Category: gallstone
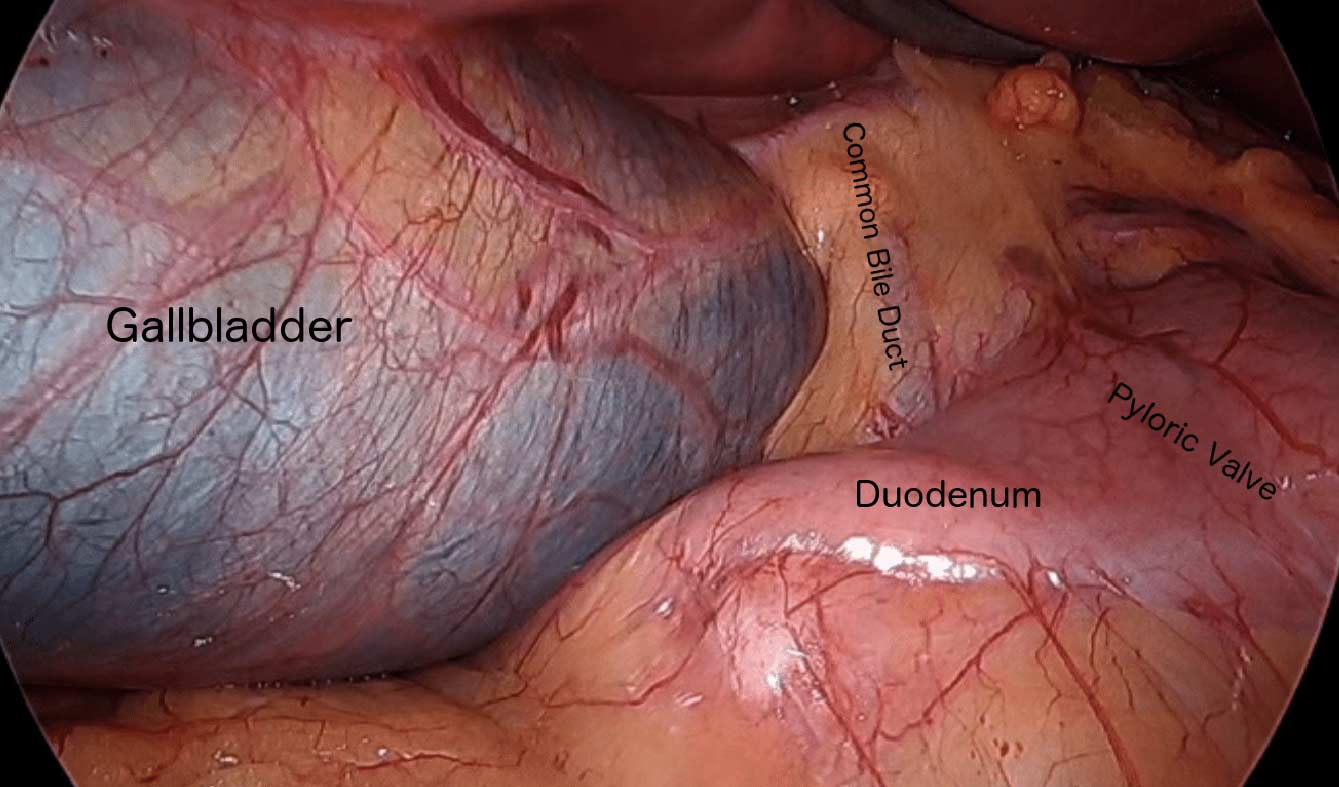
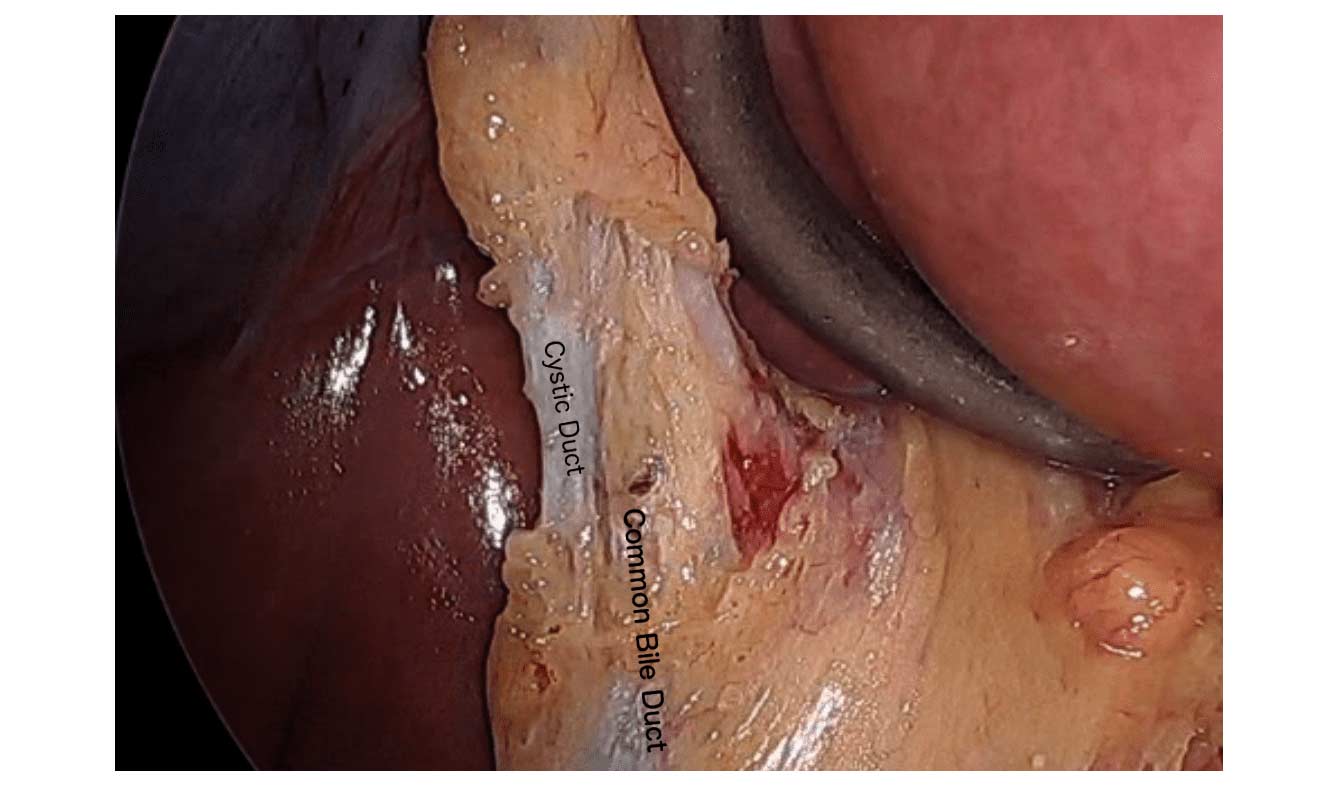
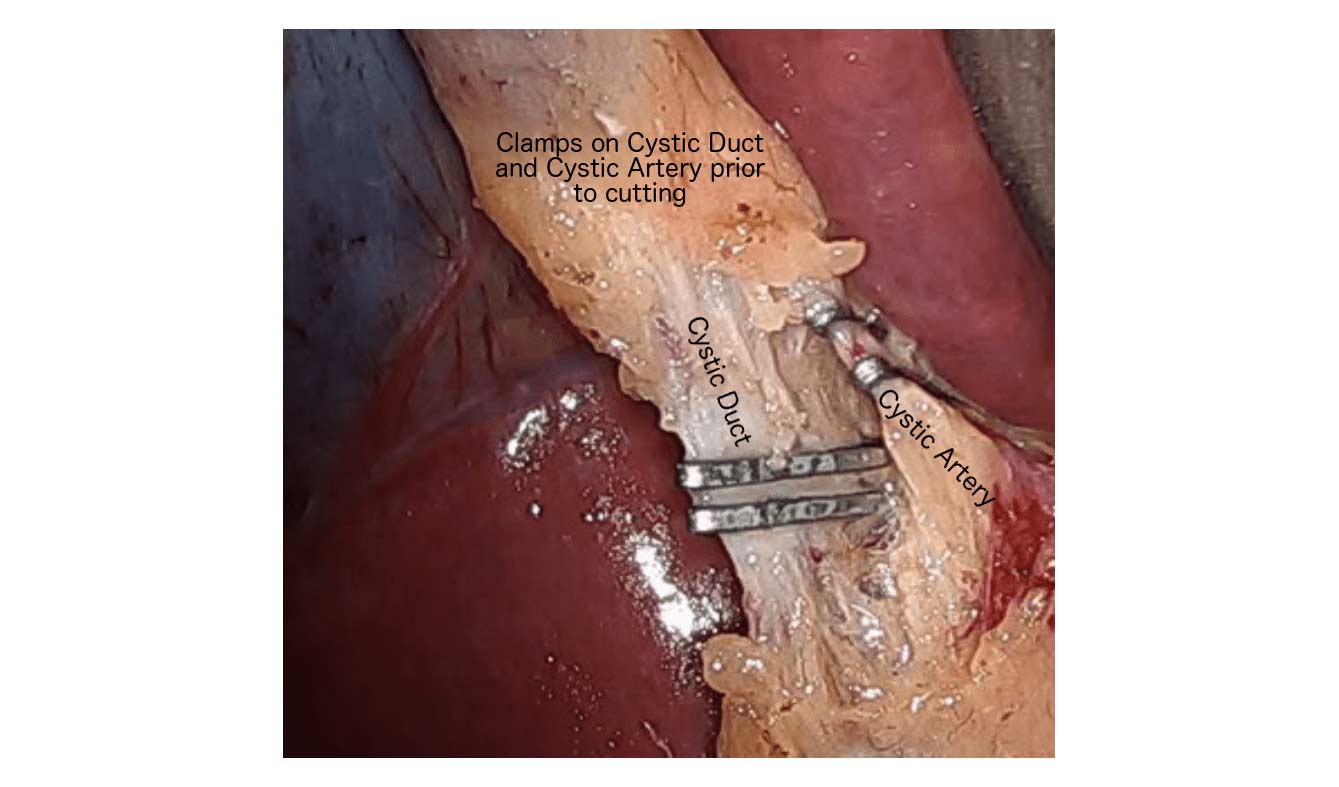
Cholecystectomy-Gallbladder Removal
September 10, 2018 9:44 am
There are differing opinions, based on a broad set of scientific publication, wether or not gallbladder should be removed at the time of weight loss surgery. Obviously, Cholecystectomy is a stand alone general surgical procedure that is often performed due to gallstones and/or gallbladder disease with a variety of symptoms. However, the focus of this blog will deal with Bariatric Surgery and Cholecystectomy.
Rapid weight loss can increase a patients chance of forming gallstones. This rapid weight loss can be as little as 3-5 pounds per week. Weight loss surgery can increase your risk for gallstone formation. Several of the common thought processes the mechanism of this is, obesity may be linked to higher cholesterol in the bile, larger gallbladders, high fat diet and larger abdominal girth.
When a patient is having the Duodenal Switch (DS) Bariatric operation, or having a revision of a failed gastric bypass to the DS, I always remove the gallbladder. This is because there isn’t an anatomical route to utilize endoscopic procedure for an ERCP should the need rise.
In the case of a patient undergoing Vertical Sleeve Gastrectomy, if there are any indications or complaints of abdominal pain then an ultrasound is done. If there are findings of gallstones or other disease of the gallbladder, then a cholecystectomy is performed at the same time as the Sleeve Gastrectomy.
In my opinion, every patient having the Gastric Bypass (RNY) should also have the gallbladder removed because of the anatomical limitations after surgery that prevents the use of ERCP if needed. Some clinicians will place the patient on a long term medications to reduce the chance of gladstone formation after surgery, which themselves have side effects limiting the compliance in most patients.
Further information on Common Bile Duct Dilatation and ERCP
Evaluations of Gallbladder Disease And Function
April 11, 2015 7:03 am
Gallbladder disease can include both anatomical and functional condition. We are familiar with gallstones. Bile acids, Lecithin (a phospholipid), and cholesterol are present in the Bile. When the proportional percentage of each one of them is outside a very narrow range, gallstones are formed. Approximately 75% of the gallstones are formed because of the supersaturation of the content of the gallbladder with cholesterol which results in cholesterol stone formation. The rest are pigmented stones.
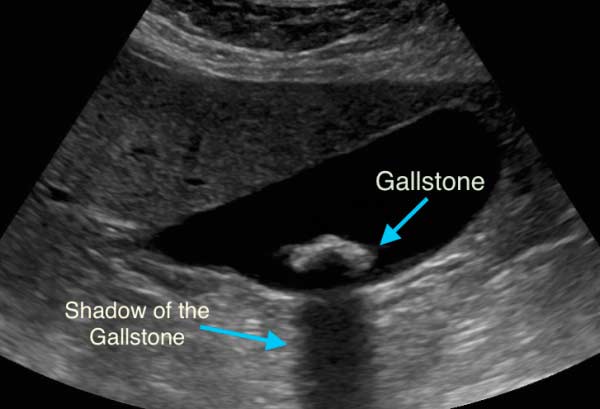
Gallstones are usually identified by ultrasound and they are seen as shadows.
There are patients that have a normal gallbladder ultrasound result that continue to have signs and symptoms of gallbladder disease, such as abdominal pain in the right upper quadrant, nausea and vomiting with fatty meals, and bloating to name a few. These patients should be evaluated by a dynamic HIDA scan.
A dynamic HIDA scan study evaluates the function of the gallbladder, by creating a movie of the gallbladder, where as an ultrasound takes pictures of the gallbladder.
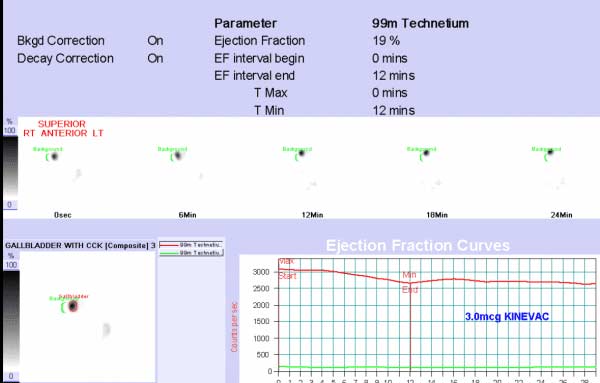
In a dynamic HIDA scan, and contractility of the gallbladder is reported in form of ejection fraction (%EF). This represent the amount of gallbladder contraction in response to the stimulation by a fatty meal mediated thru cholecystokinin (CCK). A normal EF is greater that 35%. Anything less than than with the sign and symptoms of gallstones, should be highly suspect for acalculous cholecystitis. Calculus because there is no stone.
(The bright white collection represents the filling of the gallbladder)
This short movie represents the uptake of the radio nuclear material in the gallbladder and its normal secretion in the small bowel.
These are the static images before the injection of CCK.
Following the injection, digital subsection of the images measure the amount of nuclear activity of the gallbladder before and after contraction and an Ejection Fraction is calculated.
- Weight loss Medications compared to surgery February 20, 2024
- SIPS-SADI and ASMBS December 31, 2023
- Survey December 16, 2023
- Long Term Outcome Survey December 1, 2023
- Weight Loss Injection May 10, 2023