Category: Gastric Bypass
Protein Sources
May 16, 2019 10:26 am
Not all proteins are created equally. The protein that we digest serves as the source of the essential amino acids, (the building blocks which make up a protein). The essential amino acids can not be made in out body. Protein sources can be animal or plant based. We’ve written a in-depth explanation of protein sources in this previous blog: Protein Optimization
The proteins can also be decided into two categories:
1-High quality or Complete proteins
Complete proteins contain all the indispensable amino acids that we need. Animal based proteins for the most part are complete proteins. These include cheese, mean, fish, mild, yogurt, egg and poetry.
2-Low quality or Incomplete proteins
Incomplete protein are mostly plant based proteins. In most cases, the incomplete proteins either lack or have insufficient about of the one or a number of amino acids to be able to satisfy our nutritional requirements.
This is why we general recommend animal based proteins.
Following weight loss surgery there are some guidelines that can be helpful in our previous blog: Importance of Protein.
SIPS, SADI-S, Loop DS
May 01, 2019 9:03 am
The American Society for Metabolic and Bariatric Surgery (ASMBS) and MBSAQUIP-A on March of 2019, published and updated list of “Endorsed Procedures and Devices”
Endorsed Procedures and Devices | American Society for Metabolic and Bariatric Surgery
Note that any surgical procedures that does not employ two anastomosis, are not endorsed and are only recommended to be performed with an IRB (Institutional Review Board) or an IRB exemption. Duodenal Switch, Sleeve Gastrectomy, Roux en Y Gastric Bypass, Gastric Balloon, Adjustable Gastric Banding, and Nerve Blocking which are endorsed procedures.
SIPS, SADI-S, SIPS, Loop DS are all in the category of the “Non-Endorsed Procedures and Devices”. To see an anatomical comparison of these procedures to the Duodenal Switch procedure.
Patients should request that their consent be clearly defined and should explicitly outline the procedure that is being proposed to them. This is to avoid a patient having a procedure that they assumed, or are led to believe to be a Duodenal Switch operation with two anastomosis. Do your due diligence and know the procedure you want. Investigate if the surgeon you are working with performs the procedure you are interested in. Have them draw a picture of the procedure or give you a diagram of the procedure.
Dr. Facebook
March 22, 2019 8:24 am
We have become reliant on the information that we obtain from the internet, specifically platforms such as Facebook. In our practice we have to continuously correct information that patients have obtained from other patients, unmonitored sites, blogs, and postings. Most of this information is based on individual experiences that has become gospel. “Fat is good for you” is one of them. To clarify, some health fat (olive oil, avocado, Omega 3) is healthy and needed for all patients. We do not recommend “fat bombs” as a part of ones daily dietary intake.
The following article was written on the accuracy of nutritional posts in support groups on Facebook.
Koalall et. all in SAORD, December 2018 Volume 14, Issue 12, Pages 1897–1902 published
“Content and accuracy of nutrition-related posts in bariatric surgery Facebook support groups”
The conclusion, as suspected, that “Over half of the posts contained inaccurate content or information that was too ambiguous to determine accuracy..:”

It is our recommendation before any dietary recommendations are taken from facebook and the like, the source of the information should be verified. As I have stated in the past, a frequent flier passenger is probably not qualified to fly a
commercial airplane, any more than a previous weight loss surgical patient providing medical and nutritional advice. We realize that there is significant value to the forum for exchange of information and sharing of experiences with other weight loss surgical patients as long as the information is well sourced and verified.

GI Bleed following Weight Loss Surgery
September 17, 2018 10:28 am
Gastrointestinal (GI) Bleed following weight loss surgery is rare but does require knowledge of the particular bariatric surgical procedure the patients has and how to proceed with diagnostics to fully evaluate the situation. Acute or chronic gastrointestinal bleeding can cause anemia in patients. However, Anemia may also be caused by nutritional deficiencies (iron, vitamin , minerals), Kidney disease, bone marrow disease and others. The work-up for anemia following weight loss surgery follows a routine protocol. If there is an evidence of bleeding from intestine (bloody emesis, bloody bowel movement, “tar” like black bowel movements) then the diagnostic work up would include an upper and lower endoscopy.
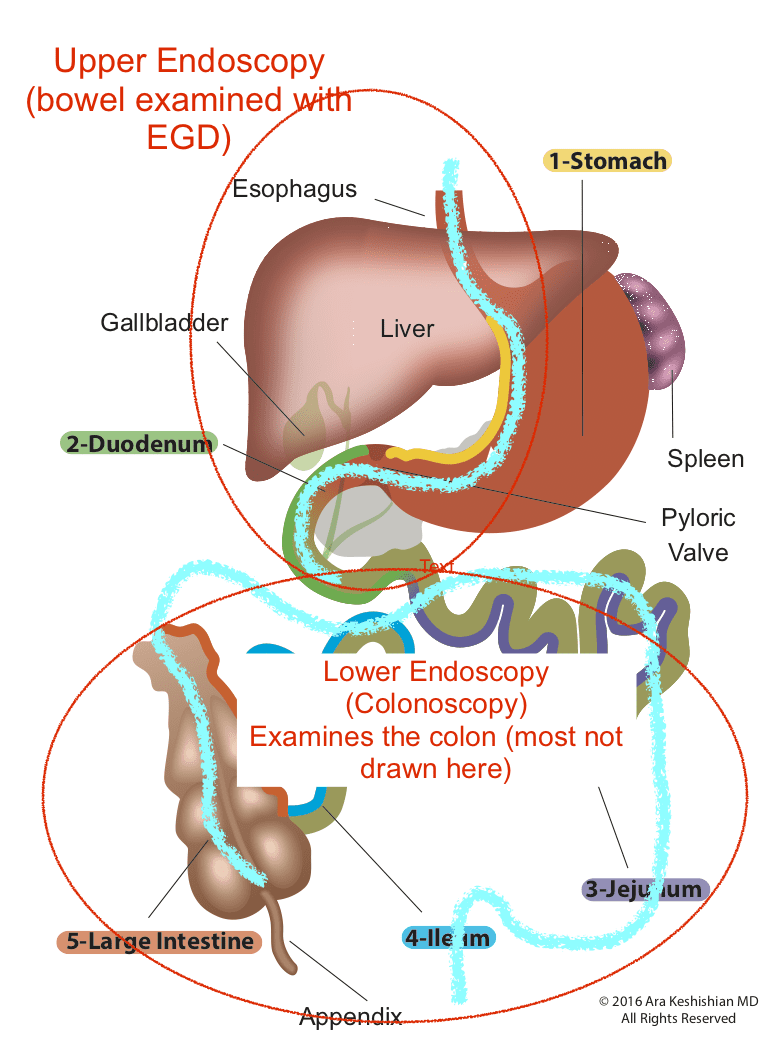
Endoscopic Procedures:
Upper endoscopy Esophagogastroduodenoscopy (EGD): evaluates the esophagus, stomach and a limited area of the duodenum past pyloric valve.
Lower endoscopy Colonoscopy or coloscopy: evaluates the rectus and the entire colon.
Between these two tests, there is still a considerable amount of the small bowel that is not accessible or visualized with endoscopic procedures. For the small bowel, examination Capsule endoscopy is an option in an intact GI tract. Patients who have had Gastric bypass RNY or the Duodenal Switch, the large segments of the small bowel can not be visualized or examined with capsule endoscopy.
Patients who have had Duodenal Switch, Gastric Bypass and SADI – S would need a tagged red cell scan or CT angiography if GI bleed is suspected in areas of the small intestine that are inaccessible by endoscopic procedures.
Candy Cane Gastric Bypass – RNY
June 21, 2018 1:05 pm
One of the findings following Gastric Bypass is a Candy Cane Gastric Bypass. Nausea and vomiting , upper abdominal pain is a common complaint of patient who have had the Gastric Bypass RNY operation. This is in addition to the high incidence of patients who experience the complications of weight regain and or dumping syndrome.
Quite frequently the symptoms of nausea, vomiting and upper abdominal pain of a patient with history of gastric bypass is evaluated by a primary care, referred to a gastroenterologist. The “routine” work up recommended is X-ray of the abdomen, maybe contrast study (Ct scan or upper GI) and for sure and upper endoscopy. The result quite frequently reported as “…nothing wrong”.
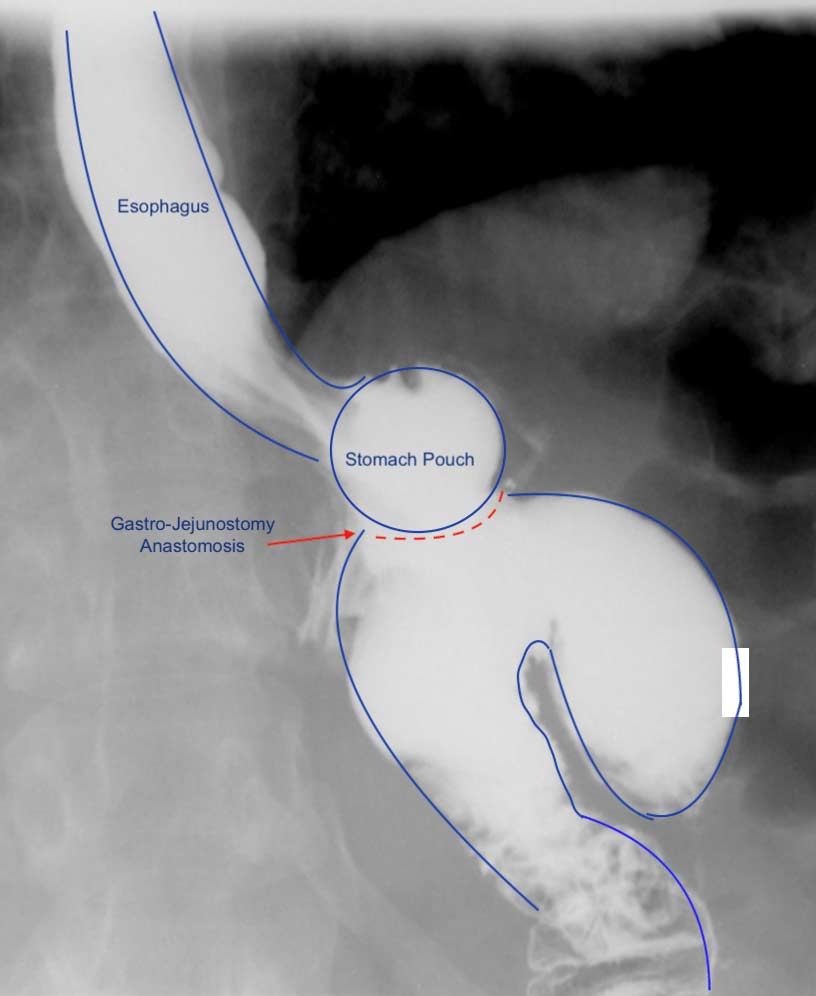
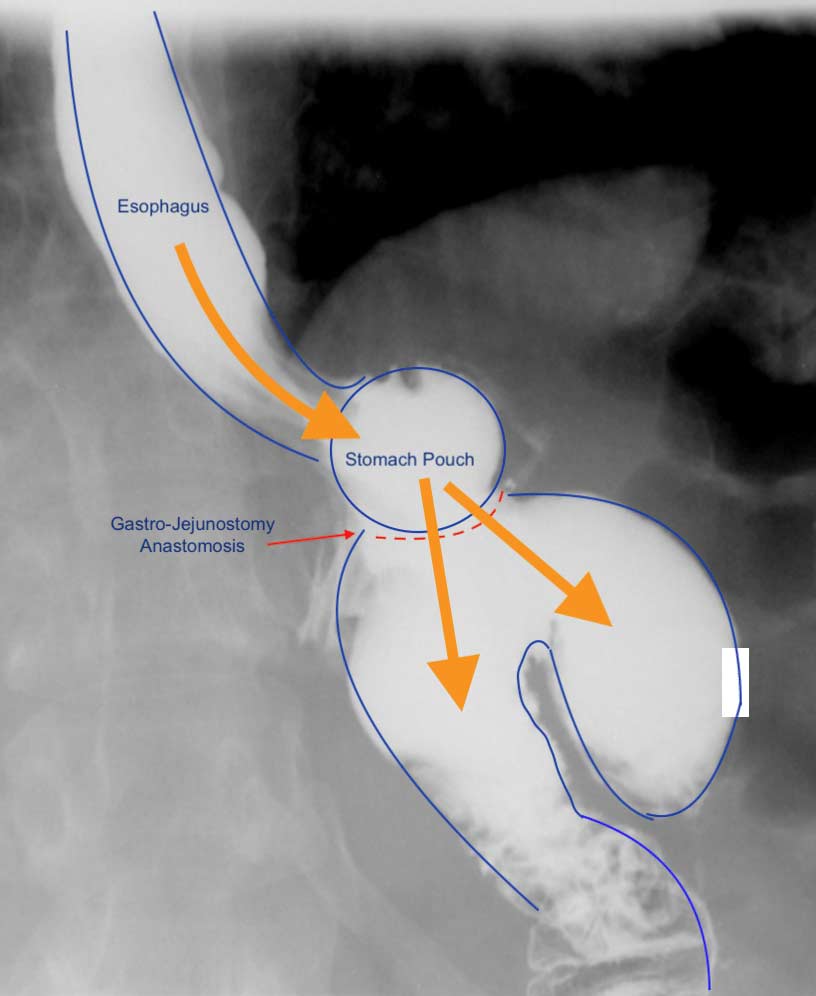
A typical upper GI in a Candy Cane Gastric Bypass situation may look like this:
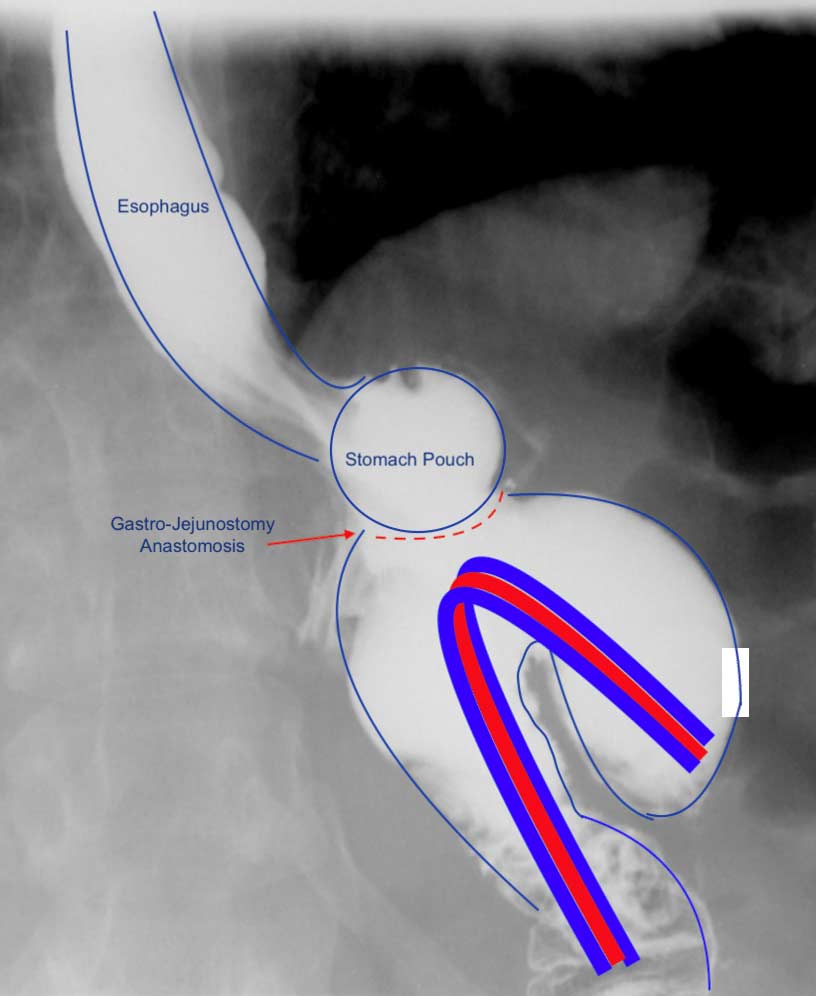
A common and underreported problem may be a Candy Cane finding. The “blind” end of the small bowel anastomosis is too long and this results in food settling in the hook of the candy cane. The symptoms of the nausea, vomiting and upper abdominal pain may be from the residual food and liquids that do not drain from this area.
Candy Cane Gastric Bypass finding
Candy Cane Gastric Bypass cases will require surgical intervention to shorten the length of the blind segment of the small bowel to improve symptoms.
It is my recommendations that any patient with history of weight loss surgery who is having any persistent gastrointestinal symptoms be evaluated by weight loss surgeon.
Calcium Lab Results
June 05, 2018 3:26 pm
Calcium is measured to evaluate function and adequacy of a physiologic processes. Calcium plays a critical role in several body functions such as, coagulation pathways, bone health, nerve conduction, and other functions. It is important whenever you are evaluating laboratory results that you look at the whole picture of the person, including medications, other laboratory studies and health history. One value is not a stand alone result. There are many factors that effect calcium results.
Factors that effect calcium results: (not an all inclusive list)
pH
Albumin
Lactate
Heparin
Anticonvulsants
Renal Disease
Pancreatitis
The two most common issues following Weight loss Surgery or Duodenal Switch may be albumin level and Vitamin D level. Please see past blogs on Vitamin D. Magnesium may also play a role in a Duodenal Switch patient.
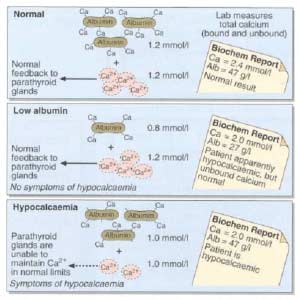
The most common calcium result drawn is the total calcium level. Laboratory results may not explicitly label it as such, however, it measures the calcium that is bound to protein. Ionized calcium is the free calcium that is representative of the true total calcium. Ionized Calcium can be measured by ordering specific lab. Alternatively, the Ionized calcium can be calculated by the following formula: Corrected calcium mg/dL = (0.8 * (Normal Albumin – Pt’s Albumin)) + Serum Ca ) or use the calculator at the bottom of this post.
The low Albumin level accounts for the low calcium level. This may be the reason for a patient with a low albumin/protein level, also having their calcium level reported as low. However, when adjusted for the protein deficiency the corrected calcium comes into normal range. Video of Trouseau’s sign of a patient with calcium deficiency.
The first step in a patient who has low calcium reported, is to make sure their protein and albumin levels are normal, along with Vitamin D.
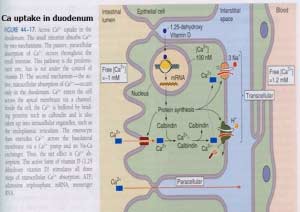
Calcium levels are managed by two processes major regularly hormones and influencing hormones. Controlling or major regulatory hormones include PTH, calcitonin, and vitamin D. In the kidney, vitamin D and PTH stimulate the activity of the epithelial calcium channel and the calcium-binding protein (ie, calbindin) to increase calcium absorption. Influencing hormones include thyroid hormones, growth hormone, and adrenal and gonadal steroids.
Further information on protein.
Further information on calcium.
Videos/Webinars on several of the above topics.
Corrected calcium = 0.8 * (4.0 – serum albumin) + serum calcium
Gas (Flatuence) GI upset
July 27, 2017 7:32 am
Following the Duodenal Switch operation, patients will have more frequent flatulence. The problem can get worse with specific dietary choices. A very simple way of looking at this would be that, in general, Carbohydrates contribute to gas and the fat contributes to causing loose bowel movements. Carbohydrate or gluten sensitivity can also increase stool production.There is a significant overlap of the effects of carbohydrates and fat intake and one has to remember that the symptoms of gas and loose stool can often accompany each other.
Weight Gain after Gastric Bypass
January 04, 2017 9:12 am
Weight loss surgical procedures have different long term results and some procedures have more dramatic weight loss than others. Some procedures also result in much more sustained and long term weight loss. Unfortunately, what may be not obvious is that the patient has very little control over the outcome of the surgery in most cases. IT is very easy to blame the patient for weight regain after weight loss surgery. However, it is important to remind ourselves that the long term data reporting outcomes of the surgical procedures in most cases, includes all patient population. All these studies include the most compliant and not so compliant patients. Comparison chart of outcomes of weight loss surgical procedures.
A larger percentage of gastric bypass patients will require revision for weight regain, or other problems. There is no evidence that the size of the pouch or the anastomosis between the pouch and the small bowel changes the weight regain outcomes. Yet, quite frequently I will see patient who have had gastric bypass revision for weight regain, by reducing the size of the pouch or the anastomosis. Here are some publications that support the notion that other than extreme dilation, the size of the pouch and the size anastomosis does not predict the outcome of the surgery. There is some correlation with the site of the pouch, anatsmosis and weight loss, but there is no correlation between the size of the pooch, the opening and the failure rate. This means that patient with smaller pouch do not have better long term outcome that the ones with larger pouch, only that the patient with smaller pouch or anatsmaosis will loose more weight.
“Influence of pouch and stoma size on weight loss after gastric bypass”
Weight regain after RNY Gastric Bypass may also be caused by a Gastro-gastric fistula, which is a new connection between the pouch and the remnant stomach. Here is further information on Weight Loss Surgery Revisions.
When considering a primary weight loss surgical procedure, be informed. Investigate all your options and consider the long term outcomes. This may mean investigating different weight loss surgical procedures on your own.
Don’t lose your Pyloric Valve over a Failed Gastric Sleeve
June 22, 2016 9:32 am
In my opinion, there are very few reasons to lose your Pyloric Valve after sleeve gastrectomy. Recently, I am hearing of people who have had regain due to a failed Sleeve Gastrectomy being revised to Gastric Bypass RNY and then seeking a Duodenal Switch due to regain from Gastric Bypass RNY. A better option is to go from Sleeve Gastrectomy to Duodenal Switch, due to the long term excess weight loss maintenance of Duodenal Switch. The benefit of the pyloric valve can not be taken lightly.
Let’s start by reminding ourselves as to how the Sleeve Gastrectomy has gained popularity. In the quest for a simple solution to the complex problem of obesity, adjustable gastric banding gained popularity only fail to deliver anything close with the results that were promoted and heavily marketed. The focus was then changed to another seemingly simple procedure, laparoscopic sleeve gastrectomy. For some surgeons this is a new procedure. Surgeons that had been doing the duodenal switch operation for decades, sleeve gastrectomy has not been a new procedure. Surgeons that just started doing sleeve gastrectomy as a stand alone procedure started experiencing complications of the sleeve gastrectomy, such as regain and are now looking for another option for these patients. This complication are even more frequent when they’re done following a failed adjustable gastric band procedures due to the metabolic issues after revising one weight loss surgery to another. A similar short sighted approach is also being promoted with SIPS/SADI procedures, which is significantly simpler to perform than the duodenal switch operation.
Laparoscopic sleeve gastrectomy has a predictable profile for weight loss. It will not have as good on the long-term success rate as a duodenal switch operation. Complications of the sleeve gastrectomy including reflux, stricture, fistula, inadequate weight loss which may warrant evaluation and possible intervention. In my opinion, as a surgeon who does the duodenal switch operation routinely, a sleeve gastrectomy requiring revision should almost never be revised to a gastric bypass. I have seen number of patient’s who have had an adjustable gastric banding which was revised to the sleeve gastrectomy then to a gastric bypass. We are contacted for a possible revision to Duodenal Switch operation because of the weight regain. One can argue that the patient should not have had the sleeve gastrectomy or gastric bypass. It is critical that the complexity of the disease of the obesity is clearly appreciated that it purely restrictive procedure will not yield the desirable outcome long-term.
Benefits of the Pyloric Valve:
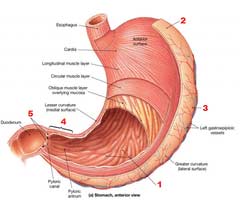
The pylorus is the valve located at the end of the stomach. It controls the release of the liquid mixture of food from the stomach into the small intestine.
The body naturally regulates the passage of food, so food will stay in the stomach for a certain period of time. We believe it is very important to continue that feeling of fullness in between meals. As a result, one of the principle functions of the pyloric valve is to regulate the amount of food products released into the small intestine where they are absorbed. This helps prevent dumping syndrome and ulceration.
The bodies natural diameter of stomach, pyloric valve and small intestine is left intact. This elevates stretching of the stomas created by RNY Gastric Bypass.
Summary
These failed Sleeve Gastrectomies should be revised to Duodenal Switch unless there are overwhelming health issues that would require another option. I always suggest several opinions from different Bariatric Surgeon’s who do a variety of Weight Loss Surgeries before deciding which type of revision to proceed with.
Weight Loss Surgery Effects On Iron Absorption
June 06, 2016 9:40 am
Anemia is a condition in which a person doesn’t have enough healthy red blood cells. Red blood cells (RBCs) function in carrying oxygen to the tissues and they are produced in the bone marrow. Iron deficiency anemia, the most common form of anemia, develops when the body is unable to produce sufficient hemoglobin because of an iron deficiency. To read more about iron deficiency anemia, please refer to our previous blog post here.
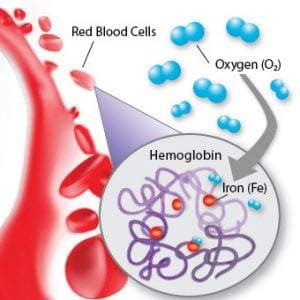
Iron is an essential mineral that is a critical component of hemoglobin. Hemoglobin (Hg) is a four protein molecule that carries oxygen from the lung
s to the tissues. It is also important in maintaining RBC shape for proper blood flow. Each of the four globulin chains in Hemoglobin contain an iron compound called a heme. An iron atom is fixed within the heme group to give the red blood color and transport oxygen and carbon dioxide. If the body does not have enough iron, the bone marrow will not produce enough Hemoglobin which results in unhealthy RBCs.
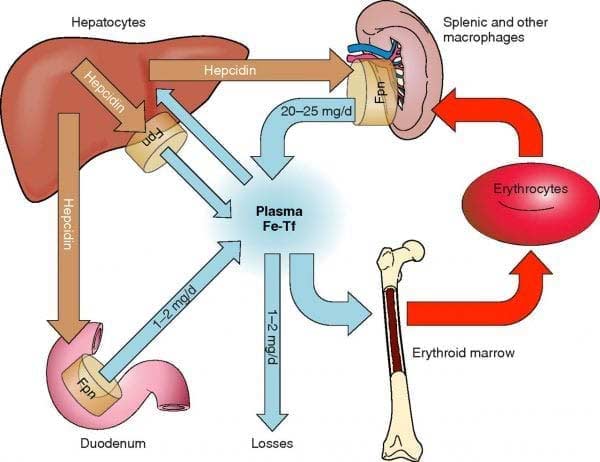
Iron is exposed to acids in the stomach, which alters the form into a configuration that allows absorption. The Duodenum of the small intestines is the main site of iron absorption. The ileum, found at the end of the small intestinal tract, is the site of secondary absorption. Once absorbed, each plasma protein transferrin transports two atoms of iron to the liver, spleen, and bone marrow (2).
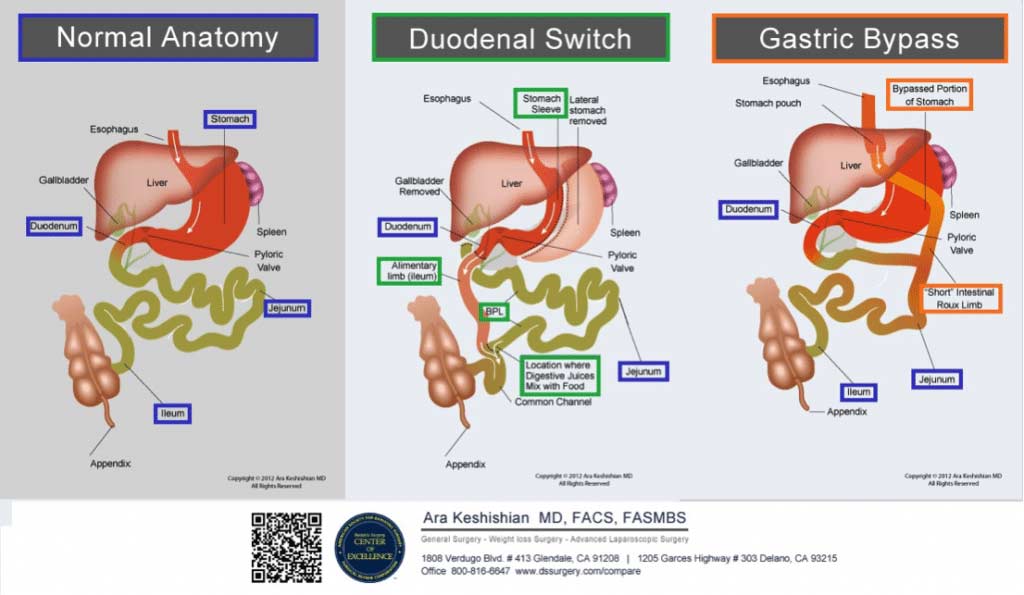
Anemia is common among patients who have undergone surgical weight loss procedures. Some weight loss procedures change the anatomy of the small intestinal tract result in malabsorption due to the restriction of food and nutrient intake. In Roux-en-Y gastric bypass (RYGB), the stomach and duodenum are completely bypassed thereby increasing the risk of iron deficiency. In the Duodenal Switch a small portion of post pyloric Duodenum is left intact to aid in iron absorption, however this may not be adequate for every individual. By redirecting the small intestinal tract in Duodenal Switch, only a small segment of the ileum is able to absorb the necessary nutrients. In both procedures however, blood tests find that patients can become iron deficient (1,3) and require oral iron supplementation or intravenous iron infusions if oral supplementation is inadequate to maintain iron levels.
Inadequate iron levels can be treated by taking iron salt supplements, especially along with vitamin C pills that help the body absorb more iron. Other types of supplements are Heme and chelated oral iron that are well tolerated without gastrointestinal upset of iron salts. For some WLS patients there may not be enough capacity for iron absorption via the GI tract and those patients may need Intravenous Iron infusions periodically. Dietary iron sources are important as a surgical weight loss patient as they are usually also high in protein (blog). Ie: Poultry, red meat, pork, seafood, eggs, beans, and green leafy vegetables are also a good source of iron.
In addition to supplementation of iron, it is important to identify any contributing factors to blood loss or decreased iron absorption such as gastrointestinal bleeding, heavy menses, surgery, pregnancy, medications or combination of supplements, infection or dietary issues. Identifying, advanced planning and/or correcting any contributing factors may reduce the iron demand for WLS patients.
In summary, iron absorption will be affected by altering the anatomy of the small intestinal tract. Although it takes a great deal of time to restore iron levels, reversing deficiency will help avoid symptoms and maintain proper blood, brain, and heart health.
Colored Coded Diagrams of where nutrients, vitamins and minerals are absorbed:
Please note this article and these diagrams are Member Exclusive Only. They are available for use by our patients ONLY. Please review your terms of use of our Member Exclusive Area.
Diagram of normal anatomy absorption here [download id=”14″].
Diagram of DS anatomy absorption here [download id=”8″].
Diagram of RNY anatomy absorption here [download id=”9″]
Written by: Mariam Michelle Gyulnazaryan & Dr. Ara Keshishian
References
- Fincannon J. Iron deficiency after gastric bypass surgery. University of Rochester Medical Center. 2016.
- Forth W, Rummer W. Iron absorption. Physiological Revies. 1973; 53(3) 724-792.
- Sawaya RA, Jaffe J, Friedenberg L, Fridenberg FK. Vitamin, mineral, and drug absorption following bariatric surgery. Curr Drug Metab. 2012; 13(9) 1345-1355.
- Von Drygalski A, Andris DA. Anemia after bariatric surgery: more than just iron deficiency. Nutr Clin Pract. 2009; 24(2) 217-226.