Category: hyperparathyroidism
Osteoporosis Medications
March 28, 2020 7:22 pm
There are a number of lectures, posting that we have done over the years on this topic. However the questions of osteoporosis medications and their benefits and risks comes up often.
The links are attached:
Here is an updated list of medication that I had previously published. I made some clarification to explain how the medications work. There are different classes of medications and the detail of the action and soda effects were described earlier at a blog post.
List of medications that effect bone health.
The table is obtained from https://www.nof.org site.
Calcium Lab Results
June 05, 2018 3:26 pm
Calcium is measured to evaluate function and adequacy of a physiologic processes. Calcium plays a critical role in several body functions such as, coagulation pathways, bone health, nerve conduction, and other functions. It is important whenever you are evaluating laboratory results that you look at the whole picture of the person, including medications, other laboratory studies and health history. One value is not a stand alone result. There are many factors that effect calcium results.
Factors that effect calcium results: (not an all inclusive list)
pH
Albumin
Lactate
Heparin
Anticonvulsants
Renal Disease
Pancreatitis
The two most common issues following Weight loss Surgery or Duodenal Switch may be albumin level and Vitamin D level. Please see past blogs on Vitamin D. Magnesium may also play a role in a Duodenal Switch patient.
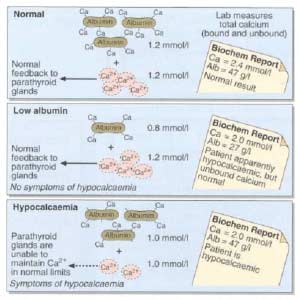
The most common calcium result drawn is the total calcium level. Laboratory results may not explicitly label it as such, however, it measures the calcium that is bound to protein. Ionized calcium is the free calcium that is representative of the true total calcium. Ionized Calcium can be measured by ordering specific lab. Alternatively, the Ionized calcium can be calculated by the following formula: Corrected calcium mg/dL = (0.8 * (Normal Albumin – Pt’s Albumin)) + Serum Ca ) or use the calculator at the bottom of this post.
The low Albumin level accounts for the low calcium level. This may be the reason for a patient with a low albumin/protein level, also having their calcium level reported as low. However, when adjusted for the protein deficiency the corrected calcium comes into normal range. Video of Trouseau’s sign of a patient with calcium deficiency.
The first step in a patient who has low calcium reported, is to make sure their protein and albumin levels are normal, along with Vitamin D.
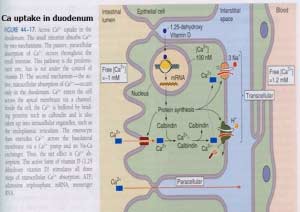
Calcium levels are managed by two processes major regularly hormones and influencing hormones. Controlling or major regulatory hormones include PTH, calcitonin, and vitamin D. In the kidney, vitamin D and PTH stimulate the activity of the epithelial calcium channel and the calcium-binding protein (ie, calbindin) to increase calcium absorption. Influencing hormones include thyroid hormones, growth hormone, and adrenal and gonadal steroids.
Further information on protein.
Further information on calcium.
Videos/Webinars on several of the above topics.
Corrected calcium = 0.8 * (4.0 – serum albumin) + serum calcium
Calcium – Revisited !Exclusive Member Content
October 05, 2015 8:06 am
Hyperparathyroidism and Weight Loss Surgery
March 13, 2015 5:57 pm
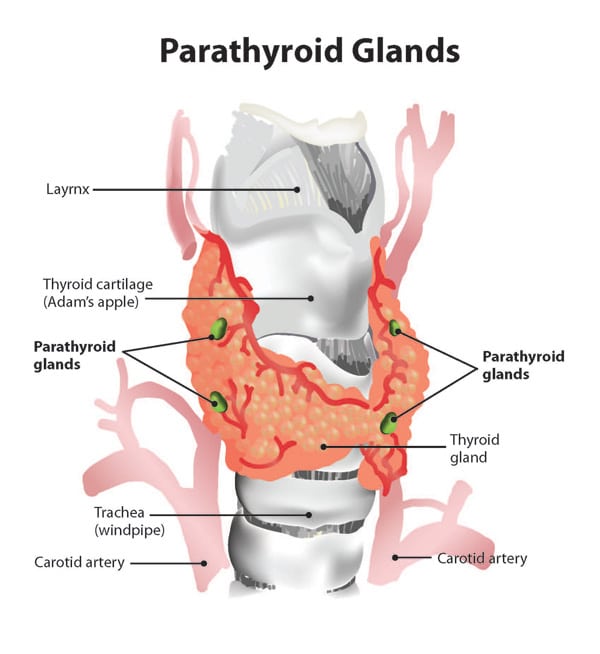
Hypoparathyroidism refers to elevated level of parathyroid hormone levels (elevated or high PTH). Parathyroid glands are two small glands that are located behind the thyroid gland. The primary function is regulation of the calcium level in the bloodstream. Parathyroid levels may be abnormally elevated for a number of reasons.
1-Primary Hyperparathyroidism
There may be abnormalities within the parathyroid glands themselves including benign and malignant tumors. Laboratory studies to assist in identifying Parathyroid hyperplasia are calcium, phosphorus, magnesium, PTH (parathyroid hormone), Vitamin D and possibly a 24 hour urine, kidney x-ray, and Dexa scan. The calcium levels in parathyroid hyperplasia are usually elevated and Vitamin D levels low. Patients can present with hypercalcemia symptoms such as kidney stones, nausea, vomiting, peptic ulcer, constipation, bone pain, bone weakness, depression, lethargy, fatigue. There are two types of Primary Hyperparathyroidism parathyroid hyperplasia and parathyroid adenomas. These both can at times be genetically linked.
Once the cause of elevated parathyroid hormone has been identified as primary hyperparathyroidism, the treatment involves surgical removal of one or more of the adenoma(s) or removal of 3.5 off all of the parathyroid glands if hyperplasia is diagnosed.
Parathyroid hyperplasia: When the growth involves all 4 of the glands. These may effect either one of the glands or all 4 of them. Majority of these are benign.
Parathyroid adenoma(s) refers to the abnormality or benign growth of one or more of the parathyroid glands.
2- Secondary Hyperparathyroidism
This is probably the most common cause of hyperparathyroidism imposed on a weight loss surgical patient. The elevated parathyroid hormone is the physiologic response all of the parathyroid glands to low calcium level. The parathyroid hormone is elevated in order to favor bone breakdown and make available for calcium to be circulating in the bloodstream. Parathyroid hormone also facilitates reabsorption of the calcium from the urine and improve absorption of the calcium from the GI tract.
The most common causes of secondary hyperparathyroidism is Vitamin D deficiency, weight loss surgery, kidney failure, Celiac or Crohn’s Disease. Lower levels of Vitamin D decrease the intestinal calcium absorption and thereby increasing PTH secretion. Vitamin D is the transport molecule for calcium. Symptoms may include bone or joint pain, muscle weakness, osteomalacia, low to normal blood calcium levels. The treatment of secondary hyperparathyroidism is correction of the underlying low calcium, low vitamin D levels. We have our Duodenal Switch patients take calcium citrate and dry water miscible type of Vitamin D3. Some people may require vitamin D injection in order to overcome deficiencies. You can find a list of supplements on our website and/or our starting point supplement recommendation in our patient workbook
Articles on Secondary Hyperparathyroidism following Weight Loss Surgery:
https://www.ncbi.nlm.nih.gov/pubmed/23015268
https://www.ncbi.nlm.nih.gov/pubmed/16354517
- Weight loss Medications compared to surgery February 20, 2024
- SIPS-SADI and ASMBS December 31, 2023
- Survey December 16, 2023
- Long Term Outcome Survey December 1, 2023
- Weight Loss Injection May 10, 2023