Category: Revision of RNY
Shared Success Story: Cyndi E. Had a Gastric Bypass to Duodenal Switch Revision
June 17, 2014 6:29 am
My journey to lose weight has taken most of my life. Losing weight is not just about food or eating too much, but a combination of genetics, emotions, and habits. My experience began at age 13 and has continued throughout my life. I have tried everything! I had a previous RNY Gastric Bypass, and knew something was wrong. I had seen another Bariatric surgeon who said there is nothing I can do for you because you failed. My primary Doctor asked me “does your husband love you?” Of course, but what does that have to do with me knowing there is something medically wrong with me? Again, I was brushed off and told to come back in two weeks. Leaving that day, I knew I was never going back. I went home and googled, “Bariatric Surgeon”, as I had for the past 3-4 years. Then, through a series of events was put in touch with Barbara Metcalf, a bariatric nurse, who lived in my town. As I explained my story to Barbara, she shared information with me about Duodenal Switch operation, and gave me names of two surgeons.
I contacted Dr. Ara Keshishian, in Glendale, and had a consultation that week. Meeting “Dr. K” was amazing! It was the first time a Doctor did not blame me for my weight. He explained that each weight loss surgery has different measures of success, percentages of weight loss by surgery, and outcomes. Dr K told me that I may have been a success with the RNY Gastric Bypass, based on the numbers, however it became clear that I did have complications associated with the gastric bypass. I was scheduled for an Endoscopy the next week, which Dr. K performed. The endoscopy confirmed that I had a Gastro-gastric Fistula. Simply put, this was an abnormal connection between the bypassed stomach and the small pouch created by the RNY Gastric Bypass surgery. Food could travel two ways, thus rendering the Gastric Bypass ineffective, and causing weight gain.
Dr. Keshishian performed a revision to the Duodenal Switch Surgery on May 31, 2013. This procedure corrected my anatomy, enabling me to lose weight and regain my health once again. I have had wonderful success and I have lost 104 pounds. More importantly, I do not have the complication of the dumping syndrome, episodes of nausea and vomiting and am leading a normal life. I am not prisoner to my weight, what I can and cannot eat or the fear of weight gain.
I contacted Dr. Ara Keshishian, in Glendale, and had a consultation that week. Meeting “Dr. K” was amazing! It was the first time a Doctor did not blame me for my weight. He explained that each weight loss surgery has different measures of success, percentages of weight loss by surgery, and outcomes. Dr K told me that I may have been a success with the RNY Gastric Bypass, based on the numbers, however it became clear that I did have complications associated with the gastric bypass. I was scheduled for an Endoscopy the next week, which Dr. K performed. The endoscopy confirmed that I had a Gastro-gastric Fistula. Simply put, this was an abnormal connection between the bypassed stomach and the small pouch created by the RNY Gastric Bypass surgery. Food could travel two ways, thus rendering the Gastric Bypass ineffective, and causing weight gain.
Dr. Keshishian performed a revision to the Duodenal Switch Surgery on May 31, 2013. This procedure corrected my anatomy, enabling me to lose weight and regain my health once again. I have had wonderful success and I have lost 104 pounds. More importantly, I do not have the complication of the dumping syndrome, episodes of nausea and vomiting and am leading a normal life. I am not prisoner to my weight, what I can and cannot eat or the fear of weight gain.
Our First Featured Success Story
May 16, 2014 9:47 am
Patricia Welborn
StomaphyX does not reduce regained weight after a failed gastric bypass.
April 17, 2014 9:26 pm
Gastro-gastric fistula after gastric bypass operation
May 10, 2013 9:09 pm
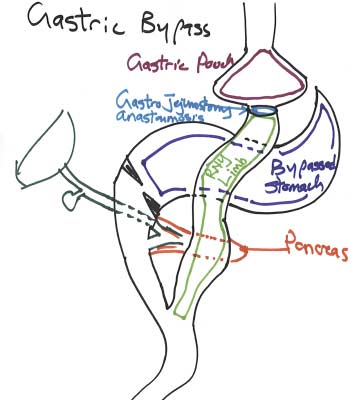
One of the complications of gastric bypass is a gastro gastric fistula. This happens when a connection between the gastric bypass pouch develops to the remnant stomach. In a gastric bypass operation, a very small pouch is created from the stomach, and connected to a segment of the small bowel.
The purpose of this operation is to decrease over 95% of the volume of the stomach. In theory, the benefits of this is to reduce the volume of food that can be consumed. Over time, the size of the stomach pouch, and/or size of the gastro-jejunostomy anastomosis might stretch. This result in weight regain that is very commonly seen in about 3 years after a gastric bypass operation.
One of the complications of gastric bypass is a gastro gastric fistula. This happens when a connection between the gastric bypass pouch develops to the remnant stomach. In a gastric bypass operation, a very small pouch is created from the stomach, and connected to a segment of the small bowel.
The purpose of this operation is to decrease over 95% of the volume of the stomach. In theory, the benefits of this is to reduce the volume of food that can be consumed. Over time, the size of the stomach pouch, and/or size of the gastro-jejunostomy anastomosis might stretch. This result in weight regain that is very commonly seen in about 3 years after a gastric bypass operation.
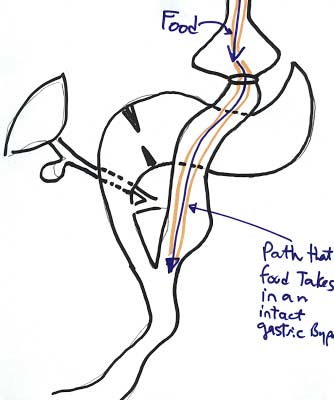
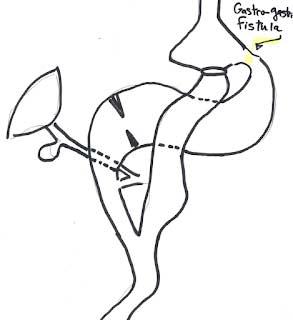
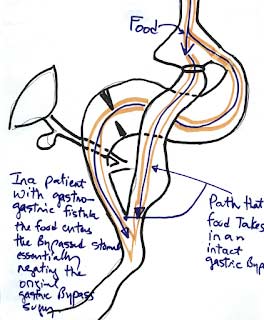
Another possible explanation for weight regain may be an abnormal connection that may develop over time between the bypassed stomach and the small pouch that was created. This abnormal connection is known as a gastro-gastric fistula. In a patient who may have a gastro-gastric fistula, the food can travel down the gastric bypass path or enter the bypassed stomach and go down the path of a normal anatomy.
In these cases, the physiological effect of a gastric bypass procedure becomes ineffective.
The treatment that I favor most for correcting the complication of the gastro-gastric fistula is is to revise the gastric bypass to the duodenal switch operation.
Revision or Reversal of the Duodenal Switch
September 08, 2012 7:00 pm
A significant portion of my practice involves the revision of the Gastric bypass and Adjustable Gastric Banding procedures to the Duodenal Switch operation. The re-operations are necessary to correct the complications that have been caused by these procedures. There are also instances of required revisions due to inadequate weight loss or weight regain. Our website contains detailed information regarding reasons for revision and the reversal of weight loss surgical procedures. I think it is important to mention that these complications are very common and almost never have anything to do with the patient’s behavior.
Duodenal switch operations may also require reversal or revision. The general reasons for a revision or reversal of the Duodenal Switch is the same as for all weight loss surgical procedures and include a variety of reasons. The reversal or revision of the Duodenal Switch operation is one of the simplest revision surgeries that I perform.
Let’s review a few facts about Duodenal switch.
The Duodenal Switch procedures has two components:
1.) The sleeve gastrectomy
2.) The separation of the biliopancreatic secretions from the food to limit its absorptions.
Clearly, the portion of the stomach that has been removed cannot be reintroduced to the abdominal cavity. The second part of the operation can, however, be easily “undone.
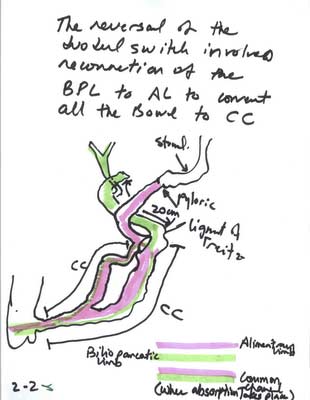
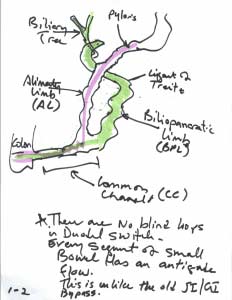
The assumption is that the bowel needs to be divided again and re-anastomosed to reconstitute its continuity. This revision or reversal of the Duodenal Switch operation is done by simply creating a new connection between a new anastomosis, located between the biliopancreatic limb, and the alimentary limb.
If a complete reversal is needed, then the connection is made just distal to the ligament of Treitz. Ligament of Treitz is the transition point between the duodenum and Jejunum. This single anastomosis is safe and simple to perform and does not involve removing the previous staple lines.
If a partial revision is needed, or the common channel needs to be lengthened, then the anastomosis is made further proximal to the junction of both the alimentary limb and the biliopancreatic limb, but distal to the ligament of Treitz to allow for increased absorption of the calories and nutrientsIn my opinion, the revision and reversal of the Duodenal Switch operation is, from a technical perspective, the simplest of all revisional weight loss surgical procedures.
In my opinion, the revision and reversal of the Duodenal Switch operation is, from a technical perspective, the simplest of all revisional weight loss surgical procedures.
Yearly lab and medication requests
October 17, 2011 5:28 pm
First, we now have preferred laboratories that have partnered with us. The laboratory results are expected to be sent to us electronically, which should cut down on the time between the blood draw and when the results are available to us. The information on the preferred labs is located at: https://www.dssurgery.com/lab. Needless to say, there are no financial incentives for us. You should also check with one of the labs, as well as with your insurance company, to make sure that they are a contracted facility and that the order is covered under your policy. It is your responsibility to make sure that your insurance company will pay for the labs ordered. We are in no way responsible for the verification of benefits for the laboratory services that we order.
Second, we have had to change the way we order our yearly lab work. As most of you are aware, it is critical that weight loss surgical patients have continuous yearly follow-up care and monitoring. It is critical that the patients continue to receive yearly follow-up care, not only by doing their scheduled laboratory studies, but also by a yearly follow up in office exam. We provide a comprehensive follow-up plan to the patients who have had the the Duodenal Switch or Revision from other failed weight loss surgical procedures. This includes ordering the laboratory studies, review and interpretation of the results, as well as office visits as frequently as required or deemed necessary.
Does Size Matter
September 28, 2009 12:14 pm
The scientific basis for weight loss surgery, for the majority of the part relies on the premise that overeating and lack of exercise are the principal mechanisms contributing to the increase in the incidence of obesity over that last decade. Much has been said about our unhealthy life style that involves sedentary activity and immobility. Fast foods, high fat content meals, calorie dense food, are some of the examples of possible contributing factors to this health crisis.
The contrary position would be that there are other factors that contribute to obesity. These may include environmental factors, food preservatives, genetics, and exposures to toxins.
If one assumes that the over eating is the core problem, then you can also assume that the most successful operation will have the smallest stomach, since it will reduce the ability to over eat most drastically. This is where the scientific evidence does not support the theory and we all have to reassess the principal that the treatments are directed toward.
Recently there have been a number of studies that have been published in scientific journals that suggest size of the stomach or the pouch does not matter. So if obesity is the result of over eating then the operation that provides the smallest stomach must work the best. This argument should be true for the pouch size after gastric bypass, and the opening of the gastro-jejunostomy (connection between the stomach pouch and the small bowel connected to it after the gastric bypass, RNY operation). The same theory applies to the sleeve gastrectomy of the duodenal switch operation.
This argument that over eating and lack of exercise is the major contributing factor seems to be loosing ground.
The studies below are outline to demonstrate the disparity between the theory and the lack of scientific support for it.
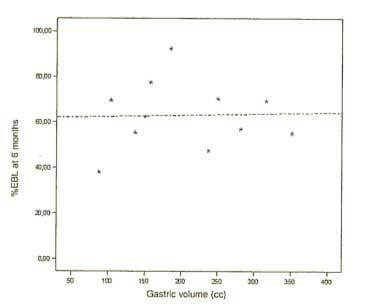
1- Sanchez-Pernaute et.al. (Obesity Surgery, 17, 2007) reported that “After DS, gastric tube volume is not directly related to weight changes.” He proposed that there are other factors that may contribute to the weight loss than the size of the gastric tube.
This graph taken from the referenced study above shows that the size of the stomach sleeve does not correlate with the %EBWL in DS patients. The smaller stomach sleeve does not result in the more weight loss.
2- O’Connor et.al. (SOARD 4(2008)399-403) reported that “With construction of divided, vertical, lesser curve-based small-volume (=<20cm3) gastric pouches, the actual size of the gastric pouch did not correlate wit the %EBWL at 1 year after Laparoscopic, GB [gastric bypass]”.
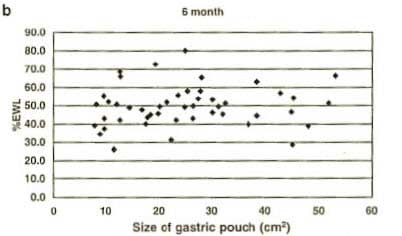
3- Nishie et.al. (Obesity surgery, 17, 2007) concluded that “pouch size area, measured by routine UGI [upper GI series] on the first post operative day, does no influence short-term postoperative weight loss”.
This a sample of a number of graph that Nishie published in her study. The similar graphs were for 3, 12, and 24 months. They all had a flat line distributions. What they are showed was regardless of the time lapsed from surgery, the %EBWL was independent of the size of the pouch measured immediately post operatively.
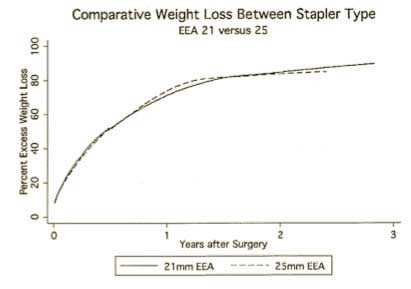
4- Cottam et.al. (Obesity Surgery, 2009, 19:13-17) reported “The level of restriction or the presence of stenosis achieved by different circular stapler sizes does not have a significant role in weight loss”.
This study was focused on the size of the opening that is made between the stomach pouch and the small bowel in the gastric bypass (RNY) operation. The weight loss did not differ in the two groups of the patients. One group had a 21mm stapler and the other one 25mm stapler used. The weight loss, as measured by %EBWL was nearly identical in both cases.
In summary, the size does not seem to matter. The size of the stomach pouch, when it gets to a certain size in not important. The smaller stomach pouch or the narrower connection of the stomach and the small bowel will not make a patient loose more weight. Doesn’t this prove, to at least some degree, that there is much more to obesity than the simple notion of eating small portion and exercising?