Category: Revision of RNY
Zoom Group Meeting
September 21, 2020 7:10 am
We are excited to announce we will be having a Zoom group meeting Tuesday, September 22, 2020 at 7:00 PM PST. We hope to see you online!
Registration is required. Please follow the link to the meeting registration.
Protein Sources
May 16, 2019 10:26 am
Not all proteins are created equally. The protein that we digest serves as the source of the essential amino acids, (the building blocks which make up a protein). The essential amino acids can not be made in out body. Protein sources can be animal or plant based. We’ve written a in-depth explanation of protein sources in this previous blog: Protein Optimization
The proteins can also be decided into two categories:
1-High quality or Complete proteins
Complete proteins contain all the indispensable amino acids that we need. Animal based proteins for the most part are complete proteins. These include cheese, mean, fish, mild, yogurt, egg and poetry.
2-Low quality or Incomplete proteins
Incomplete protein are mostly plant based proteins. In most cases, the incomplete proteins either lack or have insufficient about of the one or a number of amino acids to be able to satisfy our nutritional requirements.
This is why we general recommend animal based proteins.
Following weight loss surgery there are some guidelines that can be helpful in our previous blog: Importance of Protein.
Dr. Facebook
March 22, 2019 8:24 am
We have become reliant on the information that we obtain from the internet, specifically platforms such as Facebook. In our practice we have to continuously correct information that patients have obtained from other patients, unmonitored sites, blogs, and postings. Most of this information is based on individual experiences that has become gospel. “Fat is good for you” is one of them. To clarify, some health fat (olive oil, avocado, Omega 3) is healthy and needed for all patients. We do not recommend “fat bombs” as a part of ones daily dietary intake.
The following article was written on the accuracy of nutritional posts in support groups on Facebook.
Koalall et. all in SAORD, December 2018 Volume 14, Issue 12, Pages 1897–1902 published
“Content and accuracy of nutrition-related posts in bariatric surgery Facebook support groups”
The conclusion, as suspected, that “Over half of the posts contained inaccurate content or information that was too ambiguous to determine accuracy..:”

It is our recommendation before any dietary recommendations are taken from facebook and the like, the source of the information should be verified. As I have stated in the past, a frequent flier passenger is probably not qualified to fly a
commercial airplane, any more than a previous weight loss surgical patient providing medical and nutritional advice. We realize that there is significant value to the forum for exchange of information and sharing of experiences with other weight loss surgical patients as long as the information is well sourced and verified.

Cholecystectomy-Gallbladder Removal
September 10, 2018 9:44 am
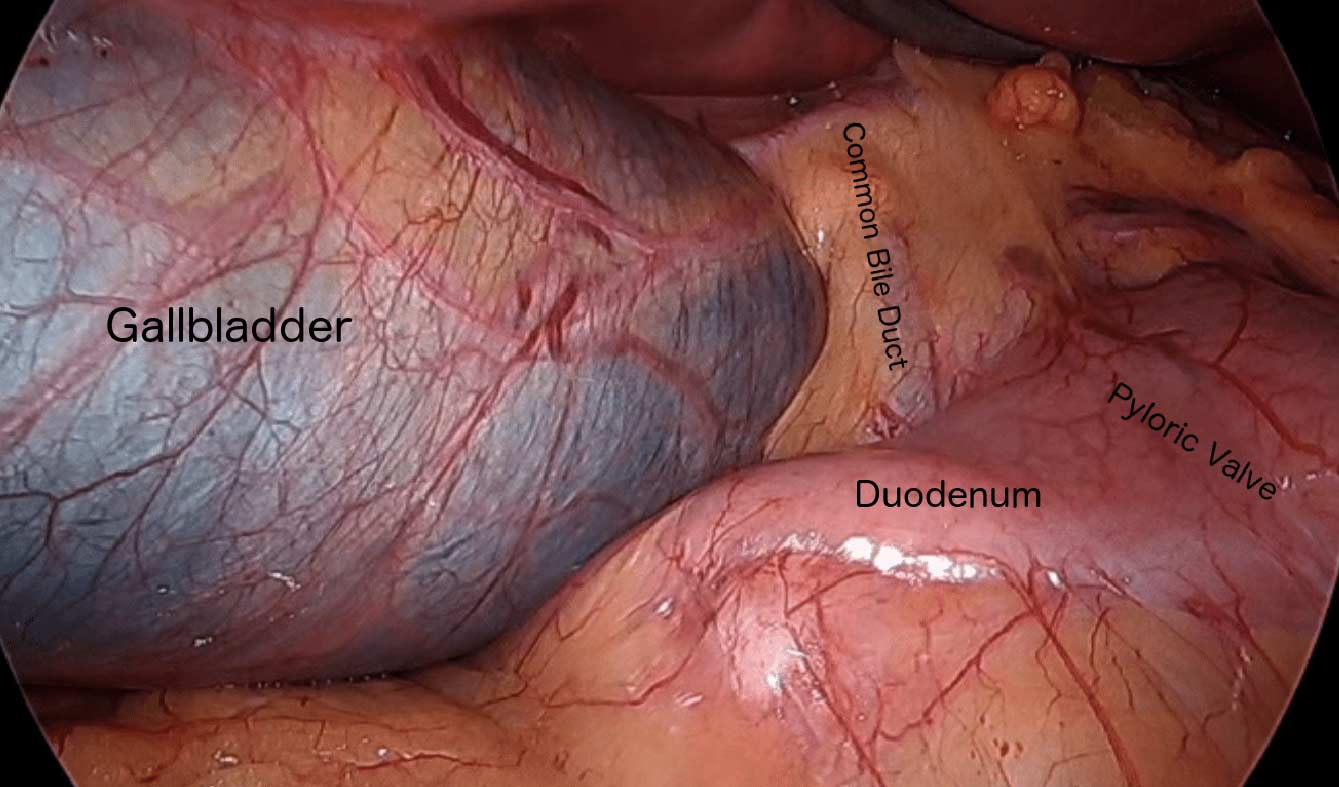
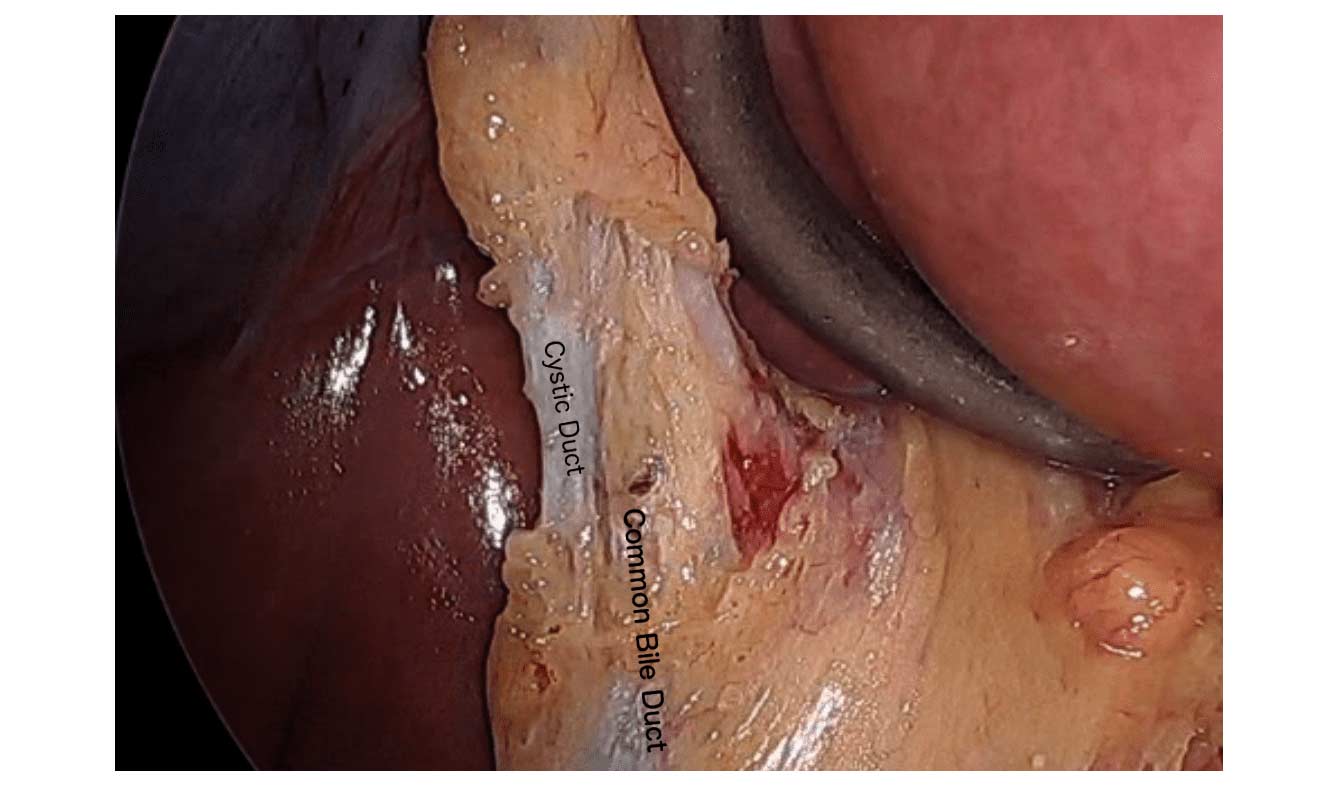
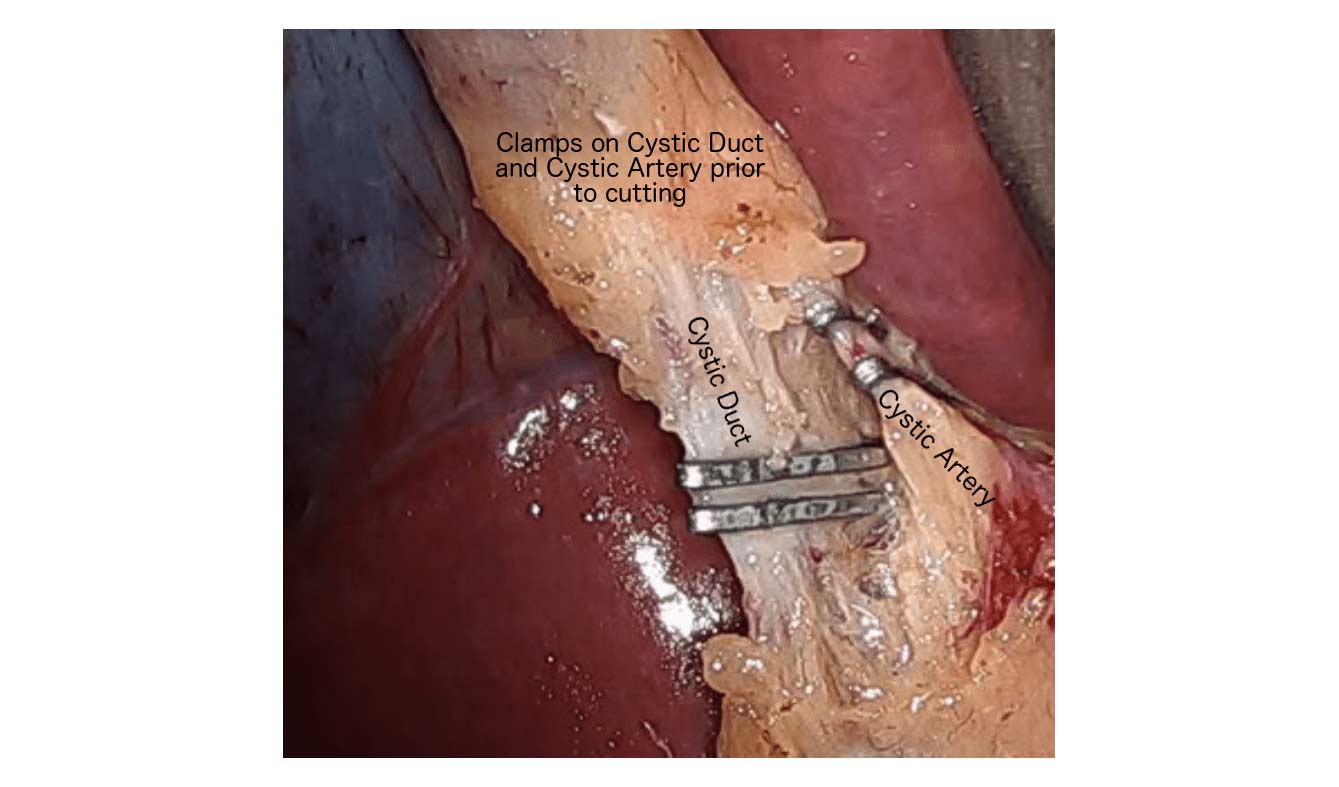
There are differing opinions, based on a broad set of scientific publication, wether or not gallbladder should be removed at the time of weight loss surgery. Obviously, Cholecystectomy is a stand alone general surgical procedure that is often performed due to gallstones and/or gallbladder disease with a variety of symptoms. However, the focus of this blog will deal with Bariatric Surgery and Cholecystectomy.
Rapid weight loss can increase a patients chance of forming gallstones. This rapid weight loss can be as little as 3-5 pounds per week. Weight loss surgery can increase your risk for gallstone formation. Several of the common thought processes the mechanism of this is, obesity may be linked to higher cholesterol in the bile, larger gallbladders, high fat diet and larger abdominal girth.
When a patient is having the Duodenal Switch (DS) Bariatric operation, or having a revision of a failed gastric bypass to the DS, I always remove the gallbladder. This is because there isn’t an anatomical route to utilize endoscopic procedure for an ERCP should the need rise.
In the case of a patient undergoing Vertical Sleeve Gastrectomy, if there are any indications or complaints of abdominal pain then an ultrasound is done. If there are findings of gallstones or other disease of the gallbladder, then a cholecystectomy is performed at the same time as the Sleeve Gastrectomy.
In my opinion, every patient having the Gastric Bypass (RNY) should also have the gallbladder removed because of the anatomical limitations after surgery that prevents the use of ERCP if needed. Some clinicians will place the patient on a long term medications to reduce the chance of gladstone formation after surgery, which themselves have side effects limiting the compliance in most patients.
Further information on Common Bile Duct Dilatation and ERCP
PolyCystic Ovarian Syndrome PCOS
September 04, 2018 9:58 am
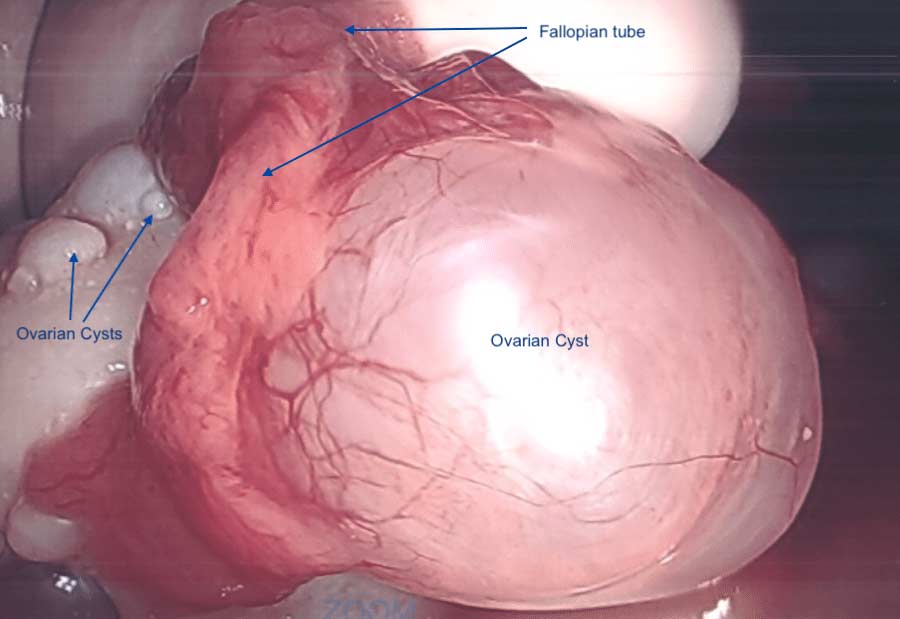
PolyCystic Ovarian Syndrome PCOS is a complex condition. The exact cause of PCOS is unknown however, it involves hormones imbalance and multiple ovarian cysts, irregular menses, and infertility. In some cases, PCOS can be compounded by diabetes, hypertension and other metabolic conditions. PCOS has been shown to effect approximately 10% of women of childbearing age with symptoms of menstrual abnormalities, poly cystic ovaries, and excess androgen (male sex hormone). PCOS should be diagnosed by ensuring there are no other underlying endocrine issues. There are several associated disease processes that seem to be related to PCOS. These related disease processes are Type 2 Diabetes, higher depression and anxiety, increased cardiovascular risks, stroke, hyperlipidemia, sleep apnea, overall inflammation, and endometrial cancer.
Anatomically, numerous cysts are found on the ovaries. These are usually diagnosed by ultrasound, blood levels of hormones, and symptoms described above.
Bariatric Surgery and PolyCystic Ovarian Syndrome PCOS
Bariatric Surgery can improve PCOS in those individuals with Type 2 Diabetes Mellitus. Further information on weight loss surgery and its effect on PCOS here.
Parathyroid Scan
July 09, 2018 11:48 am
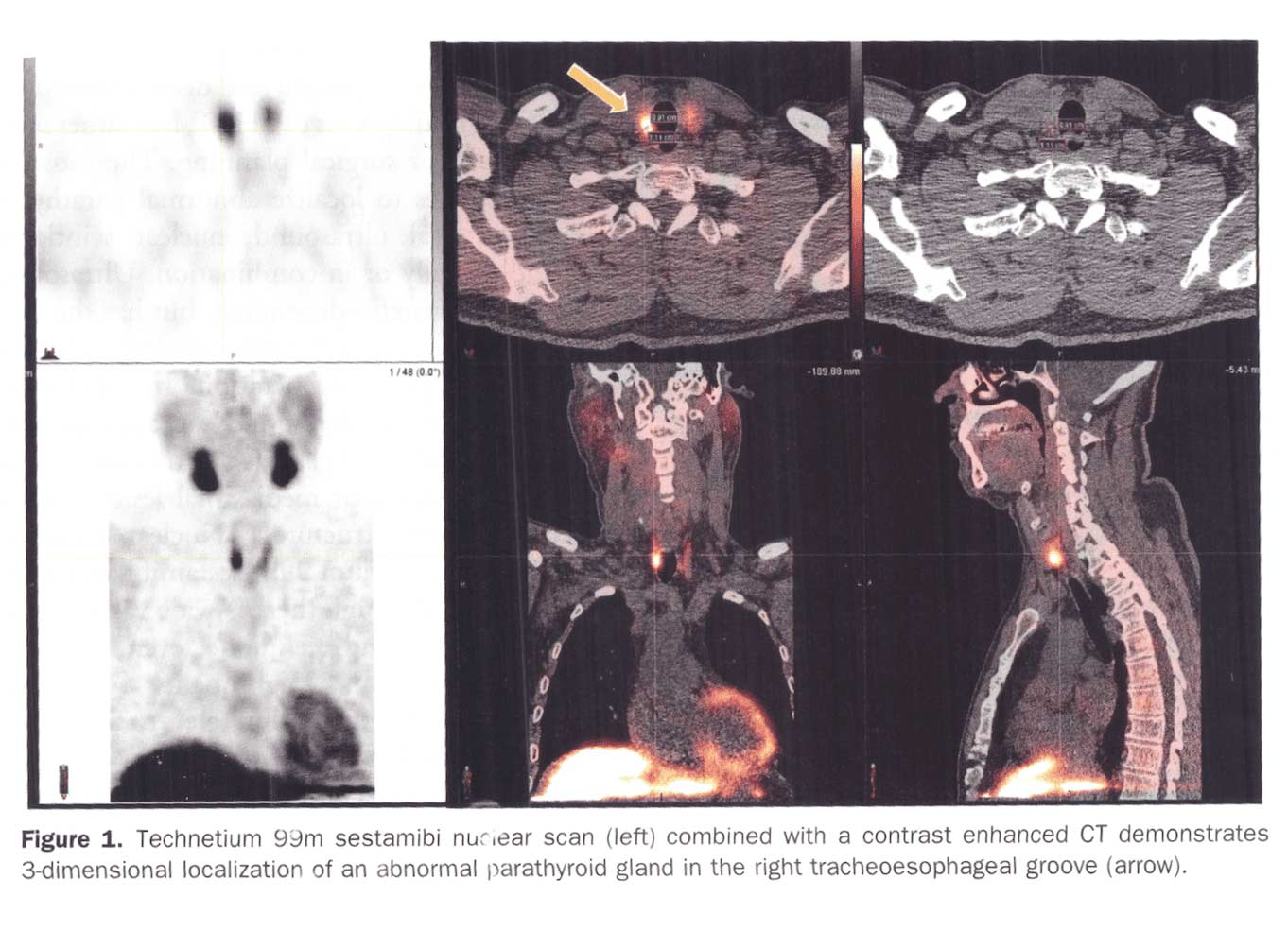
A Parathyroid scan or Sestamibi scan may be needed if the typical weight loss surgical reasons for elevated PTH levels have been addressed. Sestamibi is a small protein which is labeled with the radio-pharmaceutical technetium-99. This very mild and safe radioactive agent is injected into the veins of a patient with overactive parathyroid and is absorbed by the overactive parathyroid gland. If the parathyroid is normal it will not absorb the agent. The scan below shows the uptake of the agent.
Calcium, Vitamin D and Parathyroid hormone are routinely measured on yearly follow up for most post weight loss surgical (WLS) patients. Elevated parathyroid hormone (PTH) may be caused by Vitamin D deficiency or calcium deficiency (most common in post WLS) or by over active parathyroid gland(s). In the latter case, if one of the four glands is overactive then this is knows as a parathyroid Adenoma. If all 4 are over active and are secreting too much PTH, this is known as hyperplasia. Ultrasound of the neck, may identify an enraged parathyroid gland (adenoma) which is located behind the thyroid gland. Given the large area where the parathyroid gland may be located, additional tests are needed to not only identify the location of the gland(s) but also to distinguish between single gland (adenoma) or multiple glands (hyperplasia) cause for the elevated PTH. It is important to investigate all avenues and testing in parathyroid hormone elevation and in some cases, not to rely on one test for your diagnosis. It is also imperative that weight loss surgical patients take their supplements routinely and consistently and have their laboratory studies followed at least yearly.
Candy Cane Gastric Bypass – RNY
June 21, 2018 1:05 pm
One of the findings following Gastric Bypass is a Candy Cane Gastric Bypass. Nausea and vomiting , upper abdominal pain is a common complaint of patient who have had the Gastric Bypass RNY operation. This is in addition to the high incidence of patients who experience the complications of weight regain and or dumping syndrome.
Quite frequently the symptoms of nausea, vomiting and upper abdominal pain of a patient with history of gastric bypass is evaluated by a primary care, referred to a gastroenterologist. The “routine” work up recommended is X-ray of the abdomen, maybe contrast study (Ct scan or upper GI) and for sure and upper endoscopy. The result quite frequently reported as “…nothing wrong”.
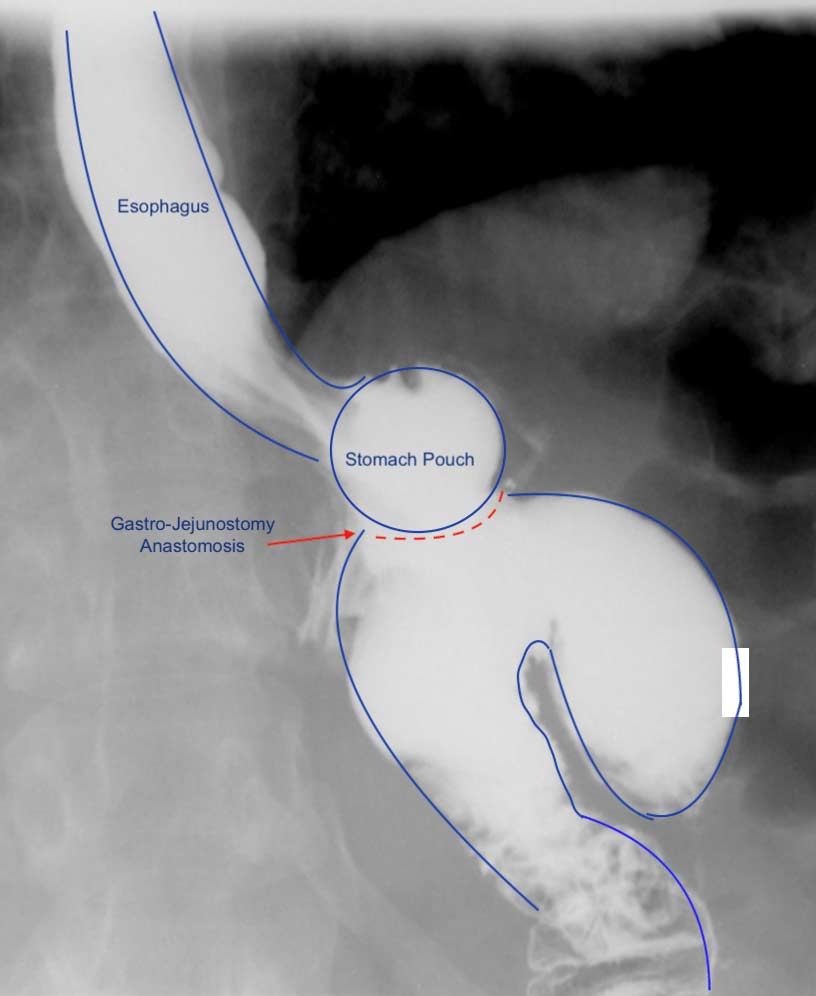
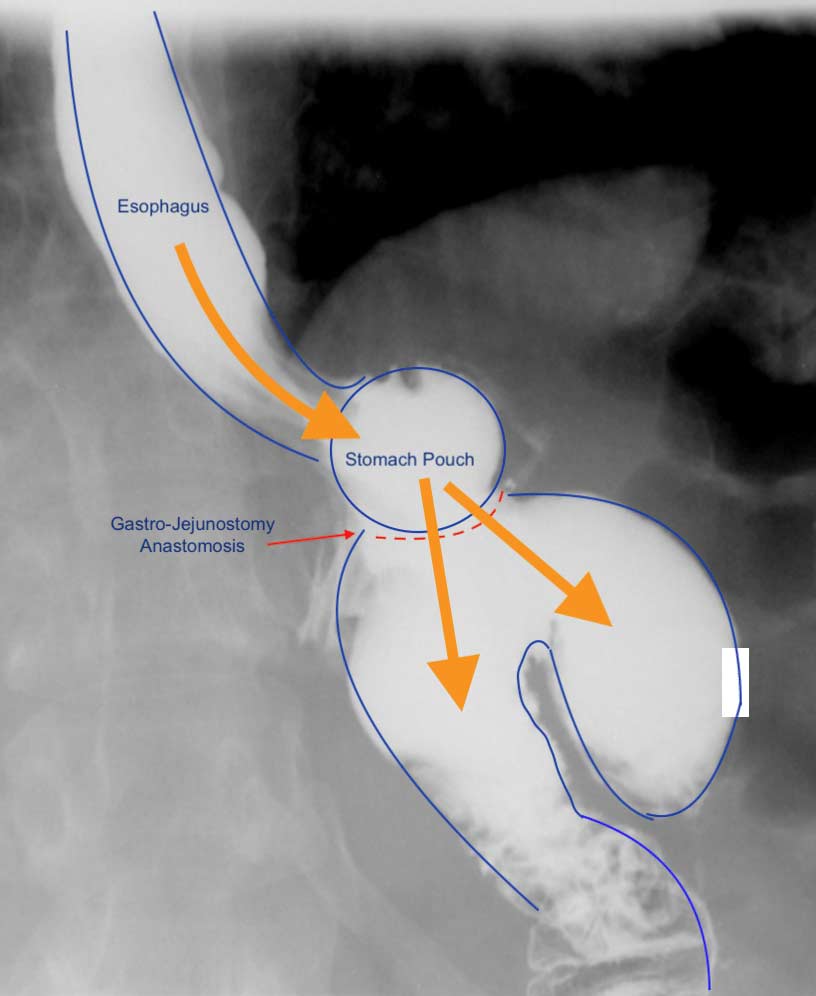
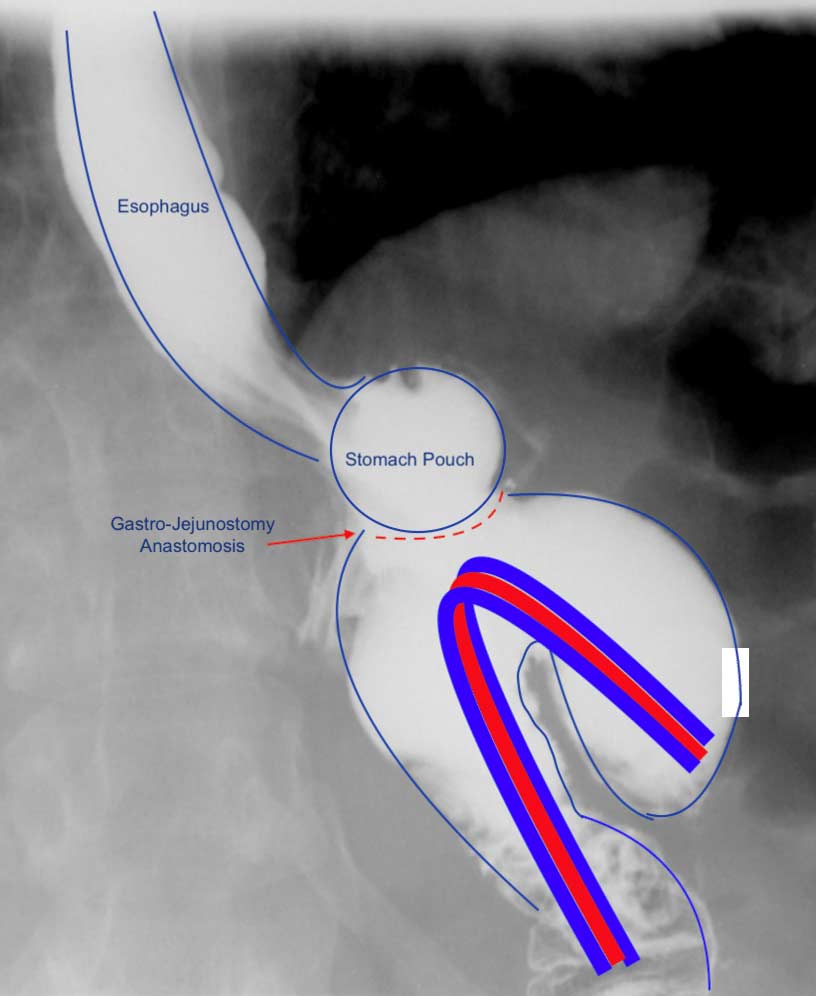
A typical upper GI in a Candy Cane Gastric Bypass situation may look like this:
A common and underreported problem may be a Candy Cane finding. The “blind” end of the small bowel anastomosis is too long and this results in food settling in the hook of the candy cane. The symptoms of the nausea, vomiting and upper abdominal pain may be from the residual food and liquids that do not drain from this area.
Candy Cane Gastric Bypass finding
Candy Cane Gastric Bypass cases will require surgical intervention to shorten the length of the blind segment of the small bowel to improve symptoms.
It is my recommendations that any patient with history of weight loss surgery who is having any persistent gastrointestinal symptoms be evaluated by weight loss surgeon.
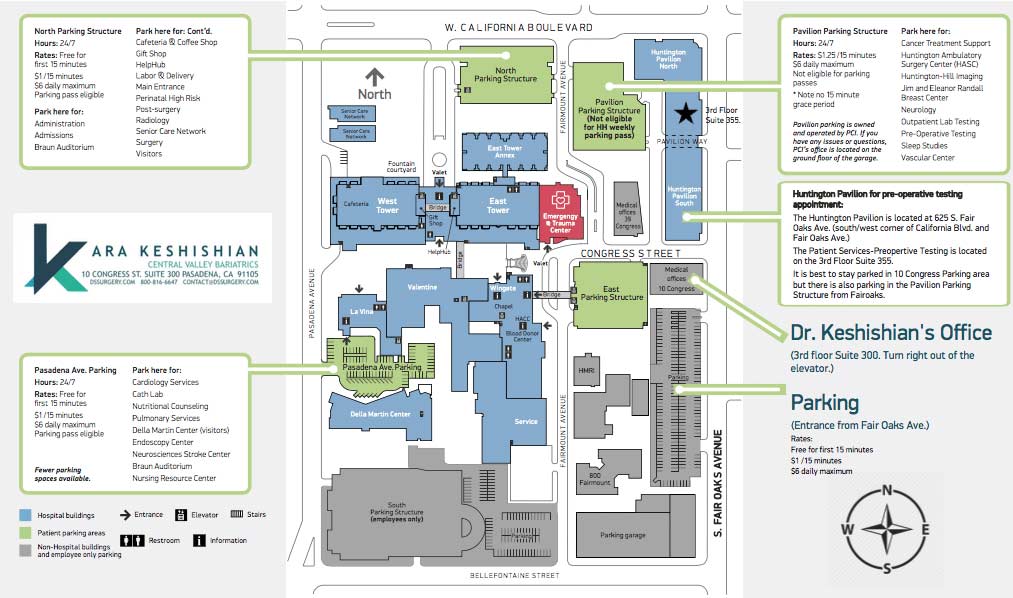
New Pasadena Office Map and Parking
August 12, 2017 8:35 am
We’ve created a helpful map and parking diagram for our new Pasadena, CA office location. It also has a general layout of the Huntington Memorial Hospital Campus and Pre-operative intake and testing area. We hope that you find it helpful on your next visit to see Dr. Ara Keshishian, General and Bariatric Surgeon.
Dr. Ara Keshishian has performed more than 2,000 Duodenal Switch procedures, thousands of Sleeve Gastrectomies and more than 500 revisions from other Weight Loss Surgeries such as RNY Gastric Bypass, Adjustable Gastric Band, and Sleeve Gastrectomy to Duodenal Switch as well as General Surgical cases over the last 18 years of private practice.
Insurance Appeals And Denials
August 07, 2017 7:08 am
Whenever you are dealing with insurance issues it is important to have a general understanding of insurance ins and outs. The Obesity Action Coalition has a good general guide to the insurance process here. If you are having issues with out of network, out of area, or insurance appeals and denials for Duodenal Switch, there may be some additional assistance from two individuals who have had the Duodenal Switch procedure themselves. We are grateful that they have provided assistance throughout the years to the Duodenal Switch community. The following is their statement on insurance.
The majority of insurance companies are in the business of making money (for profit). They can deny requests for preauthorization with impunity. These denials are often complexly worded and difficult to comply with and overcome, and are definitely overwhelming to the patient, and the busy surgeon’s office. The vast majority of patients faced with demanding if not impossible to achieve prerequisites, or denial of the request for preauthorization simply give up, and the insurance companies pocket the savings.
If you find yourself facing impossible pre-op hurdles, or a denial, we urge you to appeal, and to seek assistance in preparing the appeal. You can hire an attorney, of course, but there is an informal and free resource we suggest that you investigate as well.
If you go to BariatricFacts.org (a non-profit, patient-run site), you will find individuals who are long-term DS postops, and patient advocates. They have been helping patients, pro bono (for free), for over 10 years. They will help you draft your appeal letters, provide supporting medical and legal documentation, and prepare draft letters of medical necessity to be reviewed and signed by your surgeon supporting your appeal. They will not represent you directly, but they will help you best represent yourself. in many cases it is necessary to exhaust all internal appeals (because the insurance companies are unlikely to overrule themselves), and then file for external review, where independent reviewers often overrule improper denials. If you join and then post on BariatricFacts.org asking for help, you will be connected with them and you can decide if you want their help.
Please note that this is just a suggestion. It is neither legal nor medical advice, nor a guaranty regarding their services, and you should always consider getting legal advice and assistance from an attorney who will represent you directly. The members at BariatricsFacts.org will help you draft your own letters, but will not be your legal or medical representatives; you will be required to do a fair amount of your own work on your appeals, and to sign them yourself.
It is suggested that before or at the same time as you contact the resources suggested at the site, you gather as much of the following information as you can:
- A copy of your Evidence of Coverage, which is the usually 100+ page insurance contract between your employer and the insurance company, which you can obtain it from your HR department. If you are self-insured, it will be available directly from your insurance company. Note: it is NOT the Summary of Benefits – it needs to be the contract itself.
- If your insurance is through an employer, you need to determine whether your plan is self-funded or fully-funded. Your rights are significantly different under the two types of plans.
- If your insurance company has a separate bariatric surgery policy, provide a copy of that, too.
- A copy of your surgeon’s request for preauthorization, which provides the ICD-10 and CPT codes submitted.
- A copy of your denial letter, including the section regarding your appeal rights.
* It is strongly recommended that you obtain a copy of your surgeon’s LOMN (letter of medical necessity) before it is submitted to your insurer or for external review, so we can assist your busy surgeon in making the strongest possible case for you.
Don’t be deterred by a denial. It is unfortunately more common than it should be, but it can often be overcome if you meet the requirements for bariatric surgery, if you get help navigating the process.
Weight Gain after Gastric Bypass
January 04, 2017 9:12 am
Weight loss surgical procedures have different long term results and some procedures have more dramatic weight loss than others. Some procedures also result in much more sustained and long term weight loss. Unfortunately, what may be not obvious is that the patient has very little control over the outcome of the surgery in most cases. IT is very easy to blame the patient for weight regain after weight loss surgery. However, it is important to remind ourselves that the long term data reporting outcomes of the surgical procedures in most cases, includes all patient population. All these studies include the most compliant and not so compliant patients. Comparison chart of outcomes of weight loss surgical procedures.
A larger percentage of gastric bypass patients will require revision for weight regain, or other problems. There is no evidence that the size of the pouch or the anastomosis between the pouch and the small bowel changes the weight regain outcomes. Yet, quite frequently I will see patient who have had gastric bypass revision for weight regain, by reducing the size of the pouch or the anastomosis. Here are some publications that support the notion that other than extreme dilation, the size of the pouch and the size anastomosis does not predict the outcome of the surgery. There is some correlation with the site of the pouch, anatsmosis and weight loss, but there is no correlation between the size of the pooch, the opening and the failure rate. This means that patient with smaller pouch do not have better long term outcome that the ones with larger pouch, only that the patient with smaller pouch or anatsmaosis will loose more weight.
“Influence of pouch and stoma size on weight loss after gastric bypass”
Weight regain after RNY Gastric Bypass may also be caused by a Gastro-gastric fistula, which is a new connection between the pouch and the remnant stomach. Here is further information on Weight Loss Surgery Revisions.
When considering a primary weight loss surgical procedure, be informed. Investigate all your options and consider the long term outcomes. This may mean investigating different weight loss surgical procedures on your own.