Category: Gastric Bypass
Fluids and Electrolytes After Weight Loss Surgery
January 29, 2016 7:06 am
Fluids and Electrolytes after weight loss surgery are an important part of recovery and lifestyle after undergoing a weight loss surgical procedure. Potassium is an important electrolyte found in higher concentrations within the fluid of the cells. It is important in muscle contraction, heart rhythm, nerve function and co-enzyme function.
Fluids and Electrolytes
The following webinar (link) discusses the balance of fluids and electrolytes with particular attention to post weight loss surgery concerns. Deficiencies can cause heart arrhythmias, muscle weakness and cramping, intestinal paralysis, and neurological deficits.
The Daily Recommended Amount for Potassium is 4,700mg
Here is a list of Lower-carb potassium sources: This is not meant to be in inclusive list. There are many higher carb sources of potassium also.
- Beet Greens- 1/2C 655 mg
- Trout 3oz – 375 mg
- Salmon 719 mg per average filet
- Halibut or Yellowfin Tuna 3oz – 500mg
- Clams 3oz- 534 mg
- Avocados 1 whole- 974 mg
- Squash 1C- 325mg
- Broccoli 1 cup 475m
- Watermelon Radish 3 oz – 233mg
- Sweet Potatoes- one potato 694mg
- Yogurt 1C – 579mg
- Tomato paste 1/4C – 342 mg
- Whole milk 1C – 366 mg
- Chicken breast meat 1 cup chopped – 358 mg
- Cauliflower 1 cup raw– 303 mg
- Peanut butter 2 T – 208 mg
- Asparagus spears 6 – 194 m
- Daikon Radish – 3″ – 280 mg
- Nuts 100-300 mg per 30g / 1 oz serving, depending on the type
- Dark leafy greens 160 mg per cup of raw, 840 mg per cooked
- Kohlrabi 3oz- 98mg
- Mushrooms 1 C- 273 mg
- Spinach – 1 cup 167 mg Potassium
- Walnuts 2 oz-250 mg
2015 ASMBS Summary
November 11, 2015 7:31 am
The 2015 ASMBS meeting was held November 2-6, 2015. It was combined with TOS (The Obesity Society) and had more than 5,600 attendees from all over the world in every aspect of obesity treatment. There were some interesting additions and deletions from this meeting compared to the past.
The one sentence that comes to my mind is “I told you so”.
One important addition was a DS course for Surgeons and Allied Health. This was very exciting, except the content and questions seemed to gravitate to SADI/SIPS/Loop rather than DS. Dr. Cottam was one of the moderators of the course. It seems that they have found the value in preserving the pyloric valve. It was clear that the discussion was driven by the need to come legitimize the single anastomosis procedures at this early stage with almost no data to prove long term outcome. With many of the Vertical Sleeve Gastrectomies having re-gain and the they are looking for a surgery that the “masses” can perform. This was actually the term used by one of the presenters, implying that the duodenal switch needed to be simplified so that all surgeons, those who have pushed all other procedures can not offer Duodenal Switch to their patients with less than desirable outcome. Several surgeons also voiced their concern and dissatisfaction with the issues and complication of the RNY and want an alternative. There was much discussion regarding SADI/SIPS/Loop being investigational and that it shouldn’t be as it is a Sleeve Gastrectomy with a Billroth II. Dr. Roslin and Dr. Cottam discussed their SIPS nomenclature saying they wanted to stay away from something that had Ileostomy, suggesting bowel issues, or the word “SAD”i due to negative connotations. The point to be made is that the SADI and SIPS and the loop are all the same. I have also noticed other surgeons using SADS (Single Anastomosis Duodenal Switch). There is a great deal of industry behind these procedures and many surgeons being trained in courses funded by industry. One surgeon stood up and informed the entire course that they need to be clear with their patients about the surgery they are performing, as he had been in Bariatric chat rooms and there is upset within the community about SADI/SIPS/Loop being toted as “the same or similar to Duodenal Switch”.
There was also presenter who said “We are doing something new about every five years.” No, “we” are not. Some of us have stood by the surgery and techniques with the best long term outcomes and not gone with every “new” thing out there. The process of Duodenal Switch may have changes, open Vs. Lap, drains, location of incisions, post operative care and stay, but the tested procedure with the best outcome has been the duodenal switch operation and not the shortcut versions. Although, those of us that are standing by long term results seems to be in the minority. Why do I stand by Duodenal Switch? Because it works, when done correctly by making the length of the bowel proportional to the patient total bowel length, and height, and not just cookie cutter length for all patients, with the right follow-up, patient education, vitamin and mineral regime and eating habits.
A new addition was the Gastric Balloon, which in the research presented had a 60-70% re-gain rate and a no more than 10-15% weight loss one year only. This data represents more than 70% weight regain when the balloon is taken out. The Gastric Balloons can be left in between 4-6 months depending on the brand or type of balloon. The Gastric Balloon is not new to the Bariatrics and was first introduced in 1985. After 20 years and 3,608 patients the results were and average of 17.6% excess weight loss. It seems that we are re-gurgiating old procedures. There are many new medications that were front and center in this meeting.
The Adjustable Gastric Bands were missing from the exhibit hall this year. It is my hope and feeling from the other attendees that we may be seeing the era of the Adjustable Gastric Band being placed in patients come to an end. Although there are some still holding out that there are some patients that can do well with the Band.
Attending the 2015 ASMBS meeting this year, as it has every year, only reemphasized the importance of avoiding what has become the norm of chasing a simple solution that is fashionable and easy now. We stay convinced that the duodenal switch operation with the common channel and the alimentary length measured as a percentage of the total length is by far the best procedure with the proven track record. The patient should avoid the temptation of settling for an unproven procedure or device, because if history holds true, there will be a need for revision surgeries in the future.
Surgical Outcomes
October 02, 2015 10:10 am
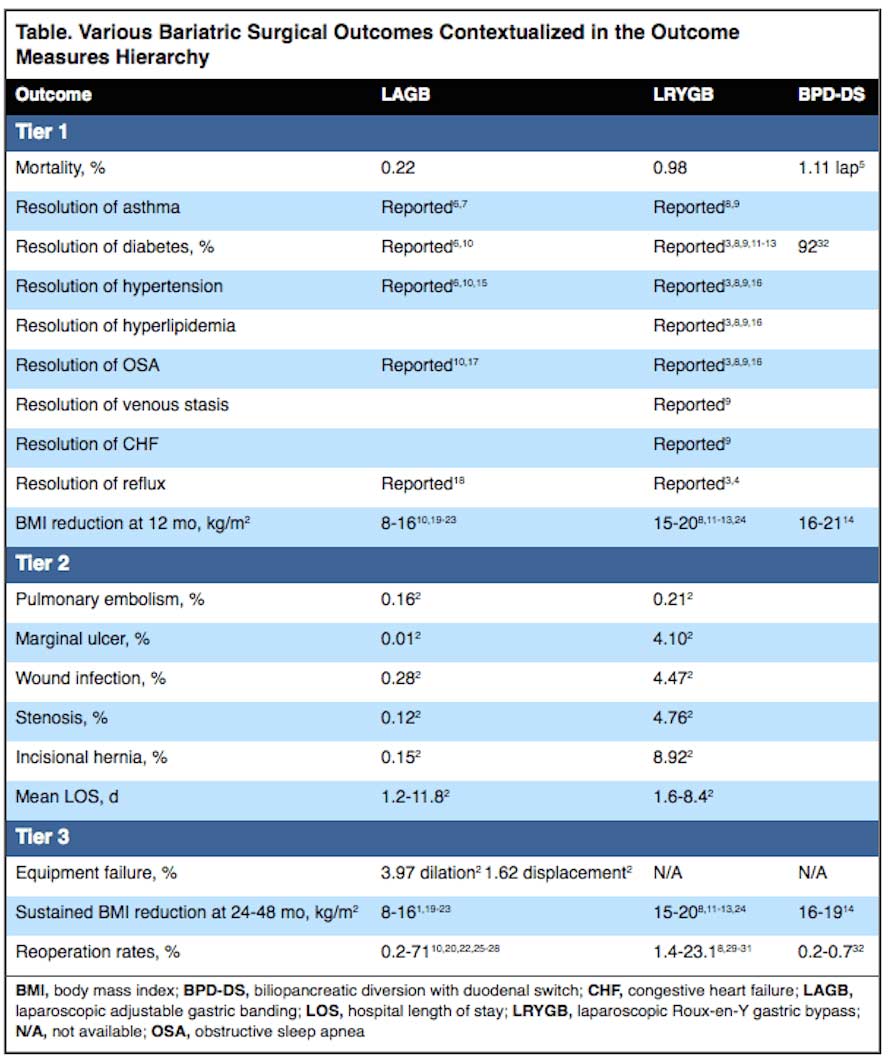
In a recent review article published in the September 2015- Volume 42:10 of General Surgery News, the surgical outcomes of different procedures were summarized. There were evaluated based on a number of measures, including re-operation rates. So interesting to note that the re-operation rate of the duodenal switch is the lowest of all surgical procedures.
Adjustable gastric banding had the highest reported re-operation rate. To be noted is the longer the time lapse the higher the need for re-operation for the band.
Original article here.
Alcohol and Weight Loss Surgery Webinar May 20, 2015
July 27, 2015 7:27 am
Informed Surgical Consent
July 18, 2015 9:39 pm
Surgical informed consent is the document that summarizes the discussion that has been carried out between the treating physician and the patient. It also outlines the expectations as well as the potential complications of the treatment being proposed.
An informed consent should mean that the patient is absolutely clear as to the procedure agreed upon and that is reflected on the consent. No abbreviations are allowed on the consent forms. Clearly, there are instances when a physician or surgeon providing service may have to deviate from the proposed plan and agreed upon procedure on the consent because of unexpected findings in the operating room.
Any patient undergoing surgery should be acutely aware of the terminology and the language used. With regards to weight loss surgical procedures, RNY and GB is not acceptable because they are both abbreviations.
Duodenal Switch is a distinct well described procedure with its unique identifiable code (43845 for open procedure) that is recognized by hospitals, insurance companies and the surgical societies.
Duodenal Switch operation is not SADI, SIPS nor a loop Duodenal switch. Any attempt to interchanges these terms or operations is inaccurate the say the least.
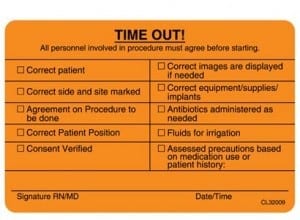
A surgical informed consent is signed by the patient ( or the guardian) and the treating physician. This document however is reviewed and confirmed by all those involved in the patient’s care delivered in the hospital. The consent is reviewed by the admission staff when taking the patient for surgery, preoperative nursing and administrative staff, operating room circulating nurse as well as the anesthesia staff. One step most patients may not be aware is initiated after the general anesthesia is induced. The operating room staff, anesthesia staff and the operating physician all go through a set of checklist known as “Time out”.
“Time out” involves confirming the patient’s identification as well as the proposed procedure as the patient had discussed with the staff and confirming the consent.
It is imperative that a patient have complete understanding of their surgical options available to them and critical that they have full knowledge of the type of surgical procedure that has been consented to and performed.
Iron Deficiency & Anemia July 15, 2015 Webinar RecordingExclusive Member Content
July 16, 2015 1:52 pm
Shared Success- Whitney a RNY to DS revision
June 09, 2015 7:43 am
I was always the big girl, pleasingly plump, chubby. I was put on my first diet at age 12. By the time I graduated High School I had yo-yoed up to 200 pounds at College graduation I was up to close to 300 pounds. In 2002 I had RNY Gastric Bypass surgery. I was 39 and weighted 280 pounds. I was told it was the Gold Standard. The Band was still considered experimental and the Duodenal Switch was never mentioned as an option. In fact, I did not even know it existed.
I lost 110 pounds and was considered a WLS success. I did not have any food restrictions and I felt great and maintained the loss for five years. Then I started to slowly gain weight. In little under 5 years I gained 70 pounds. I developed Dumping Syndrome and my Stoma was stretched out. I joined Weight Watchers and lost 5 pounds in a year. Nothing worked. I developed ulcers, osteoarthritis, planter fasciitis and could barley walk a couple of blocks without pain. I was miserable. I felt like a failure
In 2012 started to research surgical options. A local surgeon wanted to “revamp” my already tiny stomach, put a band around my stoma, and “clean up my intestines”. I asked about revision to Duodenal Switch and was strongly discouraged, but I wasn’t going to settle because that was what he was only capable of doing.
I wanted the best. I wanted long term success. So I travelled from Northern CA to Southern CA for a consult with Dr. Keshishian. The only choice for me was to revise to DS. In December of 2012, I had revision surgery of my RNY to Duodenal Switch. One week after surgery, still in the hospital, I went in for a second surgery. Dr. Keshishian found a small leak. I spent an additional two weeks in the hospital. My experience was not the norm and a leak can happen in any surgery involving the stomach.
Recovery was slow but steady. The first 2 weeks Dr. Keshishian called me every three days to make sure I was doing ok. I still have his cell number in my phone. I was back to work 14 weeks after surgery. I could have gone back sooner.
Over the past year I have lost 115 pounds. My BMI is 20, and I feel great. I have my life back. All pre-op issues have been resolved and I am going to start training for a 5K.
My advice for anyone contemplating Weight Loss Surgery is to research all of the options available. Do not settle for a substandard surgery. Get a second or even third opinion. It’s not a decision to be taken lightly. It’s your life fight for it!
Whitney B.
Neuromuscular Disease After Weight Loss Surgery
June 08, 2015 11:30 am
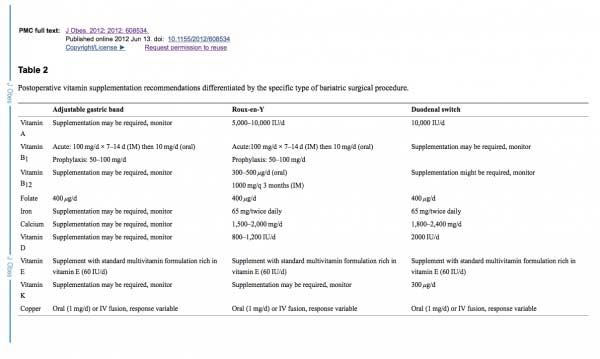
Weight loss surgical procedures may result in varying degrees of nutritional deficiencies. Some of these nutritional deficiencies may cause neuromuscular disease if left untreated, these include vitamins, minerals, and protein. The long-term effect of these deficiencies may presents as neuromuscular conditions including, weakness, numbness, confusion and all others if not-diagnosed and untreated. It is important to note that all weight loss surgical procedures require lifetime vitamin, mineral supplements and protein monitoring and possible supplements.
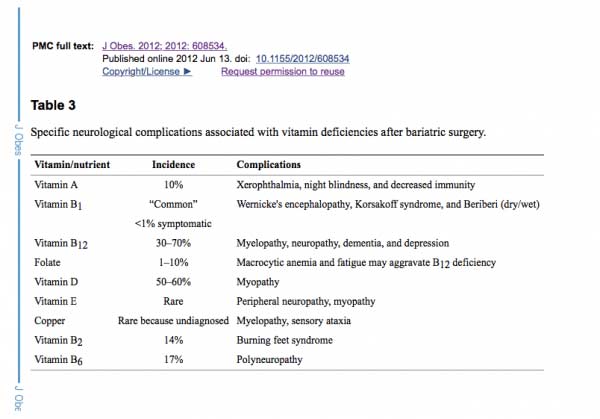
The table below outlines some of the specific neurological and neuromuscular disease complications following bariatric surgery. The most common deficiencies seen with the duodenal switch operation are fat soluble vitamin deficiencies. These include, Vitamin A, D, E and K. Duodenal Switch patients need oral supplements of Dry “Water Miscible” type of Vitamin A, D, E, and K based on their laboratory studies and needs.
The neurological deficiencies are manifested much more frequently with the Gastric Bypass than the duodenal switch operation. The most common nutritional deficients are that of B1, B12, Folate deficiencies that are common in Gastric Bypass. A list of possible neurologic deficiencies and there associated symptoms were summarized by Becker (2012). Another article with Nutritional Neuropathies.
Nutritional deficiencies are seen in a number of illnesses including weight loss surgery patients.
Duodenal Switch is a Safe Operation for Patients who have Failed Other Bariatric Operations
May 07, 2015 7:06 am
Obesity Surgery, 14, 1187-1192
Duodenal Switch is a Safe Operation for Patients who have Failed other Bariatric Operations
Ara Keshishian, MD, FACS; Karin Zahriya, MD, FACS; Teny Hartoonian, MD; Chris Ayagian, MD
Department of Surgery, Delano Regional Medical Center, Delano, CA, USA
Background: The incidence of morbid obesity and its surgical treatment have been increasing over the last few years. With this increase, there has been a rise in the number of patients who have had less than desirable outcome after bariatric operations. We perform the duodenal switch (DS) in patients for whom other weight loss surgical procedures have failed, because of inadequate weight loss, weight regain or significant complications, such as solid intolerance or dumping syndrome.
Method: From November 1999 to March 2004, 46 revisional surgeries were performed at our institution. The data was prospectively collected and reviewed, based on a number of parameters. Operative details, perioperative morbidity, and results are reported.
Results: 46 patients had their original bariatric surgical operation revised to DS. This resulted in complete resolution of their presenting complaints. The %EWL was 69% at the time of publication, with a mean lapsed time of 30 months.We had no mortality. Anastomotic leak occurred in 4 patients, 2 in our first
8 patients. We also noted that the majority of the patients were not aware of all the surgical procedures available to them at the time of their original operation.
Conclusion: In patients in whom gastroplasty, gastric bypass or both have failed to provide adequate weight loss, or worse have resulted in complications, DS can be performed as a safe revisional operation. The revision of other failed bariatric operations to DS results in both weight loss and resolution of the complications.
Introduction
Since its inception in the 1960s, weight loss surgery has been the only option for morbidly obese patients who have been unable to lose and maintain adequate weight loss through conventional non-surgical methods. In 1991, the NIH released a consensus on gastrointestinal surgery for severe obesity[1],which sparked further interest in the surgical treatment of morbid obesity, leading to an increase in the number of bariatric operations. This increase and the occasional failure and complications after these surgical procedures have resulted in an increased need for revisional surgery.
Bariatric procedures can be classified into three groups: those that restrict food intake, those that limit absorption, and those that utilize some degree of both components. Restrictive operations create a tiny neogastric pouch and a restrictive gastric outlet to decrease food intake.
Vertical banded gastroplasty (VBG) partitions the stomach along the lesser curvature, creating a channel restricted by an externally placed band. The upper pouch is approximately 5 cm long with a diameter of 1.5 cm and accommodates a volume of 20-40 ml. Gastric banding is another restrictive procedure, extensively performed in Europe and Australia, and recently in the United States. The published data varies significantly, with some reports showing <50% loss of excess body weight 9 years following the procedure.[2]
Roux-en-Y gastric bypass (RYGBP) is primarily restrictive, but also limits absorption of calories and nutrients to a varying degree. This procedure involves division of the stomach to create a tiny proximal pouch with approximate volume 15 ml. This pouch is then anastomosed to a Roux-en-Y jejunal limb, bypassing the stomach, pylorus and duodenum, adding a limited malabsorptive component. Although the original descriptions of RYGBP defined the Roux-limb to be <100 cm, in almost all of the RYGBP revisions, we have measured the Roux-limbs to be >100 cm.
The biliopancreatic diversion with duodenal switch (DS) is a hybrid operation involving both components of weight loss surgery. In the DS, a lateral gastrectomy provides a restricted gastric volume of approximately 100 cc, while excess fat absorption is limited by shortening the functioning length of the intestine. This involves diversion of the biliopancreatic secretions by partitioning the bowel into two limbs – an alimentary channel, and the biliopancreatic (afferent) limb. These two limbs of small bowel are reconnected to form the common channel.[3][4] DS appears to be the most effective bariatric operation to date. It produces the most sustained weight loss, without the unwanted side effects present with other bariatric operations (i.e. dumping syndrome, marginal ulceration, and solid food intolerance).[5][6] This is accomplished without any increase in the perioperative morbidity and mortality rate.
Restrictive operations have had varying results in long-term weight loss and complications.[7] Van Gemert et al.[5] reported a 12% incidence of revision after RYGBP and a 56% incidence of revision after VBG.[8] The need for revision after gastric banding has also been reported.[2][9]
Revision of failed bariatric procedures has resulted in morbidity rates of 12-41%. The perioperative revision complication rate has been three times higher when compared to a primary procedure. Gagner reported a morbidity rate of 22%.[10]
Behrns et al.[11] studied the choice of procedure for revisional surgery. They reported that when the primary operation had been a VBG, the most effective second operation was the RYGBP. The question arises as to what revisional surgery should be performed for failed RYGBP. The majority have been revised to a distal RYGBP. [11][12][13][14] However, Fobi et al.[14] showed that this was accompanied by only moderate weight loss and a protein malnutrition rate of 23%. Owens[15] and Schwartz[16] advised against revision of an operation performed satisfactorily, to one of the same type, because it is unlikely to produce a significant benefit.
Between November 1999 and March 2004, we performed 614 primary DS operations with excellent weight loss and minimal (<2%) hypoalbuminemia. During the same period, we elected to perform the DS as our revision operation of choice on 47 referred patients, and the data on the latter are hereby presented.
Methods
From November 1999 to March 2004, 47 patients were referred to us for revision to a DS, a period when 614 primary DS operations were performed. The primary operation for the patients seeking revision had been VBG (16), RYGBP (26), and both (5). The five patients with both procedures had an initial VBG, later revised to a RYGBP and were now presenting for their second revision. All of our patients who underwent revisional surgery had either regained all (31) or some (>50% – 7) of their original weight loss, or had failed to lose sufficient weight (9). The other presenting complaints were: severe dumping syndrome (20); intolerance to solid foods (16); persistent nausea and vomiting (4); and severe gastroesophageal reflux disease (14) (Table 1).
In this series, all 19 patients who had severe dumping syndrome had also regained a significant amount of weight. This appears to contradict the notion that dumping syndrome is a beneficial sideeffect of RYGBP as a behavior modification tool.
All patients were assessed by the surgeon, and had psychological, nutritional and medical evaluations. Extensive preoperative education was carried out to
[table id=1 /]
ensure adequate informed consent, and to bolster postoperative compliance. The work-up before revisional surgery included: complete metabolic panel; mineral, vitamin and lipid profile; liver function tests; upper GI series, and upper endoscopy.
Surgical Technique
The revision of any previous bariatric operation to DS involves a thorough study of the patient’s existing anatomy. The work-up includes review of prior medical records whenever available, as well as a detailed examination of the patient, followed by an upper GI series and an endoscopy performed at our institution by the operating surgeon. The peritoneal cavity is entered through a midline laparotomy incision.
Revision from VBG to DS entails exposure of the greater curvature of the stomach by ligation of the short gastric vessels. The stomach is then accessed through a gastrotomy at the greater curvature. A linear stapler is then used to divide the band through the gastrotomy and the distal end of the vertical partitioned stomach. Lateral vertical subtotal gastrectomy is accomplished over a 39-Fr bougie. The gastrectomy resection line includes the previous VBG staple-line, to prevent ruminant gastric tissue with compromised blood supply.
Revision of the RYGBP to DS involves a significantly greater degree of planning. The earlier open Roux-en-Y procedures were more likely to have left behind a larger stomach pouch with an intact left gastric artery than those performed laparoscopically. The reason for this is that most of the pouches were based on the greater curvature (horizontal), and little dissection was performed involving the lesser curvature. With the laparoscopic RYGBP procedures, the gastrojejunostomy anastomosis has been performed on the lesser curvature, and the left gastric artery has been frequently transected. Without the short gastric arteries, the pouch relies on the esophageal branches for its blood supply. The Lap-RYGBP patients have smaller pouch sizes and are exposed not only to an increased risk of leaks, but also have the potential for occurrence of stricture as a result of the tenuous blood supply. This may explain the high incidence of gastro-jejunostomy strictures needing balloon dilatation after lap- RYGBP.
Revision of RYGBP to DS involves taking down the gastro-jejunostomy anastomosis without compromising the blood supply of the proximal gastric pouch. The greater curvature of the bypassed stomach is then mobilized by ligation of the short gastric vessels to the level of the splenic hilum. The gastric continuity is then reconstructed by linear or circular staple firing between proximal stomach pouch and the gastric fundus of the mobilized bypassed stomach through a gastrotomy opening on the greater curvature. The staple-line is then over-sewn by a 3- 0 Vicryl® in a running fashion. A lateral vertical subtotal gastrectomy is then performed over a 39-Fr bougie. This gastrectomy now includes both the previous gastric pouch and the bypassed stomach in continuity.
Small bowel continuity is restored by first taking down the Roux-limb, and reconnecting it in a sideto- side fashion at the previously placed biliopancreatic limb. The total length of the small bowel is measured on the anti-mesenteric side. The common channel and alimentary limbs are then based on the percentage of the total length of the bowel (8%-12% for common, and 35%-45% for the alimentary). All of the small bowel entero-enteric anastomoses, with the exception of the duodeno-ileostomy anastomosis, are done in a side-to-side fashion as previously described.[17]
The duodenal switch is then performed by first dividing the duodenum 5 cm distal to the pylorus. The alimentary tract is then pulled through a retrocolic plane to the right of the middle colic artery, and an end-to-side anastomosis is created between the end of the transected proximal duodenum and the anti-mesenteric side of the small bowel, with a linear stapler, reinforced with a 3-0 Vicryl® in a running fashion.
All patients also undergo liver biopsy, appendectomy and cholecystectomy at the time of the revision operation. A feeding jejunostomy tube is routinely inserted in the biliopancreatic limb distal to the ligament of Treitz, in all revisional operations.
Results
The mean age of the patients was 47.3 (33-64), 3.3 years older than the average age for primary DS. Average pre-revision body mass index (BMI) was 47.3 kg/m2 (range 24.5-73.7), and average pre-revision weight was 128.3 kg (range 76.0 to 214.3). This is comparable to averages of 50.6 kg/m2 and 143.4 kg respectively, for primary DS. The average time elapsed between the primary operation and revision was 11.8 years (range 2.7 to 23). The female to male ratio was 9:1 compared with 6:1 in our primary DS patients.
A questionnaire administered to all revision patients at the time of the initial presentation, revealed that 96.2% of patients had been unaware of other surgical weight-loss options at the time of their primary operation, even though at the time the other bariatric operations were available.
The findings on preoperative radiological and endoscopic evaluation are shown in Tables 2 and 3. [table id=2 /] [table id=3 /].
The average operative time for revisional patients was 3.5 hours (2.3-5.7), and the average length of stay was 4.8 days. For primary DS, this has been 1.7 hours and 3.2 days, respectively.
Peri-operative complications included leaks in four patients (8.5%), one wound infection (2.1%), and one hernia (2.1%). All four of our patients who had leaks had undergone a previous RYGBP. Two of the four patients had undergone both a VBG and a RYGBP, and DS was their second revision. Two leaks occurred in the first 8 patients, and the remaining 2 in the following 38 patients. Two of the leaks were at the site of gastro-gastrostomy anastomosis, and the other two were located at the site of the lateral gastrectomy, just proximal to the gastro-gastrostomy anastomosis. Two of the four patients with leaks required further surgical interventions to completely resolve their complications. The other two were treated with enteral feeding and NPO, with drainage by means of the closed suction drains placed at the time of the operation. There has been no protein malnutrition and no deaths. The leak-rate for our primary DS patients has been 0.9%
Following a mean elapsed time of 30 months since revision to DS, the average BMI has dropped from 48.9 to 29.2 kg/m2 and the %EWL has been 67%. Mean weight has fallen from 128 kg to 80 kg (P<0.0001). The presenting complications of the original surgery have resolved in 100% of patients who underwent revision to DS. The BMI has remained stable after revision of failed VBG and RYGBP at 2.4 years after the DS. The data is summarized in Table 4.[table id=5 /]
Discussion
As more patients undergo bariatric surgery for treatment of morbid obesity, an increase in the number of patients with the need for revision are encountered. In our experience, the most common indication for re-operative surgery was inadequate weight loss (15 out of 35 patients, 43%). This has been confirmed by others. The reason could be due to a technical failure (eg. anastomotic dilatation, staple-line disruption). In the majority of the patients, however, we found no clear technical explanation for the failure of the operation. In restrictive operations such as VBG, patients recognize the smaller capacity of their postoperative stomach, and frequently modify their diet to comprise mainly high-calorie liquids or foods such as ice-cream and milkshakes.[7] Intolerance to solid foods related to stricture or stenosis also makes patients resort to this type of diet. Gawdat[18] found that 61% of revised patients had had no abnormality found at the time of the revisional operation.
The average BMI of our patients at the time of their primary operation had been 51.8 kg/m2. Problematic weight loss in the super-obese has led to the proposition that some degree of malabsorption should be incorporated into bariatric operations in these patients.[19] We agree with this, and we recommend that the DS be the primary operation of choice for patients with super-obesity.
Revision from a primary restrictive operation to DS involves complete conversion of the previous operation to essentially normal anatomy before the DS operation is completed. This necessitates working on a gastric pouch or remnant with tenuous blood supply. Paying heed to this danger during the operation has allowed us to limit our complication rates to those of previously published data. It is evident from our experience that the rate of complications such as leaks is increased in revisional operations. Complication rates are higher after RYGBP revision, and 100% of our leaks occurred in patients with prior RYGBP.
Gastric bypass has been shown to have better weight loss than VBG, justifying previous revision of failed VBG. However, DS has been shown to have better overall and long-term weight loss than the RYGBP. Therefore, our revision patients should have better results than if they had been revised to another to RYGBP.
With regards to patients with failed RYGBP, the options promoted by others have been to revise to another RYGBP, or to add a malabsorptive component by lengthening the Roux-limb (i.e. distal gastric bypass). Neither option has been very successful. As reported by Fobi[14] and by Sugerman,[20] problems with protein malnutrition occasionally follow distal RYGBP. Others have opted to manage these patients with strict diets and anorectic drugs. These modalities failed before weight-loss surgery in these patients, and are unlikely to be beneficial at this stage. Our decision to convert failed RYGBP patients to DS has led to good weight loss results. Additionally, we have encountered no issues of protein malnutrition, partly because a larger stomach is left with DS compared to RYGBP.[21][22] The average size of the stomach remaining after primary DS or after DS for previously failed bariatric surgery is approximately 100 cc.
Conversion to DS resulted in weight loss in all patients, with an average weight loss per month of 5.4 kg (range 0.3-16.1). However, the increased risk of complications following the re-operation implores serious consideration of the primary reason for the revision. We believe that if the presenting complaint is exclusively that of weight gain or inappropriate weight loss, the increased risk does not warrant revision in patients whose preoperative BMI is lower than the guidelines set by the National Institutes of Health.1 However, in patients presenting with primary surgical complications, such as dumping syndrome, intolerance to solids or persistent nausea and vomiting, where the patient’s quality of life has deteriorated, DS is a highly successful procedure. Our data indicates that 100% of initial complaints were resolved following revision.
The other major consideration in revisional bariatric surgery is patient education. In this study, 96.2 % of the patients claimed that they were unaware of other weight-loss surgical options at the time of their primary operation. One could possibly question the validity of the informed consent at the time of the original operation. Our program incorporates an extensive preoperative education plan geared towards explaining the DS procedure in detail, clarifying the general risks of surgery, the resulting change in anatomy and the long-term follow- up requirements, including supplementation requisites to maintain vitamin, mineral and nutritional levels within normal limits. Patients undergoing DS as their primary operation are in addition required to attend group meetings for all other surgical procedures, in order to assure adequate informed consent. The surgeon has the duty to provide the patient with the information necessary for the patient to make an educated decision as to whether to consent to the recommended operation. For a patient to properly make that decision, all major surgical options, their advantages and disadvantages must be discussed. Patients who are fully aware of all their weight loss surgery options, will better select their primary operation, and will likely decrease their need for future revisional surgery. In our practice, we recommend that our patients not only attend group meetings but also seek a second opinion regarding other bariatric surgical procedures.
References:
[1. Gastrointestinal surgery for severe obesity. National Institutes of Health Consensus Development Conference Draft Statement. Obes Surg 1991; 1: 257-66]
[2. Martiknainen T, Pirinen E, Alhava E et al. Long-term results, late complications and quality of life in a series of adjustable gastric banding. Obes Surg 2004; 14: 648-54]
[3. Hess, DS, Hess DW. Biliopancreatic diversion with a duodenal switch. Obes Surg 1998; 8: 267-82]
[4. Marceau P, Hould FS, Simard S et al. Biliopancreatic diversion with duodenal switch. World J Surg 1998; 22: 947-54]
[5. Biron S, Hould FS, Lebel S et al. Twenty years of biliopancreatic diversion: what is the goal of surgery? Obes Surg 2004; 14: 160-4]
[6. Rabkin RA. The duodenal switch as an increasing and highly effective operation for morbid obesity. Obes Surg 2004; 14: 861-5]
[7. Arribas del Amo D, Martinez Díez M, Elía Guedea M et al. Vertical banded gastroplasty: is it durable operation for morbid obesity? Obes Surg 2004; 14: 536-8]
[8. van Gemert WG, van Wersch MM, Greve JWM et al. Revisional surgery after failed vertical banded gastroplasty: Restoration of vertical gastroplasty or conversion to gastric bypass. Obes Surg 1998; 8: 21-8]
[9. Chevalier JM, Zinzindohoué F, Douard R et al. Complications of laparoscopic adjustable gastric banding for morbid obesity: experience with 1,000 patients over 7 years. Obes Surg 2004; 14: 407-14]
[10. Gagner M, Gentileschi P, De Csepel J et al. Laparoscopic reoperative bariatric surgery: lessons learned to improve patients selection and results. Ann Surg 1993; 218: 646-53]
[11. -]
[12. Jones KB Jr. Revisional bariatric surgery – safe and effective. Obes Surg 2001; 11: 183-9]
[13. Benotti PN, Forse RA. Safety and long-term efficacy of revisional surgery in severe obesity. Am J Surg 1996; 172: 232-5]
[14. Fobi MAL, Lee H, Igwe D Jr et al. Revision of failed gastric bypass to distal Roux-en-Y gastric bypass: A review of 65 cases. Obes Surg 2001; 11: 190-5]
[15. Owen BM, Owen ML, Hill CW. Effect of revisional bariatric surgery on weight loss and frequency of complications. Obes Surg 1996; 6: 479-84]
[16. Schwartz RW, Strodel WE, Simpson WS. Gastric bypass revision: Lessons from 920 cases. Surgery 1988; 104: 806-12]
[17. Keshishiam A, Zahriya K. Stapled Roux-en-Y anastomosis: an illustrated technique. Obes Surg 2003; 13: 450-2]
[18. Gawdat K. Bariatric reoperations: are they preventable? Obes Surg 2000; 10: 525-9]
[19. Dolan K, Hatzifotis M, Newbury L et al. Comparison of laparoscopic adjustable gastric banding and biliopancreatic diversion in super-obesity. Obes Surg 2004; 14: 165-9]
[20. Sugerman HJ, Kellum JM, De Maria EJ. Conversion of proximal to distal gastric bypass for failed gastric bypass for superobesity. J Gastrointest Surg 1997; 1: 517-25]
[21. Yashkov YI, Oppel TA, Shishlo LA et al. Improvement of weight loss and metabolic effects of vertical banded gastroplasty by an added duodenal switch procedure. Obes Surg 2001; 11: 635-9]
[22. Rabkin RA, Rabkin JM, Metcalf B et al. Nutritional markers following duodenal switch for morbid obesity. Obes Surg 2004; 14: 84-91]
Copper InformationExclusive Member Content
April 17, 2015 7:21 am