Category: Osteoporosis
Osteoporosis Medications
March 28, 2020 7:22 pm
There are a number of lectures, posting that we have done over the years on this topic. However the questions of osteoporosis medications and their benefits and risks comes up often.
The links are attached:
Here is an updated list of medication that I had previously published. I made some clarification to explain how the medications work. There are different classes of medications and the detail of the action and soda effects were described earlier at a blog post.
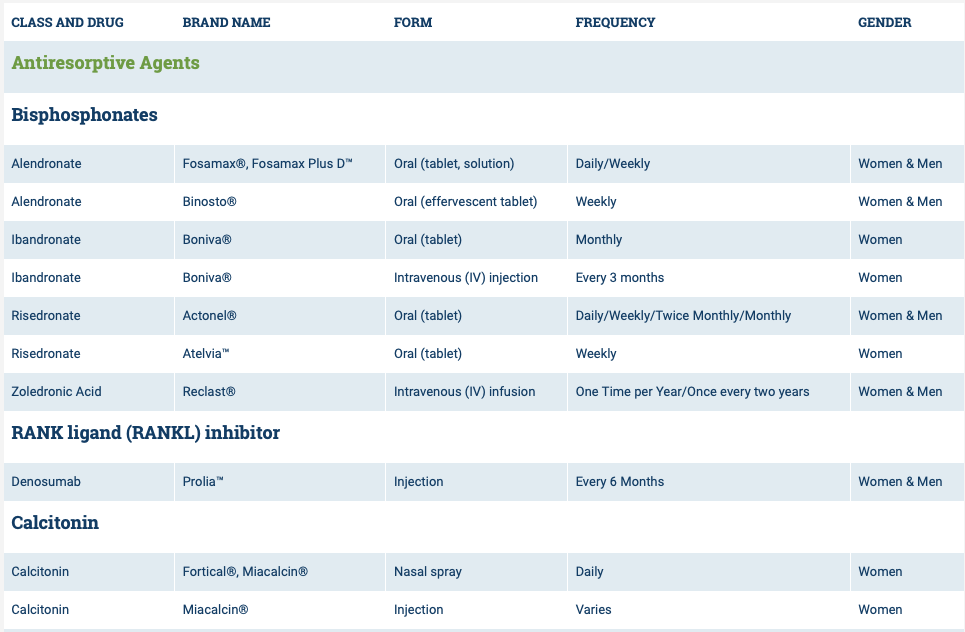
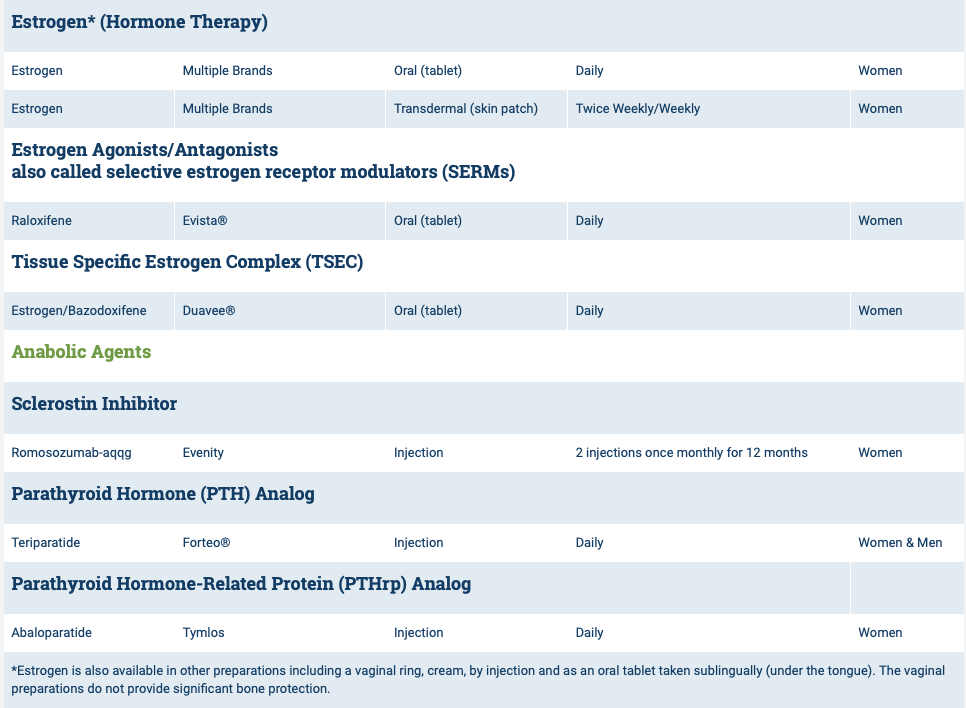
List of medications that effect bone health.
The table is obtained from https://www.nof.org site.
Osteoporosis Medications, Action and Side Effects
May 25, 2019 3:40 pm
Treatment options should be approached is a global and systemic fashion. It is critical that the nutritional status is at its best possible and optimized for important healthy bone vitamins and minerals. Low protein needs to be corrected. Special attention should be given to nutrients, minerals and vitamins. These include Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1/K2to name a few.
Healthy bones require ongoing and routine force in the form of exercise to remain health. Just as exercise improves muscle strength, it also improves bone health. Exercise is also critical in improving bone structure and density. Ideally, exercise should be weight bearing and resistance. Examples include: hiking, walking, jogging, climbing stairs, playing tennis, and dancing. Resistance type exercise is weight lifting and resistance bands. These exercise work by creating a pull or force on the bone either by gravity, movement or weight. Always check with your physician before beginning an exercise routine, start slowly and building up to longer periods of time. The ideal goal would be at least 30 minutes a day, every day, if you are able.
We frequently see patients immediately started on osteoporosis medications without checking or improving some of the nutritional markers noted above or without looking at exercise history. In some case, the medication recommended are contraindicated due to nutritional status.
The medications can be grouped in to those that help with new bone formation (Anabolic agents) or those that help by suppressing the bone breakdown phase (Antiresorptive agents).
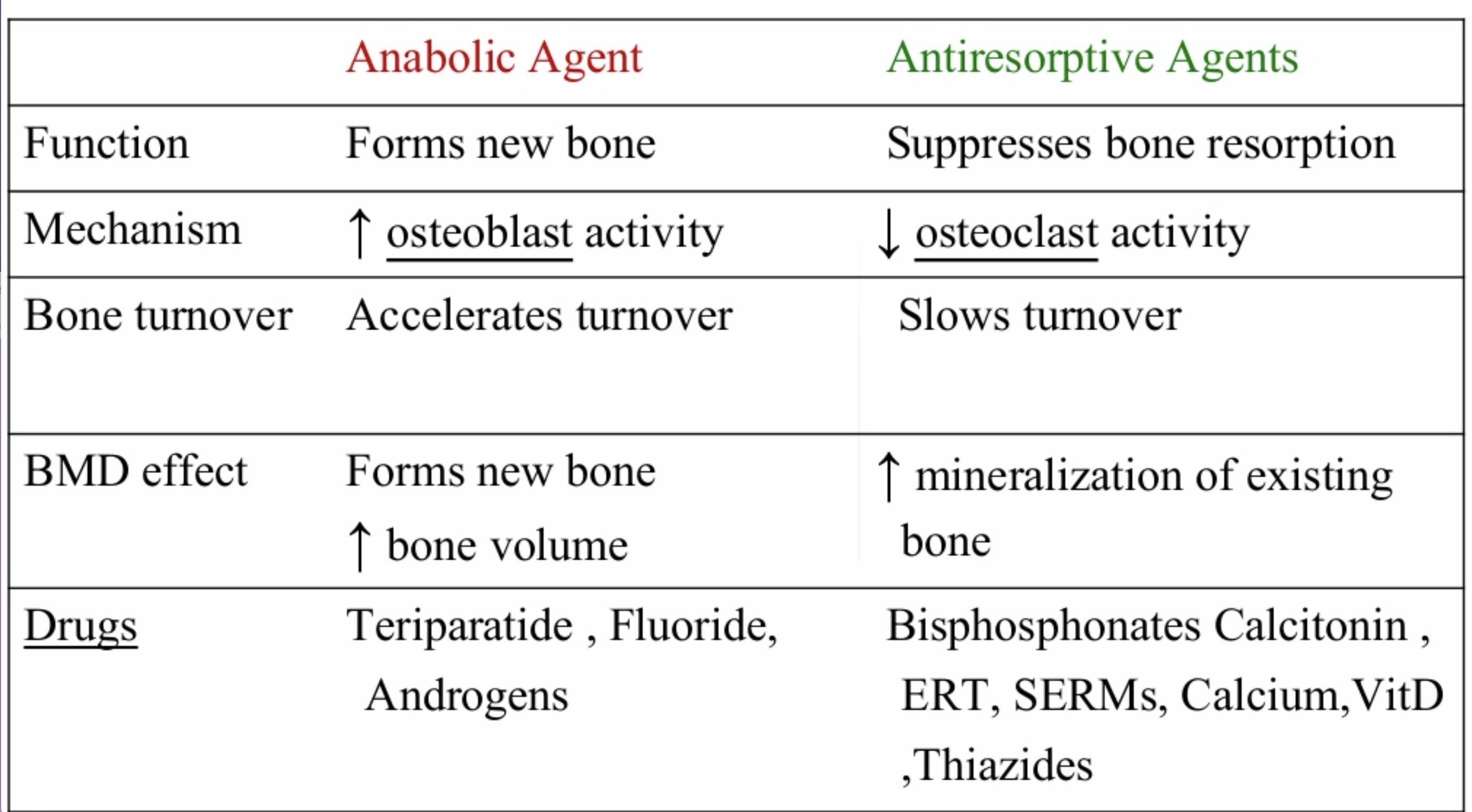
National Osteoporosis Foundation has an exhaustive list (below) of medications for treatment of Osteoporosis.
The table below outlines the side effects and mechanism of the actions of the common medications used for treatment of osteoporosis which was published by the University Health News Publication on August of 2014.
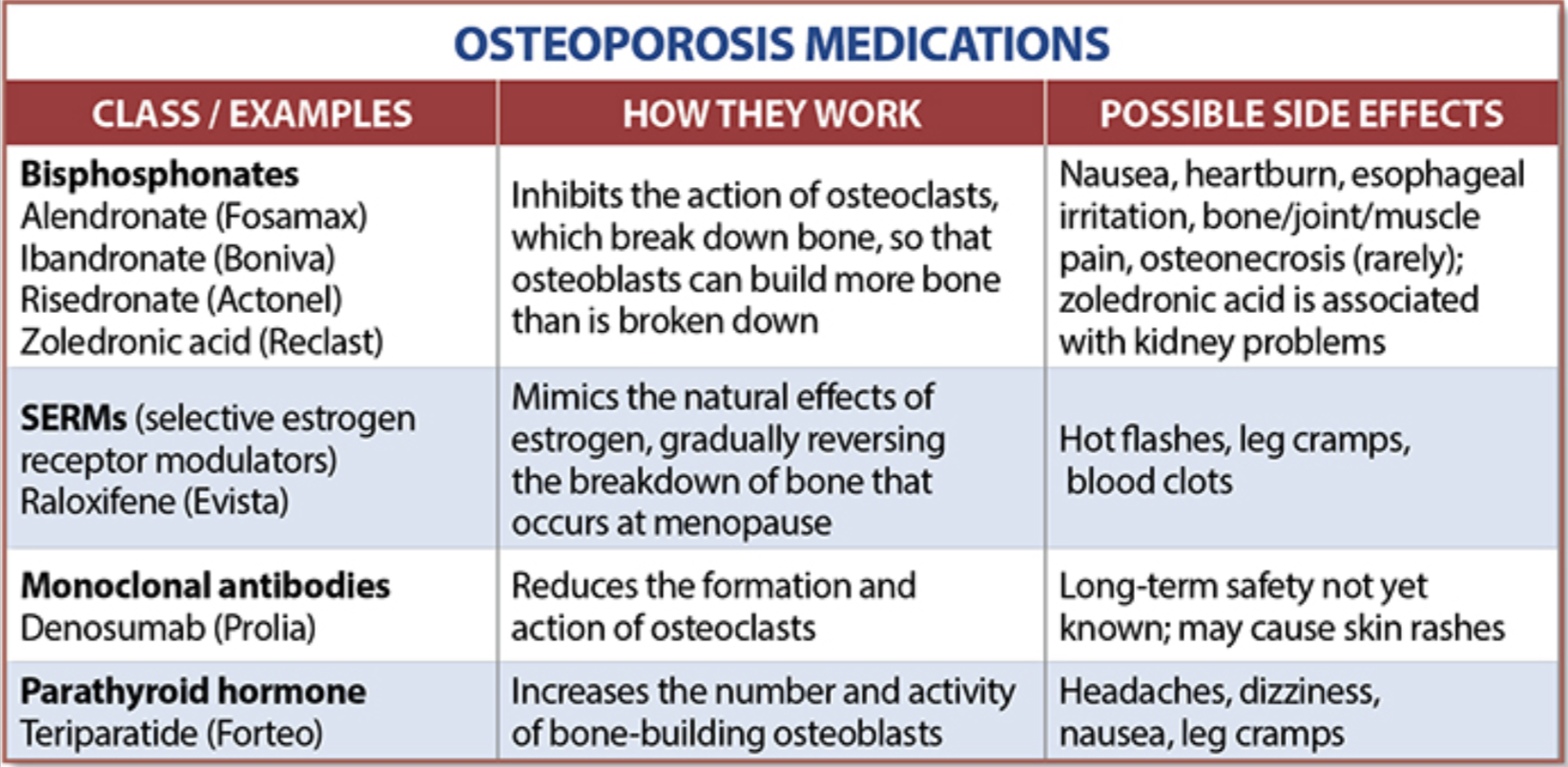
With all this information, the few points to remember is that the most important factors in healthy bone structure are the nutritional status Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1 levels.
This is an animation of normal bone Metabolism. It shows how bone structures is taken down and rebuilt continuously. This allows for a healthy bone maintainence as we age. The key is the balance of breakdown (osteoclast) and the build up (osteoblast) activity is regulated. Osteoporosis develops when there is more breakdown that build up. 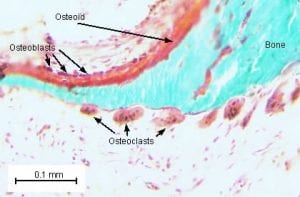
With permission of Dr. Susan Ott of University of Washington.
Additional information available on her site.
Past blogs on Bone Health.
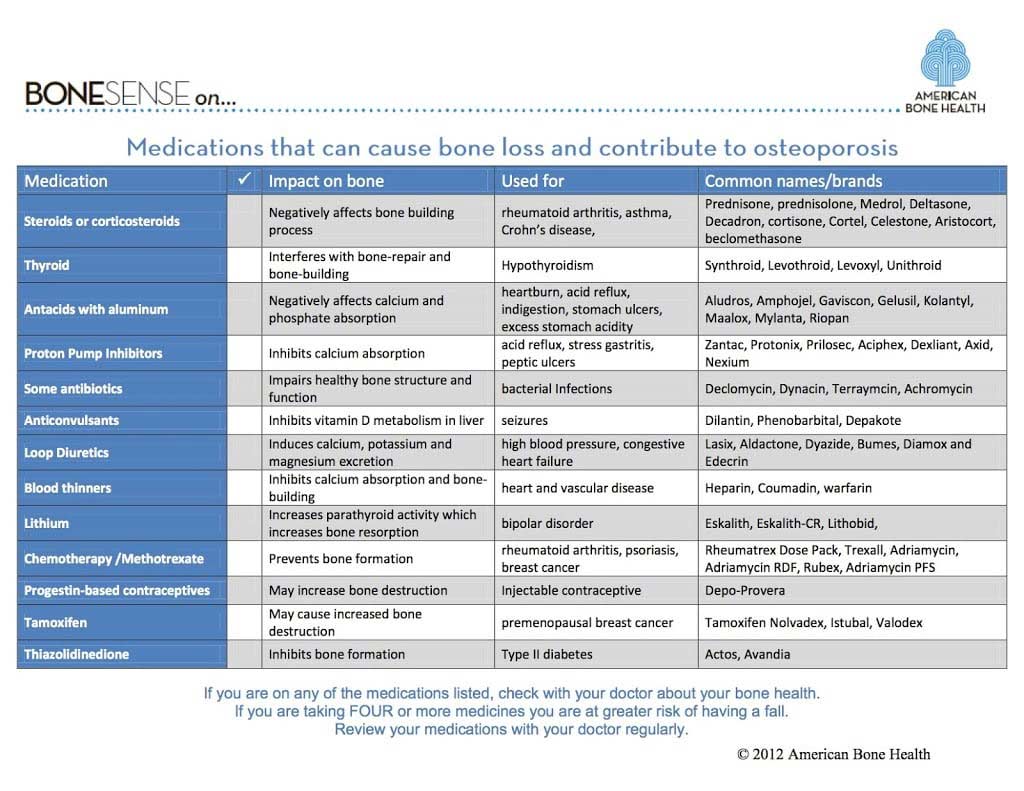
Medications that negatively affect bone loss and contribute to Osteoporosis (Moved)
March 31, 2015 4:07 pm
An Example of Medications that may cause bone loss
It should be noted that this list is NOT all inclusive and gives the type of medication but does not list all the medications in that category that may affect bone health. I would also like to point out that the Proton Pump Inhibitor labels should probably be changed to “Acid Reducers” as reducing acid is the issues. https://americanbonehealth.org
September 3, 2014 Group Meeting & Webinar Laboratory Studies and Vitamin K2Exclusive Member Content
September 06, 2014 8:03 pm
Patch or Spray Vitamins
August 15, 2014 10:37 pm
At the last group meeting, there were several questions whether vitamin D and other vitamins would be absorbed via patch (transdermal) and spray (buccal/sublingual) routes. After reviewing several resources, the only article I could find was for transdermal Vitamin D absorption. However, if we look at the mechanism for each route we can make an educated assumption.
Transdermal route of absorption (without additional absorption enhancers) (ref) requires a molecular mass less than 500 g/mole, high lipophilicity (affinity to fat or lipids), and low required daily dose (less than 2mg). The fat-soluble vitamins are definitely lipophilic, all of them have molecular weights less than 500 g/mole and daily dose is under 2mg. It seems that hydrophilic medications (that have an affinity to water) may have less ability to be absorbed with this route unless a chemical enhancer is added to the product. Most vitamins and minerals have lower molecular weights except Vitamin B12 which has too high of a molecular weight unless an enhancer is added. The transdermal route has slower absorption than buccal (oral mucosa) but faster than usual tablet oral route. The down side to transdermal route is possible skin issues due to medication, adhesives, and also different rates of absorption due to skin thickness and condition.
Buccal/sublingual route of absorption is dependent on lipid solubility, oil to water partition coeffincient, saliva pH, small to moderate molecular weight, and oral mucosa thickness. The mechanism of action is osmosis, which means items that readily dissolve in water are easily absorbed. Unlike orally ingested medicates, that take time to absorb and need to be filtered and/or processed in the liver, sublingual route is fast absorbing and the liver is bypassed. The down side to this route is it disrupts eating and drinking and is not efficient with smoking due to vasoconstriction.
An e-mail was sent to the companies inquiring about the outcomes of their products with people with malabsorption issues. No response was received from the spray vitamin companies.A request was also sent to obtain any research articles they may have but a response has not been received at this time. The following is the response I received from the maker of Patch MD.
“I am the president and founder of Patch MD. We design Patch MD to help people that have digestive issues and malabsorption. Our whole premise is to avoid the digestive track, by doing so we avoid dealing with conditions such as short bowel syndrome, acid reflux, and bariatric surgery to name a few. People also with Crohn’s disease and iliac disease are challenged with digestion and absorption every day of their life. Our patches are designed specifically to pass nutrition through the skin into the bloodstream. We get letters every day from people that have had bariatric surgery and were unable to get vitamin D, calcium, the B’s and Vitamin A and K, our product works because we use the skin as our delivery system, absorption is through the skin, avoiding all digestive potential issues. The only problem that we may have is we tell our customers to use no lotions or cream in the patch application area, as you may understand it will prevent absorption. We are going to be at a national convention this weekend in Manhattan Beach California to take part and display our products at the ObesityHelp conference. They ask us to take part as they were getting great reviews from their members that are using the patch. All were improving their blood work after taking Patch MD patches.”
Earl Hailey, President Patch MD
In light of the review of data, it would seem that the transdermal route would be beneficial to people who are having issues maintaining blood levels of fat-soluble vitamin levels. The other vitamins also have a good prospect of absorption via transdermal route. Buccal or sublingual (sprays) would seem to have a better outcome for water-soluble vitamins unless there is an additive added to the product to increase the solubility of the fat-soluble vitamins and make them water miscible. We must realize that there is no data for Duodenal Switch patients and very little data regarding these routes of absorption with vitamins specifically. If you are going to try these types of vitamins you should be extremely diligent in following your laboratory studies for vitamin levels with greater frequency until it is determined they are maintaining your blood levels.
Also, it should be noted that water miscible (dry) Vitamin A, D, E, K are the only type of these vitamins a DS patients should be taking. Over the counter Vitamin A, D, E, K are fat-soluble and due to the fat malabsorption after DS these type of vitamins are not appropriate to maintain blood levels. Water miscible (dry) vitamins should NOT be taken with fatty or oily foods and should also be taken 30 minutes prior or 30 minutes after eating. The water miscibility makes them water soluble and therefore will not have optimal absorption if taken with fat. Fat also increases the rate of digestion through the small bowel after DS and decreases the amount of time the vitamin has in the bowel and therefore, decreases absorption. They are best absorbed when taken on their own.
The good news patches and spray routes of administering medications and supplements is an up and coming area of research. There are several ongoing research studies and new developments on the horizon for increasing absorbability of transdermal route with different types of additives and techniques.
Injectable Vitamin A and Vitamin D
June 20, 2013 11:24 pm
Injectable Vitamin A and Vitamin D can improve vitamin status post weight loss surgery. One of the common side effect of all weight loss surgical procedures is nutritional and/or mineral deficiencies. Patients undergoing weight loss surgical procedures are always instructed to supplement their diet with multivitamin, calcium, iron, vitamin D and other supplements or minerals. If you do not take your supplements regularly you can become deficient. The symptoms associated with vitamin A deficiency is night blindness. Chronic vitamin D deficiency may result in low calcium, osteoporosis and other health-related issues.
Vitamin A and vitamin D, both fat-soluble vitamins, are absorbed by duodenal switch patients only if taken and a dry formulation. An alternative to oral supplement, would be injectable form of these two vitamins. Both of these vitamins can be formulated and purchased from compounding pharmacies that are equipped and experienced with the interpretation of injectable vitamins and minerals. Your primary care WILL need to contact the pharmacy of their choice for the recommendations and be willing to make the injections available to you.
We will gladly be able to provide injectable Vitamin A and Vitamin D for patients whose data laboratory studies are available to us and see us in the office.Please be aware that these are compounded and are not covered by insurance.
We will not be able to provide prescriptions for injectable vitamins to be sent to your primary care or other physicians to provide the injections.
Vitamin D supplement has been discussed previously in my Blog .
The common dosing for the vitamin D is 600,000 IU, deep IM every 6 months till the levels are normalized. The patient then can take the oral supplements only.
Vitamin A supplements was also discussed in my Blog.
The common dosing for the vitamin D is 100,000 IU, deep IM every 2-6 months till the levels are normalized. The patient then can take the oral supplements only.
Vitamin A supplements was also discussed in my Blog.
The common dosing for injectable vitamin A is 50,000 IU, deep IM every 6 months till the blood levels are corrected, and the patient symptoms are resolved.
Just as a reminder, we have no financial interest in any of the vendors that are recommended on our website. Also, note that this is not in any form or fashion a substitute for an evaluation by your primary care physician or your surgeon. This is for information only, and is not to be taken as a recommendation for any particular patients’ condition.