Category: pre-operative workup. weight loss surgery
Is Weight Loss Important Before Weight loss Surgery?
June 21, 2016 7:52 am
The question of “Is a pre operative diet and weight loss important?” No. This is the short answer. In a previous blog, “Weight Loss Before Weight Loss Surgery?” I have gone into further detail about why I don’t require a pre operative diet and weight loss program.
More recently there has been a concerted effort by a number of major health plans to require 3-6 months documented pre operative diet attempt prior to authorization for weight loss surgery. Furthermore, there are surgeons who would mandate a 10% weight loss as a precondition for the patient to have a weight loss surgery, laparoscopic sleeve gastrectomy for example. The overwhelming scientific literature fails to support any direct correlation between preoperative weight loss and the outcome of the weight loss surgery.
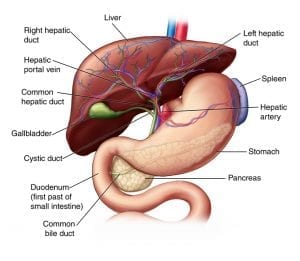
Some surgeons require preoperative weight loss as a way to reduce the size of the liver. I’ve personally have never met a liver I couldn’t work around unless it was severely diseased.
There is some literature to support this position. However, one has to critically look at all the studies. Almost all the studies have very specific population and procedures that are being looked at. Most often the recommendations had been made for adjustable gastric banding procedures. There are also some that are recommending the same for Lap Sleeve cases only siting the reduction of the liver size as a reason for the Very Low Energy Diet as a precondition to surgery. It is, however, important to remind ourselves that there is no long term studies whatsoever that show any relationship between the preoperative weight loss and the outcome of any weight loss surgery.
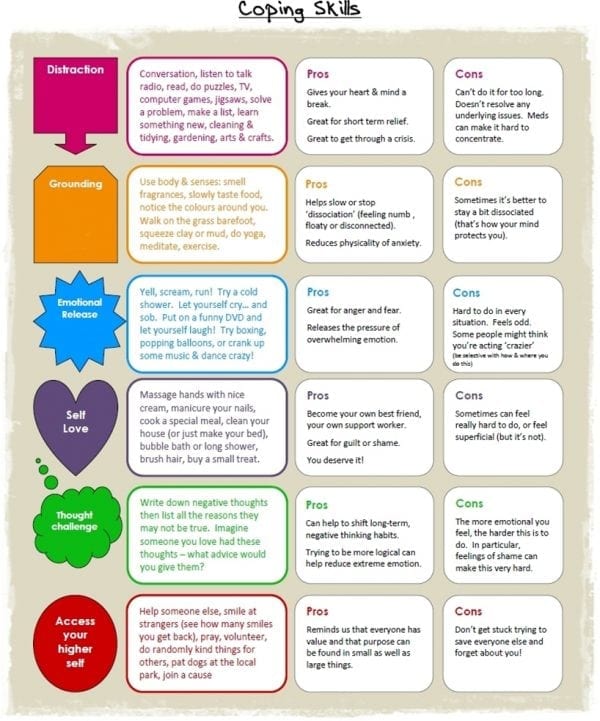
Coping Skills after Bariatric Surgery
June 02, 2015 7:23 am
For many people, food can become a coping mechanism and a way to self sooth or comfort themselves. After weight loss surgery the ability to use food in this manner is disrupted due to the smaller portions and in some cases food intolerances. Developing alternative and healthy coping skills is an imperative step after weigh loss surgery.
Obesity is a multifactorial process that has many contributing aspects. Although, obesity is not entirely the result of poor eating behavior, and lack of exercise. After weight loss surgery, we should appreciate the importance of healthy dietary choices; being sure that volume and frequency is not driven by emotion or emotional eating.
The mental aspect of weight loss surgery should not be ignored. Developing healthy coping skills can be a large part of dealing with the changes that take place. Some people go through a mourning period for the loss of the foods that once gave them comfort, made them part of a group, or the feeling of their best friend. In some cases, there may be a need to seek the assistance of a mental health care provider to be able to work through some of the issues and feelings. Never hesitate or be afraid of contact a mental health care professional.
Learning and practicing effective coping/soothing techniques can be started prior to weight loss surgery. The following are some coping skills that can be effective for some to adopt into their daily lives.
1. Nature – Get out into the great outdoors and into the sunlight. The sounds and sights of nature have a way of energizing the body and calming the mind. Sunlight is excellent for increasing Vitamin D levels which can help elevate mood and general well being.
2. Exercise – The mental and physical effects of exercise are paramount after weight loss surgery. The natural chemical release from exercise is a calming effect and gives a sense of well-being. In addition, the physical aspects of increase weight loss and change in body contour have positive mental and emotional effects.
3. Music- There are many research articles regarding the positive effects on both metal and physical aspects of music. Music has a way of soothing or energizing the soul. Turn up loud or keep it soft. Sing along. Dance it out if you need to.
4. Journaling – We always suggest to people prior to weight loss surgery to start journaling. It can give you perspective when you look back at entries. We also suggest to journal body measurements, pictures, and weights so that you might look back at how far you’ve come from your starting point.
5. Mindfulness – Using all five sense to experience life and food. Take your time to take everything in and experience the full effect. Be present in all life experiences. Ask yourself: Am I enjoying this? Does this feel like what I need? Is this getting me to where I want to be? Is this healthy for me?
6. Support groups of peers- There is nothing like having a group of people who have been there or know exactly how you may be feeling to be able to talk, share or vent. There are so many support groups that can be taken advantage of in either face to face or cyber groups.
7. Treat yourself- Treat yourself and practice self-care by doing something that you find relaxing, gratifying or energizing. Massage, manicure, an outfit, shoes, an outing, or a class.
8. Distraction- Hobbies, new skills, reading, games, bubble bath, or anything that get you out of the same mental spot can help with calming and soothing.
9. Talking- There is great value in having a close friend or trusted therapist to be a sounding board and give you an opportunity to unload some of the challenges you’ve been carrying.
Changing habits and coping skills takes practice and patience. It is not something that is easily changed over night. Focus on small steps, goals and achievements. Give yourself time and credit for the accomplishments that you’ve made. Always look at how far you have come and the positive lifestyle changes you’ve made. There may be set backs but don’t beat yourself up about it, move on and continue to take steps toward your goal.
https://www.counselorlady.com
Aetna and Blue Shield 6 month Diet Requirement Changes
May 15, 2015 3:16 pm
- Member’s participation in a physician-supervised nutrition and exercise program must be documented in the medical record by an attending physician who supervised the member’s participation. The nutrition and exercise program may be administered as part of the surgical preparative regimen, and participation in the nutrition and exercise program may be supervised by the surgeon who will perform the surgery or by some other physician. Records must document compliance with the program; the member must not have a net gain in weight during the program. Note: A physician’s summary letter is not sufficient documentation. Documentation should include medical records of physician’s contemporaneous assessment of patient’s progress throughout the course of the nutrition and exercise program. For members who participate in a physician-administered nutrition and exercise program (e.g., MediFast, OptiFast), program records documenting the member’s participation and progress may substitute for physician medical records; and
- Nutrition and exercise program must be supervised and monitored by a physician working in cooperation with dieticians and/or nutritionists, with a substantial face-to-face component (must not be entirely remote); and
- Nutrition and exercise program(s) must be for a cumulative total of 6 months (180 days) or longer in duration and occur within 2 years prior to surgery, with participation in one program of at least 3 consecutive months. (Precertification may be made prior to completion of nutrition and exercise program as long as a cumulative of 6 months participation in nutrition and exercise program(s) will be completed prior to the date of surgery.)