Tag: BPD/DS
Review & Update Giveaway!
August 31, 2016 6:27 pm
The Prize winners are Jo and Kimberly! Congratulations ladies and enjoy the Obesity Help National Conference! Thank you to all that participated in the Giveaway!
We are holding a review and update giveaway for two different prizes! Thank you for your
participation!
One Prize and One Grand Prize
Prize: two tickets to Obestiy Help National Conference Sept. 30-Oct 1, 2016
Grand Prize: two tickets to Obesity Help National Conference and one night
hotel stay October 1, 2016
Conference: 11999 Harbor Boulevard Garden Grove, California 92840 Event link here
Hotel Prize: SHERATON GARDEN GROVE – ANAHEIM SOUTH HOTEL
12221 Harbor Boulevard
Garden Grove, California
Official Rules:
How to Enter and eligibility: All entrants and winners must be 18 years of age or older at the time of entry. Up to 5 entries per person.
- Write a review of Dr. Ara Keshishian on one or all of the sites below or do an update on your profile on Obesity Help between now and Sept. 8, 2016 at 5:00 PM
2. Take a screen shot of the review or update with your username and date.
3. E-mail the screenshot to [email protected] with your contact information (name, phone number, e-mail, and mailing address )
4. Entries must be a verifiable patient of Dr. Ara Keshishian in Glendale, CA.
Promotion Timing:
The Review & Update Giveaway begins September 1, 2016 and ends September 8, 2016 at 5:00pm PST
How Winners are Chosen:
Winners will be chosen by random draw. Odds of winning vary upon the number of entries received for the giveaway.
Winner Notification and the Claiming of Prizes:
Winners will be notified via the email provided at time of entry and also published on our blog comments www.dssurgery.com/blog and on our FaceBook page. The winner will have 72 hours to respond to the winning notification email or the prize will be forfeited. The prizes have no cash value. The prizes are non-transferable and must be accepted as awarded. No changes may be made to the prizes. There is no cash value for the prizes.
General Conditions:
By entering the Giveaway, entrants agree to abide by and be bound by these Official Rules and the decisions of the Sponsor, which are final and binding in all matters relating to the Giveaway, and release and hold harmless Sponsor and its affiliates, directors, officers, employees and assigns from and against any liability, claims, lawsuits, judgments, losses, damages of any kind, injuries, death, property damage, costs and expenses, arising from, resulting from or in connection with the Giveaway, the participation in the Giveaway, or the receipt, possession, use or misuse of any prize. Sponsor is not responsible for lost, late, incomplete, inaccurate, stolen, delayed, misdirected, undelivered or illegible entries or for lost or stolen entry boxes or other errors or difficulties of any kind whether human, mechanical, electronic, typographical, printing or otherwise relating to or in connection with the Giveaway, including, without limitation, errors or difficulties which may occur in connection with the administration of the Giveaway, the processing of entries, the announcement of the prizes, or in any Giveaway-related materials. Sponsor is not responsible for technical, hardware, software or telephone malfunctions of any kind, lost or unavailable network connections, or failed, incorrect, incomplete, inaccurate, garbled or delayed electronic communications caused by the user or by any of the equipment or programming associated with or utilized in the Giveaway. Persons who tamper with or abuse any aspect of the Giveaway or who are in violation of these Official Rules, as solely determined by Sponsor, will be disqualified and all associated entries will be void. The Sponsor reserves the right, at its sole discretion, to cancel, terminate, modify or suspend the Giveaway if, in Sponsor’s opinion, it is not capable of running as planned, including, but not limited to, due to tampering, unauthorized intervention, fraud, technical or phone line failures or any other problems beyond the control of the Sponsor, and select the winners for affected drawing(s) from among all eligible entries timely received for such affected drawing(s) prior to cancellation.
Duodenal Switch
August 24, 2016 5:45 am
Buyer Beware ! There are a lot of look alike and counterfeit “Duodenal Switch” procedure being performed. A recent online chat discussion clearly demonstrates the point that just because a patient is told that they had the duodenal switch operation this is not necessarily the case.
In our practice, we always warn our patients of not comparing notes and their outcome to others. I perform the Duodenal Switch procedure the way it was described by Dr. Hess, making the common and alimentary lengths as a percentage of the total length of small bowel. This is why our patient population has very little nutritional, and gastrointestinal issues compared to others. Unfortunately when a patient is given a disproportionately long Common channel and/or Alimentary channel the patient will have inadequate weight loss. Alternatively, when patients are given a shorter alimentary channel in proportion to the total bowel length, significant nutritional deficiencies can arise. In a shorter alimentary channel situation patients have to consume higher doses of vitamins and nutrients to keep their laboratory values normal.
I have repeatedly raised the issues to clearly distinguish the single anastomosis procedures from Duodenal Switch operation.
One of the unfortunate problems is the lack of clear guidance given to the patients. It is not uncommon, when I do second opinion consultation with patient who were given generic gastric bypass post op protocol and instructions after their duodenal switch operation. This clearly shows lack of fundamental understanding of the practice performing these procedures and it is carried onto the patient.
Is Weight Loss Important Before Weight loss Surgery?
June 21, 2016 7:52 am
The question of “Is a pre operative diet and weight loss important?” No. This is the short answer. In a previous blog, “Weight Loss Before Weight Loss Surgery?” I have gone into further detail about why I don’t require a pre operative diet and weight loss program.
More recently there has been a concerted effort by a number of major health plans to require 3-6 months documented pre operative diet attempt prior to authorization for weight loss surgery. Furthermore, there are surgeons who would mandate a 10% weight loss as a precondition for the patient to have a weight loss surgery, laparoscopic sleeve gastrectomy for example. The overwhelming scientific literature fails to support any direct correlation between preoperative weight loss and the outcome of the weight loss surgery.
Some surgeons require preoperative weight loss as a way to reduce the size of the liver. I’ve personally have never met a liver I couldn’t work around unless it was severely diseased.
There is some literature to support this position. However, one has to critically look at all the studies. Almost all the studies have very specific population and procedures that are being looked at. Most often the recommendations had been made for adjustable gastric banding procedures. There are also some that are recommending the same for Lap Sleeve cases only siting the reduction of the liver size as a reason for the Very Low Energy Diet as a precondition to surgery. It is, however, important to remind ourselves that there is no long term studies whatsoever that show any relationship between the preoperative weight loss and the outcome of any weight loss surgery.
Weight Loss Surgery Effects On Iron Absorption
June 06, 2016 9:40 am
Anemia is a condition in which a person doesn’t have enough healthy red blood cells. Red blood cells (RBCs) function in carrying oxygen to the tissues and they are produced in the bone marrow. Iron deficiency anemia, the most common form of anemia, develops when the body is unable to produce sufficient hemoglobin because of an iron deficiency. To read more about iron deficiency anemia, please refer to our previous blog post here.
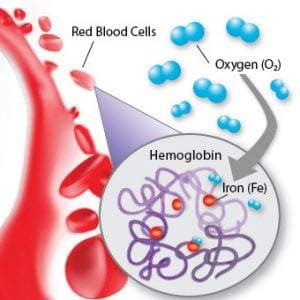
Iron is an essential mineral that is a critical component of hemoglobin. Hemoglobin (Hg) is a four protein molecule that carries oxygen from the lung
s to the tissues. It is also important in maintaining RBC shape for proper blood flow. Each of the four globulin chains in Hemoglobin contain an iron compound called a heme. An iron atom is fixed within the heme group to give the red blood color and transport oxygen and carbon dioxide. If the body does not have enough iron, the bone marrow will not produce enough Hemoglobin which results in unhealthy RBCs.
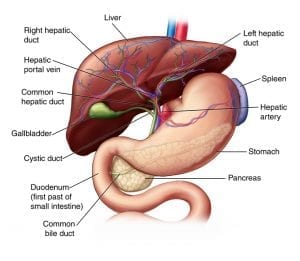
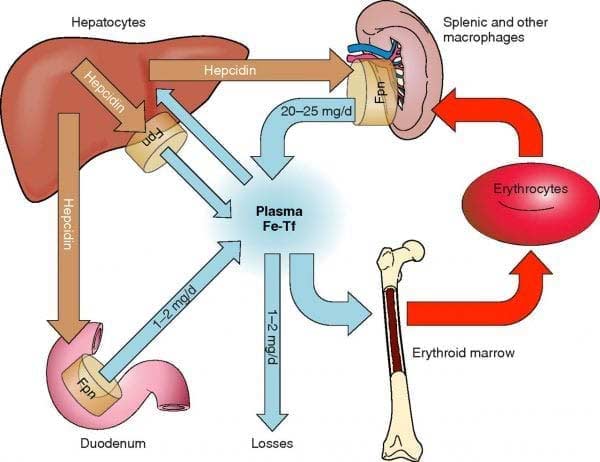
Iron is exposed to acids in the stomach, which alters the form into a configuration that allows absorption. The Duodenum of the small intestines is the main site of iron absorption. The ileum, found at the end of the small intestinal tract, is the site of secondary absorption. Once absorbed, each plasma protein transferrin transports two atoms of iron to the liver, spleen, and bone marrow (2).
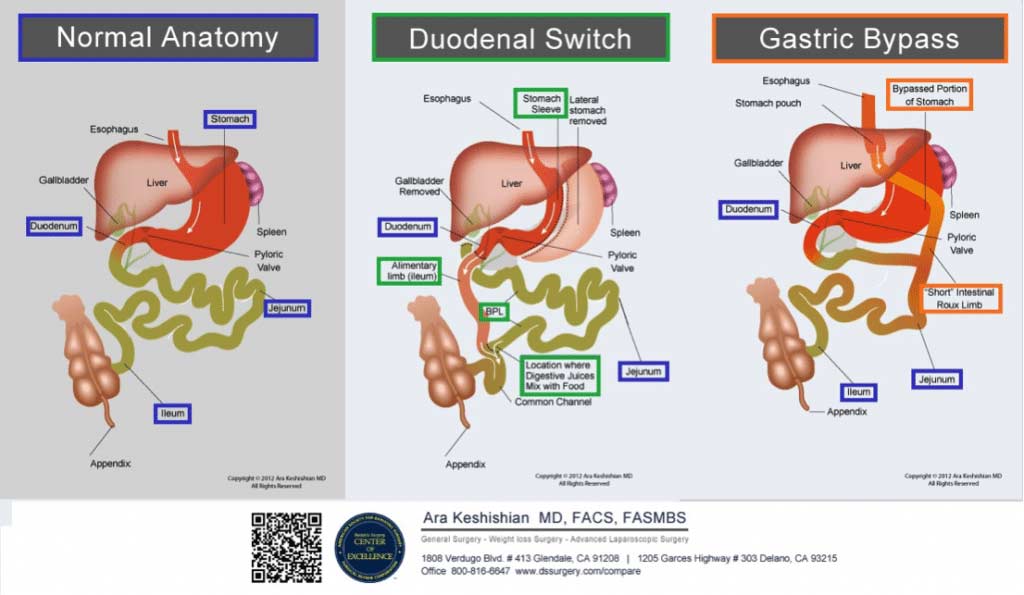
Anemia is common among patients who have undergone surgical weight loss procedures. Some weight loss procedures change the anatomy of the small intestinal tract result in malabsorption due to the restriction of food and nutrient intake. In Roux-en-Y gastric bypass (RYGB), the stomach and duodenum are completely bypassed thereby increasing the risk of iron deficiency. In the Duodenal Switch a small portion of post pyloric Duodenum is left intact to aid in iron absorption, however this may not be adequate for every individual. By redirecting the small intestinal tract in Duodenal Switch, only a small segment of the ileum is able to absorb the necessary nutrients. In both procedures however, blood tests find that patients can become iron deficient (1,3) and require oral iron supplementation or intravenous iron infusions if oral supplementation is inadequate to maintain iron levels.
Inadequate iron levels can be treated by taking iron salt supplements, especially along with vitamin C pills that help the body absorb more iron. Other types of supplements are Heme and chelated oral iron that are well tolerated without gastrointestinal upset of iron salts. For some WLS patients there may not be enough capacity for iron absorption via the GI tract and those patients may need Intravenous Iron infusions periodically. Dietary iron sources are important as a surgical weight loss patient as they are usually also high in protein (blog). Ie: Poultry, red meat, pork, seafood, eggs, beans, and green leafy vegetables are also a good source of iron.
In addition to supplementation of iron, it is important to identify any contributing factors to blood loss or decreased iron absorption such as gastrointestinal bleeding, heavy menses, surgery, pregnancy, medications or combination of supplements, infection or dietary issues. Identifying, advanced planning and/or correcting any contributing factors may reduce the iron demand for WLS patients.
In summary, iron absorption will be affected by altering the anatomy of the small intestinal tract. Although it takes a great deal of time to restore iron levels, reversing deficiency will help avoid symptoms and maintain proper blood, brain, and heart health.
Colored Coded Diagrams of where nutrients, vitamins and minerals are absorbed:
Please note this article and these diagrams are Member Exclusive Only. They are available for use by our patients ONLY. Please review your terms of use of our Member Exclusive Area.
Diagram of normal anatomy absorption here [download id=”14″].
Diagram of DS anatomy absorption here [download id=”8″].
Diagram of RNY anatomy absorption here [download id=”9″]
Written by: Mariam Michelle Gyulnazaryan & Dr. Ara Keshishian
References
- Fincannon J. Iron deficiency after gastric bypass surgery. University of Rochester Medical Center. 2016.
- Forth W, Rummer W. Iron absorption. Physiological Revies. 1973; 53(3) 724-792.
- Sawaya RA, Jaffe J, Friedenberg L, Fridenberg FK. Vitamin, mineral, and drug absorption following bariatric surgery. Curr Drug Metab. 2012; 13(9) 1345-1355.
- Von Drygalski A, Andris DA. Anemia after bariatric surgery: more than just iron deficiency. Nutr Clin Pract. 2009; 24(2) 217-226.
Weight loss Surgery for Treatment of Diabetes
May 25, 2016 7:21 am
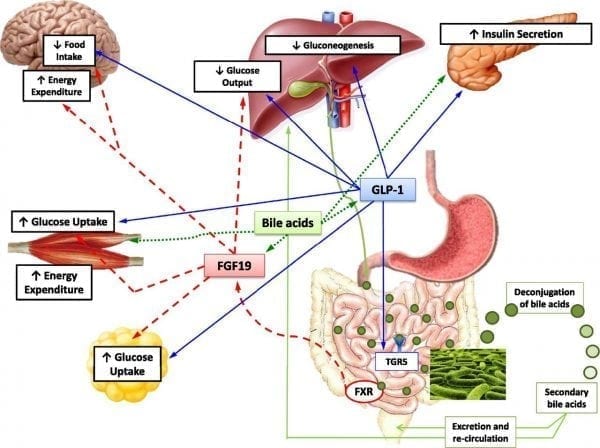
New guidelines and recommendation are coming out of the second Diabetes Surgery Summit in the Fall of 2015. One major change is Metabolic or Weight Loss Surgery for the treatment of Diabetes. With all the advances made in newer classes of medication for treatment of diabetes, the majority of patients who are being treated fail to get to achieve the desired results of lowered blood glucose level. This is in contrast where weight loss surgical procedures such as Duodenal Switch can results in >95% cure rate of type II diabetes.
The American Diabetes Association has made the recommendation for weight loss surgical procedures be considered as a treatment option for type II diabetes.
Summarizing their criteria “According to the new Guidelines, metabolic surgery should be recommended to treat type 2 diabetes in patients with Class III obesity (BMI greater than or equal to 40 kg/m2), as well as in those with Class II obesity (BMI between 35 and 39.9 kg/m2) when hyperglycemia is inadequately controlled by lifestyle and medical therapy. It should also be considered for patients with type 2 diabetes who have a BMI between 30 and 34.9 kg/m2 if hyperglycemia is inadequately controlled, the authors agreed. The Consensus S
tatement also recognizes that BMI thresholds in Asian patients, who develop type 2 diabetes at lower BMI than other populations, should be lowered 2.5 kg/m2 for each of these categories. ”
This is a remarkable change in thought and policy on diabetic treatment and long term strategies that can only improve patient outcomes. Stabilization and blood glucose hemostasis can only improve patient health, health care utilization and health care costs.
Minimally Invasive Weight Loss Surgery
May 17, 2016 9:02 am
Minimally Invasive does not mean better, easier, proven outcomes or good excess weight loss. Weight loss surgical patients should be careful of catch phrases such as “less invasive”, “simpler”, “shorter recovery”, “outpatient” and many others that had been used to described procedures with less than optimal outcome. We should not forget the lessons learned from adjustable gastric banding which was also promoted as ” less invasive, simpler to perform, and be done as an outpatient with a short recovery “. We all know how that story has panned out. The overwhelming majority of patients who had an adjustable gastric banding have undergone revision, had it removed or had additional surgeries following the complications which were associated with this simple procedure.
When evaluating outcome data for weight loss surgical procedures, it is important to bear in mind that the long-term success of these procedures will take years to document. More often than not the early weight loss is significantly better than the long-term stable weight loss. This has been clearly documented in the case of the adjustable gastric banding and the gastric bypass and laparoscopic sleeve gastrectomy operation. Duodenal switch , as described by Dr. Hess using the percentage based technique, has the best long-term documented success of all of the weight loss surgical procedures. The scientific data reports 20+ years of successful excess weight loss with a Hess Duodenal Switch procedure. There has been an alternative proposed to Duodenal Switch recently, the SIPS and SADI procedures. As I have already stated in the past, these are not the same as the duodenal switch operation. Any suggestion or innuendos that SIPS/SADI is the same as the Duodenal Switch is deceptive and misleading. We have also seen attempts to use the same catch phrases as described above to promote these unproven procedures. The published data that’s been reported with SIPS/SADI is mostly short-term in small population studies. There are no long-term studies that have documented the efficacy of the SIPS/SADI procedure and “simpler” or minimally invasive does not mean better.
Magnesium Questions
May 11, 2016 6:07 am
Since our Webinar on Magnesium, I have received several Magnesium Questions recently regarding Magnesium deficiency. There is some evidence that calcium deficiency can not be corrected with an underlying magnesium deficiency. This may be due to the fact that magnesium is essential to converting Vitamin D to it’s active form and more information here. The active form of Vitamin D is needed to actively transport Calcium within the cell. This may be the confusion that calcium absorption needs magnesium. It is not needed directly but rather indirectly via Vitamin D.
Other cofactors needed in Vitamin D metabolism are:
Zinc (high doses antagonist with Magnesium and Copper)
Boron (raises Magnesium blood levels)
Vitamin K2
Vitamin A in small amounts
Further information regarding bone health and nutrients here.
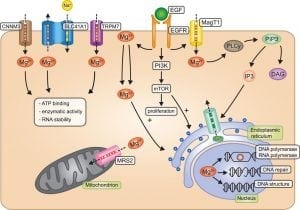
Some important facts about Magnesium are:
- It is Absorbed in the distal Jejunum and Ileum (small intestines) and to some degree the colon.
- Plays an important role in Parathyroid Hormone synthesis which is also acted upon by Vitamin D
- Vitamin D increases Magnesium absorption
- All enzymes that metabolize Vitamin D require Magnesium
- Magnesium has a positive effect on Vitamin D deficiency.
- Magnesium and calcium are antagonist to each other on a cellular level (work against each other) They use an overlapping transport system for reabsorption within the kidneys and thereby compete with each other. Magnesium may also bind to calcium binding sites and intracellular protein binding sites due to their similarity.
- Calcium supplements can decrease Magnesium absorption.
- It Activates digestive enzymes for protein, fat and carbohydrate metabolism.
- Essential for protein synthesis
- Stores and moves energy acquired from digestion.
- Regulates Calcium via Vitamin D and increasing urinary excretion of calcium
Factors inhibiting Magnesium absorption:
- PPI
- Fiber
- Phytates
- Excessive unabsorbed fatty acids
- Calcium
- Phosphorus
- Protein
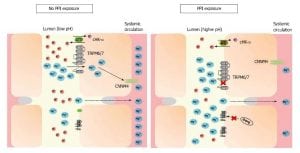
In summary, post Bariatric patients are at risk for magnesium deficiency and it plays an important role in overall health and bone health. Our practice recommends Magnesium Glycinate as the form for supplementation in at least a 2:1 ration with calcium. An example is: Calcium 2000mg daily to Magnesium Glycinate 1000mg daily. (Supplement based on your laboratory studies) We hope that this blog has answered some of your Magnesium Questions.
Dual Testimonial: Cameron’s Gastroparesis surgery & Scott’s Revision of a Duodenal Switch
February 01, 2016 8:04 am
In 2015, I came into contact with the most unique, passionate, urgently responsive; talented beyond belief and caring surgeon I have ever met. Our oldest son who is a 21-year-old cancer survivor, has had nearly five years of medical nightmare as diagnosed with severe gastroparesis resultant from his vagal nerve being severed during a previous Nissen Fundoplication surgery. We didn’t find out that this had happened until nearly two years later and only after a 4 hour gastric emptying test showed that Cameron’s stomach was only about 30% emptied after four hours (should be empty after an hour) due to gastroparesis.
I had heard about Dr. Keshishian on a Bariatric support group page on which I post and get great advice. The surgeon back in Central, IL where we live told us that Cameron needed a subtotal gastrectomy to remove 80% of his stomach! This sounded radical and no way in the world was that going to happen. I was given Dr. Keshishian’s email address so I could consult with him for his advice. It was a Saturday morning around 7 AM Central time when I sent off an email to Dr. Keshishian detailing Cameron’s medical history and current issues. I was in hoping that his office would get the email on Monday and hopefully get back to me within a week. I went out to my kitchen to get a cup of coffee and when I returned I had a missed call with a California area code. Yep, it was Dr. Keshishian. I called back and we talked for 45 minutes. He suggested several things and told me that any good general surgeon in my area could do surgery on Cameron and fix him, well that was the only time he was wrong. We couldn’t find anyone in our area who would do the surgery.
So we talked and agreed that Cameron needed a Roux-en Y drain put in place to physically drain his stomach by way of gravity (not for any weight loss as very little small bowel was bypassed). Dr. Keshishian got us in the next week and we flew out to Glendale where he met with Cameron for an examination on that Monday. On Tuesday, Dr. Keshishian performed surgery to fix Cameron’s herniated diaphragm, loose Nissen wrap, performed the Roux-n Y limb and anastomosis to the stomach. Dr. Keshishian also found a Meckel’s diverticulum (a congenital small bowel defect that can cause internal bleeding and serious issues). The following Sunday, Cameron developed severe pain due to chronic pain from his Cancer treatment and 12 subsequent surgeries, many on his abdomen. Dr. Keshishian saw Cameron in the ER and spent 3 hours fixing Cameron’s pain issue and making sure he was medically sound so we could fly home the next day.
Today, Cameron has very little to no issues which you wouldn’t have believed possible six months earlier. In the past, he had violent retching, dry heaving and bad nausea daily which had him severely incapacitated and very depressed due to a feeling of hopelessness and pain from the Gastroparesis. He didn’t believe he had a chance at a normal life but Dr. Keshishian gave Cameron his life back. We are eternally grateful for your huge heart and talent Dr. Keshishian. Thank you!
During our time in Glendale in 2015 for Cameron’s surgery Dr. Keshishian and I began discussing my situation. I had been given a virgin Duodenal Switch performed by a surgeon in Illinois in September of 2013. A year later in 2014 and 180 lbs lighter, I ended up in the hospital as I was passing out. I had a resting heart rate of 35 BPM, a blood pressure in the 75/40 range and incredibly bad labs including anemia, low copper, low zinc, and dangerously low albumin and total protein. A full cardiac work up was completed and I spent a week in intermediate care. Why? I was extremely malnourished even though I was consuming 200-250 grams of protein daily! Why was I malnourished? Because my original surgeon performed a “cookie cutter DS” on me where he didn’t measure my small bowel and arbitrarily gave this 6’2 man a 100 cm common channel and a 150 cm Alimentary limb. Way too short on the AL! Had the Hess method been followed (the only way the DS should be allowed to be completed) my CC would have been 100 cm (that was okay) but my Alimentary channel should have been 275 cm! Simply put, my absorbing portion of small bowel was 34% and the Biliopancreatic limb (non-absorbing) was 66%. It should have been a 50/50 ratio with 100 cm CC, 275 cm AL and a 375 cm BPL. In order to combat my severe malnutrition that September of 2014 I went on a pancreatic enzyme (CREON) to assist my nutrient absorption. I was taking with meals right around 400,000 IU’s of CREON (a boat load) and this was barely keeping my nutrients in range and lab values barely in range. After speaking with Dr. Keshishian, he recommended that I give it until around September of 2015 to see if my absorption increased enough to where a revision wouldn’t be required. Towards the end of July, I all of the sudden lost nearly 20 pounds in two weeks from my already frail and scrawny body. I saw my surgeon in Peoria as I was very alarmed; and I had been having bad cramping and other issues point to a possible bowel obstruction His exact words to me were “see me in 30 days, you are like the DS poster boy of good nutrition”. As you can imagine I found that completely unacceptable and soon as I was out of that appointment I emailed Dr. Keshishian. He told me that if I couldn’t get a revision ASAP I would need to immediately go on TPN. Two weeks later my wife and I landed at LAX and were in Glendale on Monday morning for an exam with Dr. Keshishian.
The job Dr. Keshishian did describing what he was going to do, and of course this was a visual presentation with Dr. Keshishian drawing (you know Dr K’s love of drawing) out for us what he was going to do. He thoroughly explained for my wife and I so she was comfortable with what was going to happen and we fully understood what he was going to do. Doc also found an umbilical hernia that he was going to repair and I had an anal fissure as well that wouldn’t heal so we discussed what he would do to examine and possibly fix during my revision surgery. The next day Dr. Keshishian performed surgery where he fixed the umbilical hernia, measured my total small bowel length to determine appropriate channel lengths and found an repaired a huge mesenteric defect (intestinal hernia and Dr K has a picture of my guts with the huge hole in the mesentery that he has posted on his blog discussing intestinal hernias and blockages), fixed my fissure (Thank you!) and put in a side by side anastomosis that effectively lengthened my AL by 125 cm and my CC by 25 cm worth of absorption. This put my absorbing intestine to BPL ratio where it should have been in the first place (50/50 ratio).
I am pleased to say that I immediately went off the CREON and my absorption and subsequently my lab values improved tremendously. At surgery on August 18, 2015 I weighed a whopping 170 lbs. Today I am weighing in at 183 pounds and well on my way to Dr. Keshishian’s suggested optimal weight target of 205.
Dr. Keshishian is absolutely amazing and the best in the world when it comes to performing the Duodenal Switch and revision to DS Surgery (Band to DS, RnY to DS, Channel extending revision to DS). I would recommend Dr. Keshishian to any patient who needs a virgin Duodenal Switch to get their health back and especially to those who were sold a garbage RnY or Crapband procedure that ultimately failed you (it failed you, you did not fail). In fact, I am trying very hard to convince my brother and Step Mother to fly to Glendale and have Dr. Keshishian perform a Duodenal Switch on them. They very much need it for their health and Dr. Keshishian is the best in the world having performed over 2,000 DS procedures.
I don’t say this lightly. Ara, you are one of the finest human beings I have ever had the good fortune of knowing and your surgical skills are second to none. I really do admire and love this gentleman like a brother and consider him to be a friend. Thank you for using your incredible skill to fix my health issues resultant from the failed cookie cutter Duodenal Switch I was given two years earlier by another surgeon. Had I met you back then and knew what I know now, you would have performed my virgin DS and I would not have suffered for two plus years. Thank you from the bottom of my heart, Dr. K!
NSAIDS Use After Duodenal SwitchExclusive Member Content
January 30, 2016 9:19 am
Fluids and Electrolytes After Weight Loss Surgery
January 29, 2016 7:06 am
Fluids and Electrolytes after weight loss surgery are an important part of recovery and lifestyle after undergoing a weight loss surgical procedure. Potassium is an important electrolyte found in higher concentrations within the fluid of the cells. It is important in muscle contraction, heart rhythm, nerve function and co-enzyme function.
Fluids and Electrolytes
The following webinar (link) discusses the balance of fluids and electrolytes with particular attention to post weight loss surgery concerns. Deficiencies can cause heart arrhythmias, muscle weakness and cramping, intestinal paralysis, and neurological deficits.
The Daily Recommended Amount for Potassium is 4,700mg
Here is a list of Lower-carb potassium sources: This is not meant to be in inclusive list. There are many higher carb sources of potassium also.
- Beet Greens- 1/2C 655 mg
- Trout 3oz – 375 mg
- Salmon 719 mg per average filet
- Halibut or Yellowfin Tuna 3oz – 500mg
- Clams 3oz- 534 mg
- Avocados 1 whole- 974 mg
- Squash 1C- 325mg
- Broccoli 1 cup 475m
- Watermelon Radish 3 oz – 233mg
- Sweet Potatoes- one potato 694mg
- Yogurt 1C – 579mg
- Tomato paste 1/4C – 342 mg
- Whole milk 1C – 366 mg
- Chicken breast meat 1 cup chopped – 358 mg
- Cauliflower 1 cup raw– 303 mg
- Peanut butter 2 T – 208 mg
- Asparagus spears 6 – 194 m
- Daikon Radish – 3″ – 280 mg
- Nuts 100-300 mg per 30g / 1 oz serving, depending on the type
- Dark leafy greens 160 mg per cup of raw, 840 mg per cooked
- Kohlrabi 3oz- 98mg
- Mushrooms 1 C- 273 mg
- Spinach – 1 cup 167 mg Potassium
- Walnuts 2 oz-250 mg