Calcium Lab Results
June 05, 2018 3:26 pm
Calcium is measured to evaluate function and adequacy of a physiologic processes. Calcium plays a critical role in several body functions such as, coagulation pathways, bone health, nerve conduction, and other functions. It is important whenever you are evaluating laboratory results that you look at the whole picture of the person, including medications, other laboratory studies and health history. One value is not a stand alone result. There are many factors that effect calcium results.
Factors that effect calcium results: (not an all inclusive list)
pH
Albumin
Lactate
Heparin
Anticonvulsants
Renal Disease
Pancreatitis
The two most common issues following Weight loss Surgery or Duodenal Switch may be albumin level and Vitamin D level. Please see past blogs on Vitamin D. Magnesium may also play a role in a Duodenal Switch patient.
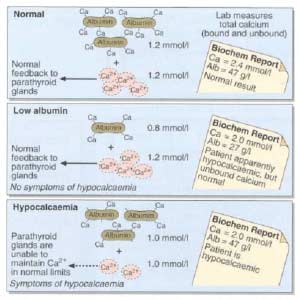
The most common calcium result drawn is the total calcium level. Laboratory results may not explicitly label it as such, however, it measures the calcium that is bound to protein. Ionized calcium is the free calcium that is representative of the true total calcium. Ionized Calcium can be measured by ordering specific lab. Alternatively, the Ionized calcium can be calculated by the following formula: Corrected calcium mg/dL = (0.8 * (Normal Albumin – Pt’s Albumin)) + Serum Ca ) or use the calculator at the bottom of this post.
The low Albumin level accounts for the low calcium level. This may be the reason for a patient with a low albumin/protein level, also having their calcium level reported as low. However, when adjusted for the protein deficiency the corrected calcium comes into normal range. Video of Trouseau’s sign of a patient with calcium deficiency.
The first step in a patient who has low calcium reported, is to make sure their protein and albumin levels are normal, along with Vitamin D.
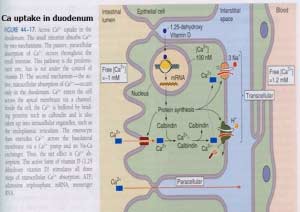
Calcium levels are managed by two processes major regularly hormones and influencing hormones. Controlling or major regulatory hormones include PTH, calcitonin, and vitamin D. In the kidney, vitamin D and PTH stimulate the activity of the epithelial calcium channel and the calcium-binding protein (ie, calbindin) to increase calcium absorption. Influencing hormones include thyroid hormones, growth hormone, and adrenal and gonadal steroids.
Further information on protein.
Further information on calcium.
Videos/Webinars on several of the above topics.
Corrected calcium = 0.8 * (4.0 – serum albumin) + serum calcium
Calcium Metabolism and Calcium Oxalate Stones
April 10, 2016 4:10 am
Trousseau sign due to calcium deficiency
April 10, 2016 4:05 am
Calcium – Revisited !Exclusive Member Content
October 05, 2015 8:06 am
Calcium May Cut Cancer Risk
March 06, 2009 11:10 am
Calcium May Cut Cancer Risk
Higher Calcium Intake May Reduce Risk of Colorectal and Other Types of Digestive Cancers
Here’s yet another reason to bone up on calcium. It may help reduce your risk of cancer. A new study shows that older men and women who got the most calcium from food and supplements had a 16% lower risk of colorectal and other cancers of the digestive system than those who got the least calcium.
Among women, those cancer-fighting benefits were even stronger. Women who got the most calcium from food and supplements had a lower risk of all cancer and a 23% lower risk of cancers of the digestive system than those who got the least.
Calcium is already known to boost bone health, but researchers say previous studies on calcium’s effect on cancer have produced mixed results.
“Our study suggests that calcium intake is associated with a lower risk of total cancer and cancers of the digestive system, especially colorectal cancer,” write researcher Yikyung Park, ScD, of the National Cancer Institute and colleagues in the Archives of Internal Medicine.
Calcium May Lower Cancer Risk
The Institute of Medicine recommends 1,200 milligrams of calcium per day for men and women over age 50. Dietary guidelines also call for adults to eat three cups of fat-free or low-fat dairy foods, such as milk, yogurt, and cheese to meet their daily calcium needs. This does not include conditions or diseases that my limit the absorption of the Calcium such as weight loss surgical procedures.
One 8-ounce serving of skim milk or yogurt contains about 300 milligrams of calcium. Other nondairy sources of calcium include beans, broccoli, spinach, and other green, leafy vegetables.
In the study, researchers analyzed data from nearly 300,000 men and 200,000 women 50 to 71 who participated in the National Institutes of Health-AARP Diet and Health Study. Participants answered a questionnaire about the foods and supplements they ate, and cancer rates were linked through state cancer registries over seven years of follow up.
The results showed that total calcium intake was not associated with a lower risk of cancer in general in men, but women who got up to 1,300 milligrams of calcium per day had a lower risk of cancer overall.
However, total calcium intake from both food and supplements was linked to a lower risk of colorectal cancer and other cancers of the digestive system in both men and women.
Men who got the highest levels of total calcium per day through food and supplements had a 16% lower risk of these cancers than those who got the least amount per day. Women who get the most calcium per day had a 23% lower risk than those with the least reported intake per day.
Researchers conclude that “our findings suggest that calcium intake consistent with current recommendations is associated with a lower risk of total cancer in women and cancers of the digestive system, especially colorectal cancer, in both men and women.”
SOURCES: Park, Y. Archives of Internal Medicine, Feb. 23, 2008; vol 169: pp 391-401.
Opinion and Commentary: The above two articles that were taken from internet sites, reflect the continues and ever evolving nature of the science behind most of the recommendations made.
Just imagine the treatment of a patient with a disease process. Almost certainly the surgical and medical treatment that may have been recommended years ago may not be an option today.
This is why it is important for us, providers and patients alike to continue to stay vigilant with our surveillance of our health condition and adapt to any pertinent information that may have an impact on it. One of the most commonly asked question is about the type and the amount of the calcium that patients are required to take.
The issue of the types of the calcium supplement is discussed in great length in the FAQ section of our website (dssurgery.com, weightlossinla.com). The table outlines the differences between the types. The bottom line is that for most patients there may not be much of a difference as long as the patients are consistently taking them. There are cases however when we have recommended one type or another.
The most recommended dose is 2000-3000 mg per day in divided dose. Before some of you start calling or emailing us as to how come you were told to only take 1500 and not 2000, remember what I said earlier in this section that this is an ever evolving field. If you have taken 1500mg in divided doses and have had your yearly lab work with no further recommendation from us, do not make any changes unless instructed so.
The other most common concern regarding the calcium, is its relationship with kidney stones. Most common Kidney stone is Calcium Oxalate in post weight loss surgical patients. The treatments Does not include cutting back on Calcium. Calcium Oxalate search of our website will provide further detail.
Ara Keshishian Md, FACS
Calcium
January 25, 2001 9:28 pm
Race Case of Vitmain D toxicity
February 08, 2021 2:47 pm
Vitamin D and COVID 19
June 13, 2020 4:40 pm
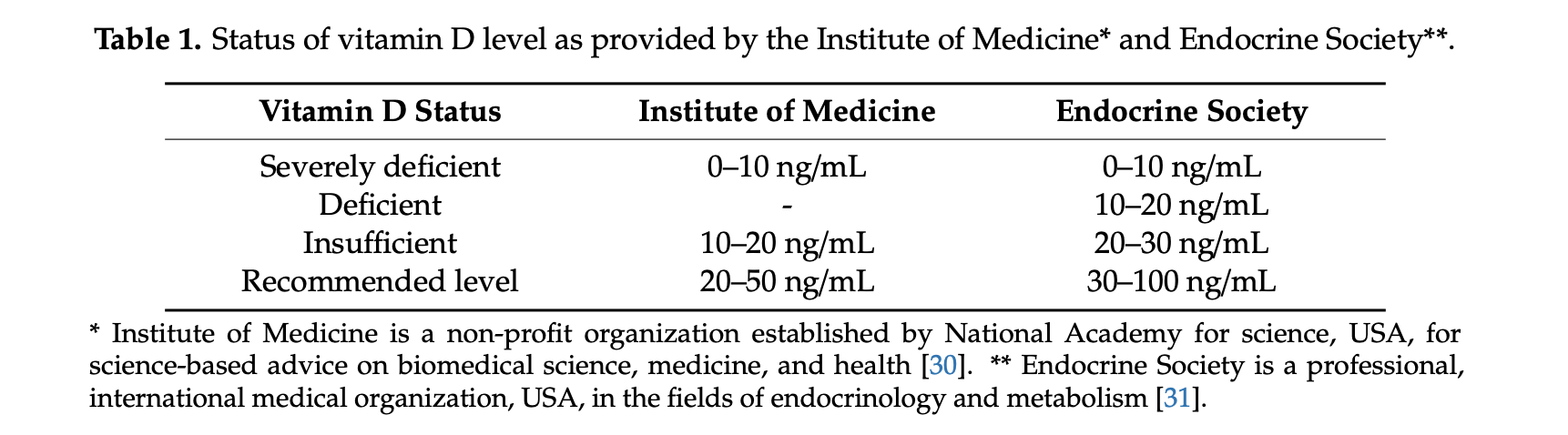
There has been extensive discussion on the importance of Vitamin D published over the last few years in regards to bone health, immune health and Calcium physiology. The importance of vitmain D and bone structure has been discussed extensively. It is also important in the absorption of Calcium. It further plays role in immune modulation.
What is new is the possible correlation of Vitamin D and COVID 19. Recently it is been shown that low vitamin D may increase the risk of a poor outcome with Covid-19 exposure and infection.
There are different standard recommendation for the Vitamin D levels.
In our practice we aim to maintain a Vitamin D level of 0ver 60 in post weight loss surgical patients.
There are a number of theories as to how the Vitamin D deficiency may play a role in this. An emerging observation is that low Vitamin D may cause abnormal and excessive blood clot formation. Mohammad et. al. in 2019 published a study on the association of low vitamin D and “…Pathogenesis of Thrombosis”
This pathologic blood clot formation in COVID-19 patients may explain the extensive lung injury and multi system organ failure in some patient. It is also one of the reason that some COVID-19 patients have loss limbs or appendages.
Please follow all supplement recommendations based on your laboratory studies and all COVID-19 recommendations. We would recommend frequent hand washing, surface cleaning, social distancing, and wearing face masks as the most basic precautions and increase precautions based on your health status.
Fat Soluble Vitamins
April 26, 2020 10:20 am
Written By: Maria Vardapetyan, Eric Baghdasaryan, Osheen Abnous
Vitamins are chemicals that facilitate many processes in the human body such as blood clot formation, good vision, fight infections etc. There are two classes of vitamins. Water soluble vitamins and fat soluble vitamins. Water soluble vitamins dissolve in water. This makes it possible for them to be absorbed through all mucous membranes. Fat soluble vitamins on the other hand do not dissolve or pass through mucous membranes. Fat-soluble vitamins are absorbed in the intestine along with fats in the diet. These vitamins have the ability to be stored in the fat tissues of the human body. Water-soluble vitamins are not stored in the body and have to be taken in daily with the food and dietary supplements. Solubility of a vitamin is not a function of its physical state. There are fat soluble vitamins that have a liquid form and almost all of the water soluble vitamins come in form of pills or powders.
In this article, we are going to focus on fat soluble vitamins. They are all complex molecules made of carbon, hydrogen, and oxygen in different arrangements (see figures 1, 2, 3 and 4). These fat soluble vitamins are vitamin A, D, E and K.
Vitamin A
Vitamin A has a major role in vision, immune function, cell growth, and maintenance of organs such as heart, kidneys, lungs, etc. It plays a pivotal role in the health of our eyes, specifically the retina1. Rhodopsin protein, a major protein that has the leading role in the process of vision, is found in the retina where it allows us to perceive light. This protein requires vitamin A to function properly. Without vitamin A, rhodopsin cannot sense light and thus cannot initiate the process by which vision occurs.
Figure 1: Chemical structure of Vitamin A molecule
Vitamin D
Vitamin D regulates different chemical reactions that are associated with bones, muscles, and the immune system. The simplified way it does this regulation is it helps absorb calcium from dietary nutrients which in turn strengthens the bones, helps neurons exchange signals to move muscles and helps the immune system to fight against viruses and bacteria2.
Figure 2: Chemical structure of Vitamin D molecule
Vitamin E
Vitamin E acts as an antioxidant. Antioxidants are naturally occurring chemicals that neutralize toxic byproducts of many chemical reactions in the human body. When food is consumed and digested, the human body converts it into energy. As a result of metabolism free radicals (toxic byproducts) are formed and are neutralized with the help of vitamin E. In addition, free radicals are also in the environment. Furthermore, vitamin E stimulates the immune system to fight against bacteria and viruses3.
Figure 3: Chemical structure of Vitamin E molecule
Vitamin K
Vitamin K can be obtained from food and dietary supplements. There are two forms of vitamin K: phylloquinone (Vitamin K1), which is found in spinach, kale and other greens and menaquinone-4 (Vitamin K2), which is found in animal products. Vitamin K1 is involved in blood clotting, and Vitamin K2 is involved in bone tissue building. Vitamin K1 is the main Vitamin K in human diet (75-90% of all vitamin K consumed), however, it is poorly absorbed in the body4,5.
Figure 4: Chemical structures of Vitamin K1 and K2 molecules
Absorption of fat soluble vitamins
Polarity describes the inherent charge(positive or negative) or lack of charge for any given substance or molecule. Molecules that are charged are referred to as “polar”, while those that lack charge are “nonpolar”. When discussing solubility, it is important to remember the phrase “like dissolves like”. That means polar (charged) substances like to interact with a polar environment like water, since water contains a slight negative charge. Hence, charged substances are water-soluble. Nonpolar substances on the other hand readily interact with nonpolar environments such as fat, which contains no charge. Therefore, molecules that lack a charge such as vitamins A, D, E, and K are referred to as fat soluble.
Due to their water fearing nature, these fat soluble vitamins cannot simply be absorbed directly into the bloodstream (which is mostly water) like the sugars and amino acids in our diet. As their name suggests, these fat soluble vitamins like to be embedded in fatty droplets, which facilitate their absorption in the following way. Fat soluble vitamins group together with other fat molecules to form fatty droplets, effectively reducing the amount of interaction with the watery environment of the intestines. Therefore, without an adequate amount of fat in your diet, your body is unable to effectively absorb these fat-soluble vitamins. This may be true in an intact anatomy, however, post weight loss surgical patients can not increase their fat soluble vitamin levels by increasing their fat intake. This is due to the fact that a high fat diet causes excessive bowel movement which in turn washes away any vitamins taken by mouth. DS limits fat absorption (thus the great weight loss) which can cause vitamin A and D deficiency that can not be easily corrected with oral supplementation.
As mentioned before, fat soluble vitamins are hydrophobic and nonpolar, which means they are also fat loving or lipophilic. Excess fat soluble vitamins can be stored in the liver and fat tissue. Therefore, these vitamins do not need to be eaten every single day since stores of these vitamins can sustain a person for some time. It may take several weeks or months for our body to deplete these stores of fat soluble vitamins which is why it generally takes a longer amount of time for fat soluble vitamin deficiencies to manifest themselves. The ability to store these fat soluble vitamins in tissues can also lead to vitamin toxicity – marked by an excess of vitamin stores in our body.
Clinical manifestations of A, D, E, K deficiency
| Vitamin | Clinical Deficiency manifestations |
| Vitamin A | Vision Problems
Dryness of the eye |
| Vitamin D | Softening and weakening of the bones
Bone shape distortion Bowed legs (generally in children) Hypocalcemia |
| Vitamin E | Damage to red blood cells
Tissue/organ damage due to inability to supply enough blood Vision problems Nervous tissue malfunction |
| Vitamin K1 | Excessive bruising
Increased bleeding time Small blood clots under nails Increased bleeding in mucous membrane |
| Vitamin K2 | Weak bones
Increased plaque deposits along gumline Arterial calcification |
References
- Office of Dietary Supplements – Vitamin A. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminA-HealthProfessional/#. Accessed April 26, 2020.
- Office of Dietary Supplements – Vitamin D. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminD-Consumer/. Accessed April 26, 2020.
- Office of Dietary Supplements – Vitamin E. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminE-Consumer/. Accessed April 26, 2020.
- Vitamin K. The Nutrition Source. https://www.hsph.harvard.edu/nutritionsource/vitamin-k/. Published July 2, 2019. Accessed April 26, 2020.
- Beulens JWJ, Booth SL, van den Heuvel EGHM, Stoecklin E, Baka A, Vermeer C. The role of menaquinones (vitamin K₂) in human health. The British journal of nutrition. https://www.ncbi.nlm.nih.gov/pubmed/23590754. Published October 2013. Accessed April 26, 2020.
Osteoporosis Medications, Action and Side Effects
May 25, 2019 3:40 pm
Treatment options should be approached is a global and systemic fashion. It is critical that the nutritional status is at its best possible and optimized for important healthy bone vitamins and minerals. Low protein needs to be corrected. Special attention should be given to nutrients, minerals and vitamins. These include Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1/K2to name a few.
Healthy bones require ongoing and routine force in the form of exercise to remain health. Just as exercise improves muscle strength, it also improves bone health. Exercise is also critical in improving bone structure and density. Ideally, exercise should be weight bearing and resistance. Examples include: hiking, walking, jogging, climbing stairs, playing tennis, and dancing. Resistance type exercise is weight lifting and resistance bands. These exercise work by creating a pull or force on the bone either by gravity, movement or weight. Always check with your physician before beginning an exercise routine, start slowly and building up to longer periods of time. The ideal goal would be at least 30 minutes a day, every day, if you are able.
We frequently see patients immediately started on osteoporosis medications without checking or improving some of the nutritional markers noted above or without looking at exercise history. In some case, the medication recommended are contraindicated due to nutritional status.
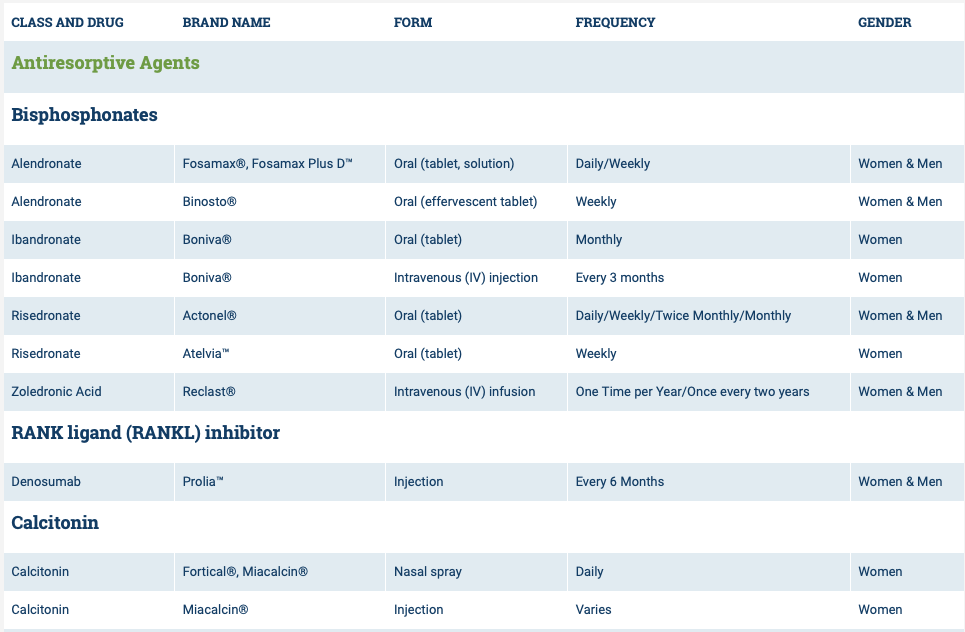
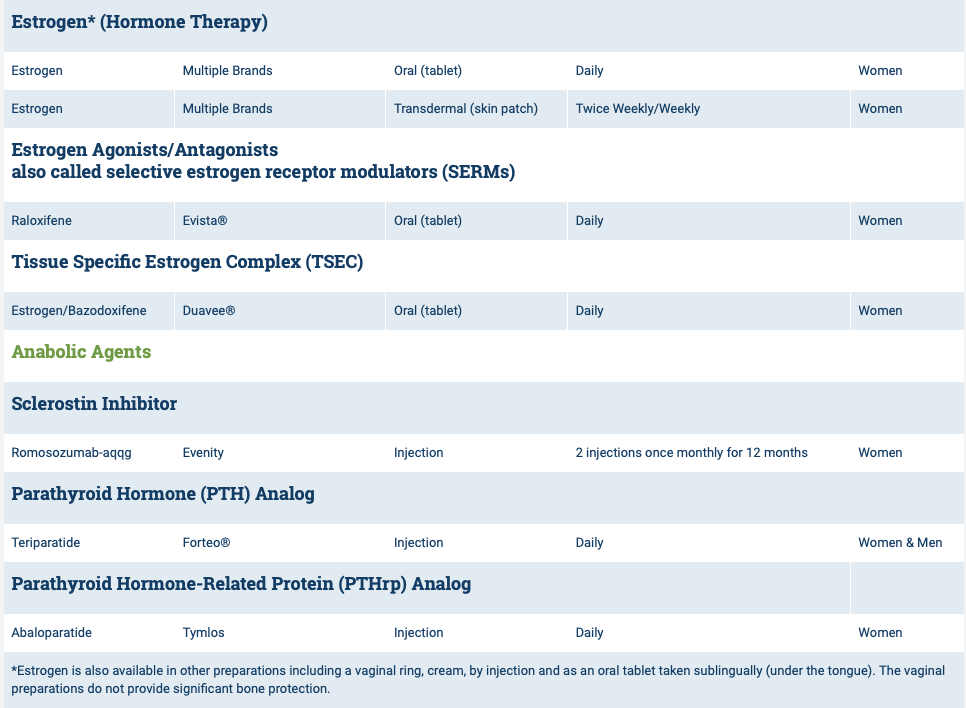
The medications can be grouped in to those that help with new bone formation (Anabolic agents) or those that help by suppressing the bone breakdown phase (Antiresorptive agents).
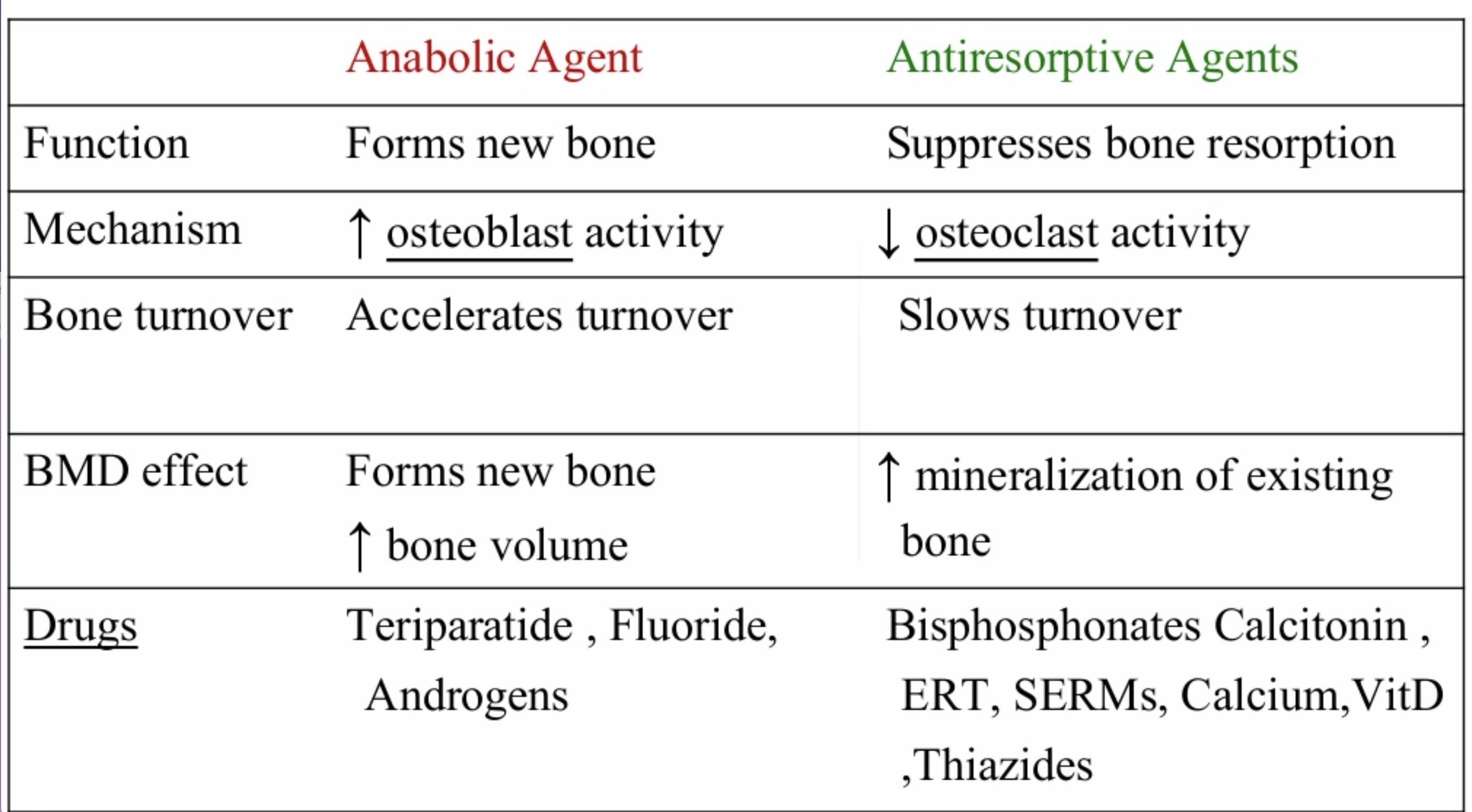
National Osteoporosis Foundation has an exhaustive list (below) of medications for treatment of Osteoporosis.
The table below outlines the side effects and mechanism of the actions of the common medications used for treatment of osteoporosis which was published by the University Health News Publication on August of 2014.
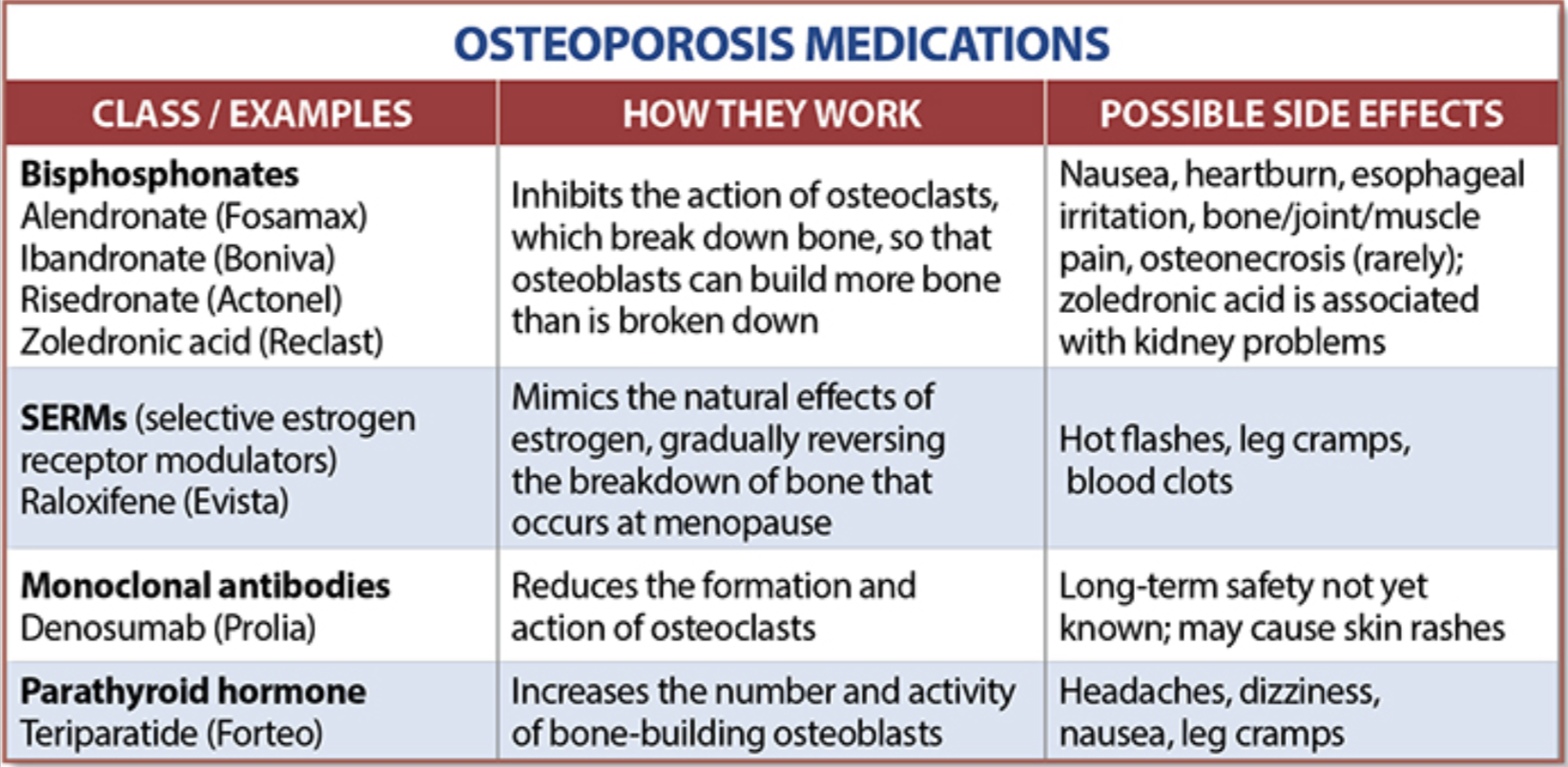
With all this information, the few points to remember is that the most important factors in healthy bone structure are the nutritional status Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1 levels.
This is an animation of normal bone Metabolism. It shows how bone structures is taken down and rebuilt continuously. This allows for a healthy bone maintainence as we age. The key is the balance of breakdown (osteoclast) and the build up (osteoblast) activity is regulated. Osteoporosis develops when there is more breakdown that build up. 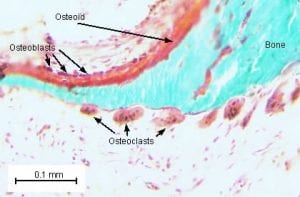
With permission of Dr. Susan Ott of University of Washington.
Additional information available on her site.
Past blogs on Bone Health.