Tag: Duodenal Switch
2015 ASMBS Summary
November 11, 2015 7:31 am
The 2015 ASMBS meeting was held November 2-6, 2015. It was combined with TOS (The Obesity Society) and had more than 5,600 attendees from all over the world in every aspect of obesity treatment. There were some interesting additions and deletions from this meeting compared to the past.
The one sentence that comes to my mind is “I told you so”.
One important addition was a DS course for Surgeons and Allied Health. This was very exciting, except the content and questions seemed to gravitate to SADI/SIPS/Loop rather than DS. Dr. Cottam was one of the moderators of the course. It seems that they have found the value in preserving the pyloric valve. It was clear that the discussion was driven by the need to come legitimize the single anastomosis procedures at this early stage with almost no data to prove long term outcome. With many of the Vertical Sleeve Gastrectomies having re-gain and the they are looking for a surgery that the “masses” can perform. This was actually the term used by one of the presenters, implying that the duodenal switch needed to be simplified so that all surgeons, those who have pushed all other procedures can not offer Duodenal Switch to their patients with less than desirable outcome. Several surgeons also voiced their concern and dissatisfaction with the issues and complication of the RNY and want an alternative. There was much discussion regarding SADI/SIPS/Loop being investigational and that it shouldn’t be as it is a Sleeve Gastrectomy with a Billroth II. Dr. Roslin and Dr. Cottam discussed their SIPS nomenclature saying they wanted to stay away from something that had Ileostomy, suggesting bowel issues, or the word “SAD”i due to negative connotations. The point to be made is that the SADI and SIPS and the loop are all the same. I have also noticed other surgeons using SADS (Single Anastomosis Duodenal Switch). There is a great deal of industry behind these procedures and many surgeons being trained in courses funded by industry. One surgeon stood up and informed the entire course that they need to be clear with their patients about the surgery they are performing, as he had been in Bariatric chat rooms and there is upset within the community about SADI/SIPS/Loop being toted as “the same or similar to Duodenal Switch”.
There was also presenter who said “We are doing something new about every five years.” No, “we” are not. Some of us have stood by the surgery and techniques with the best long term outcomes and not gone with every “new” thing out there. The process of Duodenal Switch may have changes, open Vs. Lap, drains, location of incisions, post operative care and stay, but the tested procedure with the best outcome has been the duodenal switch operation and not the shortcut versions. Although, those of us that are standing by long term results seems to be in the minority. Why do I stand by Duodenal Switch? Because it works, when done correctly by making the length of the bowel proportional to the patient total bowel length, and height, and not just cookie cutter length for all patients, with the right follow-up, patient education, vitamin and mineral regime and eating habits.
A new addition was the Gastric Balloon, which in the research presented had a 60-70% re-gain rate and a no more than 10-15% weight loss one year only. This data represents more than 70% weight regain when the balloon is taken out. The Gastric Balloons can be left in between 4-6 months depending on the brand or type of balloon. The Gastric Balloon is not new to the Bariatrics and was first introduced in 1985. After 20 years and 3,608 patients the results were and average of 17.6% excess weight loss. It seems that we are re-gurgiating old procedures. There are many new medications that were front and center in this meeting.
The Adjustable Gastric Bands were missing from the exhibit hall this year. It is my hope and feeling from the other attendees that we may be seeing the era of the Adjustable Gastric Band being placed in patients come to an end. Although there are some still holding out that there are some patients that can do well with the Band.
Attending the 2015 ASMBS meeting this year, as it has every year, only reemphasized the importance of avoiding what has become the norm of chasing a simple solution that is fashionable and easy now. We stay convinced that the duodenal switch operation with the common channel and the alimentary length measured as a percentage of the total length is by far the best procedure with the proven track record. The patient should avoid the temptation of settling for an unproven procedure or device, because if history holds true, there will be a need for revision surgeries in the future.
Bowel Length in Duodenal Switch
November 09, 2015 6:25 am
Malnutrition is one of the most feared complication of the duodenal switch operation. It may present years after surgery. What is common is a mix of nutritional deficiencies which include fat soluble vitamins, and protein calorie malnutrition. These all point to possible excessive shortening of the common channel. In my practice we have seen patients that have had lengthening of their common channel to improve their metabolic picture. What is very obvious to us, is that we see disproportionately higher number of cases coming to us for revision from practices where the common and alimentary lengths are done as a “standard” numbers with no specific adjustments made for the patient, their anatomy and situation. I have said for years, that the length of the bowel that is measured to be become the common and the alimentary limb should be a percentage of the total length of small bowel, rather than a pre-determined measurement. Here is a visual description of how this works.
If a common channel and the alimentary limb is measured to be a percent of the total length then the chance of protein calorie malnutrition is minimized since this will take into account the bowels absorptive capacity which is being reduced. This decrease in the absorption is done as a fraction of the total length.
Raines et al. published a study in 2014, that showed how small bowel length is related more closely to a patient’s height and not weight. And yet, some surgeons totally based the length of the common channel and the alimentary limb arbitrarily based on the patient pre operative BMI and nothing else. Could this be the cause of why I see some patients coming to us for revision of their duodenal switch for malnutrition?
Duodenal Switch Look Alikes- SADI/SIPS/Loop
October 23, 2015 4:06 pm
There is no substitute for the Duodenal Switch (DS) operation. The other easier procedures that are being presented as DS equivalent are untested, and unproven operations that in my opinion will fall short of the outcome patients expect. The coding definition of BPD/DS is as follows: A Gastric restrictive procedure with partial gastrectomy, pylorus-preserving duodenoileostomy and ileoileostomy (50 to 100cm common channel) to limit absorption (biliopancreatic diversion with duodenal switch) Please not that there are two anastomosis within the definition.
As a patient advocate and a surgeon who has seen a number of recent complications (significant bile reflux gastritis, inadequate weight loss, etc..) of these “Duodenal Switch” substitute procedures, (SADI/SIPS/Loop) I would recommend that any patient considering anything other than the anatomically accurate and proven standard DS procedure realize that they are being subjected to a procedure with an unknown long-term outcome other than what is published in a few studies with a very short-term follow-up. The weight loss of SADI/SIPS/Loop studies have only been measured in terms of months versus years. I would predict that for the majority of those patients, the long-term weight loss will be inadequate and further corrective surgery will be needed, either for inadequate weight loss or other complications such as bile reflux.
Teaching Nursing Students about Duodenal Switch!
October 19, 2015 11:34 am
Dr. Keshishian explaining the different weight loss surgical procedures to nursing students. Including the duodenal switch before cases to a number of nursing students on a board in the operating room. Dr. Keshishian is always willing to educate and draw with a smile but not always with a bowtie!
Cindy Porcell, Surgical tech put the finishing touches on it.
In case you are wondering, surgical scrubs do not have bowties!
Calcium – Revisited !Exclusive Member Content
October 05, 2015 8:06 am
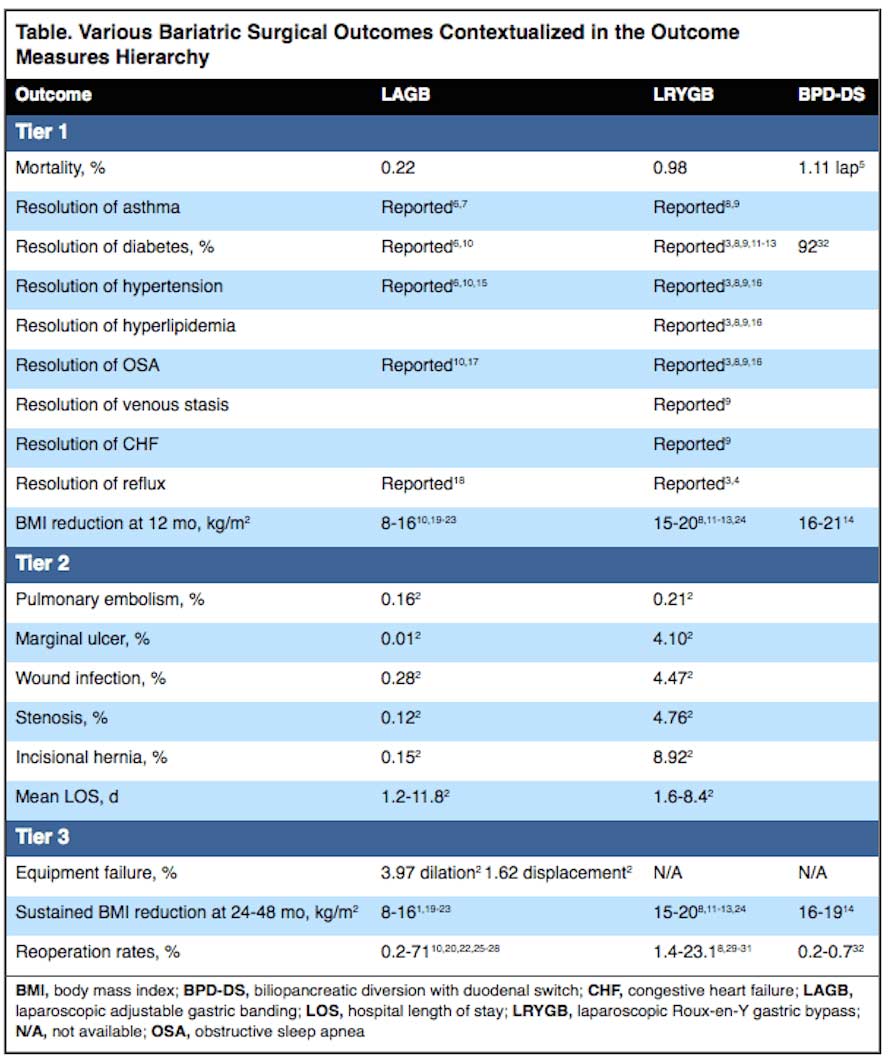
Surgical Outcomes
October 02, 2015 10:10 am
In a recent review article published in the September 2015- Volume 42:10 of General Surgery News, the surgical outcomes of different procedures were summarized. There were evaluated based on a number of measures, including re-operation rates. So interesting to note that the re-operation rate of the duodenal switch is the lowest of all surgical procedures.
Adjustable gastric banding had the highest reported re-operation rate. To be noted is the longer the time lapse the higher the need for re-operation for the band.
Original article here.
Failure of Anti-Reflux Procedures
September 28, 2015 7:13 am
A recent study Published in JAMA Surgery, quoted rate of 10-20% of patients who have had anti-reflux surgical procedures will have recurrence of his symptoms within the research data. There are numerous studies that have identified predictive factors leading to return of the symptoms after surgical intervention. Some of these predictive factors are improper diagnosis, inadequate work up and technical issues.
Due to the significant rise of sleeve gastrectomy as well as a high failure rate of the lap band, we have seen several patients presenting with significant reflux disease after weight loss surgery. There is a little scientific data regarding the failure of anti-reflux procedures in patients who have had previous weight loss surgical operations. In our practice, however, we have extensive experience with anti-reflux operations in patient who have had previous weight loss surgeries including Gastric Bypass, Adjustable Gastric Banding, Sleeve Gastrectomy and Duodenal Switch operation.
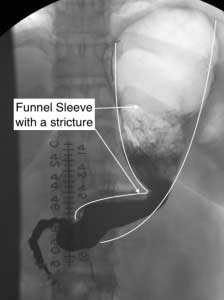
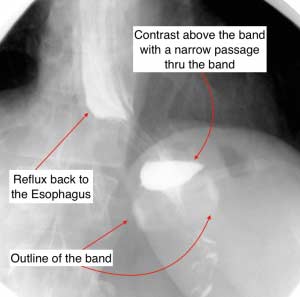
Improper diagnosis, inadequate work up, and technical issues have been cited as possible causes for recurrence of symptoms in patients who have not had weight loss surgery. One could assume that those variables are still a factor in addition to other factors resulting from a previous weight loss surgery. The complications of a previous weight loss surgery can not be under-estimated; an example would be a patient with significant esophageal motility issues directly related to an Adjustable Gastric Band. Other situations that exacerbate symptoms of reflux are an hour glass shaped sleeve or a stricture mid stomach post Sleeve Gastrectomy or Duodenal Switch.
In our experience, some patients have responded well with anti-reflux surgical procedures and mesh placement if indicated after a compete work up with has included and upper endoscopy, upper GI series, manometry and Ph studies. Any patient with symptoms of reflux after weight loss surgery, should be evaluated, and a complete work up should be performed to establish the proper treatment options. It is not wise to have patients be treated with proton pump inhibitors as a default treatment without a complete work up for any patient with reflux. These class of medications have significant side effects associated with them. Furthermore, prolonged reflux is a factor in development of Barret’s Esophagus, a pre-cancerous condition.
Shared Success: Kriston & Shirden
August 27, 2015 5:27 am
My wife, Kriston, and I have struggled with our weights for most of our lives. Over the years we have tried dieting, exercise, medications, and so on….with no luck. A few years ago she started to bring up the idea of weight loss surgery as a possibility. This was an idea that I was dead set against partly for fear of having major surgery and partly because it felt like cheating to me. In my mind, I believed that I should have been able to lose the weight if I really wanted to do so. Kriston continued to bring up the subject. She talked about friends who had had the surgery and how well they were doing with their weight loss. I still resisted the idea until she made the argument that if we didn’t do something about our weight then we might not live to see our daughter grow up and have children of her own someday. That was when I realized that I had to investigate the surgery and what it entailed.
We made an appointment to meet with Dr. Keshishian for an orientation and listened to him as he talked about the problems many people have with weight loss, obesity, genetics, metabolism, what surgeries were available, and the pros and cons of each of them. After meeting him and learning about the surgeries and obesity, I felt very confident that this was the man that could help us with our weight loss struggles. We decided to go with the Duodenal Switch and I scheduled my surgery for June of 2013 and Kriston scheduled hers for November of that same year. We felt this would allow me time to heal and then I would be able to help Kriston after her surgery. I won’t go in to all the details of the surgeries except to say that they both went very well. My recovery was a bit rocky, my wife will say that I was a big baby, but I did recover. I will admit that she was a much better patient than I. Fast forward two years and we are both doing very well. I have lost 180 lbs and Kriston has lost a little over 100 lbs. We look and feel great and we enjoy a much happier and active life style, we even went ocean kayaking last week which is something I could have never done at 370 lbs. This surgery has changed our lives and we could not be happier. We will be forever grateful to Dr. Keshishian, and his incredible staff, for all that they have done to help us become the healthy and happy people we are today.
Hypertrophy of Small Bowel and Weight Gain Years After Duodenal Switch
August 21, 2015 7:53 pm
Duodenal switch (DS) operation results in the highest success rate of all weight loss surgical procedures. Patients, over time, will experience some weight gain many years after DS procedure. There are a number of suspected mechanisms that may be responsible for the weight gain:
1-Ageing may slow the metabolism and the activity down.
2-Over time patients may not be as adherent to healthy dietary and lifestyle changes as they may have been immediately after surgery.
3- Hypertrophy of the alimentary and common channels over time increases in surface area f allowing greater caloric absorption leading to increased weight gain.
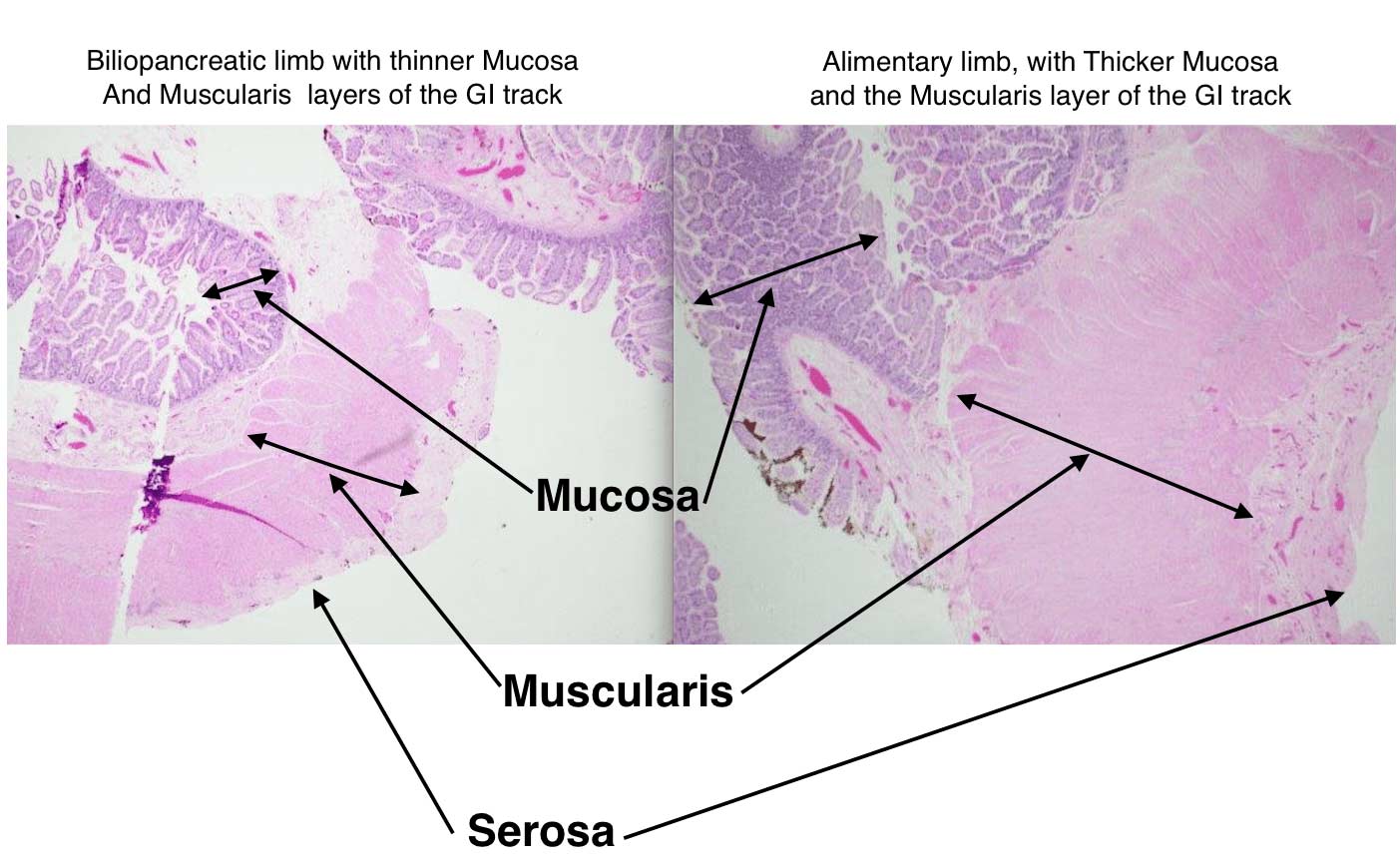
It has been demonstrated in bowel resection studies, as well as rat studies, that the nutrient stimulated regions of small intestine increase villus height and total weight, crypt depth and proliferation as well as wall thickness, as an adaptation to compensate for the loss of absorptive capacity in the resected bowel. This observation may be applied to DS procedure as seen in histological slides from a patient who had to have an operation done requiring bowel resection. The segment of the bowel resected included the junction of the biliopancreatic, common and alimentary limbs.
Internal Hernia And Bowel Obstruction
August 21, 2015 7:49 pm
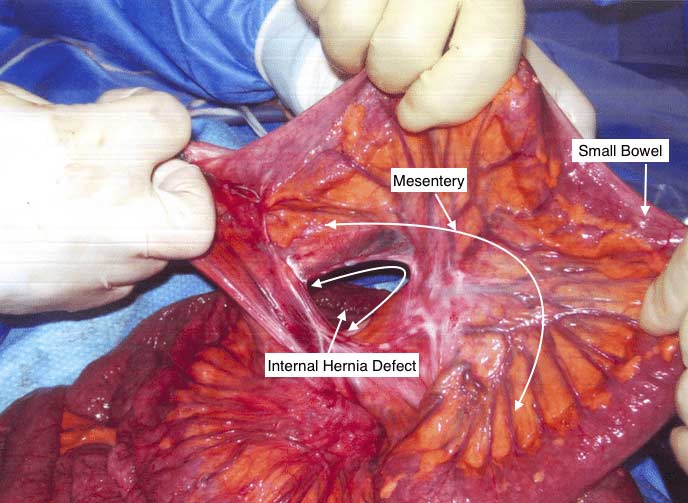
Whenever there is a bowel resection with anastomosis made there will be a defect in the mesentery (the tissue that holds the blood supply and the nerves etc going to and from the bowel) that needs to be closed. In this particular case, the stitches that were used to close the defect were intact and yet the tissue had separated from it. The result is an internal hernia. This can cause bowel obstruction, where by a loop of the bowel can go through the defect and kink the bowel causing the blockage. In some cases, the internal hernia may reduce itself with intermittent symptoms of the bowel obstruction and in other cases it may require immediate emergent surgery. A CAT scan with oral and IV contrast is needed after Duodenal Switch to visualize the alimentary and bioliopancreatic limbs.
Symptoms may include but are not limited to:
- nausea
- vomiting
- abdominal bloating
- abdominal tenderness
- cramping abdominal pain
- diarrhea, constipation
- feeling of inability to completely empty bowels
- fever
- severe abdominal pain.