Category: Surgical
GI Bleed following Weight Loss Surgery
September 17, 2018 10:28 am
Gastrointestinal (GI) Bleed following weight loss surgery is rare but does require knowledge of the particular bariatric surgical procedure the patients has and how to proceed with diagnostics to fully evaluate the situation. Acute or chronic gastrointestinal bleeding can cause anemia in patients. However, Anemia may also be caused by nutritional deficiencies (iron, vitamin , minerals), Kidney disease, bone marrow disease and others. The work-up for anemia following weight loss surgery follows a routine protocol. If there is an evidence of bleeding from intestine (bloody emesis, bloody bowel movement, “tar” like black bowel movements) then the diagnostic work up would include an upper and lower endoscopy.
Endoscopic Procedures:
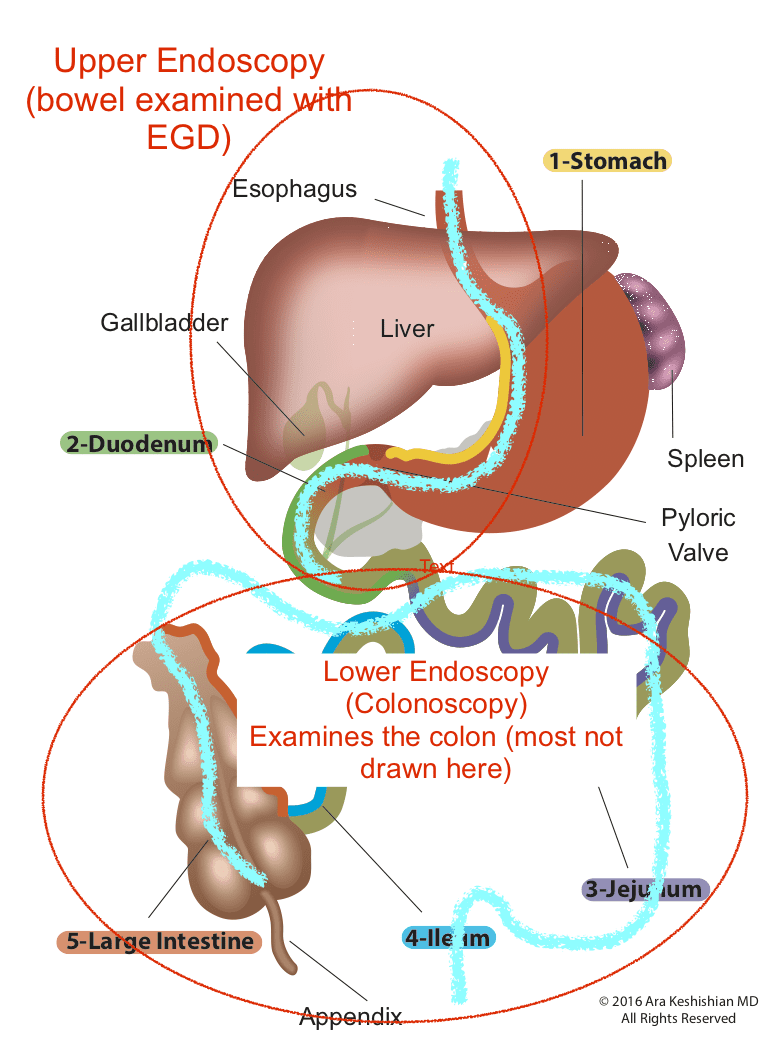
Upper endoscopy Esophagogastroduodenoscopy (EGD): evaluates the esophagus, stomach and a limited area of the duodenum past pyloric valve.
Lower endoscopy Colonoscopy or coloscopy: evaluates the rectus and the entire colon.
Between these two tests, there is still a considerable amount of the small bowel that is not accessible or visualized with endoscopic procedures. For the small bowel, examination Capsule endoscopy is an option in an intact GI tract. Patients who have had Gastric bypass RNY or the Duodenal Switch, the large segments of the small bowel can not be visualized or examined with capsule endoscopy.
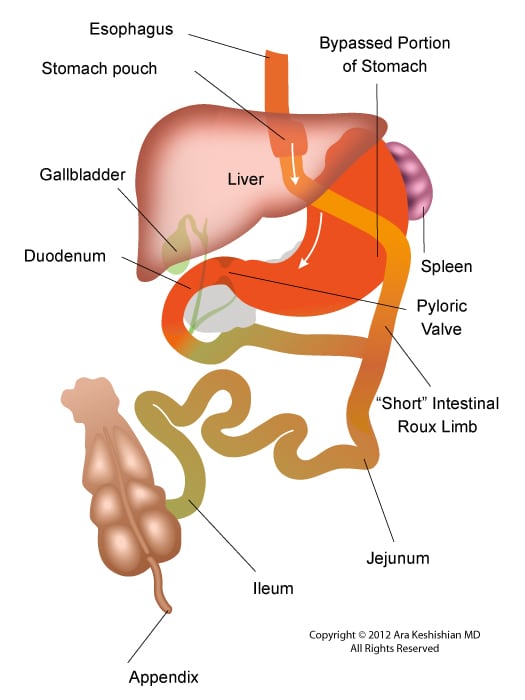
Patients who have had Duodenal Switch, Gastric Bypass and SADI – S would need a tagged red cell scan or CT angiography if GI bleed is suspected in areas of the small intestine that are inaccessible by endoscopic procedures.
New Pasadena Office Map and Parking
August 12, 2017 8:35 am
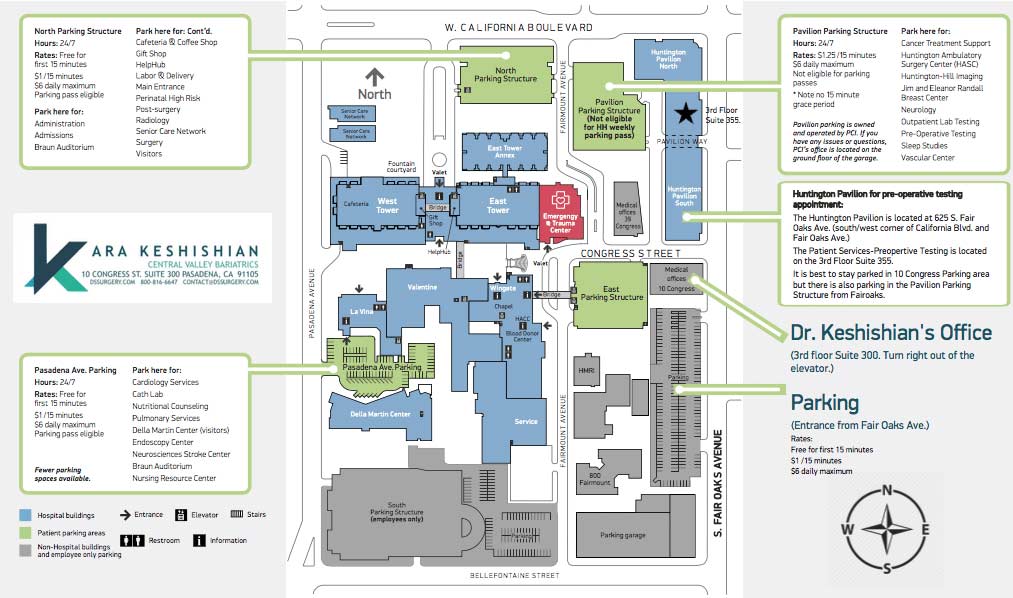
We’ve created a helpful map and parking diagram for our new Pasadena, CA office location. It also has a general layout of the Huntington Memorial Hospital Campus and Pre-operative intake and testing area. We hope that you find it helpful on your next visit to see Dr. Ara Keshishian, General and Bariatric Surgeon.
Dr. Ara Keshishian has performed more than 2,000 Duodenal Switch procedures, thousands of Sleeve Gastrectomies and more than 500 revisions from other Weight Loss Surgeries such as RNY Gastric Bypass, Adjustable Gastric Band, and Sleeve Gastrectomy to Duodenal Switch as well as General Surgical cases over the last 18 years of private practice.
Seroma
September 21, 2016 12:06 pm
A seroma is a collection of a serum that builds up under the skin or between tissue layers, usually at surgical sites or where tissues has been removed. The development of a seroma usually doesn’t appear for a week or so after surgery or drains are removed.
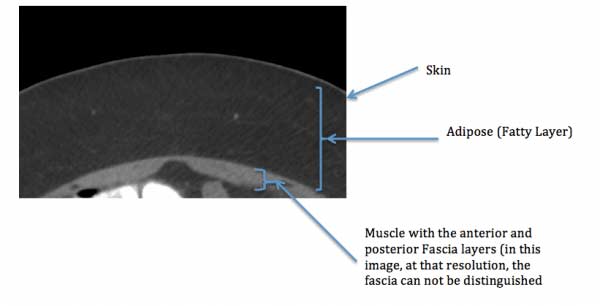
The best way to understand a seroma formation at an abdominal site is to know the anatomy of the abdominal wall. The abdominal wall has a number of distinct layers. Starting from outside to inside they are: the skin, adipose (fatty layer), muscle and then the peritoneal. I should mention that this is over simplification since depending on what part of the body we are specifically looking at the thickness of each layer may be different. Additionally, there may be other fascia or muscle layers that overlap at certain places that do not for example in the midline.
The skin is self explanatory, it is a protective layer.
The fatty layer, underneath the skin layer, is where energy is stored. The key with this layer is that there are very few blood vessel and lymphatic channels located in this layer. From a metabolic standpoint, fat is not very active so there is no need for it to have significant amount of circulation, unlike a skeletal muscle that may be involved with movement of large bones for example.
The muscle layer is well drained by lymphatic system and has excellent venous and arterial supply and drainage.
The peritoneal cavity is where the organs are encased with in the peritoneum (thick membrane).
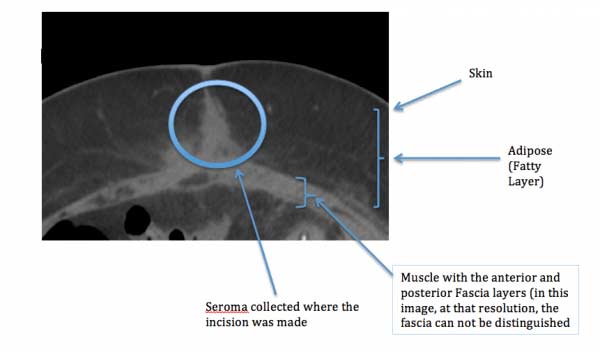
When an incision is made, it traverses thru all the planes of the abdomen, from the skin all the way down to peritoneal. The fatty layer, as mentioned above lack lymphatic channels and drainage. Its’ blood supply, arteries and veins are sporadic. This results in an environment with poor drainage properties. Any small amount of fluid either left behind from irrigation, or any fluid that collects in the tissue, caused by the swelling , inflammation which results from the injury of the surgery, can potentially collect.
There are a number of ways to help prevent seroma formation, however, depending on the individual, their health status, inflammatory response, healing process, medications, etc. they may still form. In order to provide for a way for the fluid to drain a number of things can be done. Sometimes different drains are placed within the fatty layer allowing the fluid to drain out or collect in the drain. Another technique is to close the incision with skin staples far apart, allowing the fluid to drain between the staples. I close the incisions with the absorbable stiches, but leave the top and the bottom of the incision open by 1cm (1/4”). These openings in the incision allow for natural drainage of fluids out of the abdominal space, which we want. These openings also allow me to gently place a sterile q-tip in the office to make sure there is no fluid collection and to drain if any has formed. Wearing compression binders or garments can help to reduce swelling and risk of seroma formation.
As healing takes place seromas may reoccur and need draining. Although they are bothersome seromas are rarely serious and will eventually resolve with healing and if needed draining. The fluid draining from an incision should be thin and clear, yellowish clear or pink clear. It should not be milky, thick, purulent, or green. If you are experiencing anything out of the ordinary, please do not hesitate to call your surgeon.
Informed Surgical Consent
July 18, 2015 9:39 pm
Surgical informed consent is the document that summarizes the discussion that has been carried out between the treating physician and the patient. It also outlines the expectations as well as the potential complications of the treatment being proposed.
An informed consent should mean that the patient is absolutely clear as to the procedure agreed upon and that is reflected on the consent. No abbreviations are allowed on the consent forms. Clearly, there are instances when a physician or surgeon providing service may have to deviate from the proposed plan and agreed upon procedure on the consent because of unexpected findings in the operating room.
Any patient undergoing surgery should be acutely aware of the terminology and the language used. With regards to weight loss surgical procedures, RNY and GB is not acceptable because they are both abbreviations.
Duodenal Switch is a distinct well described procedure with its unique identifiable code (43845 for open procedure) that is recognized by hospitals, insurance companies and the surgical societies.
Duodenal Switch operation is not SADI, SIPS nor a loop Duodenal switch. Any attempt to interchanges these terms or operations is inaccurate the say the least.
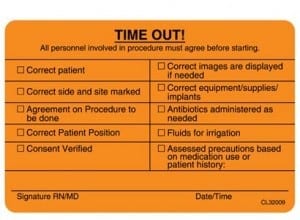
A surgical informed consent is signed by the patient ( or the guardian) and the treating physician. This document however is reviewed and confirmed by all those involved in the patient’s care delivered in the hospital. The consent is reviewed by the admission staff when taking the patient for surgery, preoperative nursing and administrative staff, operating room circulating nurse as well as the anesthesia staff. One step most patients may not be aware is initiated after the general anesthesia is induced. The operating room staff, anesthesia staff and the operating physician all go through a set of checklist known as “Time out”.
“Time out” involves confirming the patient’s identification as well as the proposed procedure as the patient had discussed with the staff and confirming the consent.
It is imperative that a patient have complete understanding of their surgical options available to them and critical that they have full knowledge of the type of surgical procedure that has been consented to and performed.
Shared Success Story- Odessa D.
April 07, 2015 10:20 am
My name is Odessa D. I am going to talk about my weight loss journey with the lap band which started in 2006. At my heaviest I weighed 270 pounds and was a size 24 waist. I had high blood pressure, was a border line diabetic, had lower back pain, I had no energy, I was tired all the time, and I had sleep apnea.
My family doctor had suggested weight loss surgery but I was hesitant because I was afraid of surgery. Until one night my 8 year old daughter found me not breathing in my sleep. I made the decision to go through with the surgery.
Prior to surgery I did as much research as I could about the lap band. At the time I felt it was the right decision. On the day of the surgery everything went well. The first few months were great. I was losing weight, feeling good, feeling happy, and healthier then I have in years.
Then it began, all the symptoms of a slipped band. I started vomiting, nausea, acid reflux, and I was having trouble drinking and eating on a daily basis. My doctor confirmed it was a slipped band. We decided to replace the band because I was still overweight. On day of surgery I weighed 210 lbs.
After a month I started having symptoms of a slipped band. My doctor performed x-rays but everything looked fine. After 2 years with these symptoms and numerous doctor visits and x-rays I just gave up and learned to live with it. In 2 years I lost 4 lbs. My high blood pressure and sleep apnea came back. I finally decided to get the lap band removed. I wanted my life back and if that meant gaining the weight back that I lost then I was willing to make that sacrifice.
Dr. Keshishian was referred to me by 2 of his past patients. From the moment I walked into his office I was already at ease. When I first met Dr. Keshishian, I knew I was in good hands and I knew he could help me. He confirmed I had another slipped band and a detached port. At this point we discussed removing the lap band and switching to the Sleeve Gastrectomy. Finally everything was going to be fixed and everything was going to be right.
I can’t express how much my life has improved since removing the second band and switching to the sleeve. I have lost 46 pounds in 9 months. I now weigh 160 pounds and wear a size 8 waist. Now I look forward to each and every day with joy and pleasure knowing I don’t have to deal with a bad band and all the horrible symptoms that came with it.
Since the surgery and losing more weight I have been very active. I go hiking almost every weekend. I have literally climbed a mountain! I did my first 5k mud obstacle course in which my second 5k is in October. I even have a purple Mohawk! I have 100% confidence in myself and in everything that I do. My life has greatly improved since the sleeve. All thanks to Dr. Keshishian. It has been a very bumpy road with my weight loss journey but Dr. Keshishian has smoothed out the bumps and I plan on traveling the distance with many adventures along the way.
I would like to leave a huge “Thank You” to Dr. Keshishian and his staff. Thank you for making me feel welcomed, being friendly, making me feel comfortable, and especially for giving my life back to me. I can’t wait to see what the future holds for me and my family!
Thank you Dr. Keshishian and staff!
Odessa D.
Gall Bladder- Should the Gall Bladder Be Removed During Duodenal Switch?
February 16, 2015 1:17 pm
The indication for concurrent cholecystectomy (gall bladder removal) with weight loss surgery is not clear. There is some scientific literature that recommends against cholecystectomy at the time of the Gastric Bypass RNY operation. To the best of my knowledge, there is no such studies looking specifically at the indication of cholecystectomy with duodenal switch operation.
My rationale for doing a cholecystectomy with every Duodenal Switch patient is that there is not only higher incidence of asymptomatic cholecystitis present but also due to limited access to the biliary tree. The transection of the duodenum and removal of the greater curvature of the stomach both limit access to the biliary tree. Additionally, the patient recovering from weight loss surgery, may not be in the best nutritional status to undergo a subsequent operation for gallbladder removal. A second surgery could add to nutritional issues due to protein needs for healing, risk of infection, hernia formation, etc.
From a technical aspects, in Duodenal Switch operation, the liver and the gall bladder need to be elevated in order to expose the anterior surface of the duodenum where the transection of the duodenum is performed. Doing a cholecystectomy at the time of the duodenal switch operation, more often than not only add a few minutes to the operation. In the majority of patients, long-term this saves them the potential need for a subsequent operation at a later date should they develop gallstones or gall bladder attack.
When I perform a Sleeve Gastrectomy the duodenum is not transected or dissected, and thus I do not remove the gall bladder when doing sleeve gastrectomy. I do, however, remove the gall bladder when doing primary Duodenal Switch for revision from a Gastric Bypass RNY to the Duodenal Switch operation.
Single-Anastomosis DuodenoIleal Bypass (SADI), SIPS, Loop
June 23, 2014 1:45 pm
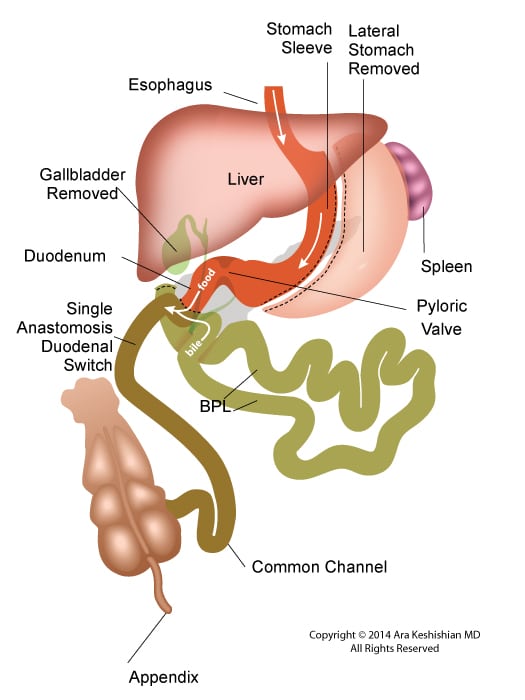
Single anastomosis duodenal switch, also known as Single Anastomosis DuodenoIleal Bypass (SADI) is a procedure that is being discussed more frequently in the literature. There have been a few series of case reports that have been published in the last few years. I would like to review the procedure and share my opinion.
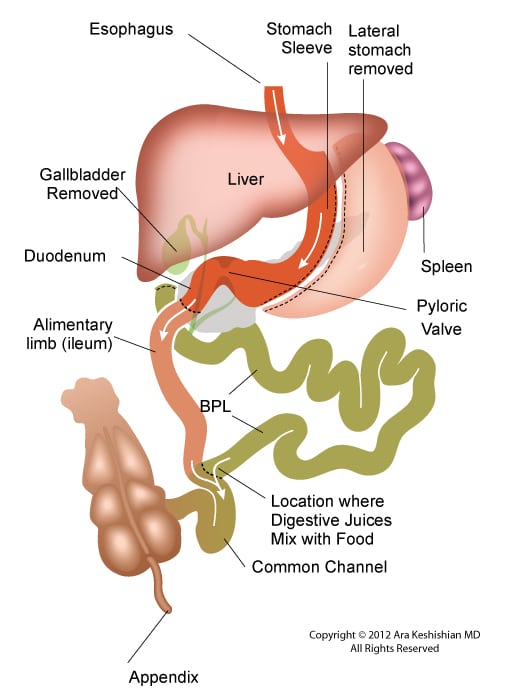
The theory behind the SADI has been to simplify the duodenal switch procedure. In “classical” duodenal switch procedure, the small bowel is divided in two places, (duodenum, and distal ileum) and two anastomosis are created (duodeno-ileostomy, and ileo-lieostomy). This can theoretically provide two potential places for leak, bleeding, adhesions as complications. In SADI, there is a single bowel division of the duodenum and a single anastomosis of the duodenum and the ileum. The sleeve component of the procedure is the same for both procedures. This is where their similarities end.
In the duodenal switch operation, the bowel is partitioned in to two parallel limbs- one that carries the biliopancreatic juices and a parallel limb that bring the food down from the post pyloric duodenum. They then join and form the common channel. The length of the biliopancreatic limb is so long that it does not allow bile to reflux back into the duodenum or back to the stomach causing the complication of bile reflux gastritis. With the single anastomosis of the SADI, the length of the bowel where the bile meets the duodenum is shorter than it is in normal anatomy. This significantly increases the possibility of the bile reflux. The second difference is the selective nature of the reduced absorption of the fat in the duodenal switch, in comparison to that of the carbohydrates. Duodenal switch operation has two absorptive lengths- the Alimentary channel, which is involved with protein and carbohydrate absorption, and the common channel that absorbs, fat, protein and carbohydrates. One can make changes to the common channel and impact the fat absorption significantly more than that of the carbohydrate and the proteins. In SADI procedure, that common channel and the alimentary limb are both the same- there is no way to selectively adjust the fat absorption without making significant changes to that of the protein and carbohydrate absorption.
Other than the obvious anatomical variations described above, it is important to mention that the concerns outlined above are mostly theoretical.
There are a number of publications that have reported the short-term outcome of the SADI procedure. They appear promising, but they are short-term results. Long-term data is needed. If the outcome does not change significantly over time, then I could see a role for SADI in the treatment for obesity. In the mean time, patients need to be made aware that the suggestion that SADI is the same as the duodenal switch is probably not correct since we do not have the data to support this oversimplification.
The animation of the Duodenal switch is here.
For comparison of duodenal Switch and SADI please check our web site here.