Tag: protein
Copper Metabolims And Weight Loss Surgery
May 01, 2020 12:31 am
Written By: Osheen Abnous, Maria Vardapetyan, Eric Baghdasaryan
Copper is an essential element to all organisms, and it is a contributor in several enzymes vital to the function of hematopoietic, vascular, and skeletal tissues, as well as the structure and function of the nervous system.
As a crucial metal, copper plays an important role in chemical reactions throughout the human body; this includes the central nervous system. Enzymes are substances that facilitate chemical reactions. There are many copper-dependent reactions in the human body. In humans, the major site of absorption of dietary copper is still unclear. Copper in humans is absorbed in the proximal small bowel, duodenum, and ileum. This is after it has passed the acidic environment of the stomach.
Copper deficiency can be caused by malnutrition, prematurity, parenteral or enteral feeding without copper supplementation, gastrectomy, and excessive zinc therapy. The common causes of copper deficiency have been zinc supplementation, and changes to the PH (acidity) of the stomach. This can be the result of the alteration of the stomach anatomy, and by chronic acid suppression by proton pump inhibitors (antacids), and similar medications. Physicians need to be alert with patients who show signs of copper deficiency or are at a high risk of developing a copper deficiency.
It is important to raise greater awareness about copper deficiency because there is a growing number of patients undergoing surgeries for obesity, as the occurrence of copper deficiency will increase in the future.
Studies of patients who have had weight loss surgery in the past experience common symptoms such as pain involving the feet, gait abnormality (unusual walking), lower limb weakness, and recurrent falls. Common lab results include unusually low serum copper and serum ceruloplasmin levels. In some cases, elevated zinc levels are also present. Treatment includes cupric sulfate infusion until normal copper levels are reached, which then need to be maintained for the future. Vitamin B-12 deficiency has also been reported as a possible cause of myelopathy, which is a nervous system disorder that affects the spinal cord. As stated earlier, neurological damages are often irreversible and cause permanent damage to patients. Early diagnosis from physicians is crucial for patients who have undergone gastric bypass surgery, and the sooner they are diagnosed, the less permanent damage the patient will endure.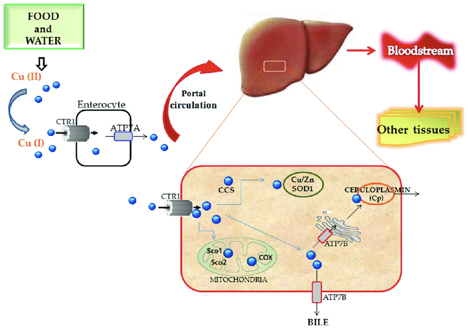
Case Discussions:
A 49-year-old woman had gastric bypass surgery for obesity 24 years age. She presetend with increasing lower limb stiffness and numbness. Additionally she reported tingling of the feet. As her pain continued to increase, she began using a walker, and her symptoms continued to worsen. After undergoing a neurological examination, results showed that the patient had increased lower limb tone and an absent perception of vibration at the toes and ankles. Laboratory results showed that the patient had copper levels barely detectable. This included serum copper and serum ceruloplasmin levels. In addition, the patient had reduced serum carotene (vitamin A) levels.
The patient received cupric sulfate intravenously daily through an 8-week period. After each daily infusion of cupric sulfate, the patient reported to have slight decreases in numbness and an increased tingling sensation. After the 8-week period, lab results showed that serum copper levels were normal and are needed to be maintained. Her night blindness was corrected by vitamin A injections.
In another case, a 53-year-old woman had symptoms of abnormal gait (abnormal walking) and anemia (lack of healthy red blood cells), and was seen for evaluation. The patient complained of pain in the lower legs, which would worsen over time and move up towards her thighs. As her ability to walk continued to worsen, the patient resorted to using a wheelchair. Her medical history consisted of an RYGB surgery for obesity. The only significant supplementation she received was 1000 μg vitamin B12 subcutaneously for several years. She had absent positional and vibratory sensation in the lower extremities to the knee. In addition, touch sensation was decreased. Laboratory examination revealed an elevated serum zinc level, and extremely low serum copper and ceruloplasmin levels.
For treatment, the patient received intravenous copper over a 6-day period, was discharged home, and then received weekly intravenous copper infusions thereafter. After a month of receiving intravenous copper, serum copper levels returned to normal. In addition, the patient’s pain in the lower leg improved, but vibratory sensation remained absent in the same area. Four months after being discharged from the hospital, the patient began walking with a cane.
Protein Intake
October 14, 2019 7:08 am
Protein intake requirements change over time following weight loss surgery. This is based on the requirements imposed on our body by a number of variables. These include, activity level, muscle mass, over all health condition to name a few.
A very young muscular athletic male with a BMI or 30 will require much higher protein intake (and absorption) that an inactive older Female with the same BMI. The same young athletic male will require much higher protein intake is he is recovering from a surgery than his baseline.
As we have stated in the past, the protein intake, should be adequate and not excessive. High level of protein intake that are not accounted for based on muscle mass and activity level, will eventually result in weight gain. The best measure of protein intake in a stable weight patient over 3-4 years post op is their albumin and protein level. Following your yearly laboratory values at a minimum is an important part of weight loss surgery follow up care.
You also need to adjust protein intake when necessary. Protein needs increase depending on physical needs, infection, healing, pregnancy, surgery, age, injury, etc. Plastic surgery requires higher protein needs for appropriate healing.
Information on protein sources and quality here.
The basic formula for protein intake is 1gm/kg of ideal body weight. The calculator below will provide a guide for the protein into based on your stable weight in lbs.
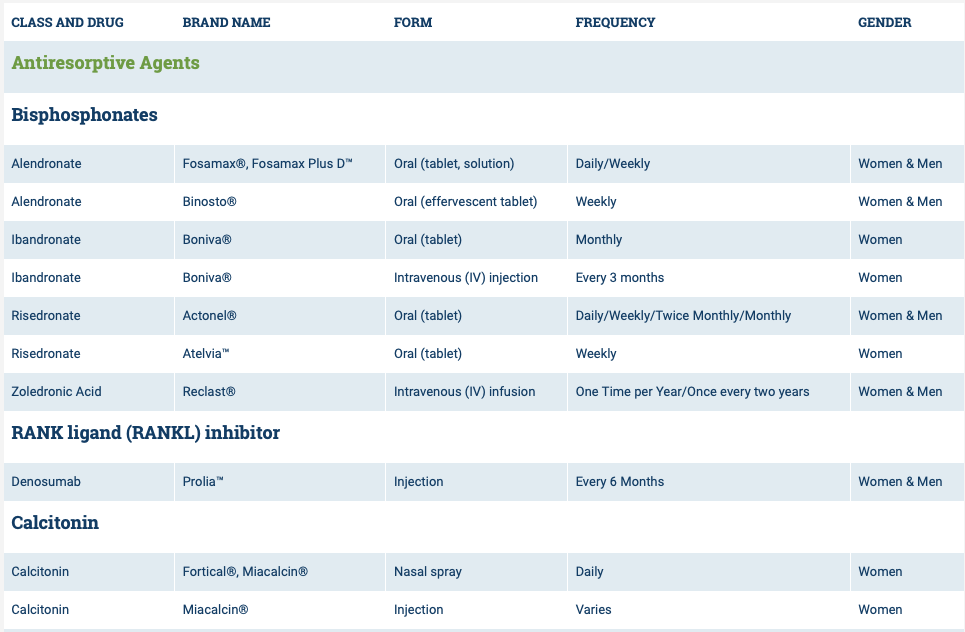
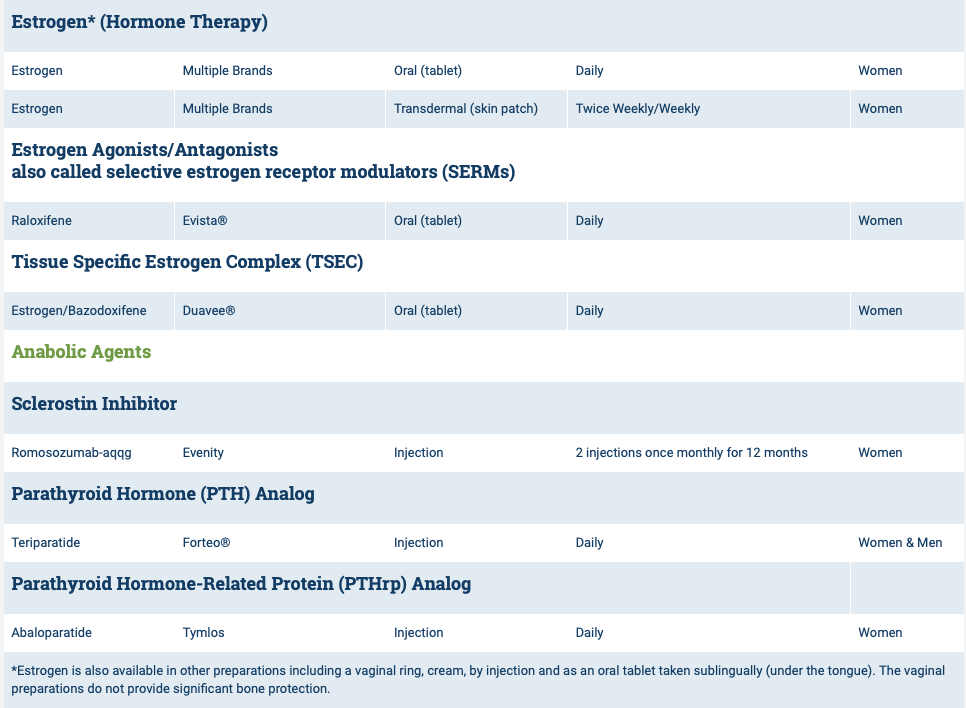
Osteoporosis Medications, Action and Side Effects
May 25, 2019 3:40 pm
Treatment options should be approached is a global and systemic fashion. It is critical that the nutritional status is at its best possible and optimized for important healthy bone vitamins and minerals. Low protein needs to be corrected. Special attention should be given to nutrients, minerals and vitamins. These include Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1/K2to name a few.
Healthy bones require ongoing and routine force in the form of exercise to remain health. Just as exercise improves muscle strength, it also improves bone health. Exercise is also critical in improving bone structure and density. Ideally, exercise should be weight bearing and resistance. Examples include: hiking, walking, jogging, climbing stairs, playing tennis, and dancing. Resistance type exercise is weight lifting and resistance bands. These exercise work by creating a pull or force on the bone either by gravity, movement or weight. Always check with your physician before beginning an exercise routine, start slowly and building up to longer periods of time. The ideal goal would be at least 30 minutes a day, every day, if you are able.
We frequently see patients immediately started on osteoporosis medications without checking or improving some of the nutritional markers noted above or without looking at exercise history. In some case, the medication recommended are contraindicated due to nutritional status.
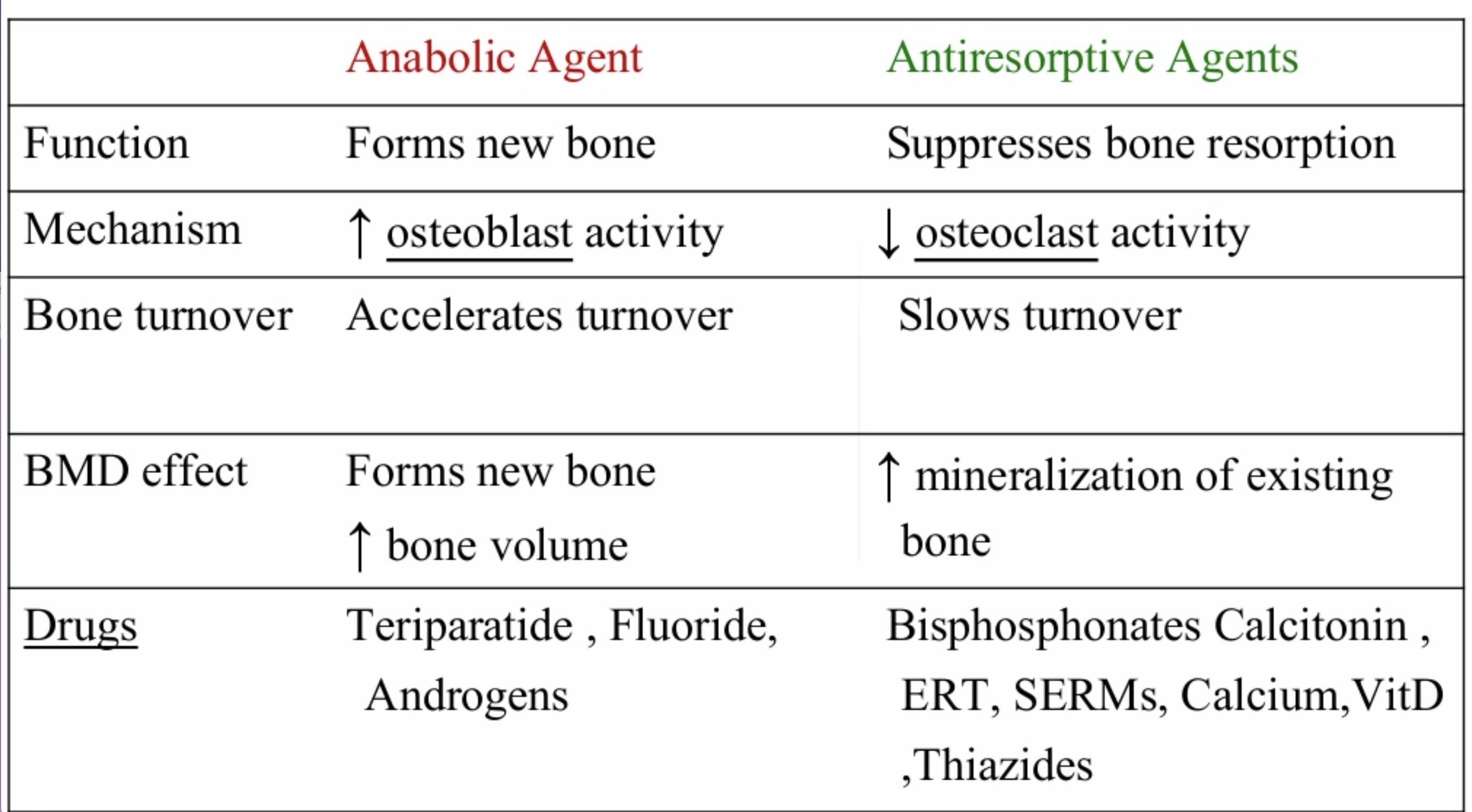
The medications can be grouped in to those that help with new bone formation (Anabolic agents) or those that help by suppressing the bone breakdown phase (Antiresorptive agents).
National Osteoporosis Foundation has an exhaustive list (below) of medications for treatment of Osteoporosis.
The table below outlines the side effects and mechanism of the actions of the common medications used for treatment of osteoporosis which was published by the University Health News Publication on August of 2014.
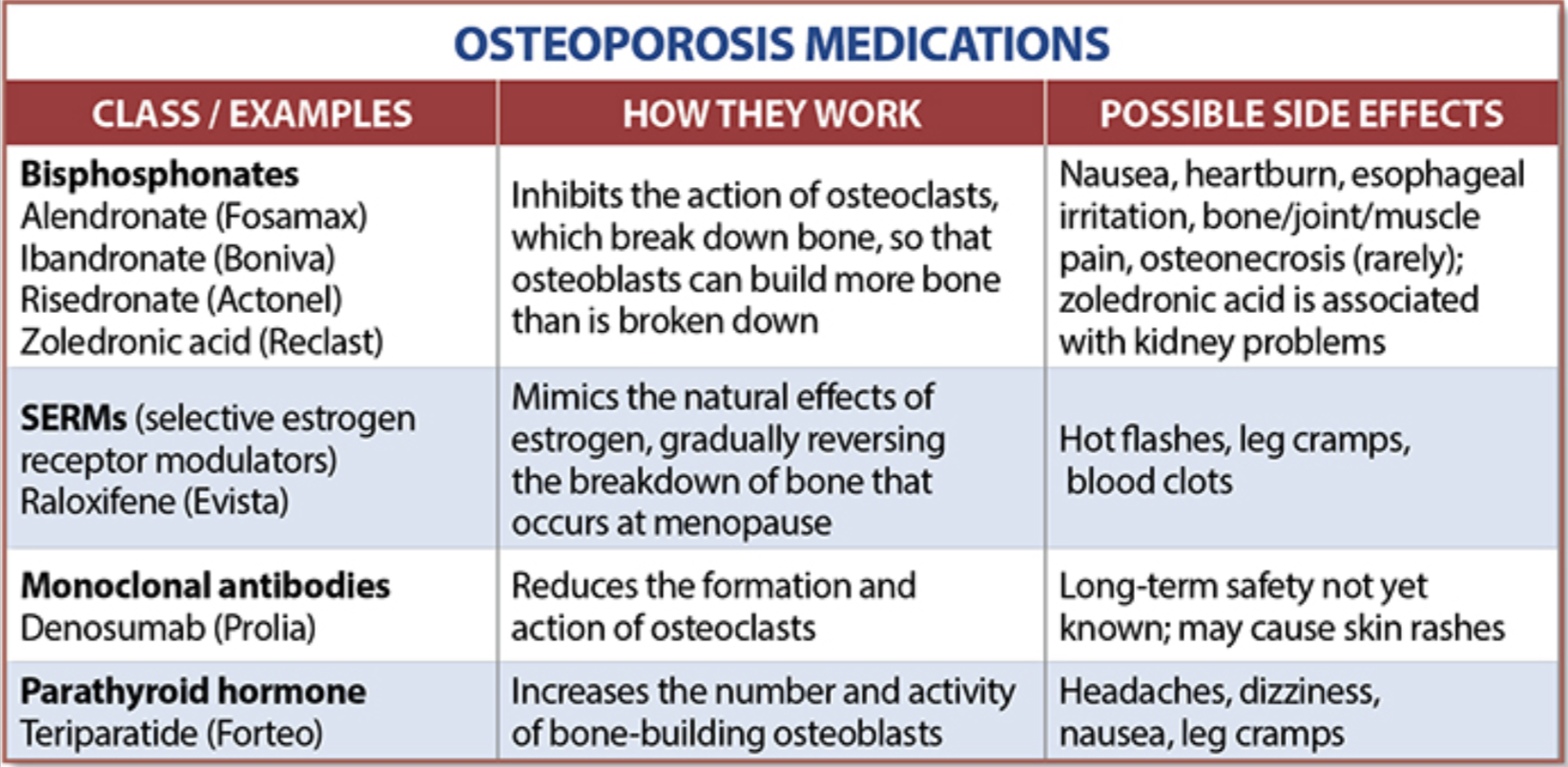
With all this information, the few points to remember is that the most important factors in healthy bone structure are the nutritional status Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1 levels.
This is an animation of normal bone Metabolism. It shows how bone structures is taken down and rebuilt continuously. This allows for a healthy bone maintainence as we age. The key is the balance of breakdown (osteoclast) and the build up (osteoblast) activity is regulated. Osteoporosis develops when there is more breakdown that build up. 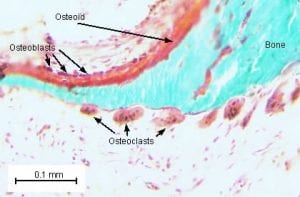
With permission of Dr. Susan Ott of University of Washington.
Additional information available on her site.
Past blogs on Bone Health.
2018 Back on Track
January 28, 2018 11:38 am
Join our 2018 Back on Track challenge and let’s get back on track for 2018! The holidays were wonderful but if you find yourself with a few extra souvenirs don’t feel alone. The average American gains between 1-8 pounds during the holiday season and I am no exception. Let’s get back on track 2018 together.
Time to clear out the kitchen! Disposing of temptations and high trigger foods is the first step to getting back on track. Throw it all away and don’t allow them back in. If foods are difficult to acquired then they are less likely to be consumed.
Stock up on high protein and whole, unprocessed foods that are low carbohydrate and nutrient dense. When quality foods are easily available we are more likely to stay on track with the types of foods we should be eating. Simple sugars/carbohydrates are the biggest culprit of holiday weight gain. We need to go back to the basics of hydration, high protein, low carbohydrate/sugar, vitamin/mineral supplements and exercise. Simple sugars and carbohydrates are easy for our bodies to use and absorb. Cutting them out can jump start your weight loss. Each individual needs to identify the daily carbohydrate intake that works for them. Some people stay under 50 grams of carbohydrates daily and some can tolerate more daily grams. You may also need to look at your protein and fat intake. All excess nutrients absorbed have the potential to turn into fat mass and inhibit weight loss. Metabolism video.
Hydration is an important ways to start getting back on track. Water is essential to life functions. The brain is 85% water, blood is 80% and muscle is about 70% water. Hydration aids in digestion, eliminating waste, byproducts and toxins. It also can decrease the feeling of hunger. Lack of hydration can increase fatigue which can lead to craving high carbohydrate foods to increase energy.
Protein’s importance in almost every bodily function and muscle mass can not be ignored. High quality complete Protein sustains muscle mass during weight loss, aids immunity, antioxidant function, and enhances leptin and insulin function. Filling up on protein first will help with carbohydrate carvings and give a sustained satisfied feeling. A prior blog post gives additional information on the importance of protein and the effects of protein malnutrition. WLS makes daily protein intake important but especially after Duodenal Switch, protein is a necessity of daily life.
Vitamins, minerals and supplements will ensure the body has the nutrients it needs to function adequately and can keep cravings at bay. Deficiencies in vitamins and minerals can cause cravings for foods. Vitamin and minerals are essential to muscle function, red blood cell production, bone health, and numerous other physiologic functions. We may all slack off on our supplements occasionally but now is the time to get back into the habit of daily vitamins and mineral supplements. A daily vitamin, mineral, and supplement routine is a lifetime commitment after Duodenal Switch or any WLS. Here is a list of commonly used supplements. If you haven’t kept up with your minimum yearly laboratory studies, now is the time to be seen and have your labs done.
Exercise can increase weight loss, overall well being, mental well being, mood, alertness, improve digestion, improve sleep, and increases energy levels. Exercise does not have to be a daunting task. Simply adding 15-30 minutes of activity can give added benefits. Yoga, walking, dancing, lifting weights, hiking, and sports activities can be included or added to more traditional forms of exercise. There are many free online videos for all types of exercise available. This year we are teamed up with The Kinesis Centre to offer a 4 week training program that can be accessed from anywhere. A 4 week training program will be included in our 2018 Back On Track Grand prize.
Finding a new hobby can keep both your hands and mind busy, curbing the unconscious eating of foods that are high in sugar and carbohydrates. Adult coloring books, drawing, painting, knitting, crocheting, sewing, dance lessons, gardening, learning to play an instrument and many others are great ways to use your time and expand your quality of life and brain function. New hobbies can also help establish new coping skills. Our previous post on Coping Skills After Bariatric Surgery can be found here. There are a whole host of online videos for “how to” on new hobbies.
Teaming up with others can also help increase weight loss and compliance. Support from friends, family and other groups will assist you. There is a whole gamut of support group online and in person. If you have fallen out of the habit of attending our support group or webinars get back to them. You can find our schedule and announcements regarding webinars here. Our Central Valley Bariatric Facebook page also gives daily inspirational messages, protein recipes and articles and any new information or research available. There is also our Duodenal Switch Facebook Group. Anything that increases accountability is a benefit and motivates us to stay on track.
Experiment with new recipes and flavors that are bariatric friendly and within your dietary needs. There are so many options for quick and easy meals that are whole foods, high protein, and low carbohydrate. We have several recipes on our page for all stages following weight loss surgery and Duodenal Switch. However, there are endless option on the internet in Paleo, low carb, and high protein type recipes.
In the spirit of new starts and getting back on track 2018, we are having a giveaway with the basics to get back into the swing of things. This year we are looking for before and after weight loss surgical journeys for our Grand Prize. Share your weight loss journey! Don’t be shy, your journey can inspire others and/or motivate yourself. To enter the Back on Track 2018 Giveaway, please submit your weight loss surgical journey with before and after pictures to contact@dssurgery.com or you can also post your before and after pictures on our Facebook page. You will also need to sign a release for the use of your story on our website. We will draw 2 names from those that enter by announcing it on our FaceBook page or by e-mail on February 14, 2018. You must submit your mailing information to contact@dssurgery.com in order to claim the prize. You must be a verifiable patient of Dr. Ara Keshishian.
We are also doing 3 prizes of a 4 week training with the Kinesis Centre if you share an achievement picture on our FaceBook page . This achievement picture can be a milestone in your journey, something you’ve haven’t done before, a non-scale victory, a goal that you reached, anything that you are proud of achieving. Let’s do this 2018 Back on Track challenge!
Please remember that medications, health status, age, bowel motility, genetics, and diet all play a role in weight and weight maintenance. Please have a physician review your health history and medications.
*NOTE: Giveaway items may or may not be identical to the pictured items.
We are not affiliated with any of the products nor do we endorse any one type of product. There is no cash value to the prizes.
Importance of ProteinExclusive Member Content
September 08, 2016 2:43 pm
Fat, Protein – Post Duodenal Switch Diet
May 23, 2016 6:43 am
Fat and Protein after weight loss surgery…. This is a subject that seems to come up all the time.
What I recommend is “…Water, protein, vitamins, supplements and every thing else….”
Dehydration can cause a lot of problems, stay hydrated.
Weight Loss Surgery (WLS) is a surgically imposed catabolic state (surgical induced starvation). The weight is lost by not allowing enough caloric intake/absorption and forcing the body rely on stored sources of energy, mostly fat mass. The rationale for the high protein intake is to minimize net muscle mass loss during the catabolic state. Low carbs and low fat further push the body into catabolizing the fat mass, and reducing the net loss of protein content. As the fat mass is broken down it will release hormones and other byproducts that the body will eliminate. Hydration is crucial to every bodily function and even more so in the weight loss phase to allow for elimination of some of these byproducts.
The mechanism by which Duodenal Switch works during the weight loss phase is by limiting the caloric intake. Long term Duodenal Switch keeps the weight off due to the malabsorptive component as the caloric intake increases. Protein intake, Vitamin/Mineral supplementation and diligence in surveillance of vitamin/mineral levels is imperative and a life long commitment after WLS.
There are a number of different types of Fatty Acids. Our bodies naturally produce, from other components, all but 2 essential fatty acids: Omega 3 and Omega 6. Most fatty acids require bile salts to be absorbed within the small intestines. Those are the fatty acids that are absorbed to a lesser degree after Duodenal Switch. Medium chained fatty acids do not require bile salts and can be absorbed into the blood stream from the small intestines. Medium chained fatty acids are used for energy as they are processed in the liver. Medium chained fatty acids are actually given to patients with Short Bowel Syndrome to decrease fatty stool and increase their body weight. This is also a possible reason some fats cause DS patients more loose stools and others do not (medium chained fatty acids). Adding fats is a purely individualized process. Each person has a different length of small bowel, alimentary limb, common channel, percentage of excess weight to lose and metabolism. Patient’s tolerance for fat in regards to vitamin/mineral levels, stool consistency and frequency is completely individualized.
Fats and Fatty acids can be divided according to their structure in groups:
A) Saturated Fat (animal fats, butter, lard- solid in room temperature)
B) Unsaturated Fat (liquid in room temperature)
The main focus in the weight loss phase should be hydration, hydration, hydration, protein, low carb, low fat and vitamin/mineral supplementation (page 22). Rest is key in the early post op phase but gradually adding exercise is also important in ensuring the body does not breakdown muscle mass. Adequate intake of protein and use of muscles diminishes the bodies natural response of breaking down muscle mass in a low caloric intake state.
Post Surgical Needs for the first 90 days in order of importance:
This is to allow healing to take place before adding additional stress on the body and surgical sites.
Minimum of 64 ounces of fluids daily
Minimum 80-100 grams of protein daily (protein requirements are based on ideal body weight)
30 gms by 30 days post-op
60 gms by 60 days post-op
90 gms by 90 days post-op
Vitamin/Mineral Supplements
Low carb
Low fat
Rest (early Post-op)
Exercise
Proteins are important, not only for structure (muscle) but for functions. We know that proteins and amino acids are involved in all aspects of our body’s function. This is even more critical during the rapid weight loss phase. Protein needs may increase and change based on health status, pregnancy, surgeries, healing, etc.
When it comes to fat, I do not recommend patients consuming excessive amounts of fat- At the same time I do not recommend patients go on a low fat diet. There is this misconception that since DS is causing fat and fat soluble vitamin malabsorption, then taking more fat (in excessive amounts) can solve the problem of vitamin deficiency. How about the possibility that some patients are causing their own vitamin deficiency by taking large volumes of fat which may results in more frequent bowel movements and decreased vitamin absorption.
It is not to be forgotten that each patient will respond differently with dietary changes after duodenal switch. Some patients may tolerate more and some less fat in their diet. After the initial 90 day post op phase I recommend that patients go slowly in adding new food items by giving it several days before adding another food item. i.e.; add carrots for 3-5 days to see how your body handles it before attempting to add another new item. The above is not the entire weight loss process or education and is only a small portion of the education needed before undergoing any WLS procedure. These recommendation are my recommendations for my patients with the Hess technique for Duodenal Switch.
Metabolic Processes In Different TissuesExclusive Member Content
February 11, 2016 8:29 am
Pregnancy And Weight Loss SurgeryExclusive Member Content
November 21, 2015 5:34 pm
Duodenal Switch and Fat in The Diet
May 21, 2015 12:35 pm
When I perform the duodenal switch operation, the common channel is a percentage of the total small bowel length and I also account for the patient’s metabolic rate. Two individuals with a BMI of 50, should not have the same common channel. If we compare two patients, one of them is a 20 years old male who is 6’2″ and the second patient is a 60 year old female who is 5’4″, we can see how this applies. These two patients have very different metabolic needs and requirements. When the Duodenal Switch is performed in this fashion, the common channel based on a percentage of total small bowel length and metabolic needs, the patients post op diet works best when it is a well balanced, protein based diet. The basic principals are : Hydration (water), Protein and Everything else, low carb, avoid artificial sweeteners, avoid carbonated drinks, have frequent smaller meals and avoid processed food. Listen to you body as to what it tolerates and what it doesn’t. This is what I recommend for my patients.
I am not aware of any scientific evidence that proves any benefit to excessive amounts of fat for DS patients who have had their length of the common and alimentary bowels based as a percentage of the total length.
My recommendation are to have a well balanced high protein diet. I do not recommend a low fat diet, except in the healing phase after surgery. However, there is no reason to consume excessive amounts of fat long term.
High fat diet is used to facilitate bowel movements for some patients who have constipation. It may be prudent to try and identify what may be causing the constipation and correct or eliminate them before one resorts to a very high fat diet as a “treatment” for constipation after Duodenal Switch. The possible causes for constipation after duodenal switch may be metabolic-organic (where some patients have infrequent bowel movements before DS, hypothyroidism), length of the common and the Alimentary channels and medications (pain meds, narcotics, antidepressants).
In addition, Medium Chain Fatty Acids do not require bile salts to be absorbed and are directly absorbed into the Portal Vein in the liver. Medium Chain Fatty Acids are not malabsorbed post Duodenal Switch. Medium Chain Fatty Acids included Caproic acid, Caprylic acid, Capric acid, and Lauric acid. Commonly found in varying amounts within coconut oil and palm oil. MCT supplement is made with Medium Chain Fatty Acids.
In summary, I recommend that Duodenal Switch patients who have had surgery with our practice have a high protein balanced diet. I do not recommend avoiding fat, or going on a low fat diet. I am not sure if there a reason to consume excessive amount of fat, which may in fact have unexpected metabolic and nutrient consequences.
Every patient, as their weight stabilizes, will find what works and what does not work for them. Some patients will tolerate a higher fat intake and other will not be able to tolerate higher fat intake.