Category: Billroth I
Minimally Invasive Weight Loss Surgery
May 17, 2016 9:02 am
Minimally Invasive does not mean better, easier, proven outcomes or good excess weight loss. Weight loss surgical patients should be careful of catch phrases such as “less invasive”, “simpler”, “shorter recovery”, “outpatient” and many others that had been used to described procedures with less than optimal outcome. We should not forget the lessons learned from adjustable gastric banding which was also promoted as ” less invasive, simpler to perform, and be done as an outpatient with a short recovery “. We all know how that story has panned out. The overwhelming majority of patients who had an adjustable gastric banding have undergone revision, had it removed or had additional surgeries following the complications which were associated with this simple procedure.
When evaluating outcome data for weight loss surgical procedures, it is important to bear in mind that the long-term success of these procedures will take years to document. More often than not the early weight loss is significantly better than the long-term stable weight loss. This has been clearly documented in the case of the adjustable gastric banding and the gastric bypass and laparoscopic sleeve gastrectomy operation. Duodenal switch , as described by Dr. Hess using the percentage based technique, has the best long-term documented success of all of the weight loss surgical procedures. The scientific data reports 20+ years of successful excess weight loss with a Hess Duodenal Switch procedure. There has been an alternative proposed to Duodenal Switch recently, the SIPS and SADI procedures. As I have already stated in the past, these are not the same as the duodenal switch operation. Any suggestion or innuendos that SIPS/SADI is the same as the Duodenal Switch is deceptive and misleading. We have also seen attempts to use the same catch phrases as described above to promote these unproven procedures. The published data that’s been reported with SIPS/SADI is mostly short-term in small population studies. There are no long-term studies that have documented the efficacy of the SIPS/SADI procedure and “simpler” or minimally invasive does not mean better.
Billroth I or II and Diabetes
March 01, 2016 8:37 am
I have previously discussed the two variations of anastomosis that can be created between the stomach and the first segment of the small bowel. Historically, Billroth I and II procedures were named after Dr. Theodor Billroth who did the first of this type of operation in the 1881 (BI) and then in 1885 (BII).
The following article published in Bariatric Times 2016;13(2);8-10. discusses the resolution of diabetes and its outcomes based on these two types of the anastomosis between the stomach and the small bowel.
Billroth I VS Billroth II
This study concludes that “In summary, we concluded that based on our analysis of the literature, BII reconstruction is more effective than BI reconstruction for achieving postoperative diabetes control.”
Lets remind ourselves that Duodenal switch is a BII reconstruction where as the SIPS, SADI and other lookalikes are BI.
This study only reiterates that these unproven operations need to be studies further and that the patients need to be aware of the consequences of their decisions when choosing a particular operation. Be aware and informed to know the differences between Duodenal Switch and the procedures that are promoted as similar one – which they are not.
Visual comparison of Duodenal Switch and SADI/SIPS/Loop here.
Further description of Duodenal Switch here.
Billroth I & II, SIPS, SADI, Loop
July 27, 2015 1:30 pm
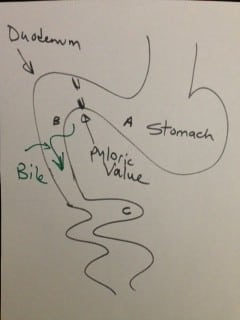
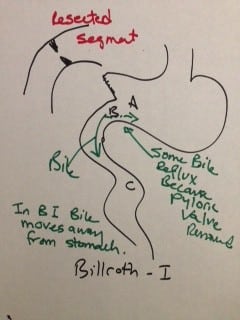
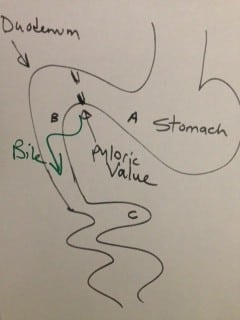
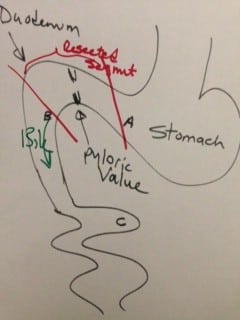
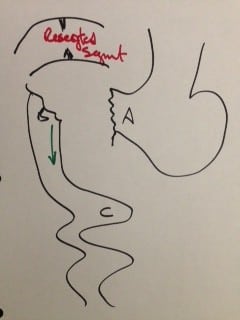
In 1881, Dr. Theodore Billroth performed the first successful gastrectomy for pyloric tumor. He removed the distal part of the stomach and tumor of the pyloric region and reconnected the distal end of the transected stomach directly to the segment of the duodenum. This was later renamed as Billroth I procedure. In Billroth I the anastomosis allows the food pathway to stay in the same directional flow with the exception of pyloric valve having been removed. There is, however, increased incidence of bile reflux with the pyloric value removal.
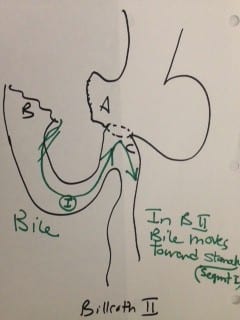
There are incidences where the resected segment is so large that the proximal stomach and the distal duodenal can not be mobilized and brought close to each other to be able to create the Billroth-I anastomosis. Larger resection, where the Billroth I could not be completed Dr. Billroth in 1885 created a procedure call the Billroth II. The Billroth II was performed when the tumor was very large and the continuity of the GI track was created by a loop gastrojejunostomy. This procedure was named Billroth II.
In the Billroth II the bile flow from the small bowel flows toward the stomach, and this results in a much higher incidence of Bile reflux and its associated complication.
The lesson learned from Billroth I and Billroth II was that bile reflux can be a significant problem when creating the continuity of the proximal GI track with exclusion of the pyloric valve. In Bilroth II, there is the additional burden of the bile flowing toward the stomach unlike the Billroth I.
The SADI or SIPS, Loop procedures that are incorrectly promoted as “duodenal switch” employ a loop anastomosis, which results in a biliary flow toward the post pyloric duodenum significantly increasing the chance and the possible incidence of Bile reflux.
All these unknowns about the SIPS, SADI Loop are yet to be investigated.
- Weight loss Medications compared to surgery February 20, 2024
- SIPS-SADI and ASMBS December 31, 2023
- Survey December 16, 2023
- Long Term Outcome Survey December 1, 2023
- Weight Loss Injection May 10, 2023