Category: probiotics
Flagyl
September 25, 2019 9:07 am
Flagyl is sometimes prescribed for excessive gas and diarrhea. It is an antibiotics that works well on certain bacteria that accumulates in the GI tract and contributes to the gas and the bloating.
These bad bacteria flourish when patients consume significant and excessive fiber and carbohydrates (sugars, salad, pasta etc.) The FIRST line of defense against flatulence, bloating, and diarrhea should be eleminating the culprits in the diet. This point can not be stressed enough. Adding a daily dose of yogurt may improve symptoms due to yogurts probiotic benefits. To be beneficial, Yogurt should contain live bacteria cultures, not contain artificial sweeteners or have a high sugar content.
Artificial sweetness also area source of the excessive gas and should be avoided.
The Flagyl eliminates and reduces the bad bacteria. Along with a Probiotic and healthy dietary choices Flagyl can help to significantly improved or eliminate those symptoms of gas and diarrhea.
Before Flagyl is prescribed, it is important that the diet is critically examined to make sure that the carbohydrates and the fiber as source of gas and bloating is minimized or eliminated. Excessive use of medications that may be needed for other infections should be avoided.
Chronic diarrhea should be evaluated to rule out GI infection with C. diff bacteria or other bacteria or parasite.
Additional Information on C. Diff (Clostridium Difficile) and probiotics.
Gas (Flatuence) GI upsetExclusive Member Content
July 27, 2017 7:32 am
Gut Biome and Body Fat
October 06, 2016 7:02 am
The Gut Biome and body fat link continues to be an interesting and new front in the science of obesity. Although we know more factors in obesity it has remained an elusive multi-factorial process. The following article is yet another piece of the puzzle.
Study finds link between faecal bacteria and body fat “Researchers at King’s College London have found a new link between the diversity of bacteria in human poo – known as the human faecal microbiome – and levels of abdominal body fat.
The research, published today in Genome Biology, also provides further evidence of possible genetic influences on obesity, through heritable bacteria found in the faecal microbiome.”
View the rest of the article here. The research paper here.
Our past posts on gut biome and probiotics here
Probiotics and Prebiotics
May 26, 2016 1:59 pm
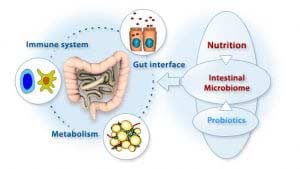
Probiotics and Prebiotics are an important part of our overall general and gastrointestinal health. The gastrointestinal (GI) tract is a large, muscular tube that allows the digestion of food. The intestinal lining of the tract plays a role in absorbing vital nutrients and acts as a barrier for the macromolecules and microorganism from circulation. Our GI system is exposed to many bacterial agents that undergo fermentation in the mucosa. The type of fermentation carried out in the gut is greatly influenced by the types of bacteria found in the lumen.
The GI microflora is an elaborate ecosystem consisting of neutral and beneficial bacteria whose balance impacts overall health. This microenvironment consists of about 400 different bacterial species that make up approximately 100 billion organisms in the gut. The flora functions in nutrient consumption, vitamin production, detoxification, hormone activity, and other regulatory processes. Abnormal microbial balance or colonization results in dysbiosis, where the deviant nature of bacteria may become pathological (7). Dysbiosis is a contributing factor to many degenerative and chronic diseases.
Benefits of Probiotics and Prebiotics:
Our bodies are full of both good and bad bacteria. Probiotics contain live bacteria and yeasts, whose activity is beneficial when present in appropriate amounts (11,12). These helpful microorganisms regulate the body’s systems in several ways:
- Gastrointestinal: Probiotics work to reduce infectious diarrhea, specifically types identified by antibiotic use (1). Certain strains enhance stool consistency and bowel movement frequency. Probiotics have also proven effective in alleviating bloating and gas found in irritable bowel syndrome (9). Further studies suggest that specialized strains aid in milder forms of ulcerative colitis, an inflammatory bowel disease. A recent Russian study suggested eradication of SIBO and IBS using a combination of Bifidobacterium bifidum, Bifidobacterium longum, Bifidobacterium infantis and Lactobacillus rhamnosus, called Florasan-D available in Russia. These findings were presented at the 2015 Gut Microbiota for Health World Summit in Barcelona, Spain by Elena Polouektova, MD, a researcher at I.M. Sechenov First Moscow State Medical University.
- Weight Loss: A clinical study (8) revealed reduced body fat in patients who consumed yogurt (probiotic source), although there were no observed changes in weight. Another study, published in the 2011 European Journal of Clinical Nutrition (6), found that subjects who consumed fermented milk that contained a specific bacterial strain observed abdominal fat and weight loss, when compared to subjects drinking a control.
- Immunity: Although the clinical implications of this evidence are still being studied, it has been found that immune response strength is greatly improved through certain strains of probiotics (2,4). They have also been shown to lighten hypersensitivity reactions and normalize added mucosal dysfunction.
- Other Uses: Bacteria also reside in the mouth. Probiotics play an essential role in oral health, where they reduce throat infection, bad breath and periodontal disease, a gum infection (5). There have been claims that probiotics lower the effects of some skin conditions, prevent colon cancer, lower blood pressure and cholesterol, and alleviate anxiety and depression (3). Future studies are working towards the consistency of these claims.
Probiotics regulate the movement of food through the digestive system. They help replace unwanted bacteria and maintain the mucosal microenvironment to avoid dysfunction. Prebiotics are fiber compounds that move through the GI tract undigested. Prebiotics are important in stimulating probiotic growth and maintaining a stable environment for their optimal activity (13). The best way to get all the powerful benefits of probiotics is through consuming foods that are prepared by bacterial fermentation. Supplements are also available. Previous blog regarding probiotic supplements here. Previous blog regarding probiotics, C.Diff and Hyperoxaluria here.
Written by: Mariam Michelle Gyulnazaryan & Dr. Ara Keshishian
References
- Bowen, J. M., Stringer, A. M., Gibson, R. J., Yeoh, A. S., Hannam, S., & Keefe, D. M. (2007). VSL# 3 probiotic treatment reduces chemotherapy-induced diarrhoea and weight loss. Cancer biology & therapy, 6(9), 1445-1450.
- Chiang, B. L., Sheih, Y. H., Wang, L. H., Liao, C. K., & Gill, H. S. (2000). Enhancing immunity by dietary consumption of a probiotic lactic acid bacterium (Bifidobacterium lactis HN019): optimization and definition of cellular immune responses. European journal of clinical nutrition, 54(11), 849-855.
- Foster, J. A., & Neufeld, K. A. M. (2013). Gut–brain axis: how the microbiome influences anxiety and depression. Trends in neurosciences, 36(5), 305-312.
- Isolauri, E., Sütas, Y., Kankaanpää, P., Arvilommi, H., & Salminen, S. (2001). Probiotics: effects on immunity. The American journal of clinical nutrition, 73(2), 444s-450s.
- Krasse, P., Carlsson, B., Dahl, C., Paulsson, A., Nilsson, A., & Sinkiewicz, G. (2005). Decreased gum bleeding and reduced gingivitis by the probiotic Lactobacillus reuteri. Swedish dental journal, 30(2), 55-60.
- Merenstein, D., Murphy, M., Fokar, A., Hernandez, R. K., Park, H., Nsouli, H., … & Shara, N. M. (2010). Use of a fermented dairy probiotic drink containing Lactobacillus casei (DN-114 001) to decrease the rate of illness in kids: the DRINK study A patient-oriented, double-blind, cluster-randomized, placebo-controlled, clinical trial. European journal of clinical nutrition, 64(7), 669-677.
- Myers, S. P. (2004). The causes of intestinal dysbiosis: a review. Altern Med Rev, 9(2), 180-197.
- Omar, J. M., Chan, Y. M., Jones, M. L., Prakash, S., & Jones, P. J. (2013). Lactobacillus fermentum and Lactobacillus amylovorus as probiotics alter body adiposity and gut microflora in healthy persons. Journal of functional foods, 5(1), 116-123.
- Prantera, C., & Scribano, M. L. (2009). Antibiotics and probiotics in inflammatory bowel disease: why, when, and how. Current opinion in gastroenterology, 25(4), 329-333.
- Reid, G., Jass, J., Sebulsky, M. T., & McCormick, J. K. (2003). Potential uses of probiotics in clinical practice. CLINICAL microbiology Reviews, 16(4), 658-672.
- Rolfe, R. D. (2000). The role of probiotic cultures in the control of gastrointestinal health. The Journal of nutrition, 130(2), 396S-402S.
- Sanders, M. E. (2008). Probiotics: definition, sources, selection, and uses. Clinical Infectious Diseases, 46(Supplement 2), S58-S61.
- Schrezenmeir, J., & de Vrese, M. (2001). Probiotics, prebiotics, and synbiotics—approaching a definition. The American journal of clinical nutrition, 73(2), 361s-364s.
Probiotics, C. diff & Enteric HyperoxaluriaExclusive Member Content
July 26, 2014 3:21 pm
Bloating and Excessive Gas
April 17, 2012 7:36 am
The relationship between the consumption of food, bloating, and excessive gas is a subject that comes up frequently. In our practice, this is a complaint usually raised 3 or 4 years after receiving the duodenal switch operation. It appears that patients eventually disregard the recommendations made for a healthier diet of low carbohydrate, high protein, hydration, supplements, and then everything else.
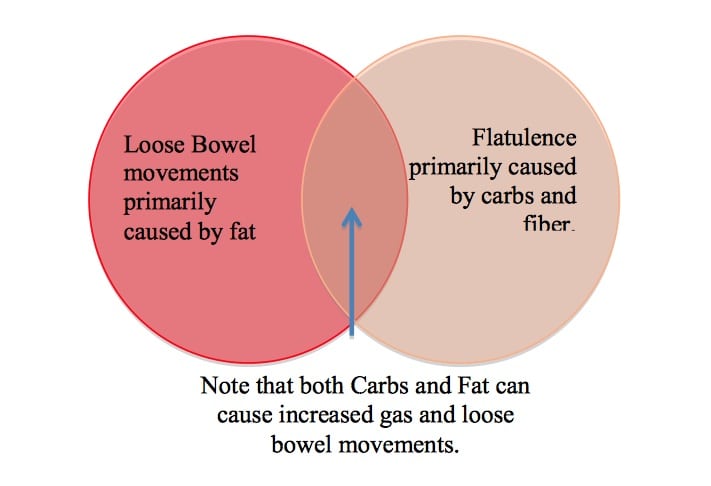
In general, carbohydrates, carbonated drinks, artificial sweeteners (such as Splenda®, sugar alcohols, etc.), vegetables, excessive amounts of food, and an intake of fat will cause significant gas and bloating. This is not to be taken out of context and assumed that one cannot consume any of these products. However a diet that has fruits and vegetables will cause significant gas and bloating. These can not be controlled by probiotics, antibiotics, or other products such as Beano.
Simple carbohydrates/sugars (sugar, candy, cakes, cookies, pies, regular soda pop, jelly, jam, syrup, ice cream, sherbet, and sorbet, etc.) are easily absorbed. Simple carbohydrates/sugars can increase diarrhea due to the Duodenal Switch allowing more undigested sugars/fuel for intestinal bacteria to feed upon, multiply and form gas. The end result can be gas, bloating, and diarrhea.
Complex carbohydrates have more structure than simple carbohydrates/sugar which are harder for the intestinal bacteria to break down and may cause less bloating, gas and diarrhea. Also, complex carbohydrates usually contain higher fiber content. The fiber in the colon will help to absorb water from the stool and can reduce diarrhea. However, this is not the case for all Duodenal Switch patients.
When a patient reports these problems, I recommend that the consumption of all carbonated drinks should be stopped. No patient should consume carbonated drink of any sort. Artificial sweeteners should also be avoided all together. A good alternative would be honey, maple syrup or Stevia. Minimize or reduce the carbohydrate intake.
It has been our experience in the majority of cases that excessive gas and bloating is a result of dietary indiscretion. In some patients, once the dietary sources have been ruled out, it should be further evaluated by a barium enema to rule out the diagnoses of a redundant colon.
The best approach would be to first go back to a high protein and low carbohydrate. This should allow a patient to rule out any dietary sources for the bloating and excessive gas. It is recommended to next be seen by your physician for a further workup.
To summarize, when a patient has excessive amount of gas, diarrhea and bloating, the first line of treatment is elimination of all of the possible causes. These include carbohydrates, fruits, vegetables, artificial sweeteners, carbonated drinks and milk products. I can not overemphasize the importance of this step prior to anything else such as antibiotics or probiotics.
“Gas problem”
March 25, 2011 3:15 am
Prebiotic Potential Of Almond
July 01, 2008 7:07 pm
Almonds, as well as being high in vitamin E and other minerals, are also thought to have other health benefits, such as reducing cholesterol. Recently published work by the Institute of Food Research has identified potential prebiotic properties of almonds that could help improve our digestive health by increasing levels of beneficial gut bacteria.
Our digestive system maintains large population of bacteria that live in the colon. Prebiotics are non-digestible parts of foods that these bacteria can use to fuel their growth and activity. These ‘good’ bacteria form part of our body’s defense against harmful bacteria and play a role in the development of body’s immune system. The prebiotics work by stimulating the growth of these bacteria. However, in order to get to where they are needed prebiotics must be able to get through the upper part of the intestine without being digested or absorbed by the body.
Funded by the Almond Board of California, IFR scientists first used the Model Gut, a physical and biochemical simulator of the gastro-intestinal tract, to subject almonds to the same conditions experienced in the stomach and small intestine. They then added the digested almonds to an in vitro batch system to mimic the bacterial fermentation in the large intestine and monitored its effect on the populations of intestinal bacteria.
The study, published in Applied and Environmental Microbiology, found that finely ground almonds significantly increased the levels of certain beneficial gut bacteria. This effect was not seen when the fat content was removed from the almond preparation, suggesting that the beneficial bacteria use the almond lipid for growth, and this is the basis for the prebiotic effect of almonds.
Previous studies have shown that the amount of available lipid is reduced if the almonds are not processed, for example by grinding as in this study or by chewing. The length of time the almond spends in the digestive system also affects the amount of available lipids and proteins. More detailed studies on the digestibility of almonds are now required, and the prebiotic effect of almond lipids needs to be tested in human volunteers.
Health benefits of taking probiotics
Bacteria have a reputation for causing disease, so the idea of tossing down a few billion a day for your health might seem — literally and figuratively — hard to swallow. But a growing body of scientific evidence suggests that you can treat and even prevent some illnesses with foods and supplements containing certain kinds of live bacteria. Northern Europeans consume a lot of these beneficial microorganisms, called probiotics (from pro and biota, meaning “for life”), because of their tradition of eating foods fermented with bacteria, such as yogurt. Probiotic-laced beverages are also big business in Japan.
Enthusiasm for such foods has lagged in the United States, but interest in probiotic supplements is on the rise. Some digestive disease specialists are recommending them for disorders that frustrate conventional medicine, such as irritable bowel syndrome. Since the mid-1990s, clinical studies have established that probiotic therapy can help treat several gastrointestinal ills, delay the development of allergies in children, and treat and prevent vaginal and urinary infections in women.
Self-dosing with bacteria isn’t as outlandish as it might seem. An estimated 100 trillion microorganisms representing more than 500 different species inhabit every normal, healthy bowel. These microorganisms (or microflora) generally don’t make us sick; most are helpful. Gut-dwelling bacteria keep pathogens (harmful microorganisms) in check, aid digestion and nutrient absorption, and contribute to immune function.
The best case for probiotic therapy has been in the treatment of diarrhea. Controlled trials have shown that Lactobacillus GG can shorten the course of infectious diarrhea in infants and children (but not adults). Although studies are limited and data are inconsistent, two large reviews, taken together, suggest that probiotics reduce antibiotic-associated diarrhea by 60%, when compared with a placebo.
Probiotic is a nondigestible supplement. a dietary supplement in the form onondigestible carbohydrate that fthe growth of desirablemicroflora in the large bowel.
Probiotic is a substance containing beneficial microorganisms: a substance containing live microorganisms that claims to be beneficial to humans and animals, e.g. by restoring the balance of microflora in the digestive tract.
Probiotic therapy may also help people with Crohn’s disease and irritable bowel syndrome. Clinical trial results are mixed, but several small studies suggest that certain probiotics may help maintain remission of ulcerative colitis and prevent relapse of Crohn’s disease and the recurrence of pouchitis (a complication of surgery to treat ulcerative colitis). Because these disorders are so frustrating to treat, many people are giving probiotics a try before all the evidence is in for the particular strains they’re using. More research is needed to find out which strains work best for what conditions.
Probiotics may also be of use in maintaining urogenital health. Like the intestinal tract, the vagina is a finely balanced ecosystem. The dominant Lactobacilli strains normally make it too acidic for harmful microorganisms to survive. But the system can be thrown out of balance by a number of factors, including antibiotics, spermicides, and birth control pills. Probiotic treatment that restores the balance of microflora may be helpful for such common female urogenital problems as bacterial vaginosis, yeast infection, and urinary tract infection.
Many women eat yogurt or insert it into the vagina to treat recurring yeast infections, a “folk” remedy for which medical science offers limited support. Oral and vaginal administration of Lactobacilli may help in the treatment of bacterial vaginosis, although there isn’t enough evidence yet to recommend it over conventional approaches. (Vaginosis must be treated because it creates a risk for pregnancy-related complications and pelvic inflammatory disease.) Probiotic treatment of urinary tract infections is under study.
Probiotics are generally considered safe — they’re already present in a normal digestive system — although there’s a theoretical risk for people with impaired immune function. Be sure the ingredients are clearly marked on the label and familiar to you or your health provider. There’s no way to judge the safety of unidentified mixtures.
In the United States, most probiotics are sold as dietary supplements, which do not undergo the testing and approval process that drugs do. Manufacturers are responsible for making sure they’re safe before they’re marketed and that any claims made on the label are true. But there’s no guarantee that the types of bacteria listed on a label are effective for the condition you’re taking them for. Health benefits are strain-specific, and not all strains are necessarily useful, so you may want to consult a practitioner familiar with probiotics to discuss your options. As always, let your primary care provider know what you’re doing,