Category: weight loss
SIPS-SADI and ASMBS
December 31, 2023 1:21 pm
Weight Loss Injection
May 10, 2023 1:06 pm
Semaglutide (Ozempic, Rybelsus, Wegovy, Saxenda) and tripeptide (Mounjaro) treat type II diabetes. They work thru several complex pathways. An observed side effect that has been noted in diabetic patients has been weight loss.
Some have been advocating using the class of medications for weight loss. However, Wegovy is the only medication approved for weight loss in non-diabetic patients.
There is a lot to be discussed here:
1-the use of the medications for weight loss is an off-label use (except Wegovy)- meaning that the FDA did not approve the medication as a weight loss drug.
The practical implication is that the medication’s safety and complication profile in non-diabetic patients looking to lose weight may be unknown and has not been studied.
2-The medication has become available thru compounding pharmacies. It is crucial to appreciate that compounding medications do not meet the same rigor and standards and may, in fact, not be the same formula as the FDA has stated.. This also means that a compounding pharmacy does not approve the medications in several states.
3-The most critical issue for me is the lack of a “long-term plan.” It is not clear what would happen when the patient stopped the medication. Will the patient experience weight regain? Will the patient require higher doses of the medication to maintain the weight loss, or will the medication stop working altogether? Unfortunately, we do not have these answers. For those skeptical about my questions, let me remind you that phentermine has significant side effects, and almost all patients experience weight gain when they have to stop the medication because of the cardiovascular complication of medication.
Sleeve Gastrectomy in Adolescent patients
September 23, 2020 5:44 am
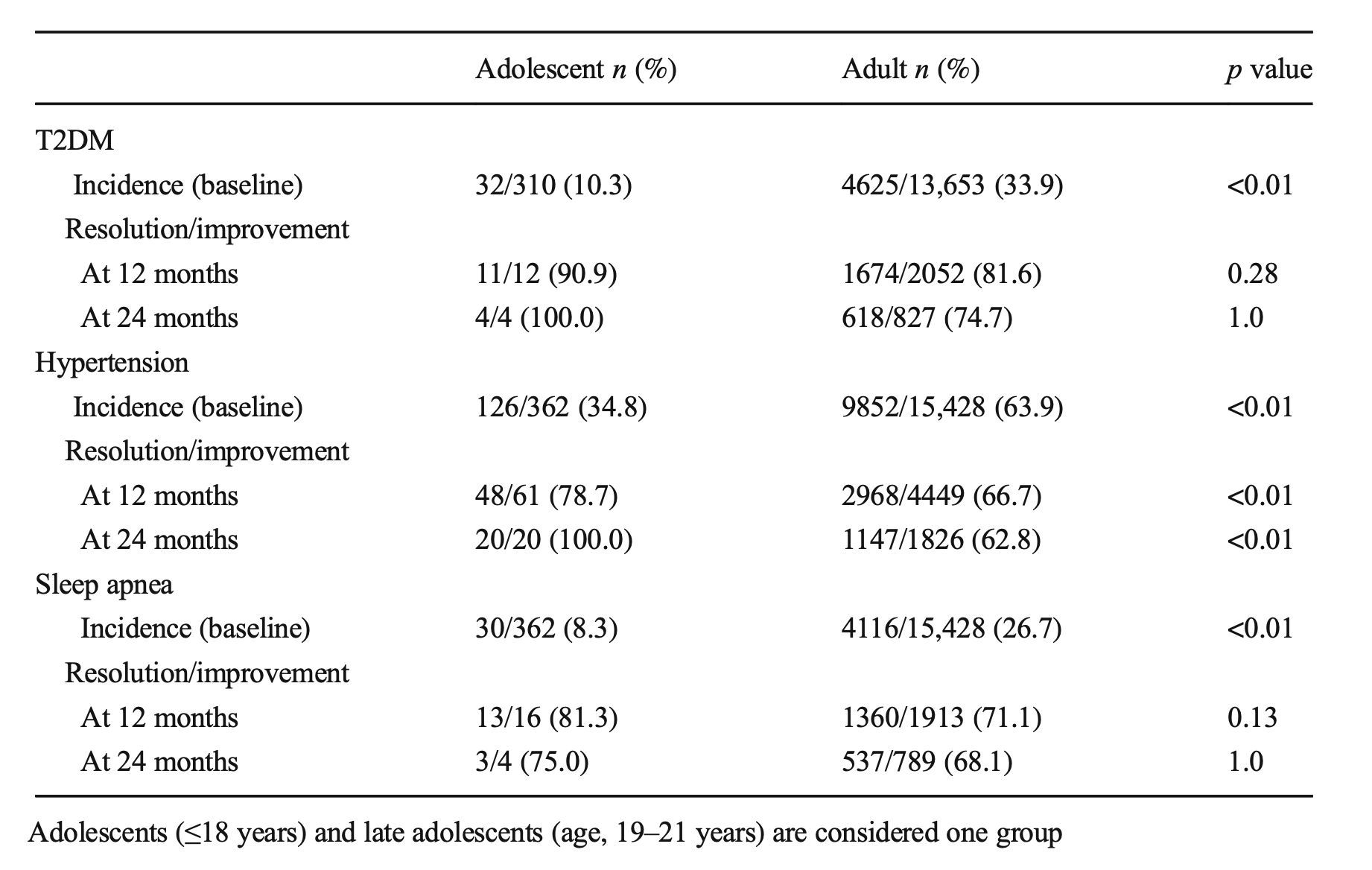 Sleep apnea resolved at the same rate. These early interventions can mean there may be lower long-term risk and associated conditions for these teens as they age.
A recent article was written from several adolescent weight loss surgical patients’ perspectives: This included their feelings of hope for their futures and health.
Sleep apnea resolved at the same rate. These early interventions can mean there may be lower long-term risk and associated conditions for these teens as they age.
A recent article was written from several adolescent weight loss surgical patients’ perspectives: This included their feelings of hope for their futures and health.
Gastric Balloon
March 12, 2019 9:10 am
Here we go again…. There is a new cure for obesity, Gastric Balloon, with minimal to no risk, is an outpatient procedure and/or can be done in the surgeons office with no anesthesia. Have we not similar claimed like this before (Adjustable gastric band) ?
Randomized sham-controlled trial of the 6-month swallowable gas-filled intragastric balloon system for weight loss published in Surgery for Obesity and Related Diseases 14 (2018) 1876–1889, by Sullivan et. al reports
“Conclusions: Treatment with lifestyle therapy and the 6-month swallowable gas-filled intragastric balloon system was safe and resulted in twice as much weight loss compared with a sham control, with high weight loss maintenance at 48 weeks.”
This sound very promising, however is very vague and leaves out significant, critical, and pertinent information.
The outcome of weight loss at 24 weeks was reported in Total Body weight loss % (TBWL%), Excess weight % (EWL), weight loss, and BMI change. Of those, the last three were statistically significant changes.
The outcome the weight loss was reported to be at 7% TBWL% at 24 weeks with some weight regain, with the patient employing post REMOVAL life style changes. 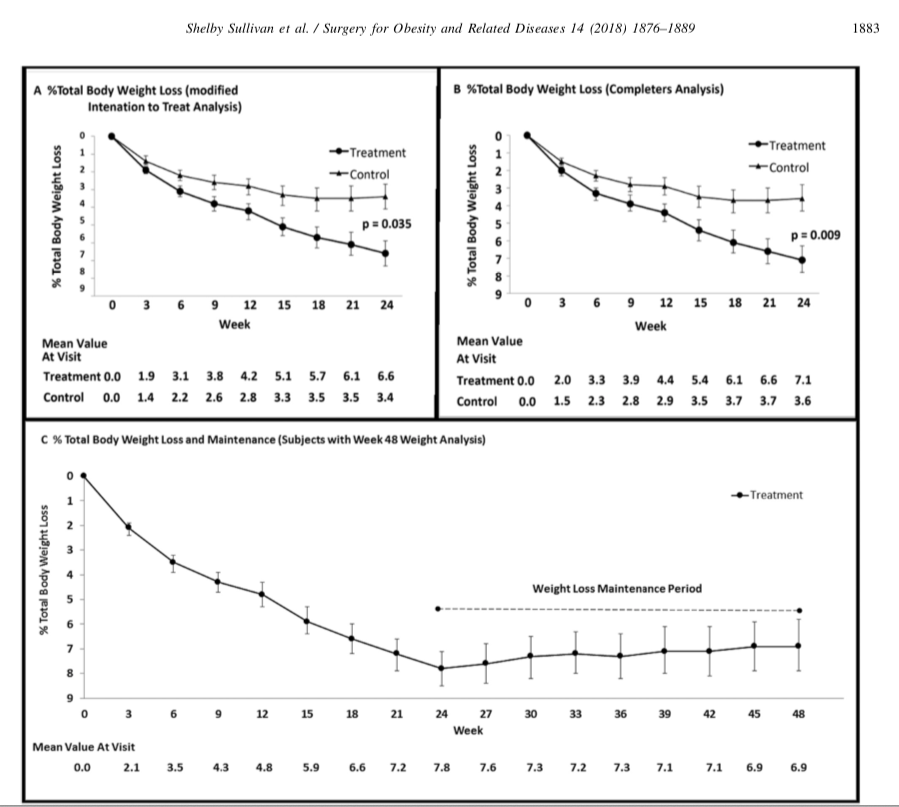
It is stated that the Gastric Balloon is temporary device that needs to be removed in 6 months and should be considered in low BMI patients (<35kg/m2). It is is important for those patients who are considering this temporary expensive measure for minimal weight loss to entertain the alternative of the same temporary results that may be obtained by lifestyle changes. These results may be maintained by a healthy lifestyle, exercise, and eating without the need for a device.
Cholecystectomy-Gallbladder Removal
September 10, 2018 9:44 am
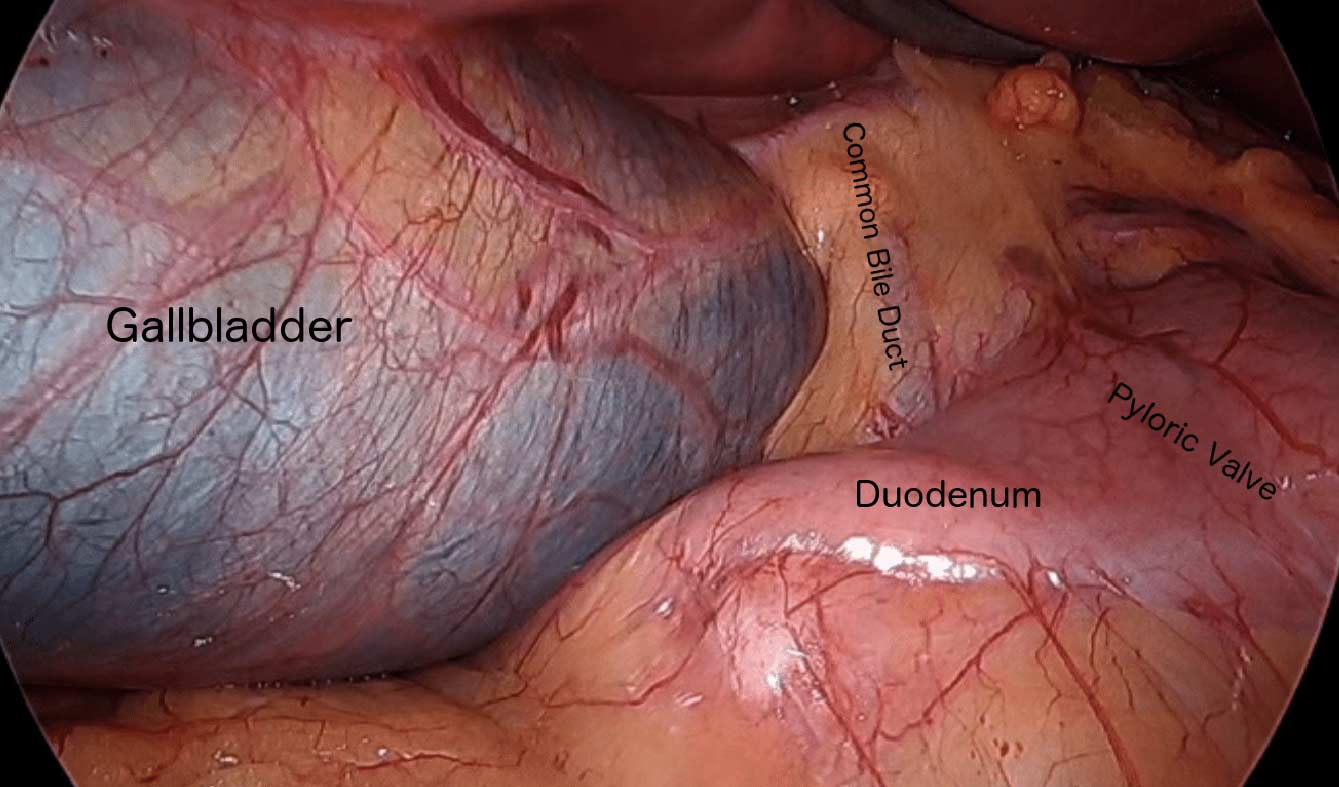
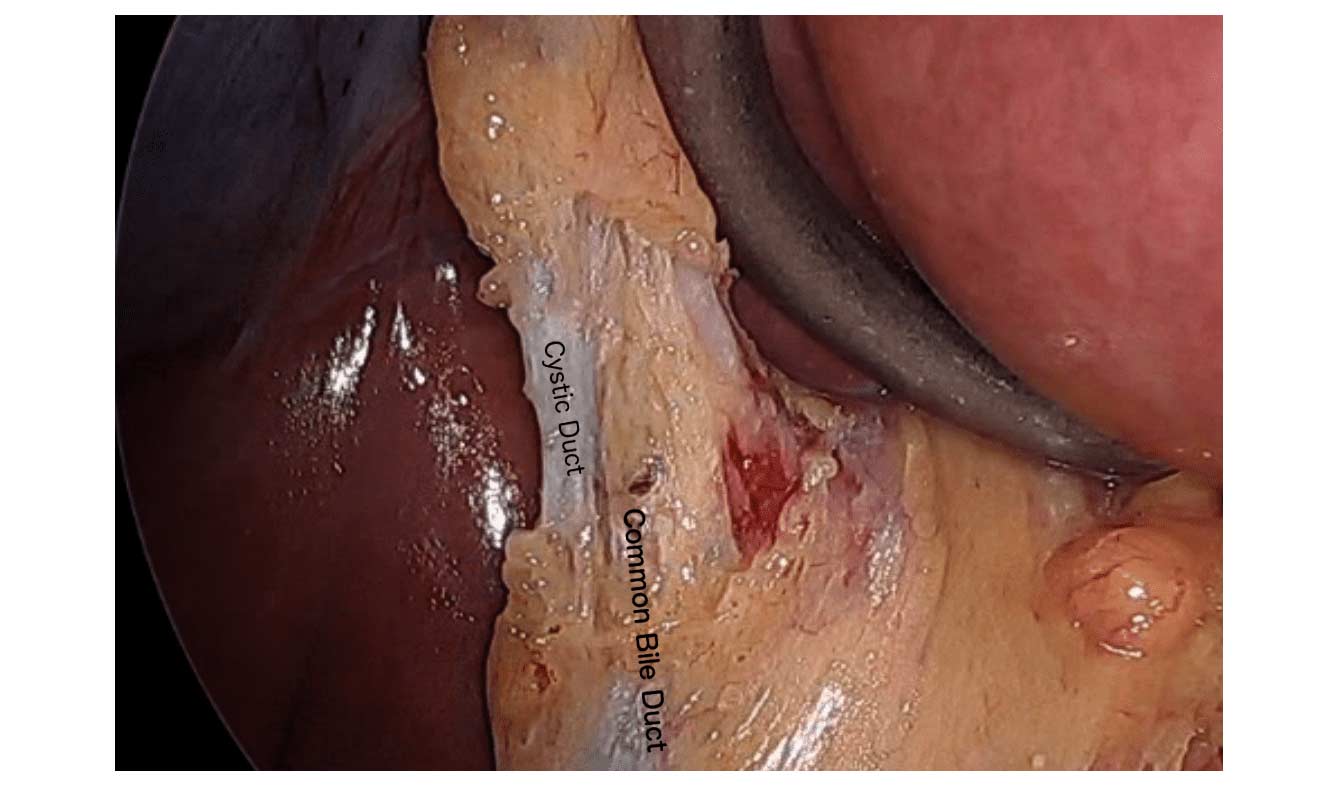
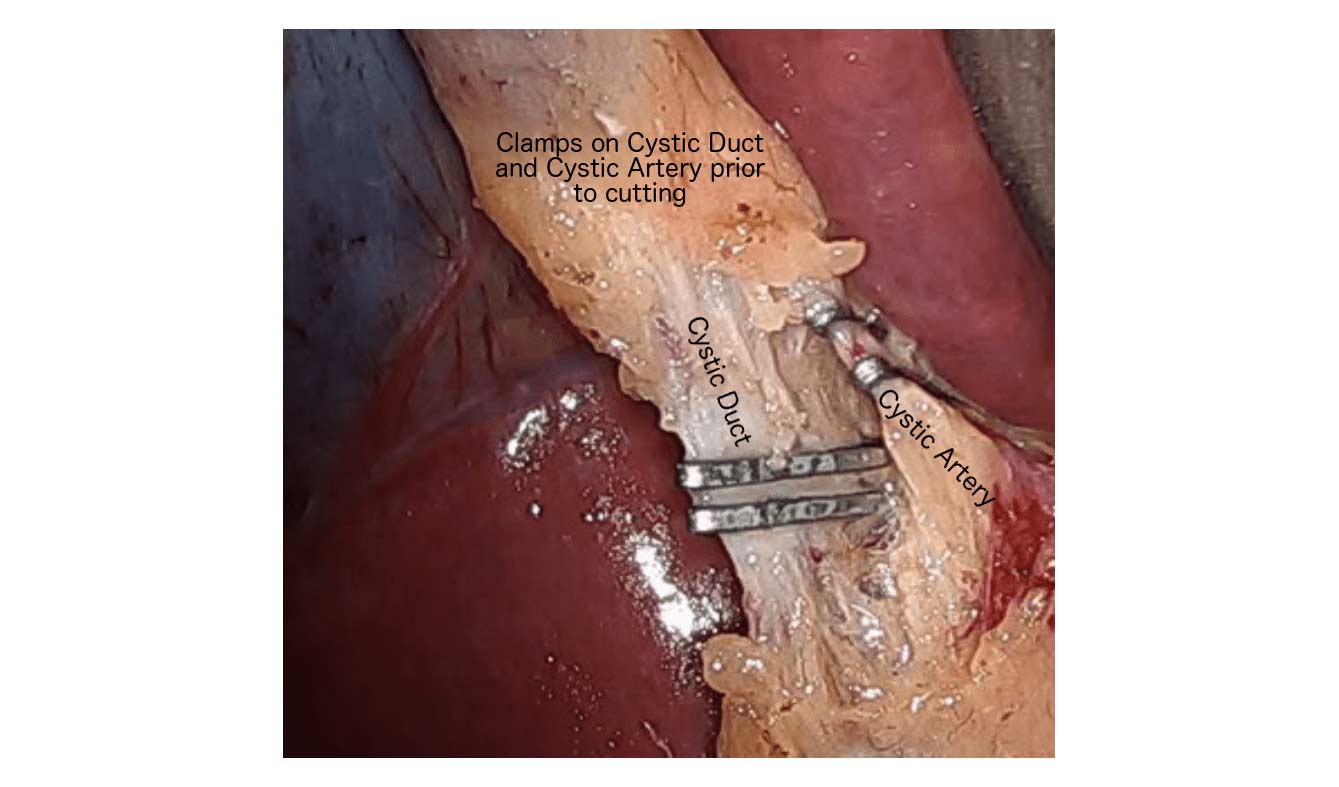
There are differing opinions, based on a broad set of scientific publication, wether or not gallbladder should be removed at the time of weight loss surgery. Obviously, Cholecystectomy is a stand alone general surgical procedure that is often performed due to gallstones and/or gallbladder disease with a variety of symptoms. However, the focus of this blog will deal with Bariatric Surgery and Cholecystectomy.
Rapid weight loss can increase a patients chance of forming gallstones. This rapid weight loss can be as little as 3-5 pounds per week. Weight loss surgery can increase your risk for gallstone formation. Several of the common thought processes the mechanism of this is, obesity may be linked to higher cholesterol in the bile, larger gallbladders, high fat diet and larger abdominal girth.
When a patient is having the Duodenal Switch (DS) Bariatric operation, or having a revision of a failed gastric bypass to the DS, I always remove the gallbladder. This is because there isn’t an anatomical route to utilize endoscopic procedure for an ERCP should the need rise.
In the case of a patient undergoing Vertical Sleeve Gastrectomy, if there are any indications or complaints of abdominal pain then an ultrasound is done. If there are findings of gallstones or other disease of the gallbladder, then a cholecystectomy is performed at the same time as the Sleeve Gastrectomy.
In my opinion, every patient having the Gastric Bypass (RNY) should also have the gallbladder removed because of the anatomical limitations after surgery that prevents the use of ERCP if needed. Some clinicians will place the patient on a long term medications to reduce the chance of gladstone formation after surgery, which themselves have side effects limiting the compliance in most patients.
Further information on Common Bile Duct Dilatation and ERCP
PolyCystic Ovarian Syndrome PCOS
September 04, 2018 9:58 am
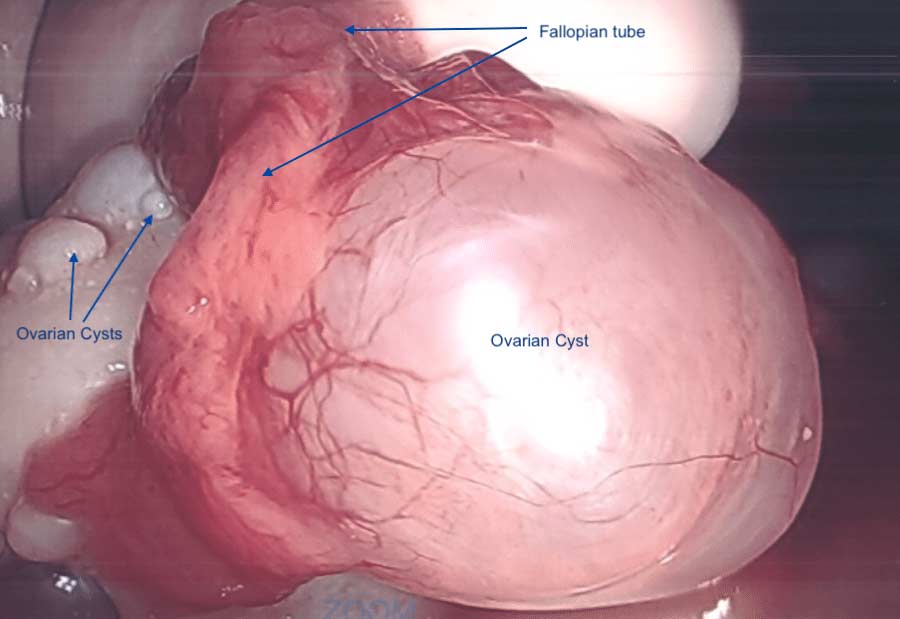
PolyCystic Ovarian Syndrome PCOS is a complex condition. The exact cause of PCOS is unknown however, it involves hormones imbalance and multiple ovarian cysts, irregular menses, and infertility. In some cases, PCOS can be compounded by diabetes, hypertension and other metabolic conditions. PCOS has been shown to effect approximately 10% of women of childbearing age with symptoms of menstrual abnormalities, poly cystic ovaries, and excess androgen (male sex hormone). PCOS should be diagnosed by ensuring there are no other underlying endocrine issues. There are several associated disease processes that seem to be related to PCOS. These related disease processes are Type 2 Diabetes, higher depression and anxiety, increased cardiovascular risks, stroke, hyperlipidemia, sleep apnea, overall inflammation, and endometrial cancer.
Anatomically, numerous cysts are found on the ovaries. These are usually diagnosed by ultrasound, blood levels of hormones, and symptoms described above.
Bariatric Surgery and PolyCystic Ovarian Syndrome PCOS
Bariatric Surgery can improve PCOS in those individuals with Type 2 Diabetes Mellitus. Further information on weight loss surgery and its effect on PCOS here.
Parathyroid Scan
July 09, 2018 11:48 am
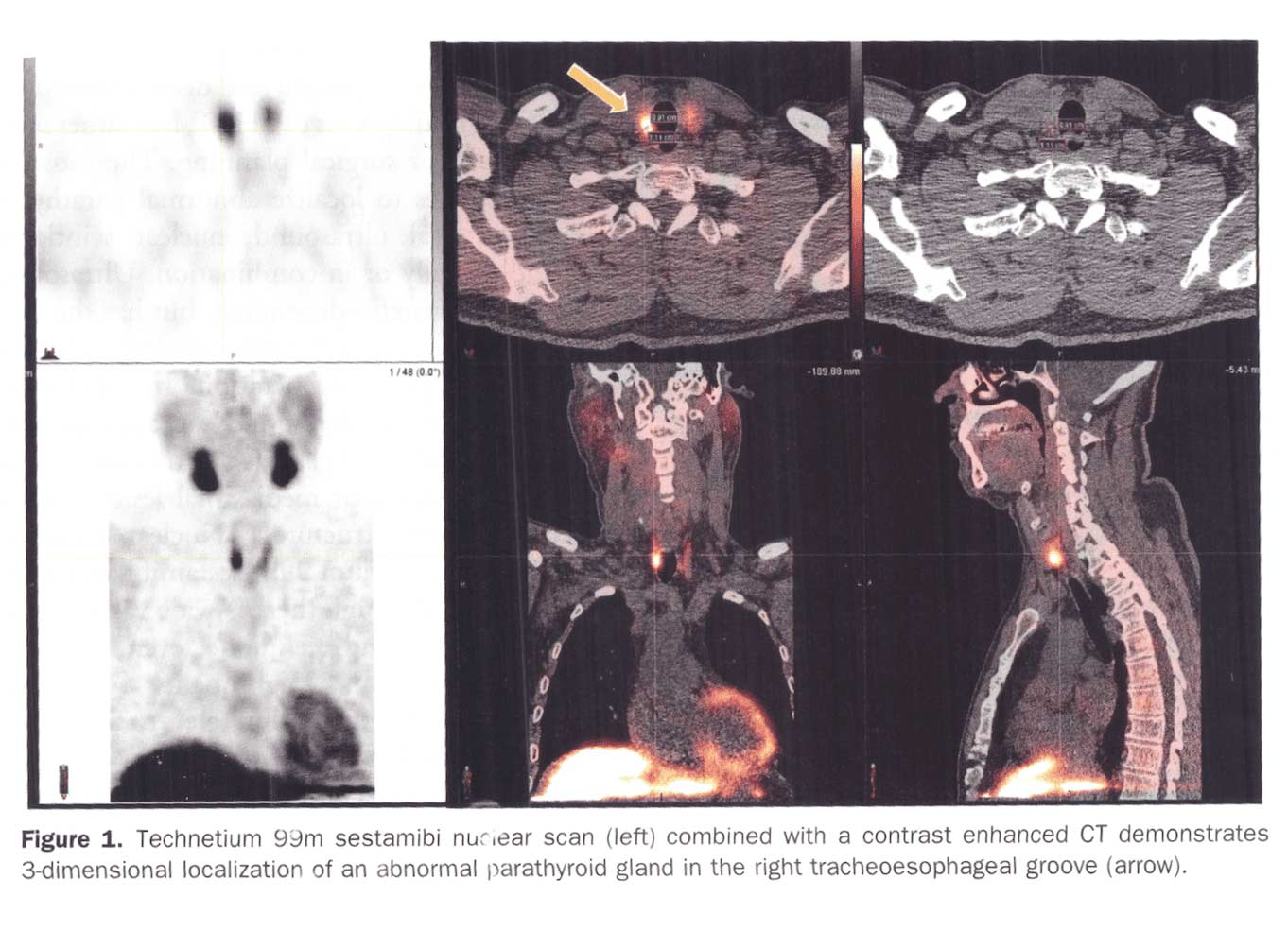
A Parathyroid scan or Sestamibi scan may be needed if the typical weight loss surgical reasons for elevated PTH levels have been addressed. Sestamibi is a small protein which is labeled with the radio-pharmaceutical technetium-99. This very mild and safe radioactive agent is injected into the veins of a patient with overactive parathyroid and is absorbed by the overactive parathyroid gland. If the parathyroid is normal it will not absorb the agent. The scan below shows the uptake of the agent.
Calcium, Vitamin D and Parathyroid hormone are routinely measured on yearly follow up for most post weight loss surgical (WLS) patients. Elevated parathyroid hormone (PTH) may be caused by Vitamin D deficiency or calcium deficiency (most common in post WLS) or by over active parathyroid gland(s). In the latter case, if one of the four glands is overactive then this is knows as a parathyroid Adenoma. If all 4 are over active and are secreting too much PTH, this is known as hyperplasia. Ultrasound of the neck, may identify an enraged parathyroid gland (adenoma) which is located behind the thyroid gland. Given the large area where the parathyroid gland may be located, additional tests are needed to not only identify the location of the gland(s) but also to distinguish between single gland (adenoma) or multiple glands (hyperplasia) cause for the elevated PTH. It is important to investigate all avenues and testing in parathyroid hormone elevation and in some cases, not to rely on one test for your diagnosis. It is also imperative that weight loss surgical patients take their supplements routinely and consistently and have their laboratory studies followed at least yearly.
Importance of ProteinExclusive Member Content
September 08, 2016 2:43 pm
Revision of Gastric Bypass
July 20, 2009 10:02 pm
Terry had the gastric bypass operation 3 years ago in an a major referral center by an established surgeon. The surgery went well, and lasted about one hour. The postoperative course was uneventful, and the patient was discharged home on post op day 2. The 3-6 month post-op period was complicated by a stricture at the gastro-jejunostomy anastomosis. An upper endoscopy and dilation. He continued to loose weight as expected. He attended the support meetings early on and then ended up missing some of them after the third year. The follow up appointments with the surgeon were all kept. The episodes of dumping syndrome, the feeling of passing out, diarrhea, high heart rate, nausea amongst others were scary early on. They became less frequent but not any less concerning. He was told by the surgeon that it s a part of the gastric bypass operation. In fact someone at the surgeons office told him that “..you hope you have it, since it will help you with your diet and prevent weight regain..”
He started feeling weak and tired at times after the second year. He also gained about 50 pounds back after the third year. The weight gain did not stop till I was within reach of my pre gastric bypass operation. What is worse is that he had to use CPAP machine for sleep apnea that had gone away with weight loss. He also was started back on some of his medications including those for diabetes. He went back to his surgeon, whose first reaction was that “….You must be doing something wrong…”
He was then referred to see the nutritionist, had an upper endoscopy, and an upper GI series. When he went back, he was told that there is nothing wrong and that he should eat correctly and exercise more.
This is not a story but a real example of many more patient that I see in our office all the time. As the facts are pretty accurate, clearly the name, and the specific details have been altered in this article.
What this patient has experienced is what I hear in the office all the time from patients who had the gastric bypass and they “….did not know….” about any other weight loss surgical procedure. After the surgical “honey moon” period of about 2-3 years (much longer than my real honey moon) the reality sets in. Weight regain, inadequate weight loss, nutritional deficiencies, dumping syndrome, and solid intolerance are examples of problems which will direct a patient to seek a solution.
The published data show that the small size of the pouch, in gastric bypass, does not predict excess weight loss (O’Connor et.al. SOARD 4, 2008, 399-403), (Nishie et.al, Obesity Surgery 17, 2007, 1183-1188). The size of the gastrojejunostomy anastomosis also does not assure adequate weight loss (Cottam et.al. Obesity Surgery 19, 2009, 13-17). Dumping syndrome does not improve gastric bypass surgery outcome. And the incidence of resolution of the obesity related illnesses is significantly better with duodenal switch operation that the gastric bypass or the adjustable gastric banding procedure. Patients with diabetes or cholesterol and triglyceride problem, in my opinion, should not have gastric bypass or adjustable gastric banding done.
A review of the published scientific articles in JAMA, shows that the outcome of Duodenal switch operation is far better than the alternatives with all measured parameters of excess weight loss, diabetes resolution, and improvement of hyperlipidemia.
Let me pose a question. If a patient is told that there are two antibiotics and one of them will treat the urinary track infection in 83.7% of the time and the alternative will treat it in 98.9% of the time, which one would you like to be treated with, if the overall risks all the same?
| Significant Hyperlipidemia Improvement | Diabetes Resolution |
Excess Weight Loss |
|
| Duodenal Switch | 99.50% | 98.90% | 70.10% |
| Gastric Bypass | 93.60% | 83.70% | 61.60% |
| Gastroplasty | 80.90% | 71.60% | 68.20% |
| Gastric Banding | 71.10% | 47.90% | 47.50% |
Source:JAMA, review of published data based on more than 22000 patients outcome.
As a Duodenal switch surgeon the answer is clear. I am only trying assure that no patient ever goes to the operating room without having all their options entertained. An informed consent is only valid if all the information was presented. Too often the alternative are either never discussed or barely discussed. A review of the websites demonstrates this point. Very few surgical practices that do not offer the duodenal switch operation discuss this alternative.
And to those that ask, “Why are there more surgeons doing the duodenal switch operation?” I think this a question that needs to be posed to those that do not do it. Here are some of the reasons:
- The perceived malnutrition is usually given as a reason. There is a large body of published data in the literature that documents the incidence of malnutrition to be significant in gastric bypass operation. In fact, because of the dietary restriction after gastric bypass there are as many if not more nutritional deficiencies that develop after this operation than the duodenal switch operation.
- The need for follow up. I am not clear as to why would this be a reason not to offer a surgery. The scientific evidence again shows that the more structured the follow up the better the outcome. Obesity is a chronic disease, that has a surgical, medical and maintenance phase. The broad picture of treatment plan for obesity in my opinion is no different than that of a cancer patient, who may need surgery, followed by chemo-radiation, and routine follow up.
- Last, and most vividly discussed is the issue of increased flatus, and loose bowel movements. There is no dispute that the duodenal switch operation does cause increase in flatulence and loose bowel movement. But here are the facts- in my more than 10 years in private practice, in an office that at times the waiting room is full of pre and post op patients, we have never had to evacuate the building because someone let one go! It has been my experience that that in overwhelming number of cases that have problem with significant gas and diarrhea the problem is easily corrected with minor changes in diet. Polish sausage, bagel and cream cheese for breakfast, deep dish pizza for lunch, and deep fried turkey may give some patients increased gas and diarrhea! With this said however, I have had patients in whom after exhausting all non surgical options (dietary modifications, medications etc) revision of the duodenal switch operation has been done.
In my opinion, the best patient is the most knowledgeable patient. Please make sure that you have taken the time to investigate not only the the surgeon, but also the available procedures.