Category: sleeve
SIPS-SADI and ASMBS
December 31, 2023 1:21 pm
Revision of a Sleeve Gastrectomy or RNY
August 31, 2015 6:32 am
These are examples of two types of patients referred to us for revision surgery.
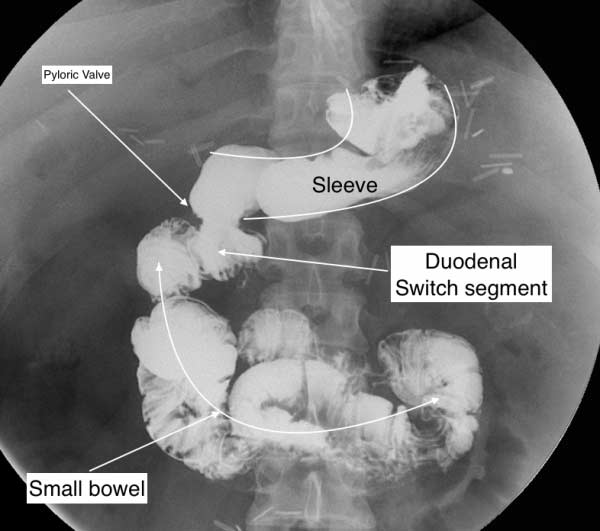
The first example is a gastric bypass that we revise to the duodenal switch operation. The upper GI series after the revision, shows a “banana shaped” stomach, the pyloric valve and the duodo-ilesotomy anatomosis component of the duodenal switch.
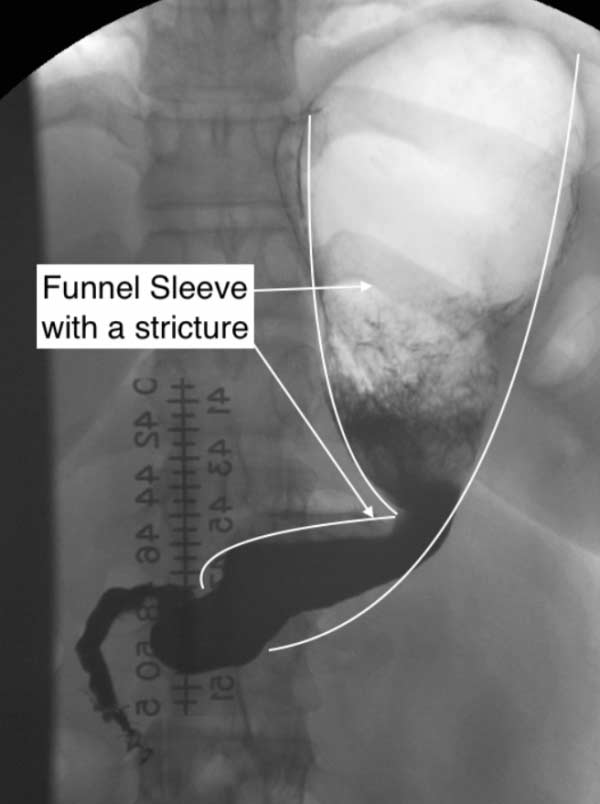
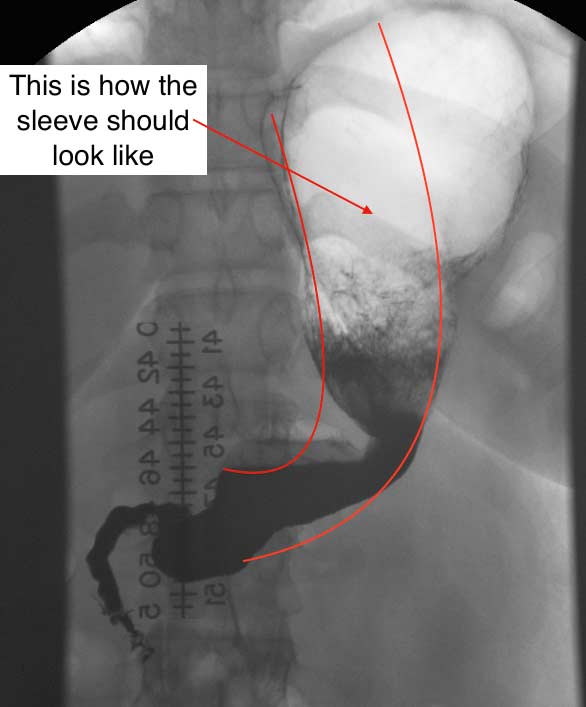
The second example, images noted below, is that of a sleeve revised to the duodenal switch – both operations done at different institution. Note how the stomach is not a “banana shaped” and more like a funnel with a narrowing at the bottom of the stomach- a stricture.
Surgical Treatment of Gastric Fistula
August 05, 2015 7:45 pm
Weight Loss before Weight Loss Surgery?
October 19, 2014 2:54 pm
I am frequently confronted by the question “Are you going to make me lose weight before I have weight loss surgery”? My answer is no, for several reasons, it makes little or no sense and there is scant scientific data to support it.
1-Anatomical and 2-psychological-behavior related variables have been suggested as the reasoning for the recommendations for diet before weight loss surgery.
Let’s see what the scientific evidence says about this.
1-Liver can be divided into two anatomical lobes. The tail end of the left lobe may extend all the way to the upper left side of the abdomen covering the upper 1/3 of the stomach, the gastro-esophageal junction (GEJ) and the esophageal hiatus. It was suggested that the access to the GEJ could be made easier, if the left lobe of the liver was smaller.
“A decrease in the size of the liver by 18% was shown in patients who were subjected to a very low-energy diet for 12- weeks.” This was published by Colles et.al in a small study of 39 subjects.
It is important to appreciate that this reduction in liver size meant that a patient would have to tolerate an ultra low caloric diet (less than 500/day) for 12 weeks. The interesting observation was that even with this reduction in the size of the liver there was “… no difference shown in morbidity, mortality, hospital stay, and decrease in morbidity- associated diseases whether there is preoperative weight loss or not.”
2-Behavior modifications have been entertained as a necessary element to the success of adjustable gastric banding. Numerous studies have shown that there is no predictive value of preoperative weight loss in relation to the weight loss after surgery.
The overwhelming scientific data suggest that there is no value to subjecting a weight loss surgical patient to a pre-surgical ultra low caloric diet.
“The California Department of Managed Health Care recently conducted a review of weight loss prior to bariatric surgery and concluded that “there is no literature presented by any authority that mandated weight loss, once a patient has been identified as a candidate for bariatric surgery, is indicated. This comprehensive review states that mandated weight loss prior to indicated bariatric surgery is without evidence-based support, is not medically necessary, and that the risks of delaying bariatric surgery are real and measurable.” Published by the American Society for Metabolic and Bariatric Surgery in March 2011.
- Weight loss Medications compared to surgery February 20, 2024
- SIPS-SADI and ASMBS December 31, 2023
- Survey December 16, 2023
- Long Term Outcome Survey December 1, 2023
- Weight Loss Injection May 10, 2023