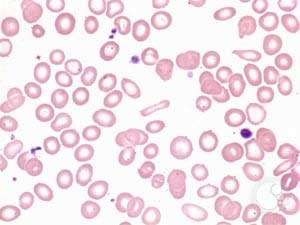
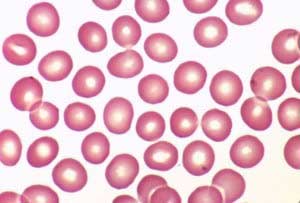
Iron Deficiency Anemia is a common problem in society and weight loss surgical patients. Anemia is usually easily treatable, although requires adequate surveillance and diligence in treatment. Microcytic/hypochromic (small pale colored red blood cells) erythrocytes indicate some inadequacy of structural matter, usually, not enough hemoglobin. This is most commonly due to an inadequate dietary supply of iron. In fact, iron deficiency anemia is the most common of all anemias.
Determining the cause of the iron deficiency is of pivotal importance in selecting appropriate therapy. Microcytic/hypochromic erythrocytes may also be seen in anemia of chronic disease, in thalassemia and in the sideroblastic anemias.
Symptoms of iron deficiency include:
- Being tired and feeling weak
- Getting frequent infections
- Feeling cold all the time
- Having swelling in the tongue
- Struggling to keep up at school or work
- Restless legs syndrome
- In children, having delayed mental development
- Feeling tired and weak
- Joint pain
- Abdominal pain
Possible Causes other than the above:
Blood loss is the most common cause of iron deficiency. Menstruation is the most likely reason in women ages 15 to 45 years. Iron deficiency anemia in adult men and postmenopausal women is most likely due to chronic gastrointestinal blood loss. Such losses are usually secondary to ulcerating lesions [peptic ulcer disease, mucosal trauma (hiatal hernias), drug ingestion (aspirin, nonsteroidal anti-inflammatory drugs, steroids, potassium), parasitic infections, inflammatory bowel disease and malignancy.
Undergoing several surgeries within a short time frame is also a source of blood loss. Frequently Duodenal Switch (DS) patients become anemic after their panniculectomy, breast reductions, arm or thigh lifts because of the short interval between operations. Also pregnancy after weight loss surgery can increase chances of developing iron deficiency anemia. After consecutive surgeries it is important to monitor your Iron, Ferritin and Transferrin, Total Iron Binding Capacity levels. Any drop in Ferritin or Transferin levels should be discussed with your DS surgeon. It is important to keep your levels with in normal limits because it can be challenging to bring these levels back up.Lack of dietary iron may cause anemia in infancy when the daily need for iron is not met by milk alone. This is why iron supplements are given to infants. Iron deficiency is a major cause of anemia in pregnancy.
Malabsorption of iron is a rare cause of iron deficiency in the general public but is seen in patients who have had a partial gastrectomy, RNY Gastric Bypass, or who have a surgical malabsorption, such as Duodenal Switch. Iron is absorbed through the duodenum and the first part of the jejunum. After DS there is only a small section (approximately 5cm) of the duodenum that comes into contact with the iron source in the GI tract. The remainder of duodenum and the jejunum after DS is now the biliopancreatic limb. There is an area of small intestine in the ileum that also absorb iron to a lesser degree in normal anatomy.
The following are definitions of Iron Deficiency Anemia diagnostic laboratory studies:
Ferritin is in essence an “iron buffer”, taking up excess iron or releasing iron as needed. Small amounts of ferritin, derived from iron stores, circulate in the plasma.
The amount of serum ferritin closely reflects iron stores, thus providing a readily measured assessment of body iron stores.
Ferritin is in essence an “iron buffer”, taking up excess iron or releasing iron as needed. Small amounts of ferritin, derived from iron stores, circulate in the plasma. The amount of serum ferritin closely reflects iron stores, thus providing a readily measured assessment of body iron stores.
-
- Transferrin, the major iron transport protein, is synthesized by the liver and macrophages (type of blood cell). Each molecule of transferrin can bind two at- oms of iron. Usually about one-third (25 – 45%) of the total transferrin is bound to iron (referred to as % saturation)Transferrin carries iron via plasma to cells throughtout the body, though the most important site of delivery is to the mar- row erythroblast. Non-heme iron (mainly Fe +++(Iron) ) is stabilized by gastric HCl; bound to mucin and then transferred to a mucosal cell surface receptor.
Most heme iron is catabolized to Fe ++ (Iron) and tetrapyrrole in the mucosal cell. In the mucosal cell the iron is bound to mobilferrin, transported through the cell to the submucosal capillary network where the iron is oxidized to Fe+++, bound to transferrin and delivered via the blood to the marrow and other tissues. Note that some iron is stored or “trapped” as ferritin in the mucosal cell. This “trapped” iron plays only a minor role in regulation of iron intake/loss as it is readily overwhelmed by ingestion of inorganic iron.
Total Iron Binding Capacity approximates a measure of transferrin. Serum iron is a measure of Fe bound to transferrin. Normally 25 – 45% of transferrin is bound to iron, ie. The % saturation of transferrin. In inflammatory and malignant conditions transferrin is decreased possibly due to macrophage degradation. Iron is decreased due to decreased release of iron from macrophages into the plasma. Iron deficiency is best screened for with serum ferritin levels (serum ferritin levels correspond to marrow stores). A serum ferritin of 12-307 ng/ml is the normal range.
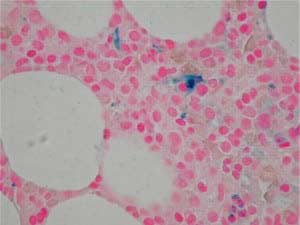
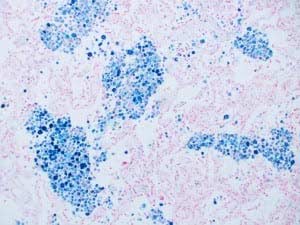
The definitive test for iron deficiency is a Prussian blue stained bone marrow. The upper image demonstrates an absence of iron in the bone marrow macro-phages of an individual with iron deficiency.
Compare the upper image with the lower image of a normal bone marrow stained with Prussian blue and demonstrating coarse granular storage iron in macrophages.
Normal Iron Ranges:
Normal results of iron testing may be different for men, women, and children. Iron and TIBC are measured in micrograms per deciliter (mcg/dL). Normal results for iron are:
- 65 to 175 mcg/dL for men
- 50 to 170 mcg/dL for women
- 50 to 120 mcg/dL for children
Normal results for TIBC are 250 to 450 mcg/dL for men and women.
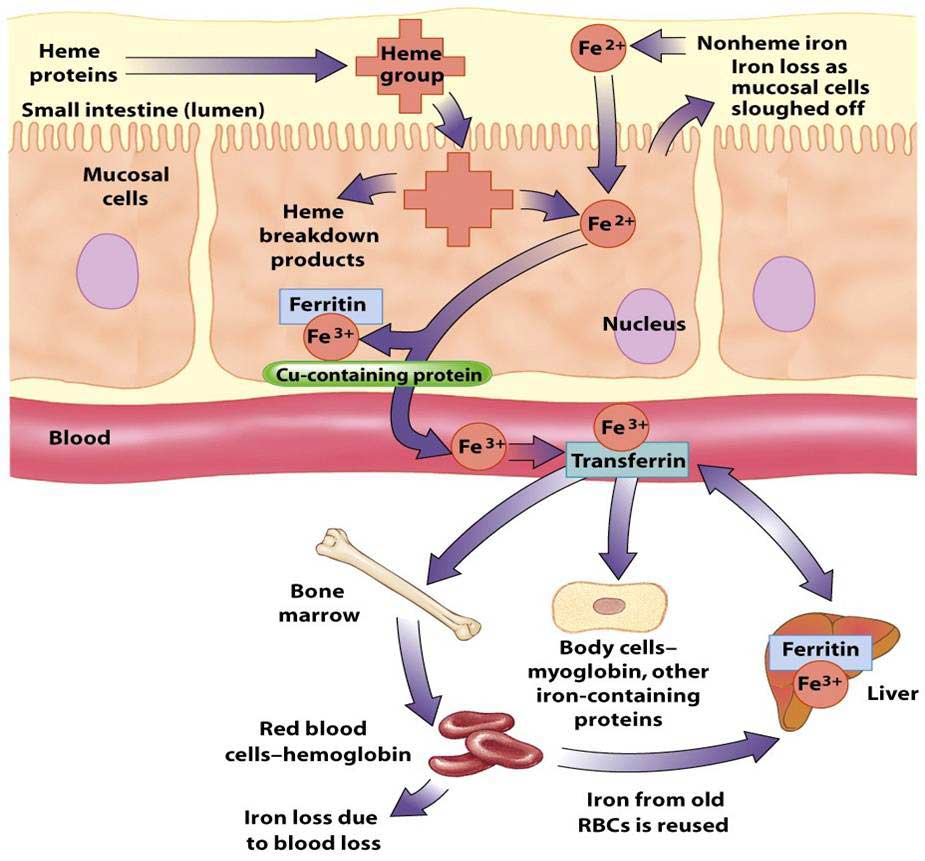
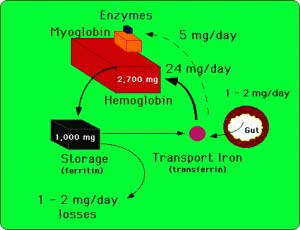
The diagram below shows the normal uptake, storage and loss of iron within the cell. An excellent explanation of iron transport physiology can be found here: https://sickle.bwh.harvard.edu/iron_transport.html
Iron is continually conserved and recycled for use in heme and non-heme enzymes. About 1 to 2 mg of iron are lost each day to sloughing of skin and mucosal cells of the gastrointestinal and genitouretal tracts. This obligate iron loss is balanced by iron absorption from the gastrointestinal tract. Only a small fraction of the 4 grams of body iron circulate as part of transferrin at any given time. Body iron is most prominently represented in hemoglobin and in ferritin.
Treatment:
There are different oral iron formulations available. I recommend heme iron instead of ferrous sulfate or ferrous fumarate. After 3 months of therapy it is necessary to repeat laboratory blood levels to determine the next course of action. Iron supplements along other medications should be stored away from children in “child proof” containers. Your pharmacist will be able to instruct you with the correct way of taking the iron supplements, and possible interference with other medications that you may be taking.
In severe anemia and/or iron deficiencies anemias resistant to oral iron supplementation, it may be necessary to have iron injections or infusions intravenously. If you have any questions please contact us either by email or phone.
In summary, iron deficiency anemia develops gradually. It also takes a great deal of time to build iron levels back up again. The importance of continued surveillance of laboratory studies is crucial after weight loss surgery. In addition, the treatment of iron deficiency anemia requires diligence in taking the iron supplement or reacting to the inability to absorb oral iron supplements by using iron infusions. Please contact our office if you have not had your yearly lab work or you may have your primary care physician order these studies.
- Weight loss Medications compared to surgery February 20, 2024
- SIPS-SADI and ASMBS December 31, 2023
- Survey December 16, 2023
- Long Term Outcome Survey December 1, 2023
- Weight Loss Injection May 10, 2023

Your timing on this couldn't have been better. I'm dealing with this right now, waiting for insurance approval to start the iron infusions. And I learned some things I wasn't aware of. Perfect! :)<br />THANK YOU!!
How much iron do you recommend for DS patients?
Hello- This all depends on a patient labs, if there is any blood loss, if they had the small bowel measured as a percentage of other total length and other factors. There is not set dosing. I would recommend contacting your surgeon for specific answers.
Thank you
Ara