Category: osteocalcin
Osteoporosis Medications
March 28, 2020 7:22 pm
There are a number of lectures, posting that we have done over the years on this topic. However the questions of osteoporosis medications and their benefits and risks comes up often.
The links are attached:
Here is an updated list of medication that I had previously published. I made some clarification to explain how the medications work. There are different classes of medications and the detail of the action and soda effects were described earlier at a blog post.
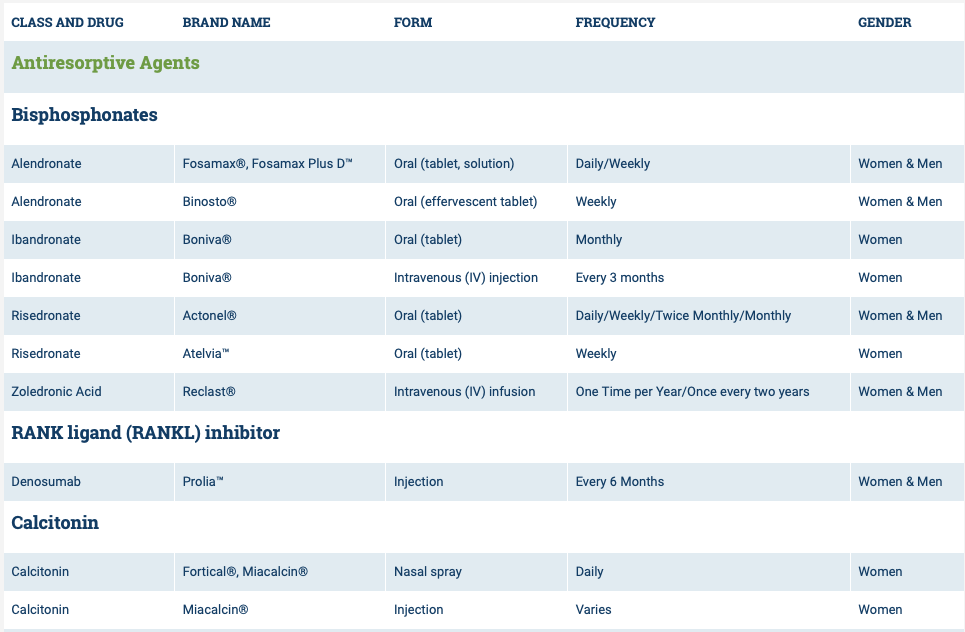
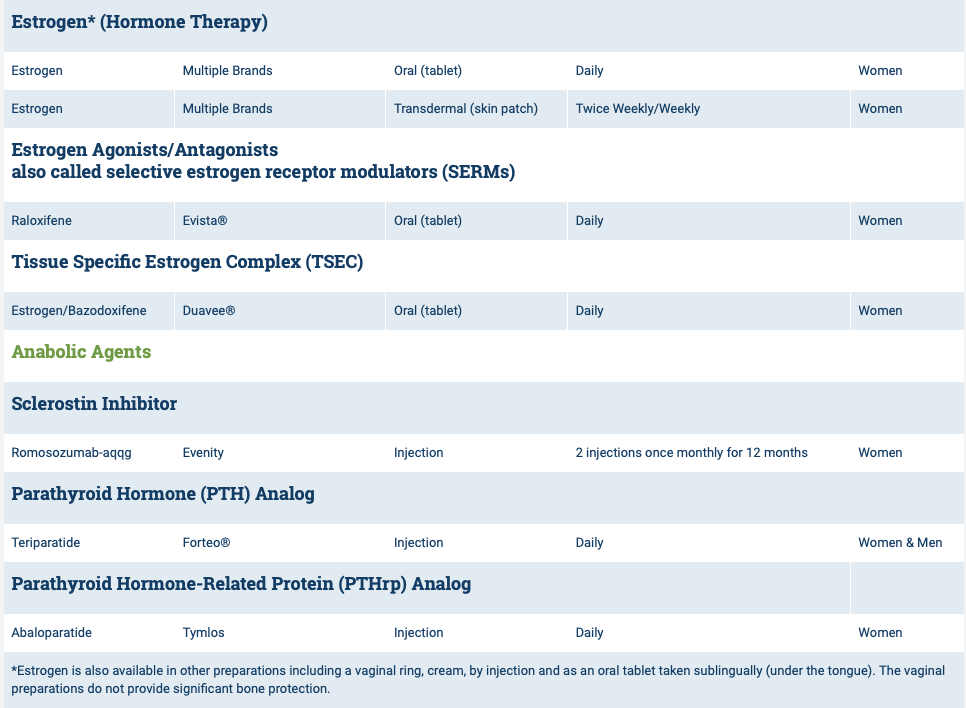
List of medications that effect bone health.
The table is obtained from https://www.nof.org site.
Osteoporosis Medications, Action and Side Effects
May 25, 2019 3:40 pm
Treatment options should be approached is a global and systemic fashion. It is critical that the nutritional status is at its best possible and optimized for important healthy bone vitamins and minerals. Low protein needs to be corrected. Special attention should be given to nutrients, minerals and vitamins. These include Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1/K2to name a few.
Healthy bones require ongoing and routine force in the form of exercise to remain health. Just as exercise improves muscle strength, it also improves bone health. Exercise is also critical in improving bone structure and density. Ideally, exercise should be weight bearing and resistance. Examples include: hiking, walking, jogging, climbing stairs, playing tennis, and dancing. Resistance type exercise is weight lifting and resistance bands. These exercise work by creating a pull or force on the bone either by gravity, movement or weight. Always check with your physician before beginning an exercise routine, start slowly and building up to longer periods of time. The ideal goal would be at least 30 minutes a day, every day, if you are able.
We frequently see patients immediately started on osteoporosis medications without checking or improving some of the nutritional markers noted above or without looking at exercise history. In some case, the medication recommended are contraindicated due to nutritional status.
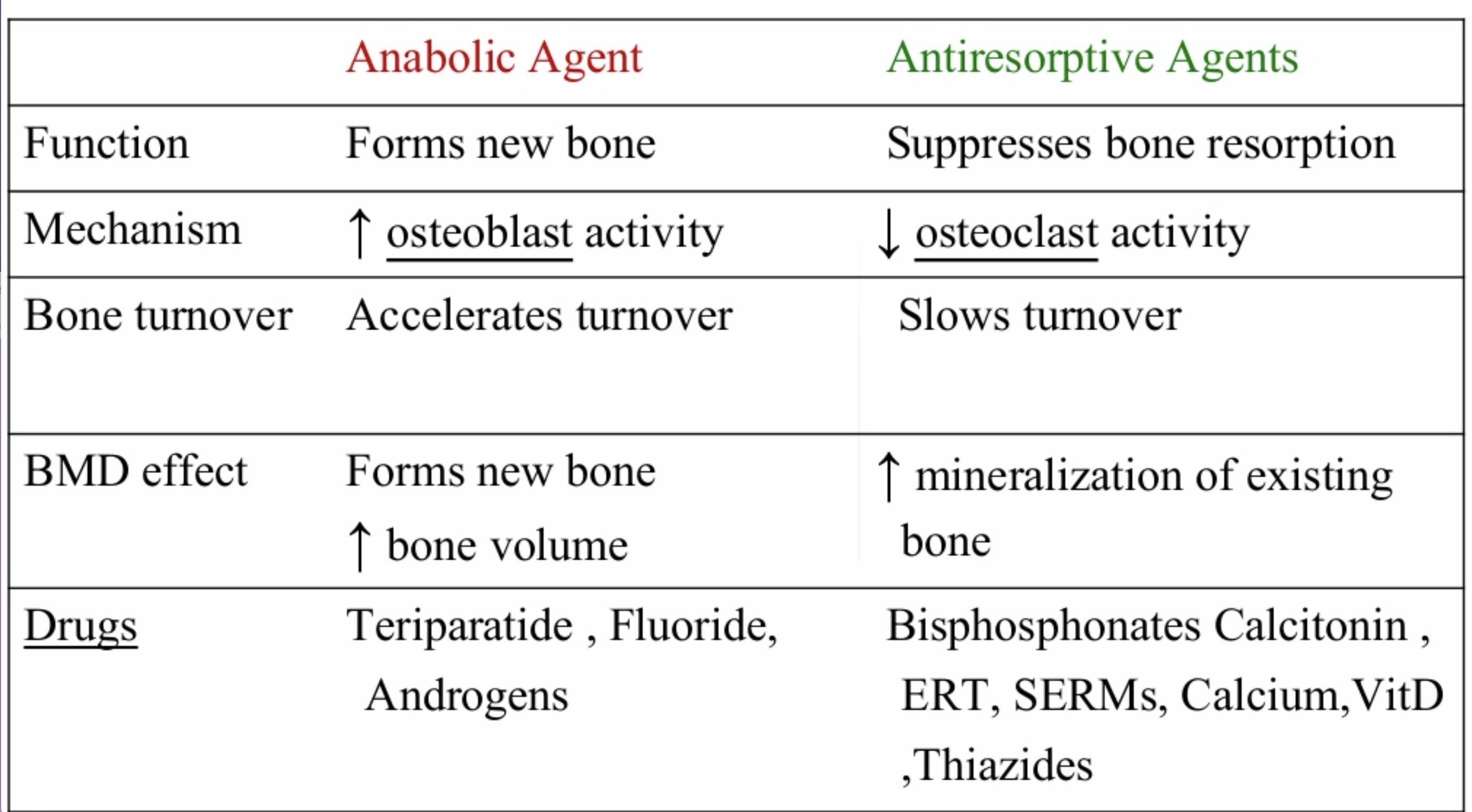
The medications can be grouped in to those that help with new bone formation (Anabolic agents) or those that help by suppressing the bone breakdown phase (Antiresorptive agents).
National Osteoporosis Foundation has an exhaustive list (below) of medications for treatment of Osteoporosis.
The table below outlines the side effects and mechanism of the actions of the common medications used for treatment of osteoporosis which was published by the University Health News Publication on August of 2014.
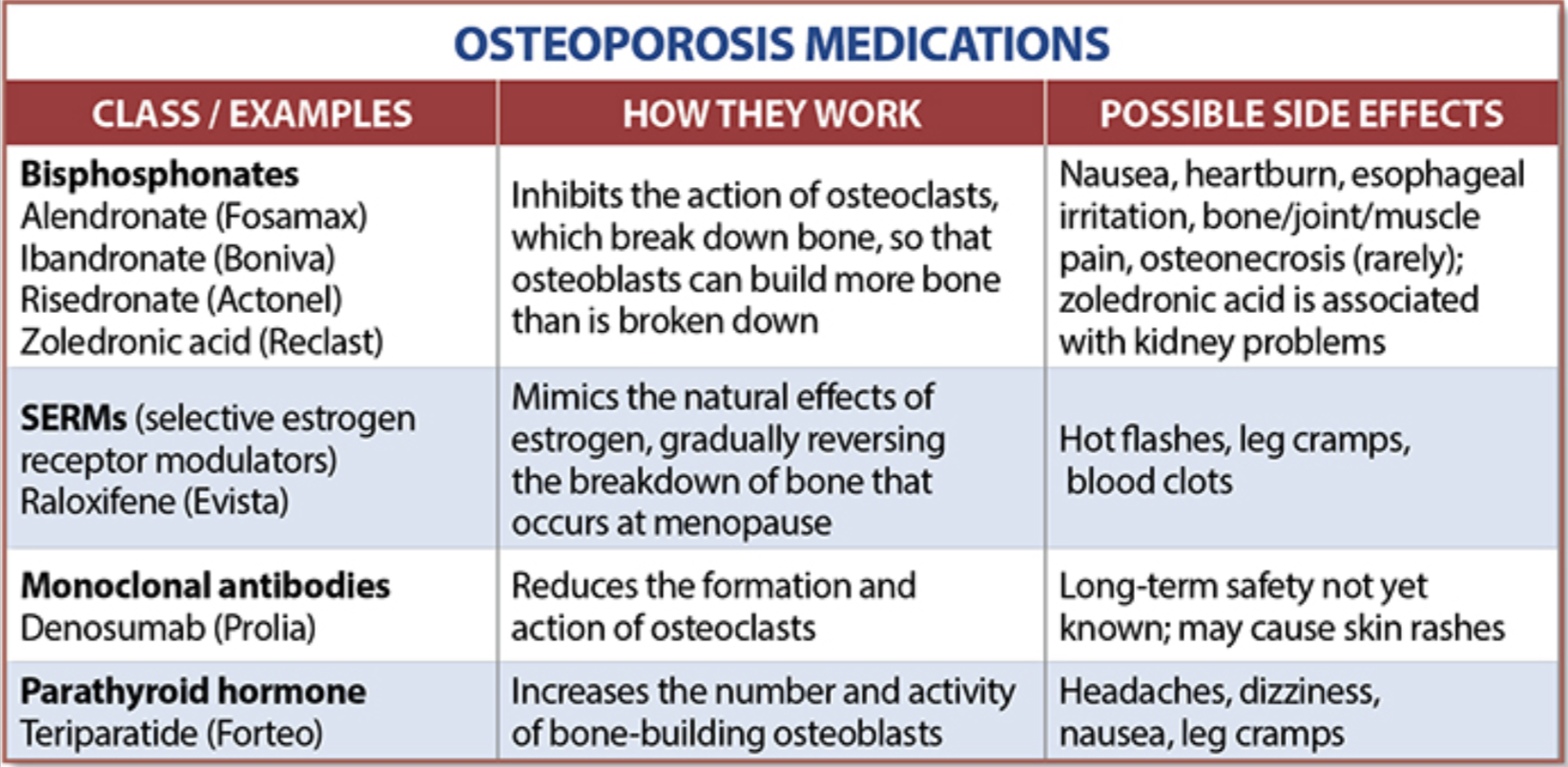
With all this information, the few points to remember is that the most important factors in healthy bone structure are the nutritional status Protein, Calcium, Magnesium, Vitamin D, and Vitamin K1 levels.
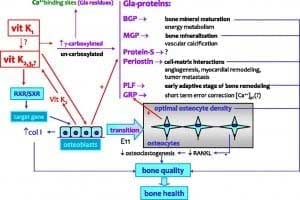
This is an animation of normal bone Metabolism. It shows how bone structures is taken down and rebuilt continuously. This allows for a healthy bone maintainence as we age. The key is the balance of breakdown (osteoclast) and the build up (osteoblast) activity is regulated. Osteoporosis develops when there is more breakdown that build up. 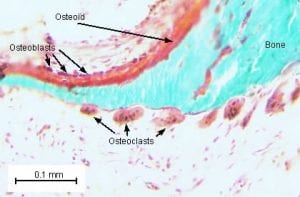
With permission of Dr. Susan Ott of University of Washington.
Additional information available on her site.
Past blogs on Bone Health.
Vitamin K1
April 08, 2015 7:16 pm
Vitamin K1 is a found in dark green leafy vegetables, asparagus, brussels sprouts, some grains, olive oil, prunes, soy bean oil, and canola oil. The body has limited storage capacity for Vitamin K and uses a recycle system to reuse it.
Vitamin K1 is a fat-soluble vitamin that after Duodenal Switch is not as easily absorbed due to the limiting contact of the food product with the bile until the common channel. Bile is needed to absorb fatty acids and fat-soluble vitamins.
Duodenal Switch patients in need of Vitamin K1 supplements should take “Dry” or water miscible type of Vitamin K1, such as Biotech brand. The patients laboratory studies will determine if a patient requires Vitamin K1 supplement. Duodenal Switch patients should have laboratory studies drawn and evaluated at least on a yearly basis. Vitamin K works in a delicate balance with other supplements and should be monitored by a physician, in at risk people.
Vitamin K1 is most know for it’s coagulation effect and the clotting cascade. Vitamin K1 works with calcium and proteins in order to accomplish coagulation synethesis. Care should be taken with Vitamin K supplementation and anti-coagulation (blood thinners) therapy. Please see your physician regarding any supplementation of Vitamin K and blood thinner medications.
A discovery of Vitamin K dependent proteins has led to research on Vitamin K1 in bone health. Bone matrix proteins, specifically osteocalcin, undergo gamma carboxylation with calcium much the way coagulation factors do; this process also requires Vitamin K. Osteocalcin is a Gla-protein that is regulated by Vitamin D. The calcium binding ability of osteocalcin requires several Vitamin K carboxylations to exert it’s effects on bone mineralization.
In adults, the causes of Vitamin K1 deficiency include the following :
Chronic illness
Malnutrition
Alcoholism
Multiple abdominal surgeries
Long-term parenteral nutrition
Malabsorption
Cholestatic disease
Parenchymal liver disease
Cystic fibrosis
Inflammatory bowel disease
Medications: Antibiotics (cephalosporin), cholestyramines, warfarin, salicylates, anticonvulsants, Cefamandole, cefoperazone, salicylates, hydantoins, rifampin, isoniazid, barbiturates, and certain sulfa drugs, higher Vitamin E can antagonized Vitamin K)
Massive transfusion
Disseminated intravascular coagulation (DIC) – Severe
Chronic kidney disease/hemodialysis
Additional information: https://lpi.oregonstate.edu/infocenter/vitamins/vitaminK/
Intake of Vitamin K1 and K2 and bone fracture risk
As always, discuss with your physicians and/or surgeon any changes in medications and supplements. This is not meant to be an all inclusive discussion of Vitamin K.
- Weight loss Medications compared to surgery February 20, 2024
- SIPS-SADI and ASMBS December 31, 2023
- Survey December 16, 2023
- Long Term Outcome Survey December 1, 2023
- Weight Loss Injection May 10, 2023