Category: malnutrition
Covid 19:Anesthesia, Weight Loss Surgery and Malnutrition
October 30, 2021 8:52 am
As the COVID-19 pandemic is charting its course into 2022, as health care providers, we have had to adapt and adjust to the transient and shifting environment. Testing for COVID-19 has been in place, and is now part of the standard for preoperative work-up. In addition, covid testing will likely be part of screening any surgical procedure for the foreseeable future.
The challenge of pandemic control is the large pockets of populations in the US and worldwide that do not have protection against the virus and are not vaccinated. Vaccination provides the only proven long-term protection against COVID-19 infection and its long-term persistent health effect. In addition, the complication rate reported in scientific journals is negligible compared to the complication and death rate from the COVID-19 infection.
There are implications of covid infection and general anesthesia published in peer-reviewed journals. The increased risk of general anesthesia after covid infection is related to the severity of the initial infection and the extent of the treatment required, and the persistence of the post covid symptoms, including shortness of breath, fatigue, and laboratory finding elevated inflammatory markers. Long after resolution of the acute COVID-19 symptoms, the most common persistent complaints are fatigue, shortness of breath, Joint and chest pain; and all these increase the risk of post-operative complications (Carfì et al., 2020)
The required delay for surgery may be as short as 2-4 weeks to as long as six months or longer if the persistent symptoms are present. Surgery may not be avoidable in a critical life-threatening situation and may be necessary even with a much-increased risk of complication (Collaborative, 2020). Recovery post-COVID-19 may not be complete with the resolution of the initial symptoms (Dexter et al., 2020)
Recent publications and scientific presentations have also shown the protection that weight loss surgery and maintained weight loss provide in those who come down with the COVID-19 infection (Aminian et al., 2021). However, the rate of weight gain, lack of weight loss is worse for weight loss surgical patients post COVID-19 disorder (Bullard et al., 2021; Conceição et al., 2021). Furthermore, patients with COVID-19 infection post weight loss are at a higher risk of malnutrition (di Filippo et al., 2021; Kikutani et al., 2021). Up to 40% of patients have malnutrition if hospitalized with COVID (Anker et al., 2021).
To summarize, Weight loss and weight loss surgery reduce the severity of the initial COVID-19 infection. However, it increases malnutrition risk, requiring nutritional support and surgical interventions in non-responsive cases.
REFERENCES:
Aminian, A., Fathalizadeh, A., Tu, C., Butsch, W. S., Pantalone, K. M., Griebeler, M. L., Kashyap, S. R., Rosenthal, R. J., Burguera, B., & Nissen, S. E. (2021). Association of prior metabolic and bariatric surgery with severity of coronavirus disease 2019 (COVID-19) in patients with obesity. Surgery for Obesity and Related Diseases, 17(1). https://doi.org/10.1016/j.soard.2020.10.026
Bullard, T., Medcalf, A., Rethorst, C., & Foster, G. D. (2021). Impact of the COVID-19 pandemic on initial weight loss in a digital weight management program: A natural experiment. Obesity, 29(9). https://doi.org/10.1002/oby.23233
Conceição, E., de Lourdes, M., Ramalho, S., Félix, S., Pinto-Bastos, A., & Vaz, A. R. (2021). Eating behaviors and weight outcomes in bariatric surgery patients amidst COVID-19. Surgery for Obesity and Related Diseases, 17(6).
Di Filippo, L., De Lorenzo, R., D’Amico, M., Sofia, V., Roveri, L., Mele, R., Saibene, A., Rovere-Querini, P., & Conte, C. (2021). COVID-19 is associated with clinically significant weight loss and risk of malnutrition, independent of hospitalisation: A post-hoc analysis of a prospective cohort study. Clinical Nutrition, 40(4). https://doi.org/10.1016/j.clnu.2020.10.043
Kikutani, T., Ichikawa, Y., Kitazume, E., Mizukoshi, A., Tohara, T., Takahashi, N., Tamura, F., Matsutani, M., Onishi, J., & Makino, E. (2021). COVID-19 infection-related weight loss decreases eating/swallowing function in schizophrenic patients. Nutrients, 13(4). https://doi.org/10.3390/nu13041113
Over the Counter Vitmain D3 better than the Prescription Vitamin D2
August 30, 2021 10:41 am

Vitamin A and Wound healing
December 21, 2020 9:37 am
Night Blindness – Vitamin A Deficiency
Nyctalopia (Night Blindness) An Early Sign of Vitamin A Deficiency with VideoA recent article discusses the types and function of vitamin A. As with the pandemic of COVID-19 continuous to stress our body and mind, we must stay vigilant with our nutritional status. Therefore, Vitamin supplements are critical in maintaining a robust immune system. For some, oral supplements are adequate; others may require injectable forms. If the oral supplements do not correct the vitamin A levels, please contact your primary care or our office to available vitamin A injections.
Fat Soluble Vitamins
April 26, 2020 10:20 am
Written By: Maria Vardapetyan, Eric Baghdasaryan, Osheen Abnous
Vitamins are chemicals that facilitate many processes in the human body such as blood clot formation, good vision, fight infections etc. There are two classes of vitamins. Water soluble vitamins and fat soluble vitamins. Water soluble vitamins dissolve in water. This makes it possible for them to be absorbed through all mucous membranes. Fat soluble vitamins on the other hand do not dissolve or pass through mucous membranes. Fat-soluble vitamins are absorbed in the intestine along with fats in the diet. These vitamins have the ability to be stored in the fat tissues of the human body. Water-soluble vitamins are not stored in the body and have to be taken in daily with the food and dietary supplements. Solubility of a vitamin is not a function of its physical state. There are fat soluble vitamins that have a liquid form and almost all of the water soluble vitamins come in form of pills or powders.
In this article, we are going to focus on fat soluble vitamins. They are all complex molecules made of carbon, hydrogen, and oxygen in different arrangements (see figures 1, 2, 3 and 4). These fat soluble vitamins are vitamin A, D, E and K.
Vitamin A
Vitamin A has a major role in vision, immune function, cell growth, and maintenance of organs such as heart, kidneys, lungs, etc. It plays a pivotal role in the health of our eyes, specifically the retina1. Rhodopsin protein, a major protein that has the leading role in the process of vision, is found in the retina where it allows us to perceive light. This protein requires vitamin A to function properly. Without vitamin A, rhodopsin cannot sense light and thus cannot initiate the process by which vision occurs.
Figure 1: Chemical structure of Vitamin A molecule
Vitamin D
Vitamin D regulates different chemical reactions that are associated with bones, muscles, and the immune system. The simplified way it does this regulation is it helps absorb calcium from dietary nutrients which in turn strengthens the bones, helps neurons exchange signals to move muscles and helps the immune system to fight against viruses and bacteria2.
Figure 2: Chemical structure of Vitamin D molecule
Vitamin E
Vitamin E acts as an antioxidant. Antioxidants are naturally occurring chemicals that neutralize toxic byproducts of many chemical reactions in the human body. When food is consumed and digested, the human body converts it into energy. As a result of metabolism free radicals (toxic byproducts) are formed and are neutralized with the help of vitamin E. In addition, free radicals are also in the environment. Furthermore, vitamin E stimulates the immune system to fight against bacteria and viruses3.
Figure 3: Chemical structure of Vitamin E molecule
Vitamin K
Vitamin K can be obtained from food and dietary supplements. There are two forms of vitamin K: phylloquinone (Vitamin K1), which is found in spinach, kale and other greens and menaquinone-4 (Vitamin K2), which is found in animal products. Vitamin K1 is involved in blood clotting, and Vitamin K2 is involved in bone tissue building. Vitamin K1 is the main Vitamin K in human diet (75-90% of all vitamin K consumed), however, it is poorly absorbed in the body4,5.
Figure 4: Chemical structures of Vitamin K1 and K2 molecules
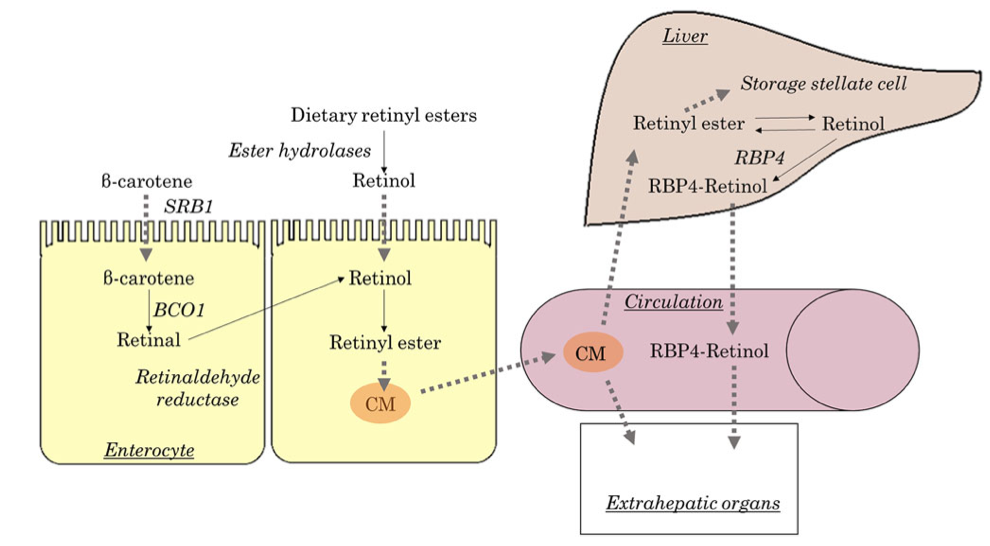
Absorption of fat soluble vitamins
Polarity describes the inherent charge(positive or negative) or lack of charge for any given substance or molecule. Molecules that are charged are referred to as “polar”, while those that lack charge are “nonpolar”. When discussing solubility, it is important to remember the phrase “like dissolves like”. That means polar (charged) substances like to interact with a polar environment like water, since water contains a slight negative charge. Hence, charged substances are water-soluble. Nonpolar substances on the other hand readily interact with nonpolar environments such as fat, which contains no charge. Therefore, molecules that lack a charge such as vitamins A, D, E, and K are referred to as fat soluble.
Due to their water fearing nature, these fat soluble vitamins cannot simply be absorbed directly into the bloodstream (which is mostly water) like the sugars and amino acids in our diet. As their name suggests, these fat soluble vitamins like to be embedded in fatty droplets, which facilitate their absorption in the following way. Fat soluble vitamins group together with other fat molecules to form fatty droplets, effectively reducing the amount of interaction with the watery environment of the intestines. Therefore, without an adequate amount of fat in your diet, your body is unable to effectively absorb these fat-soluble vitamins. This may be true in an intact anatomy, however, post weight loss surgical patients can not increase their fat soluble vitamin levels by increasing their fat intake. This is due to the fact that a high fat diet causes excessive bowel movement which in turn washes away any vitamins taken by mouth. DS limits fat absorption (thus the great weight loss) which can cause vitamin A and D deficiency that can not be easily corrected with oral supplementation.
As mentioned before, fat soluble vitamins are hydrophobic and nonpolar, which means they are also fat loving or lipophilic. Excess fat soluble vitamins can be stored in the liver and fat tissue. Therefore, these vitamins do not need to be eaten every single day since stores of these vitamins can sustain a person for some time. It may take several weeks or months for our body to deplete these stores of fat soluble vitamins which is why it generally takes a longer amount of time for fat soluble vitamin deficiencies to manifest themselves. The ability to store these fat soluble vitamins in tissues can also lead to vitamin toxicity – marked by an excess of vitamin stores in our body.
Clinical manifestations of A, D, E, K deficiency
| Vitamin | Clinical Deficiency manifestations |
| Vitamin A | Vision Problems
Dryness of the eye |
| Vitamin D | Softening and weakening of the bones
Bone shape distortion Bowed legs (generally in children) Hypocalcemia |
| Vitamin E | Damage to red blood cells
Tissue/organ damage due to inability to supply enough blood Vision problems Nervous tissue malfunction |
| Vitamin K1 | Excessive bruising
Increased bleeding time Small blood clots under nails Increased bleeding in mucous membrane |
| Vitamin K2 | Weak bones
Increased plaque deposits along gumline Arterial calcification |
References
- Office of Dietary Supplements – Vitamin A. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminA-HealthProfessional/#. Accessed April 26, 2020.
- Office of Dietary Supplements – Vitamin D. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminD-Consumer/. Accessed April 26, 2020.
- Office of Dietary Supplements – Vitamin E. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminE-Consumer/. Accessed April 26, 2020.
- Vitamin K. The Nutrition Source. https://www.hsph.harvard.edu/nutritionsource/vitamin-k/. Published July 2, 2019. Accessed April 26, 2020.
- Beulens JWJ, Booth SL, van den Heuvel EGHM, Stoecklin E, Baka A, Vermeer C. The role of menaquinones (vitamin K₂) in human health. The British journal of nutrition. https://www.ncbi.nlm.nih.gov/pubmed/23590754. Published October 2013. Accessed April 26, 2020.
Copper Deficiency Intravenous SupplementationExclusive Member Content
November 17, 2019 9:23 pm
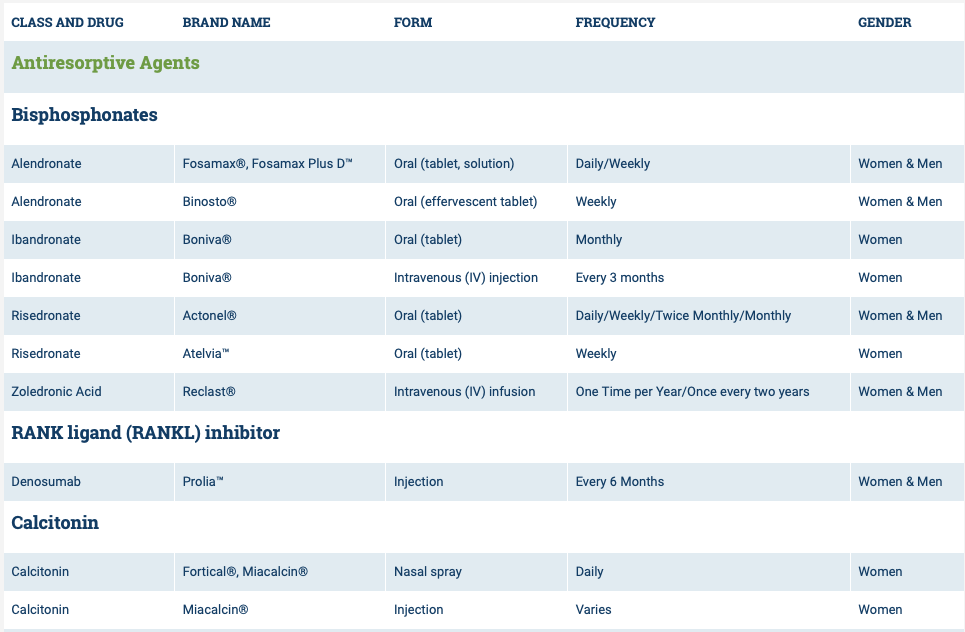
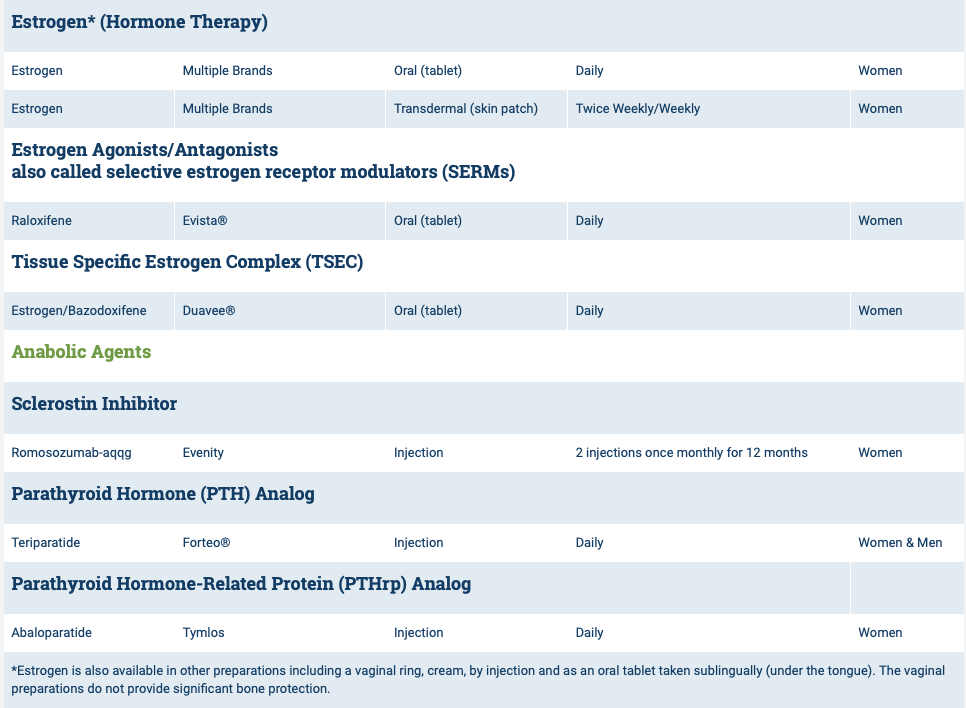
Osteoporosis Medications, Action and Side Effects
May 25, 2019 3:40 pm
Treatment options should be approached is a global and systemic fashion. It is critical that the nutritional status is at its best possible and optimized for important healthy bone vitamins and minerals. Low protein needs to be corrected. Special attention should be given to nutrients, minerals and vitamins. These include Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1/K2to name a few.
Healthy bones require ongoing and routine force in the form of exercise to remain health. Just as exercise improves muscle strength, it also improves bone health. Exercise is also critical in improving bone structure and density. Ideally, exercise should be weight bearing and resistance. Examples include: hiking, walking, jogging, climbing stairs, playing tennis, and dancing. Resistance type exercise is weight lifting and resistance bands. These exercise work by creating a pull or force on the bone either by gravity, movement or weight. Always check with your physician before beginning an exercise routine, start slowly and building up to longer periods of time. The ideal goal would be at least 30 minutes a day, every day, if you are able.
We frequently see patients immediately started on osteoporosis medications without checking or improving some of the nutritional markers noted above or without looking at exercise history. In some case, the medication recommended are contraindicated due to nutritional status.
The medications can be grouped in to those that help with new bone formation (Anabolic agents) or those that help by suppressing the bone breakdown phase (Antiresorptive agents).
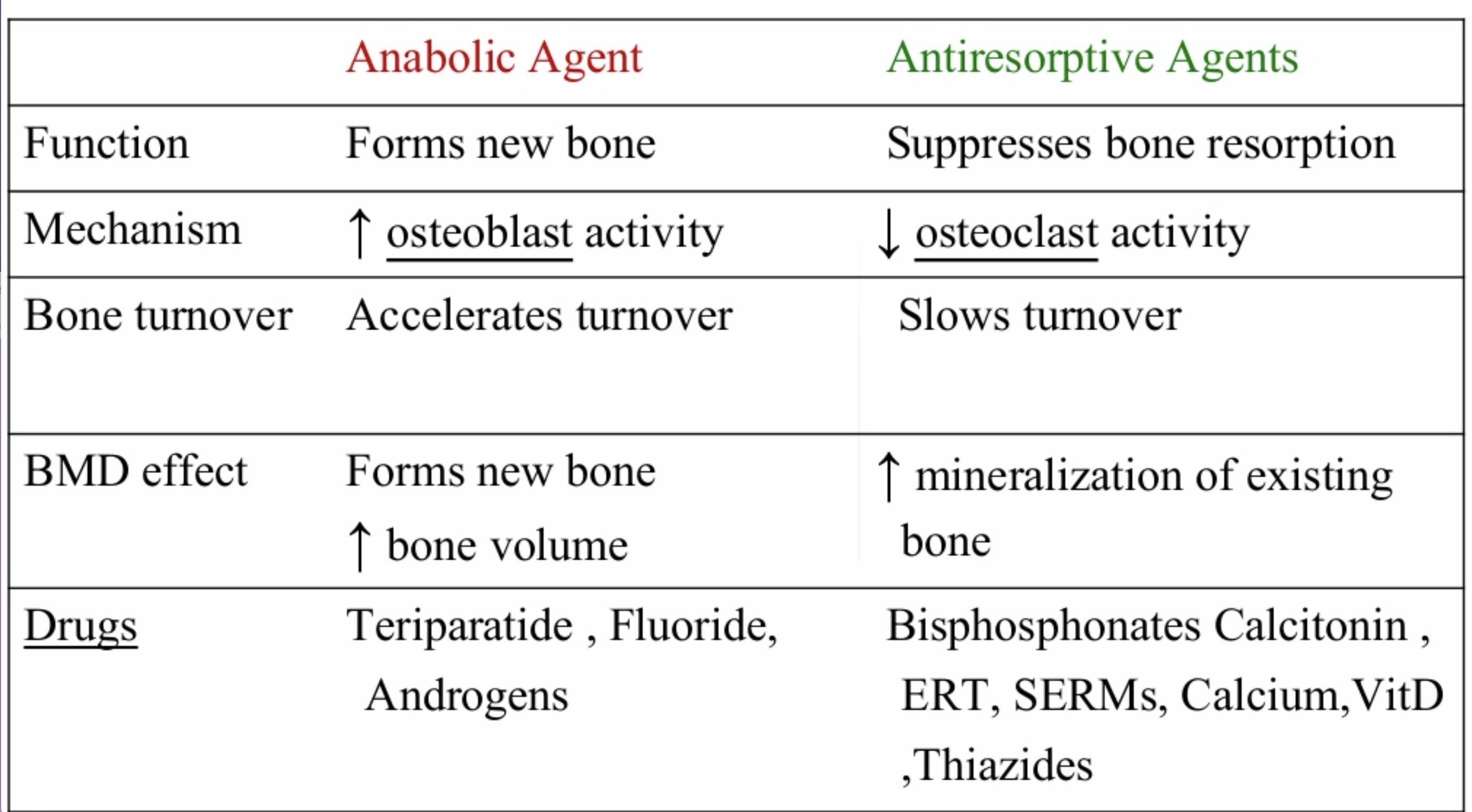
National Osteoporosis Foundation has an exhaustive list (below) of medications for treatment of Osteoporosis.
The table below outlines the side effects and mechanism of the actions of the common medications used for treatment of osteoporosis which was published by the University Health News Publication on August of 2014.
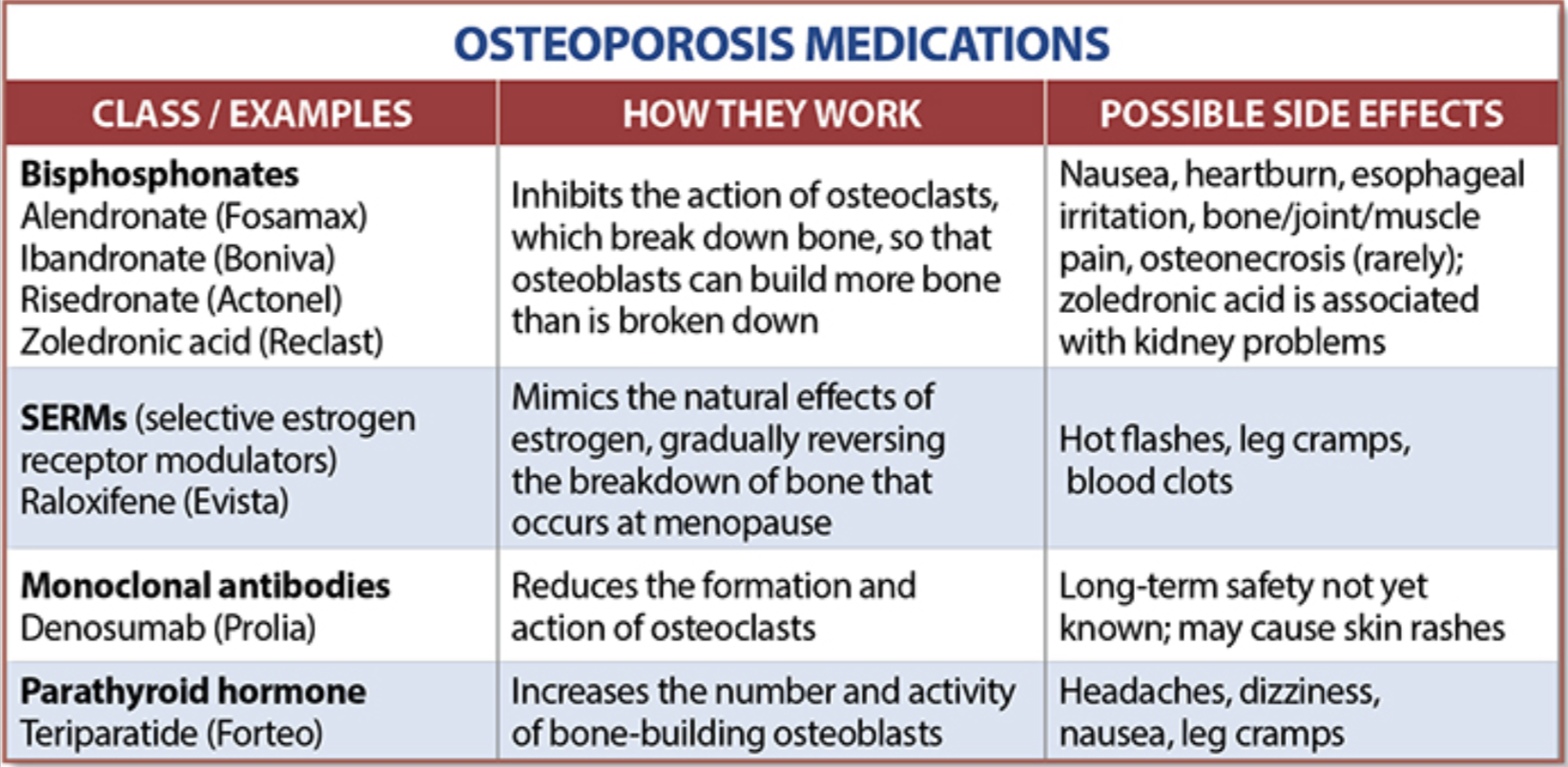
With all this information, the few points to remember is that the most important factors in healthy bone structure are the nutritional status Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1 levels.
This is an animation of normal bone Metabolism. It shows how bone structures is taken down and rebuilt continuously. This allows for a healthy bone maintainence as we age. The key is the balance of breakdown (osteoclast) and the build up (osteoblast) activity is regulated. Osteoporosis develops when there is more breakdown that build up. 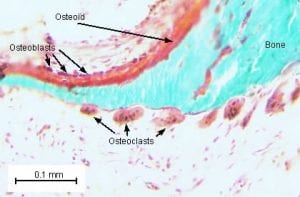
With permission of Dr. Susan Ott of University of Washington.
Additional information available on her site.
Past blogs on Bone Health.
Dual Testimonial: Cameron’s Gastroparesis surgery & Scott’s Revision of a Duodenal Switch
February 01, 2016 8:04 am
In 2015, I came into contact with the most unique, passionate, urgently responsive; talented beyond belief and caring surgeon I have ever met. Our oldest son who is a 21-year-old cancer survivor, has had nearly five years of medical nightmare as diagnosed with severe gastroparesis resultant from his vagal nerve being severed during a previous Nissen Fundoplication surgery. We didn’t find out that this had happened until nearly two years later and only after a 4 hour gastric emptying test showed that Cameron’s stomach was only about 30% emptied after four hours (should be empty after an hour) due to gastroparesis.
I had heard about Dr. Keshishian on a Bariatric support group page on which I post and get great advice. The surgeon back in Central, IL where we live told us that Cameron needed a subtotal gastrectomy to remove 80% of his stomach! This sounded radical and no way in the world was that going to happen. I was given Dr. Keshishian’s email address so I could consult with him for his advice. It was a Saturday morning around 7 AM Central time when I sent off an email to Dr. Keshishian detailing Cameron’s medical history and current issues. I was in hoping that his office would get the email on Monday and hopefully get back to me within a week. I went out to my kitchen to get a cup of coffee and when I returned I had a missed call with a California area code. Yep, it was Dr. Keshishian. I called back and we talked for 45 minutes. He suggested several things and told me that any good general surgeon in my area could do surgery on Cameron and fix him, well that was the only time he was wrong. We couldn’t find anyone in our area who would do the surgery.
So we talked and agreed that Cameron needed a Roux-en Y drain put in place to physically drain his stomach by way of gravity (not for any weight loss as very little small bowel was bypassed). Dr. Keshishian got us in the next week and we flew out to Glendale where he met with Cameron for an examination on that Monday. On Tuesday, Dr. Keshishian performed surgery to fix Cameron’s herniated diaphragm, loose Nissen wrap, performed the Roux-n Y limb and anastomosis to the stomach. Dr. Keshishian also found a Meckel’s diverticulum (a congenital small bowel defect that can cause internal bleeding and serious issues). The following Sunday, Cameron developed severe pain due to chronic pain from his Cancer treatment and 12 subsequent surgeries, many on his abdomen. Dr. Keshishian saw Cameron in the ER and spent 3 hours fixing Cameron’s pain issue and making sure he was medically sound so we could fly home the next day.
Today, Cameron has very little to no issues which you wouldn’t have believed possible six months earlier. In the past, he had violent retching, dry heaving and bad nausea daily which had him severely incapacitated and very depressed due to a feeling of hopelessness and pain from the Gastroparesis. He didn’t believe he had a chance at a normal life but Dr. Keshishian gave Cameron his life back. We are eternally grateful for your huge heart and talent Dr. Keshishian. Thank you!
During our time in Glendale in 2015 for Cameron’s surgery Dr. Keshishian and I began discussing my situation. I had been given a virgin Duodenal Switch performed by a surgeon in Illinois in September of 2013. A year later in 2014 and 180 lbs lighter, I ended up in the hospital as I was passing out. I had a resting heart rate of 35 BPM, a blood pressure in the 75/40 range and incredibly bad labs including anemia, low copper, low zinc, and dangerously low albumin and total protein. A full cardiac work up was completed and I spent a week in intermediate care. Why? I was extremely malnourished even though I was consuming 200-250 grams of protein daily! Why was I malnourished? Because my original surgeon performed a “cookie cutter DS” on me where he didn’t measure my small bowel and arbitrarily gave this 6’2 man a 100 cm common channel and a 150 cm Alimentary limb. Way too short on the AL! Had the Hess method been followed (the only way the DS should be allowed to be completed) my CC would have been 100 cm (that was okay) but my Alimentary channel should have been 275 cm! Simply put, my absorbing portion of small bowel was 34% and the Biliopancreatic limb (non-absorbing) was 66%. It should have been a 50/50 ratio with 100 cm CC, 275 cm AL and a 375 cm BPL. In order to combat my severe malnutrition that September of 2014 I went on a pancreatic enzyme (CREON) to assist my nutrient absorption. I was taking with meals right around 400,000 IU’s of CREON (a boat load) and this was barely keeping my nutrients in range and lab values barely in range. After speaking with Dr. Keshishian, he recommended that I give it until around September of 2015 to see if my absorption increased enough to where a revision wouldn’t be required. Towards the end of July, I all of the sudden lost nearly 20 pounds in two weeks from my already frail and scrawny body. I saw my surgeon in Peoria as I was very alarmed; and I had been having bad cramping and other issues point to a possible bowel obstruction His exact words to me were “see me in 30 days, you are like the DS poster boy of good nutrition”. As you can imagine I found that completely unacceptable and soon as I was out of that appointment I emailed Dr. Keshishian. He told me that if I couldn’t get a revision ASAP I would need to immediately go on TPN. Two weeks later my wife and I landed at LAX and were in Glendale on Monday morning for an exam with Dr. Keshishian.
The job Dr. Keshishian did describing what he was going to do, and of course this was a visual presentation with Dr. Keshishian drawing (you know Dr K’s love of drawing) out for us what he was going to do. He thoroughly explained for my wife and I so she was comfortable with what was going to happen and we fully understood what he was going to do. Doc also found an umbilical hernia that he was going to repair and I had an anal fissure as well that wouldn’t heal so we discussed what he would do to examine and possibly fix during my revision surgery. The next day Dr. Keshishian performed surgery where he fixed the umbilical hernia, measured my total small bowel length to determine appropriate channel lengths and found an repaired a huge mesenteric defect (intestinal hernia and Dr K has a picture of my guts with the huge hole in the mesentery that he has posted on his blog discussing intestinal hernias and blockages), fixed my fissure (Thank you!) and put in a side by side anastomosis that effectively lengthened my AL by 125 cm and my CC by 25 cm worth of absorption. This put my absorbing intestine to BPL ratio where it should have been in the first place (50/50 ratio).
I am pleased to say that I immediately went off the CREON and my absorption and subsequently my lab values improved tremendously. At surgery on August 18, 2015 I weighed a whopping 170 lbs. Today I am weighing in at 183 pounds and well on my way to Dr. Keshishian’s suggested optimal weight target of 205.
Dr. Keshishian is absolutely amazing and the best in the world when it comes to performing the Duodenal Switch and revision to DS Surgery (Band to DS, RnY to DS, Channel extending revision to DS). I would recommend Dr. Keshishian to any patient who needs a virgin Duodenal Switch to get their health back and especially to those who were sold a garbage RnY or Crapband procedure that ultimately failed you (it failed you, you did not fail). In fact, I am trying very hard to convince my brother and Step Mother to fly to Glendale and have Dr. Keshishian perform a Duodenal Switch on them. They very much need it for their health and Dr. Keshishian is the best in the world having performed over 2,000 DS procedures.
I don’t say this lightly. Ara, you are one of the finest human beings I have ever had the good fortune of knowing and your surgical skills are second to none. I really do admire and love this gentleman like a brother and consider him to be a friend. Thank you for using your incredible skill to fix my health issues resultant from the failed cookie cutter Duodenal Switch I was given two years earlier by another surgeon. Had I met you back then and knew what I know now, you would have performed my virgin DS and I would not have suffered for two plus years. Thank you from the bottom of my heart, Dr. K!
Bowel Length in Duodenal Switch
November 09, 2015 6:25 am
Malnutrition is one of the most feared complication of the duodenal switch operation. It may present years after surgery. What is common is a mix of nutritional deficiencies which include fat soluble vitamins, and protein calorie malnutrition. These all point to possible excessive shortening of the common channel. In my practice we have seen patients that have had lengthening of their common channel to improve their metabolic picture. What is very obvious to us, is that we see disproportionately higher number of cases coming to us for revision from practices where the common and alimentary lengths are done as a “standard” numbers with no specific adjustments made for the patient, their anatomy and situation. I have said for years, that the length of the bowel that is measured to be become the common and the alimentary limb should be a percentage of the total length of small bowel, rather than a pre-determined measurement. Here is a visual description of how this works.
If a common channel and the alimentary limb is measured to be a percent of the total length then the chance of protein calorie malnutrition is minimized since this will take into account the bowels absorptive capacity which is being reduced. This decrease in the absorption is done as a fraction of the total length.
Raines et al. published a study in 2014, that showed how small bowel length is related more closely to a patient’s height and not weight. And yet, some surgeons totally based the length of the common channel and the alimentary limb arbitrarily based on the patient pre operative BMI and nothing else. Could this be the cause of why I see some patients coming to us for revision of their duodenal switch for malnutrition?
Iron Deficiency & Anemia July 15, 2015 Webinar RecordingExclusive Member Content
July 16, 2015 1:52 pm
Zinc InformationExclusive Member Content
April 17, 2015 7:22 am