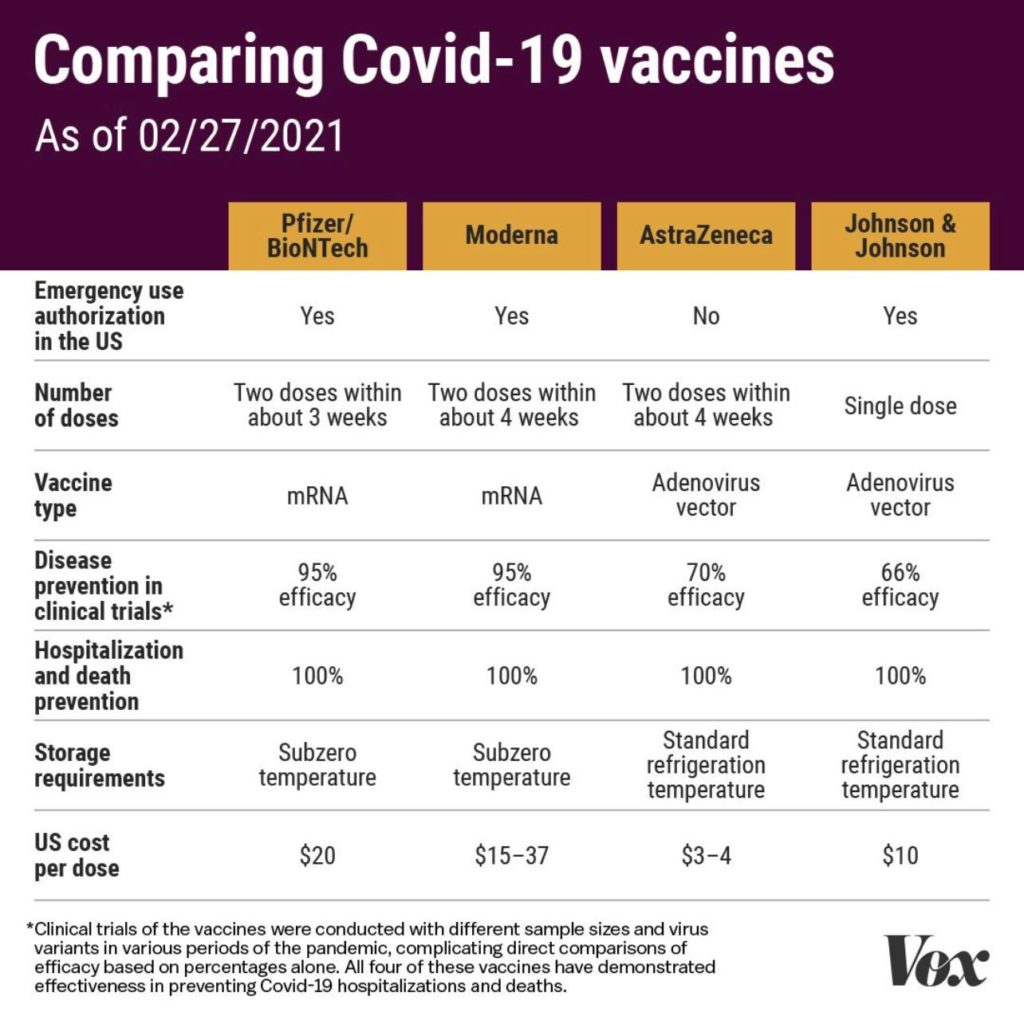
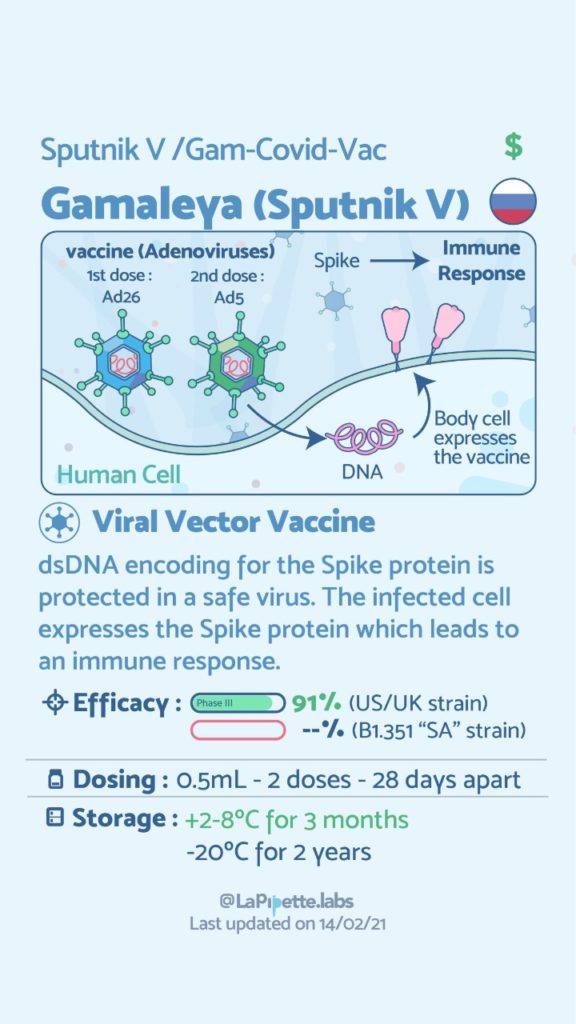
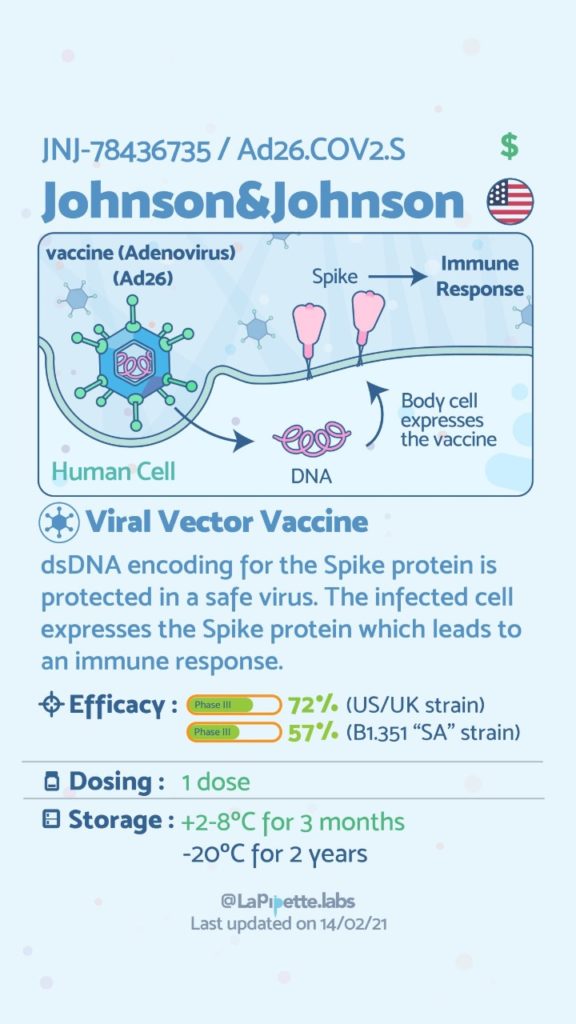
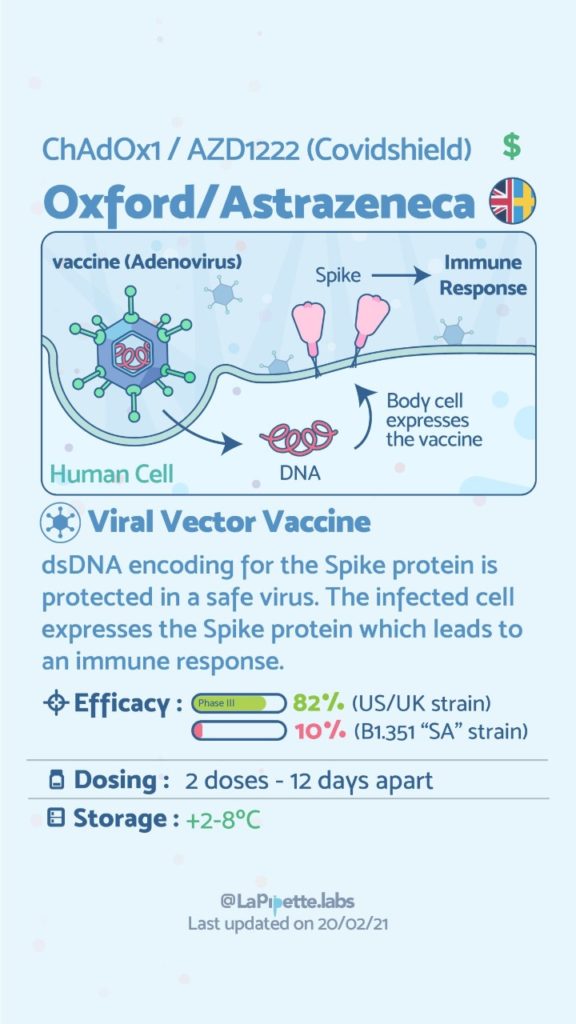
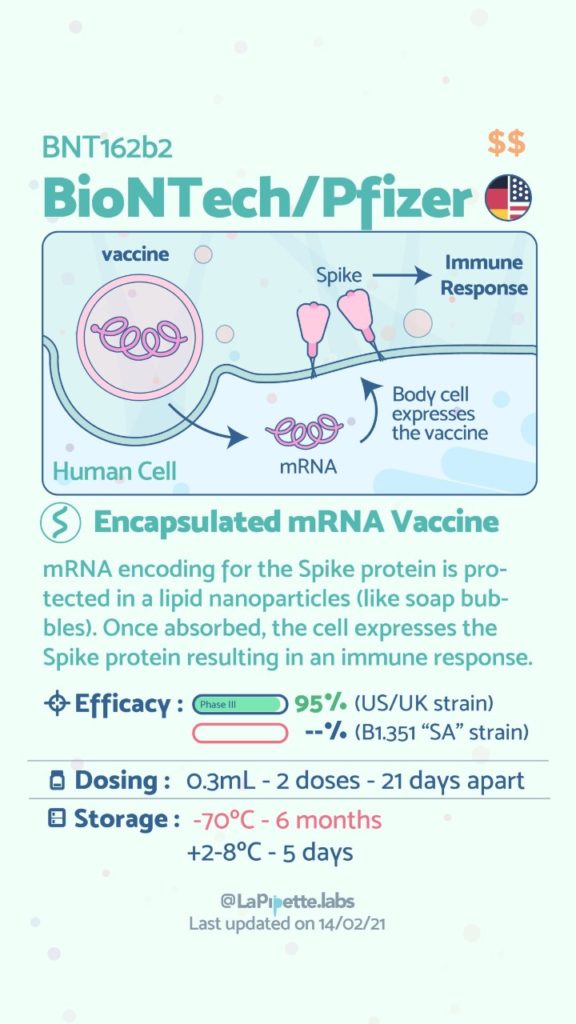
Here is a summary of the vaccines and the details of each one approved as of the publication date.
Added Sugars: Now Listed on the Nutrition Facts Label
December 07, 2020 9:46 pm
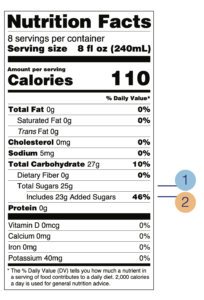
In March 2020, the Federal Food and Drug Administration updated the food labeling requirements. Therefore clarifying the information. This was to simplify and improve the information provided to the consumer.
Articles
March 22, 2020 6:57 pm
Overfed But Undernourished
October 01, 2019 11:27 am
Obesity is related to as many as 400,000 deaths each year in the US and it has increasingly been recognized as a risk factor for several nutrient deficiencies. This may seem surprising given the likelihood of over consumption of calories, however these additional calories are not from nutritious sources. One of the main reason for these nutritional deficits is the greater availability of inexpensive foods that are rich in calories and are nutrient deficient. This has led some medical professional to conclude that there is a certain group of people who are overfed but undernourished. Even with the epidemic of the obesity, there is significant nutritional deficiencies noted.
Obese subjects have increased blood volume, cardiac output, adiposity, lean mass and organ size all of which can influence volume of distribution, in addition, treatment for severe obesity involving surgical procedures can worsen these nutrient deficiencies and in some cases may cause new ones to develop.
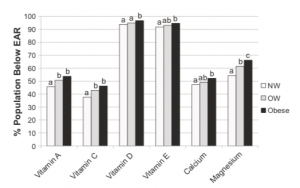
This table shows the percentage of population below the estimated average requirement (EAR) by body weight status in adults more tan 19 years old, showing that almost 90 to 100 percent of people including normal weight (NW) are below the EAR of vitamin D and Vitamin E.
 Nutritional deficiencies in obese patients may promote the development of chronic diseases including increased insulin resistance, pancreatic B-cell disfunction and diabetes, this is because specific micronutrients are involved in glucose metabolic pathways; There are other chronic diseases related to obesity that are being investigated such as decrease in focal grey matter volume and cognitive impairment or inadequate sleep due to low intake of antioxidant vitamins.
Nutritional deficiencies in obese patients may promote the development of chronic diseases including increased insulin resistance, pancreatic B-cell disfunction and diabetes, this is because specific micronutrients are involved in glucose metabolic pathways; There are other chronic diseases related to obesity that are being investigated such as decrease in focal grey matter volume and cognitive impairment or inadequate sleep due to low intake of antioxidant vitamins.
We would like to thank Miguel Rosado, MD for his significant contribution provided for this Blog.
Gastric Balloon
March 12, 2019 9:10 am
Here we go again…. There is a new cure for obesity, Gastric Balloon, with minimal to no risk, is an outpatient procedure and/or can be done in the surgeons office with no anesthesia. Have we not similar claimed like this before (Adjustable gastric band) ?
Randomized sham-controlled trial of the 6-month swallowable gas-filled intragastric balloon system for weight loss published in Surgery for Obesity and Related Diseases 14 (2018) 1876–1889, by Sullivan et. al reports
“Conclusions: Treatment with lifestyle therapy and the 6-month swallowable gas-filled intragastric balloon system was safe and resulted in twice as much weight loss compared with a sham control, with high weight loss maintenance at 48 weeks.”
This sound very promising, however is very vague and leaves out significant, critical, and pertinent information.
The outcome of weight loss at 24 weeks was reported in Total Body weight loss % (TBWL%), Excess weight % (EWL), weight loss, and BMI change. Of those, the last three were statistically significant changes.
The outcome the weight loss was reported to be at 7% TBWL% at 24 weeks with some weight regain, with the patient employing post REMOVAL life style changes. 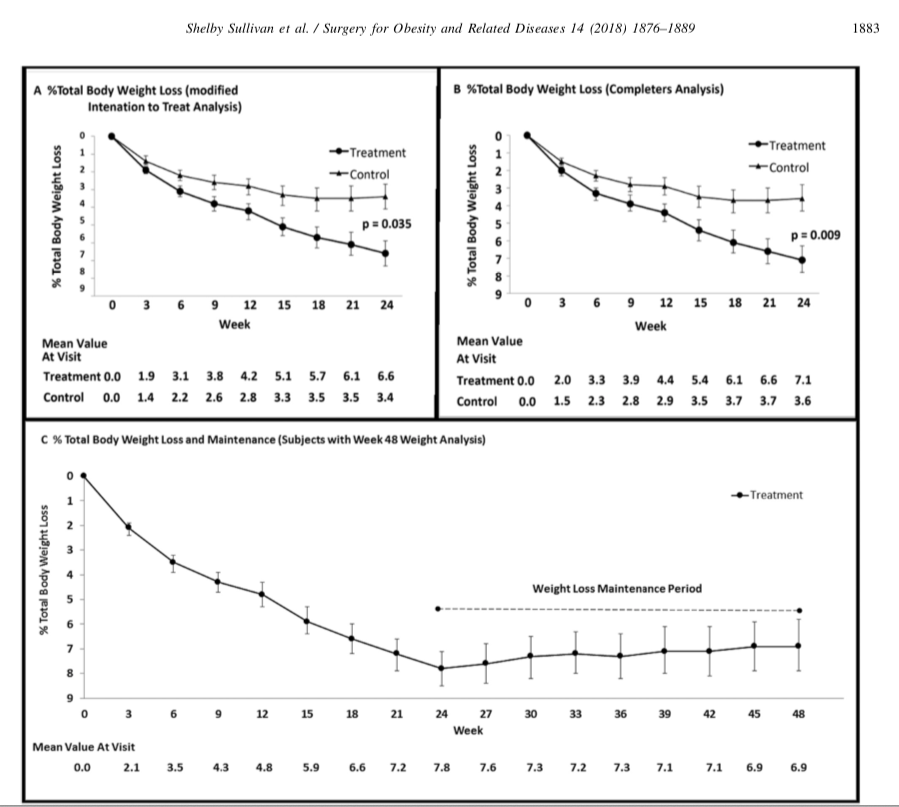
It is stated that the Gastric Balloon is temporary device that needs to be removed in 6 months and should be considered in low BMI patients (<35kg/m2). It is is important for those patients who are considering this temporary expensive measure for minimal weight loss to entertain the alternative of the same temporary results that may be obtained by lifestyle changes. These results may be maintained by a healthy lifestyle, exercise, and eating without the need for a device.
Health Insurances Working Against You
July 09, 2018 12:01 pm
Are Health Insurances working against you? Especially in people who have the disease of obesity? Insurance companies continue to lengthen the pre-operative period. The time that is required to lapse has now in some cases been extended between 6-12 months for some commercial health plans. There are yet again studies that have shown no benefit to the patient with this mandated waiting periods imposed on the patients. Unfortunately, the patients need to challenge the health care insurance companies by the means of all options that may be available to them. This may include internal appeal to external evaluation by some state agency. There are numerous studies that show pre-operative dieting does not equal better weight loss or compliance.
Liver Injury and Obesity
April 30, 2018 11:36 am
Liver is a vital organ. It has many roles in the physiologic pathways including protein productions, clotting function, iron metabolism, production of bile and cholesterol, etc. as well as metabolism and filtering of waste products. We should think of it as a refinery, for conversion of raw material from food to energy used by our body, in addition to a processing and distribution center for mineral, and nutrients. Liver injury can have devistating effects and long term ramifications if unchecked.
Liver is also very resilient and forgiving to stressors and injury. The liver will tolerate repeated insults caused by Medication (both prescription and over the counter) , obesity, Diabetes, alcohol, and herbal supplements, to name a few, but only if care is taken and the offending stressor is removed. During the injury phase, however, the liver may have a difficult time keeping up with bodily function needs due to loss of fully function cells.
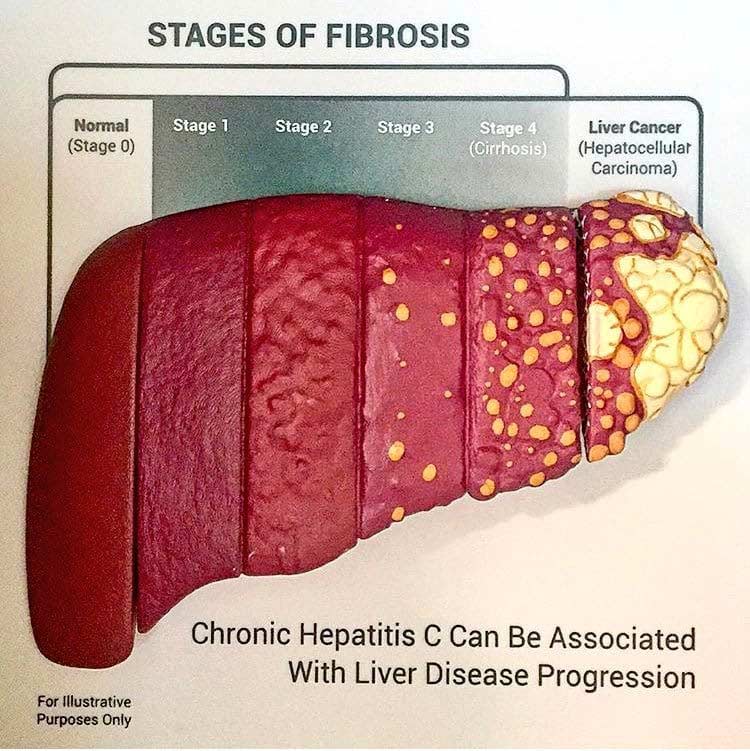
The anatomy of liver can change from normal (both visually to the naked eye and under microscope) to mild inflammation and reverse back to normal if the underlying causes of injury are removed. IF, however, the anatomy of the liver changes with fibrosis, it crosses to an irreversible range where it can only be prevented from progressing rather than reversing.
In the obese population, Non-alcoholic Fatty Liver Disease (NAFLD) causes inflammation and a slowly diminishing functionality of the liver. NAFLD is the leading cause of liver disease in the U.S. Unchecked or untreated NAFLD can progress to NASH (Non-Alcoholic Steatohepatitis. NAFLD, or “fatty” liver disease, is an accumulation of fat within the liver. NASH is a progression that can lead to inflammation of the liver cells or advance to fibrosis and cirrhosis. In addition to liver injury, there is some evidence that NAFLD also correlates with cardiovascular disease.
Causes of NAFLD:
- Obesity
- Type 2 Diabetes Mellitus
- Hypertension
- High cholesterol
- Sedentary lifestyle
Symptoms may include fatigue, right upper quadrant pain, and liver enzyme elevation.
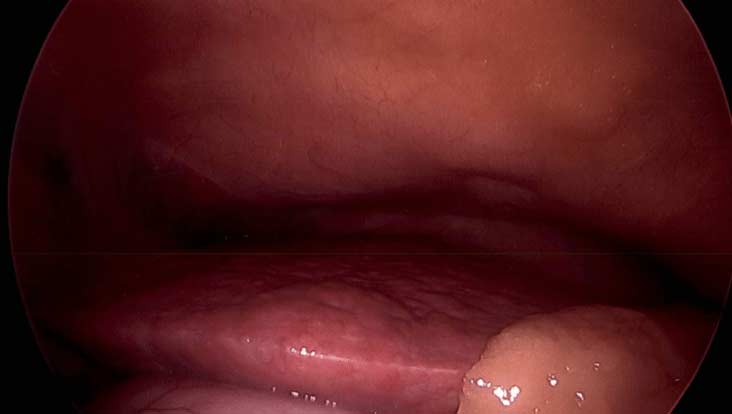
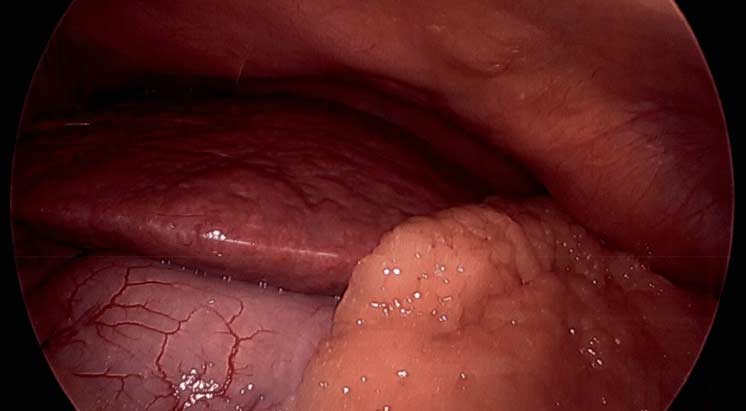
During bariatric or weight loss surgery, we visualize and occasionally biopsy the liver to define the degree of injury, if identified. Following weight loss surgical procedures, a rise in liver function enzymes may be expected due to the processing of waste products following fat mass loss. However, long-term bariatric procedures can significantly improve NAFLD and NASH. Bariatric procedures require adherence to protein and supplement requirements and regular physician visits—the past blog of liver disease.
Weight loss surgical procedures improve liver function abnormalities.
Shared Success Story- Theresa & Rodney (Duodenal Switch)
August 05, 2017 8:41 am
Life before surgery seems like a lifetime ago for both my wife and I. Being extremely overweight is not only a burden on your general health but a burden on your lifestyle in general. You have the awful label of being called obese, or morbidly obese. This is such a wonderful word that makes you feel as if you have been judged a misfit in society. We were both overweight all of our lives and had done all of the diets known on the planet throughout the years. Some worked a little some not at all and we always found ourselves back to where we were before and usually larger than that. The main focus though as we were getting older was our health. For Theresa it was very difficult. Along with being over 400 pounds she had a severe case of asthma which caused her episodes where she felt she was going to suffocate. She also had very little muscle mass which made it very difficult to get up and down from seating or lying positions. Theresa had her surgery in February of 2014 and not a moment too soon. If she had done nothing it is a good chance that she was facing a horribly short future. She also has a slight heart murmur which did not bode well for a person with her weight. She did not have diabetes thank goodness but her A1C was on the rise as was her BP. She did have sleep apnea as well and had to have a CPAP machine.
I was also severely overweight, my highest weight was nearly 400 pounds and on surgery day I was 355 pounds. I was also under the illusion that I had more control over my weight and that once Theresa had her surgery I would just be able to diet and exercise my way to a healthy weight. I was able to do this in my younger years to a certain extent and I was naive enough to think I could continue to do so. How wrong I was. I had found that no matter how much diet and exercise I did my weight would drop a bit at first but then stall and I would have to essentially starve to lose any more and of course that just makes for a bad outcome. My A1C shot up to 7.6 and this was with 1000mg of metformin a day! My BP was very high with both numbers over 100, well over. This is with a high dose of BP meds. I had a severe case of sleep apnea and could not even consider sleeping without a CPAP machine with a high pressure. I have an artificial hip that was being burdened by my 350 pound plus frame and would probably need to be replaced sooner rather than later. My future was not looking good. Dying before I was 60 seemed like a reality for me and that is not the future I was hoping for. The decision to have weight loss surgery for the both of us was tough. You of course hear the nay sayers spout what a cop out it is and it’s the easy way out! You are just weak and just simply need to not eat hamburgers, French fries and donuts. Just stick with non-fat and low calories and you will reach the promised land. What a load of BS.
Once you wrap your head around the fact that your body is wired in such a way that it will always seek a higher weight every time you lose weight, it’s time to consider the type of surgery. Everyone has heard of the Gastric bypass and that seemed to be the path at the time of Theresa’s surgery. The thing about Theresa and what I admire very much is her persistence and her ability to research to the point where a decision is spot on. She looked at all of the four possible surgeries and quickly realized that the Duodenal Switch was a no brainer. It had the greatest measure of success in the long term as well as short term. Reading about the process and talking to others who have had the surgery it became clear that it was the right choice. Finding out where to go and have the surgery was a real challenge. We were lucky to find Dr. Ara Keshishian and have the ability to travel to his location to have the surgery.
Theresa’s Stats Rodney’s Stats
Surgery Weight: 410 Surgery Weight: 355 Pounds
Total Weight Loss: 215 pounds Total Weight Loss: 170 Pounds
Surgery Type: Duodenal Switch Surgery Type: Duodenal Switch
Surgery Date: February 2014 Surgery Data: May 2016
Surgeon: Dr. Ara Keshishian Surgeon: Dr. Ara Keshishian
Life after surgery is an amazing series of challenges, changes, and a journey that transforms your life in a huge way. For Theresa, it was freedom. Freedom from the overbearing weight she was carrying that kept her from essentially moving or doing anything but staying at home. We did very little outside of the house before surgery. Only the necessities of shopping and keeping up the house on the inside and out. Even that was difficult and went by the wayside all too often. Of course eating out was easier than going to the grocery store and that made the scale just go higher. After surgery, Theresa began to lose weight and you could see day by day the changes. After the first month, you could see a dramatic change not only in her look but the fact that she was moving again! She had dropped 35 pounds in that first month and it made a huge difference. As the weight kept coming off over the next few months we began doing things we have not done before. We started to do a lot of walking and a lot more things around the house that needed to be done. Shopping became a breeze and we ate out a lot less. The dramatic change was in her health. A number of changes for the better were happening on that front. The main one and a huge relief was the asthma. It simply was no longer there. She was no longer short on breath and was simply out moving me! I could barely keep up with her. She also had a bad case of psoriasis which before surgery she could do nothing about. Since the surgery it has disappeared. It might be due to the increased in vitamins, particularly the D vitamin. Her sleep apnea went away and now she is healthy and happy. It is almost difficult to describe the changes until you see them for yourself. For Theresa it has been a life changing experience that has transformed the both of us in ways we never imagined. Theresa eats a normal diet and after 3 ½ years post op she fluctuates about 5 pounds either way. It is amazing.
For me it was not what I expected. What I mean by that is, learning to eat is a challenge. With the Duodenal Switch you are not only eating less, but what you eat is tremendously important to the success of the transformation. With the other surgeries, Lap Band, Bypass and Sleeve you do not have the degree of malabsorption. You simply eat less and you lose weight, but you are still essentially “on a diet”. With the Duodenal Switch you have to consider the malabsorption and think protein first and for most. Once you get past the first month of eating small amounts and what you can while your innards heal you need to learn what to eat and is it enough protein. You may also have to contending with the fact that you have an aversion to foods you ate before. I, for one, could not even eat cheese, and chicken. I pretty much lived on scallops, crab, shrimp and protein drinks for the first three months. Nuts were also a good source of the protein when you get to that stage. This does change and things do go back to normal as far as the taste changes, but it takes a few months. The weight in that first month pretty much peeled off. I was dropping like a pound a day. It was incredible. You think that this is going to be a breeze and you will drop it all in no time! Then that 4 week somewhat of a stall occurs. From what I can tell, everyone experiences it in one form or another. It freaks you out because you start to think about the past where you would work your butt off and either gain or drop and ounce or two. But I was lucky, my wife had gone though it two years before me so she was there to explain that it was normal. The whole “this is a journey thing”, and she was right! At the time though I was listening to the negative voice in my head from the past. That is where the support from the many groups come in. You see that pretty much everyone has the same ups and downs and then your body gives up the farm and you drop a bunch of weight in a weeks’ time. There is really a lot of science behind it. Researching and reading about this particular surgery and how it works will benefit you while you go through the process. Another important thing we face with this surgery is the necessity of Vitamins. Thank goodness for my wife and the DS groups and of course my surgeon. You will not be without knowledge if you actively join the different groups and do your research on the vitamins. I am still learning about what my body needs and am looking forward to my labs in the next month to see where I may be deficient. I have also come to realize the importance of drinking water and avoiding dehydration. I never used to drink it much before the Duodenal Switch, but since the surgery I find it aids heavily in the success if you drink it and drink a lot of it.
To conclude this has been a journey and one I wish I could have done a lot sooner in life, but it is never too late. Today Theresa and I are at weights that we are happy with and our bodies are happy with. We are more active then we have ever been before together. No more days idle in front of the television with large amounts of fast food and drinks. That is what we used to look forward too. Now we cannot wait until we go out and do something. We are not running marathons or anything but we are active and enjoy being so. We no longer have the ailments we had before surgery. Theresa’s asthma is practically nonexistent, living in the northwest with fires in the summer she may have a bout or two. Nothing even close to what she has before and a simple inhale and its gone. Both of us no longer need a CPAP! The freedom to simply lay your head on the pillow and sleep is amazing and wonderful. All of the medication we had prescribed for us are gone as well. My A1C was 5 on my last set of labs and 5.3 on the one before that. Theresa’s is the same and has been for three years. BP is normal and my hip is holding steady. Oh, and another cool thing about it is you can actually shop for clothes anywhere! Your sizes will shrink but we have found we have become quite the clothes horses since losing all this weight. It makes it fun to be able to fit into a size you haven’t seen since who knows when.
Life is always a challenge for many reasons but to remove the burden of the weight simplifies things just a bit. It is a decision we will never regret and wished we had made a long time ago. We both owe our lives firstly, to having Duodenal Switch surgery. Secondly, and most important – was in seeking out the best surgeon we could find, and that was without a doubt, Dr. Ara Keshishian. As a surgeon he is thorough, meticulous, constantly learning and keeping up on the latest research;as a person he is easy to talk to, very approachable, and genuinely cares about his patients before, during and after the surgery process. We could not imagine choosing anyone else.
Resistance Exercise BandsExclusive Member Content
July 19, 2017 12:47 pm
Shared Success- Samantha had a Sleeve to Duodenal Switch Revision
July 14, 2017 9:30 am
After struggling with obesity for most of my life I was finally fed up. I had heard about weight loss surgeries before but was always under the common misconception that it was for people who wanted the “easy” way out of a hard situation. I had been working out and reducing calories and tried every popular diet and trainer you could think of. I was still huge and each time I would stop one of these extreme programs I would only end up larger than I was before.
My husband’s cousin had the sleeve surgery and she raved about it. Watching her success is what started to open my mind to surgery, but I was only considering the sleeve gastrectomy. I went to a center in another state that offers Duodenal switch, lapband, RNY and the sleeve. The surgeon I met with strongly suggested RNY to me, but I was stuck on the sleeve. I didn’t want my intestines touched period. I had the sleeve surgery on October 9, 2013.
My high weight was 402 lbs and I weighed 343 on the day of my sleeve surgery. I actually did well with the sleeve and was able to get down to 218 as my lowest. However it was still much like dieting. It was so stressful. After a while my body wouldn’t drop the weight regardless of how little I ate and exercised. I was eating 800-1200 calories a day and low fat meals and working out and kept slowly gaining weight. I was frustrated and honestly I gave up. My reflux wouldn’t go away so I visited a bariatric surgeon in my area who suggested that we essentially re-do the sleeve surgery to make my sleeve small again so that I would eat less and lose weight again. I got a second opinion and that surgeon suggested I revise to RNY. I went to obesity help’s website to explain my situation and a lot of people with much more experience than me HIGHLY urged me to see Dr Keshishian before making a decision. He was said to be an expert in revision weight loss surgery. I almost cancelled my appointment and didn’t have hope with this doctor either, but since I was in a dead end I went anyway. Dr Keshishian told me it wasn’t my fault. WHAT!? I had never heard that before. I usually get the shame from doctors who assume I must not be trying or that I am secretly eating something wrong. He ordered tests and told me it was “simply science” and I just LOVED him! I had a stricture in my Sleeve that needed to be repaired so since I needed surgery anyway I decided to go ahead and revise to a surgery that has the highest success rate, Duodenal Switch.
I was so scared of my intestines being cut and Dr. Keshishian eased my fears. I wish I had went that route the first time but then I might not appreciate it like I do now. Duodenal switch is the ONLY surgery I would recommend to anyone. As Dr K says it’s simple numbers. It’s the surgery with the highest percent of excess weight lost and kept off. I was 252 before my revision from Sleeve to Duodenal Switch and I am just at a year out and today I weigh in the low 190’s and I am still losing. Dr K’s goal for me was about 180. My goal is about 175. I eat more fat now than I ever did even when I was 400 lbs. I enjoy what I eat and I enjoy exercising and most of all I get to enjoy seeing results from my hard work. Food no longer causes me stress and anxiety. I know with 100% certainty that I made the right decision. Thank you Dr. K for your great skill and I don’t mean just with the knife but with the way you are able to make a high anxiety situation seem like no big deal.


 Added-Sugars-New-Nutrition-Facts-Label_1
Added-Sugars-New-Nutrition-Facts-Label_1