Biofilm
April 26, 2020 9:44 am
Written By: Eric Baghdasaryan, Maria Vardapetyan, Osheen Abnous
Biofilm are tiny microorganism-filled communities found throughout the human gastrointestinal tract and oral cavity. These communities adhere to both biological and non-biological surfaces within the human body. They provide their inhabitants with many competitive advantages that help these bacterial communities withstand biological, chemical, and physical stresses1. Within these communities, microorganisms collaborate with one another to increase the likelihood of growth and multiplication despite the harsh conditions of the human gut. Not all bacteria within these biofilms are harmful, but those that are go on to cause infections and other severe health problems for the host.
Biofilm formation
Studies have shown that approximately 60-80% of bacterial infections in the human body are associated with biofilm formation. Such findings have compelled researchers to investigate the complex factors responsible for biofilm formation.
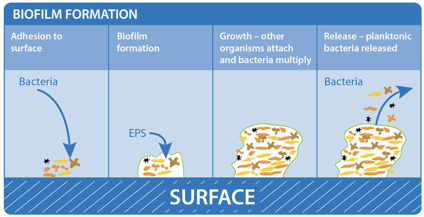
Figure 1: Biofilm adhesion, formation, and maturation. whiteley.com.au/biofilms
It was shown that bacteria anchor themselves to the mocosa surface. They collectively form a protective layer made of polysaccharides, proteins, and extracellular DNA. This forms the biofilm matrix. This biofilm matrix acts as a shield against antimicrobials, toxins, and antibodies. From here, biofilm associated bacteria go on to cause chronic infections characterized by persistent inflammation and tissue damage, initiating in the gut and adjacent regions of the gastrointestinal tract. Furthermore, some biofilm associated bacteria have shown the ability to disperse from this mature biofilm to colonize new niches, underscoring the association between local infections and systemic diseases such as atherosclerosis and rheumatoid arthritis2 caused by the buildup of biofilm dispersed bacteria and subsequent inflammation in the coronary vasculature and joint capsules, respectively. In fact, BADAS syndrome (bowel associated dermatosis-arthritis syndrome) is a condition where patients present themselves with small bumps on their inner skin (mainly along the vasculature) caused by the buildup of circulating microtoxins (very small clusters of bacteria). This may lead to chronic bacteremia in the bloodstream. Also, the over circulation of host immune complexes presents many problems for the patients, such as the development of arthritis and the accompanying joint pain, caused by the build up of white blood cells in host joint capsules. Patients often link the lumps to a dermatological condition, when in reality the condition is caused by a bacterial overgrowth originating in the gut and bowel. Clinicians now believe it is very likely these bacteria are biofilm-associated and a proper early diagnosis of the biofilm origin is critical to the prevention of BADAS and similar pathologies3.
The formation of biofilms has been studied on foreign substances such as intravenous catheters, orthopedic implants, and other biomaterials that have shown device-associated infections. However, it is commonly accepted that the majority of chronic bacterial infections involve biofilm formation on natural surfaces. The pathogenic bacterial overgrowth, forming the biofilms, have been linked to major diseases of the gastrointestinal tract including Inflammatory bowel disease and colo-rectal cancer4.
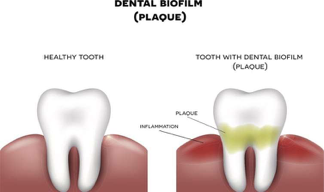
In addition to the gastrointestinal tract, biofilms can also be formed in the oral cavity. Over 700 bacterial species reside in the oral cavity. These contribute to the outgrowth of oral biofilms (otherwise known as dental plaque, see figure 2). These oral biofilms are responsible for major oral diseases such as tooth decay, gingivitis, and periodontitis. Moreover, those with periodontal infections have significantly increased risk of cardiovascular diseases, including atherosclerosis, myocardial infarction, and stroke2. The inflammation caused by oral biofilm may also be a contributing cause of conditions such as diabetes and rheumatoid arthritis1. Therefore, the control of oral biofilm growth before the development of oral infections is critical for the prevention of these system conditions.
Figure 2: Oral Biofilm Formation.
https://phys.org/news/2018-10-scientists-infection-causing-biofilms.html
This symbiotic (mutually beneficial) relationship between gut microbiota (bacteria living in our gut) and the host begins at birth and is crucial to our overall fitness and health. However, certain external and internal factors modify the gut microbiota. This causes the formation of a pathogenic biofilm, which leads to detrimental health conditions. The same bacteria that was once helping us by maintaining a healthy gastrointestinal tract, is now triggering disease conditions4.
Due to bacteria’s ability to translocate, migrate, and colonize new surfaces or niches, biofilm associated infections in the gut have been linked to systemic infections in other organs, including the joints, the skin, the eyes, the vasculature, the lungs, and even the central nervous system. It is assumed that the formation of a thick mucosal biofilm might be used as a diagnostic biomarker for the onset of systemic diseases. The outgrowth of a biofilm is widely viewed as the tipping point between two alternative states: a healthy and diseased gut1.
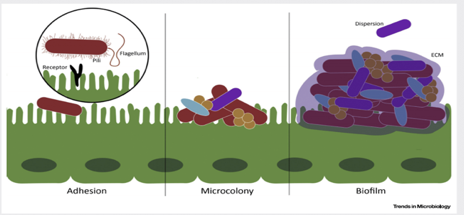
Figure 3. Biofilm matrix – a protective layer. Trends in Microbiology.
The biggest clinical challenge with biofilm-associated infections is their high resistance to antibiotic therapy. The effective therapeutic concentration of certain antibiotics to fight off bacteria within a biofilm (amount of the antibiotics needed in order to have positive therapeutic effects) is about 100-1000-fold higher than if the same bacteria were not associated with a biofilm2. The extracellular matrix, scaffold that keeps the bacteria anchored in place, prevents the penetration of host immune cells into the biofilm, thus contributing to the increased survival of the bacterial species living within the biofilm. Bacteria living within a biofilm also undergo an increased number of mutations, leading to the generation of more antibiotic-resistant phenotypes of bacteria. Finally, studies have shown that minimal concentrations of antibiotics may actually facilitate and stimulate biofilm formation, which can be extremely problematic in clinical treatment2. Therefore, to decrease the risk of biofilm induction, physicians should begin with very high doses of chemotherapeutics (antibiotics) from the very beginning of diagnosed infection. Looking ahead, there is clearly a need for novel biofilm-targeted therapies that are specifically made to prevent biofilm formation as well as eliminate the biofilm completely once it has already matured. Researchers have identified several drug candidates – DNase, lactoferrin, chlorhexidine, and taurolidine2 – that they believe have the potential to effectively penetrate and destroy components of the biofilm matrix. Further research is needed to determine their efficacy.
References
- Tytgat HLP, Nobrega FL, van der Oost J, de Vos WM. Bowel Biofilms: Tipping Points between a Healthy and Compromised Gut? Trends in Microbiology. January 2019;27(1): 17-25. doi:10.1016/j.tim.2018.08.009.
- Marcinkiewicz J, Strus M, Pasich E. Antibiotic Resistance: a “dark side” of biofilm-associated chronic infections. Polskie Archiwum Medycyny Wewnetrznej (Polish Archive of Internal Medicine). 2013;123(6):309-312.
- Buret AG, Motta JP, Allain T, Ferraz J, Wallace JL. Pathobiont release from dysbiotic gut microbiota biofilms in intestinal inflammatory diseases: a role for iron? Journal of Biomedical Science. January 2019;26(1) doi:10.1186/s12929-018-0495-4
Why Oxygenation in Covid-19 is a major problem
April 21, 2020 7:27 am
Covid-19 is a respiratory virus. The majority of patient may experience no or minimal symptoms. But small subset of those infected will unfortunately progress to have significant pulmonary dysfunction. Some will even require mechanical ventilation. Oxygenation in COVID 19 patients with severe symptoms is altered. This is the due to the changes caused by the virus.
Normal Physiology
Oxygen (O2) is exchanged with Carbon Dioxide(CO2) in the lungs. The CO2 is exhaled and the O2 is taken up by the blood. This high O2 continuing blood is then pumped to every single organ. With complete distribution network of capillary vessels, every cell then gets access to the O2 rich blood. Hemoglobin is the carrier that transports the O2.
The O2 is removed and dissociated from the Hgb depends on a number of variables. Each red cell Hgb has four binding site for the oxygen. The affinity and strength of each one of those four units for oxygen changes based on a number variables. These are CO2, Acidity (PH), DPG and temperature.
Oxygen Dissociation Curve
The oxygen dissociation curve has a long “S” shape. On the low end of oxygen in the blood most of the Hgb site are occupied. As the oxygent level increase there is little change to the saturation.
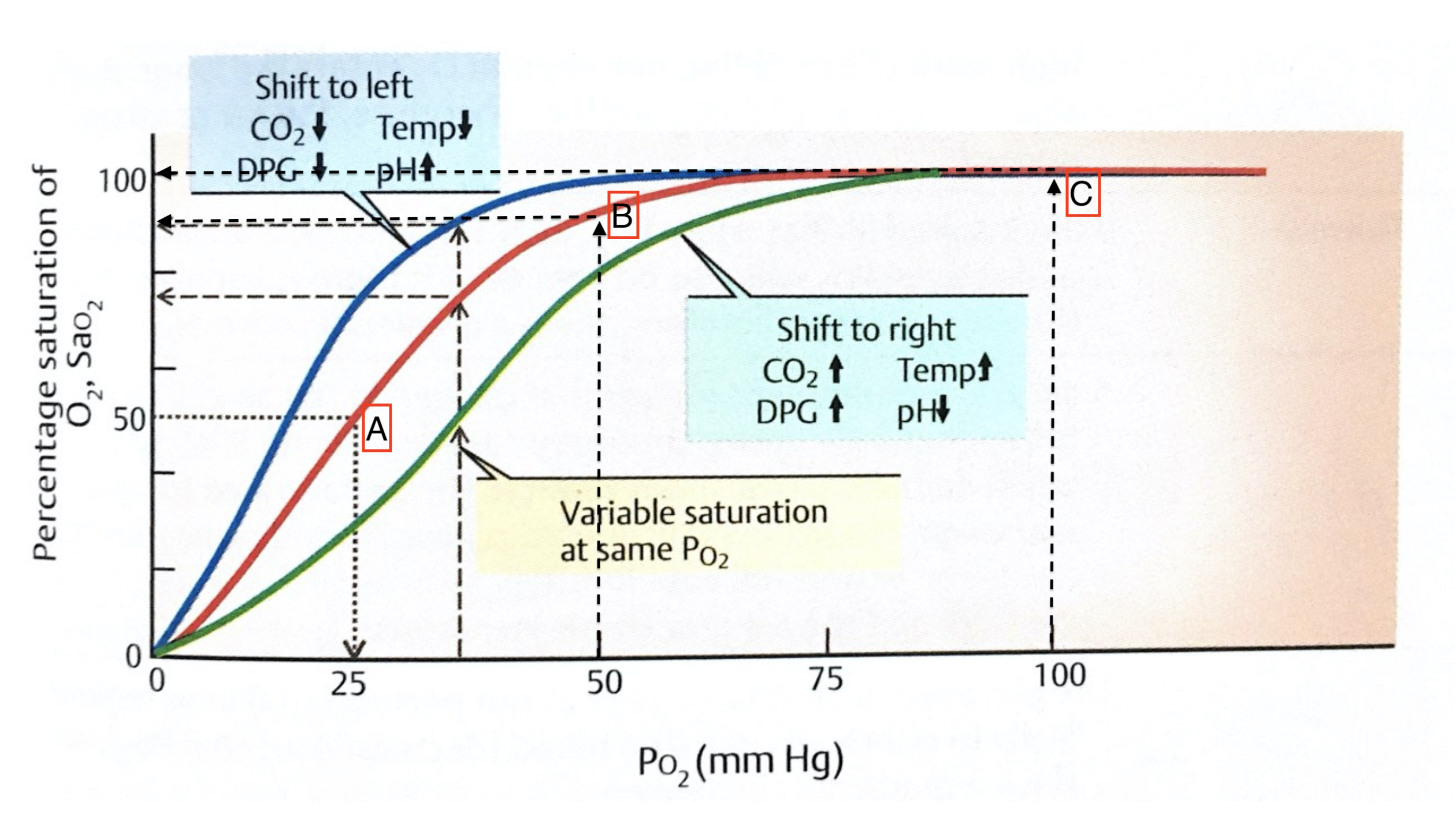
Normally the relationship of the blood in the lungs (horizontal axis) and the amount of the O2 in the red cell (vertical axis) is following the red line. When the amout of oxygen insired is 25mmhg the blood saturation is at 50% (A). The blood saturation is nearly 100% when room air is inhaled (C). Room air has PO2 of 75mmHg. Note that there is very little change in blood saturation (SaO2) by increasing the PO2 from 75 to 100 mmHg (the red line is horizontal between 75-100).
Another way to look at this: If you increase the PO2 from 25 to 50 (doubling) the Saturation goes from 50 (A) to nearly 85(B). Whereas increaseing the PO2 from 50 to 100 (doubling) only mober the Saturation from 85(B) to 100(C). This shows the efficiancy of system to be able to deliver the most amout of oxygen to the tissue even with the low level of oxygen present in the lungs.
As the Green and the Blue lines demosntrate the balance can change by changes in CO2, Acidity (PH), DPG and temperature.
COVID-19
When it comes to COVID-19 illness there may be a number of factors in play. Most patients with pre-existing conditions already have changes that may shift the curve to the right (high fever and high Co2). Furthermore, obesity, asthma and other conditions may decrease the ability to clear the lungs of secretions and mucus may contribute to decreased oxygenation. Additionally, there is significant inflammation associated with the chemicals released in COVID-19 (cytokines). These can cause devastating changes to the ability to exchange oxygen in the lungs.
Oxygenation in COVID-19 severely symptomatic patient can deprive oxygen from organ. This can progress to organ failure. One of the most common organ systems to fail is the kidneys which may require dialysis.
100% Fruit Juices and Risk of Cancer
April 16, 2020 8:54 pm
We have talked about the excess free calorie that is present with fruit juices. Now there is proven research article demonstrating the connection between surgary drinks and the increased risk of cancer. This study 
This study is significant for a number of reasons: It is a very large study with over a 100,000 subjects studied. Furthermore, it was specifically looking for association between nutrition and health.
The conclusion of this research article is self explanatory. Eliminating or cutting down high sugary drinks is an easy way of reducing cancer risk factors. The study also states that there were no identifiable association between the artificial sweeteners and cancer risks. However, this conclusion was not statistically significant. The relationship between sweeteners and cancer have been studied extensively in the past and we’ve shared several of them.
Symptoms of Coronavirus
April 15, 2020 8:10 pm
Covid-19 Pandemic and Obesity
April 12, 2020 7:44 pm
We have now seen several articles with data collection regarding patients with obesity and COVID-19 being at greater risk of hospitalization. We can look at metabolic syndrome associated with obesity as a risk factor also.
We have all been in physical isolation due to Covid-19 pandemic. The strategy of minimizing contact has worked. The data is clear when comparing information from states that instituted an aggressive containment plans compared to those who have not. This shows a sigifnicat flattening of the curve in California for example.
The CDC publishes the Morbidity and Mortality Weekle Report (MMWR) . The latest publushed summary (as of date of publucation of this blog) provides an insight to the risk factors of hospitalization.
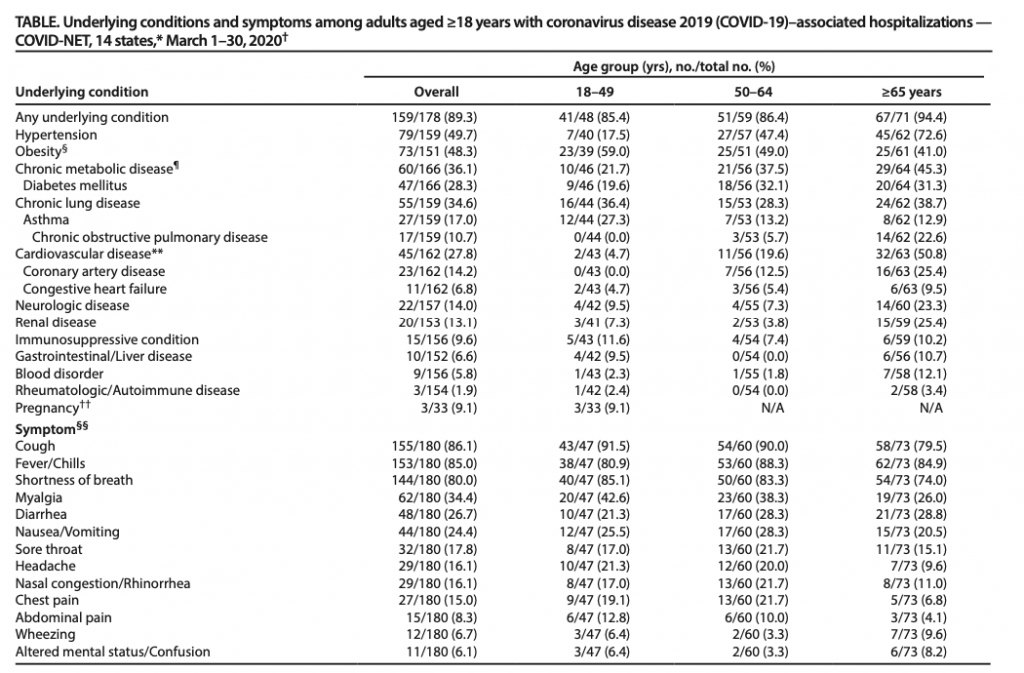 The above table outlines the underlying conditions of those hospitalized with Covid-19.
The above table outlines the underlying conditions of those hospitalized with Covid-19.
Concerning to see that a respiratory virus is more likely to hospitalize those with Obesity, Diabetes and hypertension at a higher rate than lung and pulmonary related conditions.
Let us recognize that this is only a summary collected data. Therefore, there are limitatation to making any assumption of conclusion based on this information.
With those limitation aknowldged, and relying on our obesity related comobidities, we can make a few conclusions:
Not surprising, Obesity as with other diseases, compounds Covid-19 exposure and infection. Diabates is also a risk factor. There are no indepth information available on the diabetic patients. There is now data showing superior outcome of diabetes resoultion with weight loss surgery compared ro medical treatment.
Diabetes and Weight Loss Surgery
April 06, 2020 5:51 am
The scientific literature is riddled with evidence pointing to the benefit of early metabolic surgery as a superior treatment, remission and possible cure option for diabetes. Unfortunately, the medical education, pharmaceutical companies, primary care healthcare delivery systems and third party payers (health insurance companies) have not caught up with the published data. The American Diabetes Association has changed their guidelines to reflected the benefit for combating diabetes with weight loss surgery.
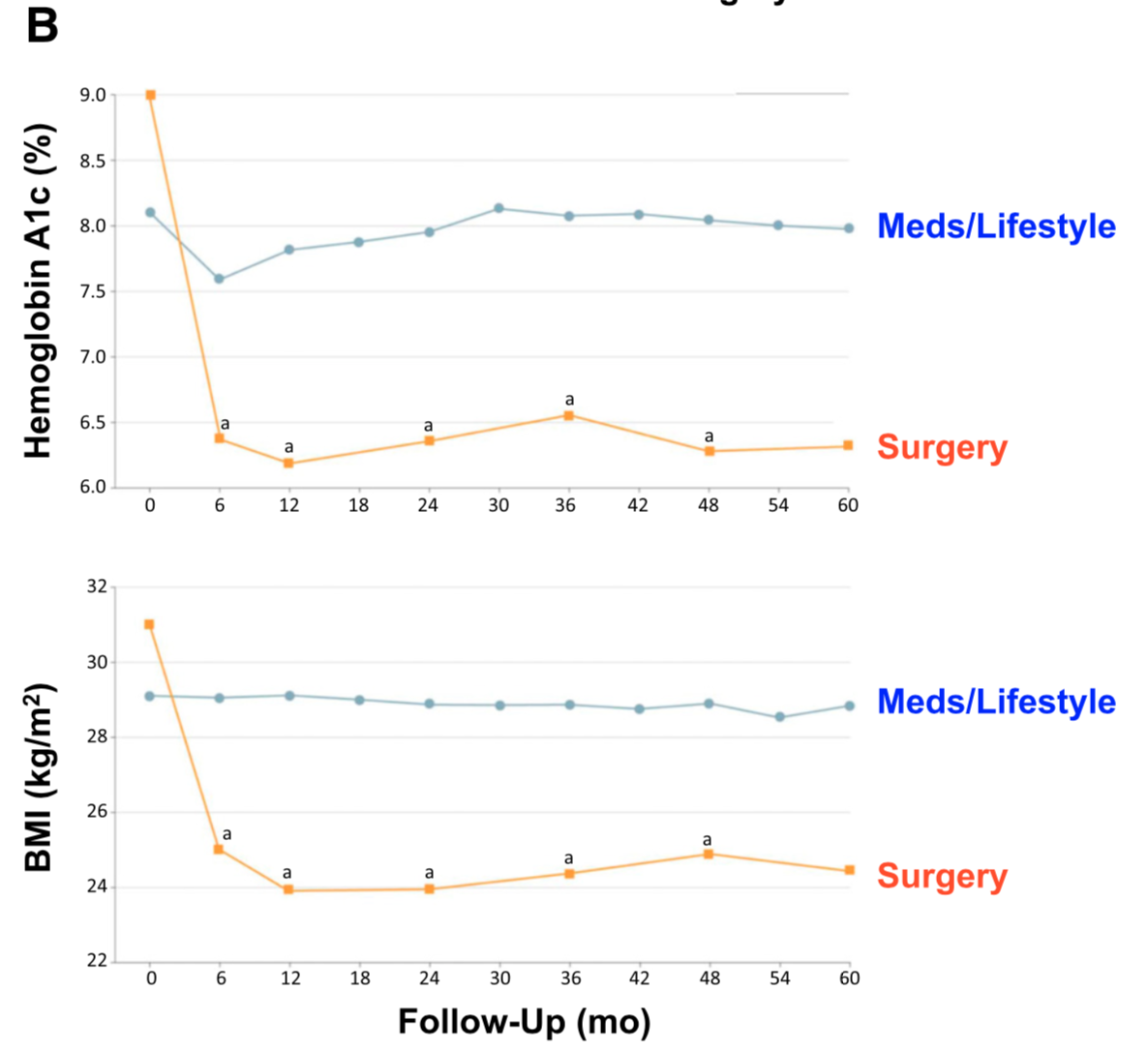
There is ample evidence of the superior outcome of surgery as a treatment option for diabetes when compared to medical managment. Cummings et.al, in a published article in Diabetes Care, showed sustained stabilization of the Hemoglobin A1C six years after surgery. In contrast, there was no significant changes noted in the non-surgical group.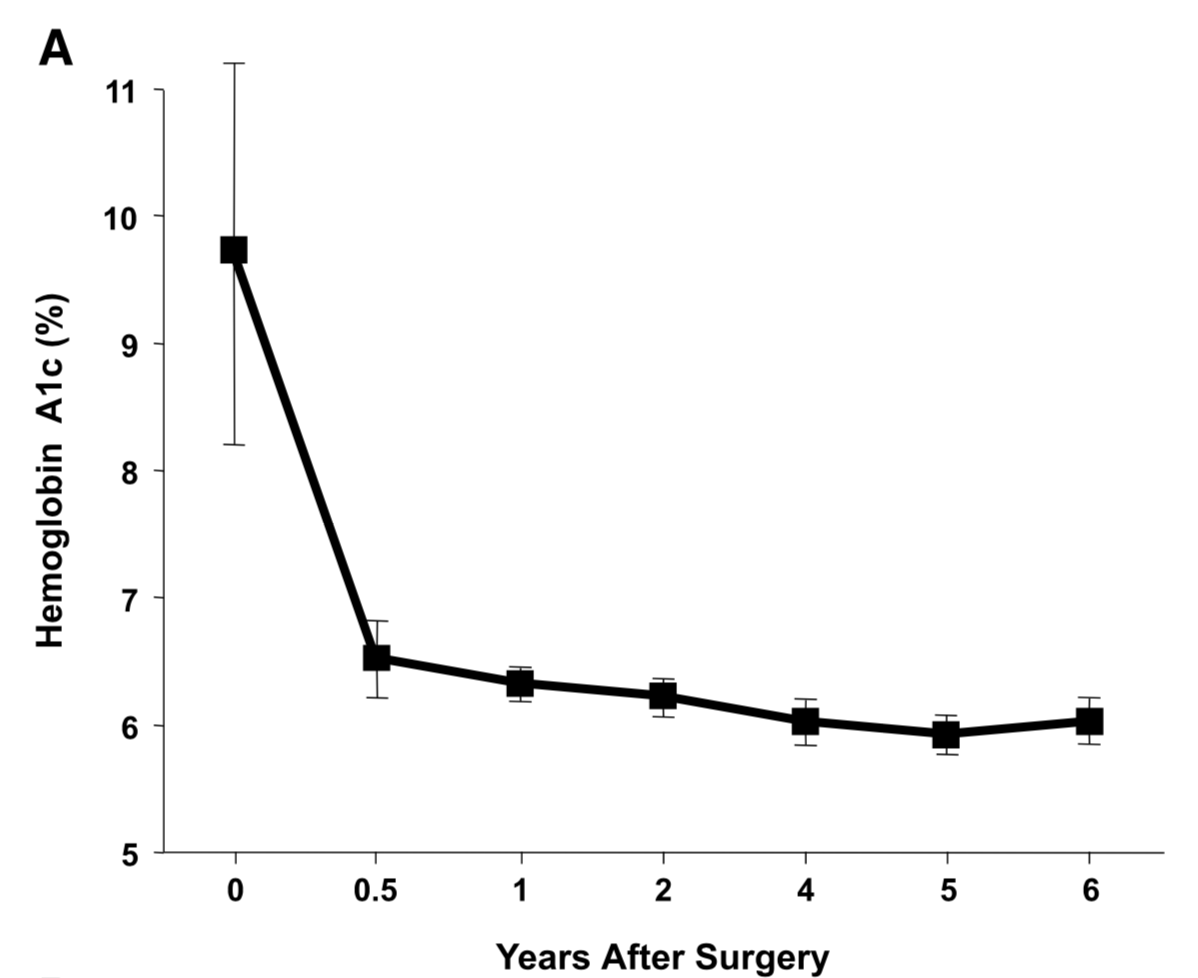
Jans et.al. , in November of 2019 showed that the patients who had NOT been on Insulin, and had metabolic surgery had the highest long term success for resolution and remission of the diabetes. This identifies that having a patient be proactive in their care by having metabolic surgery improves success rates.
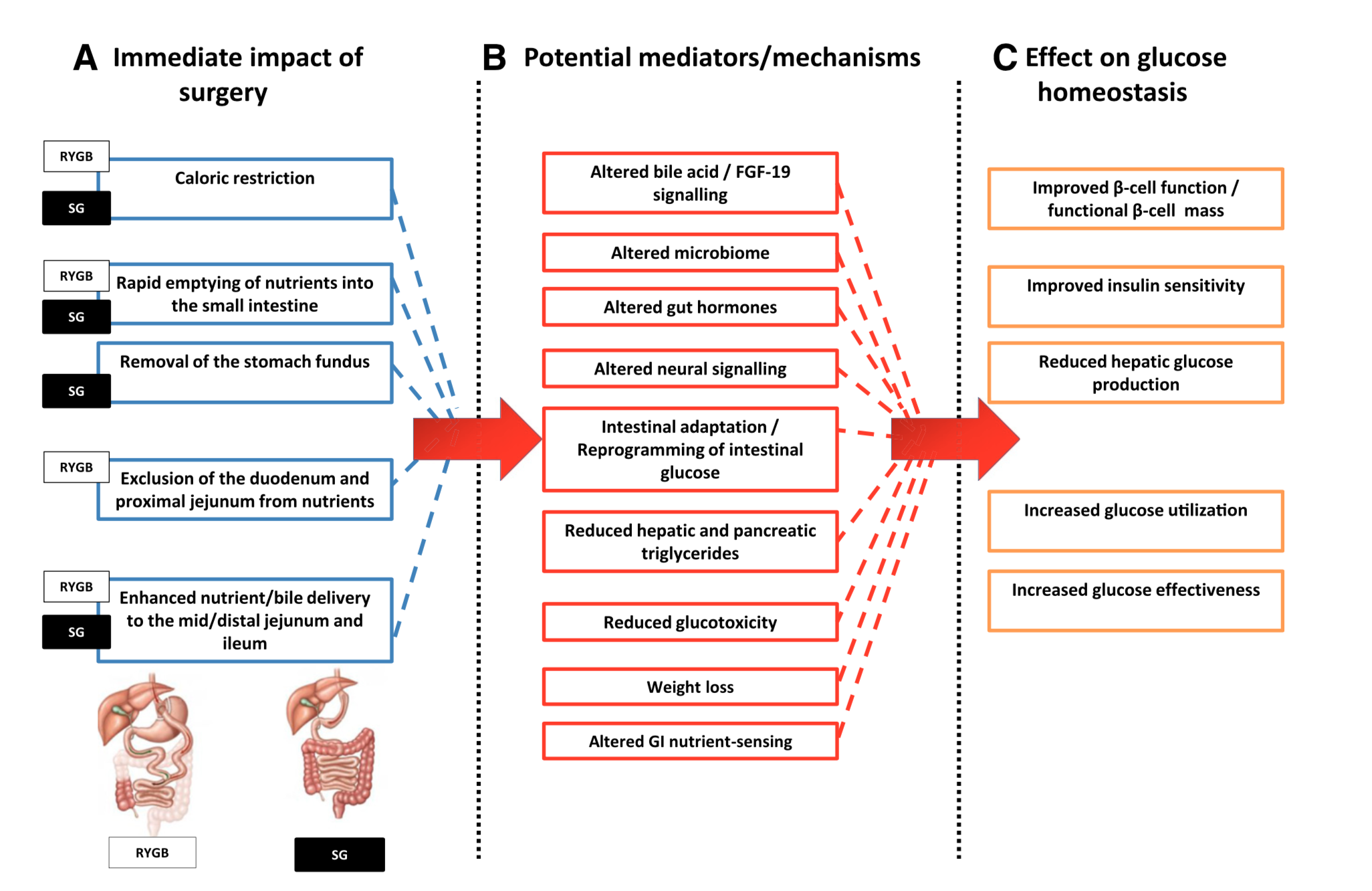
The exact mechanism by which the diabetes is resolved is unclear. The weight loss may play a role. There are numerous hormones and neuroendocrine modulators which control the complex metabolic pathways. Batterham et.al., in Diabetes Care (2016), published a summary overview of the possible mechanism involved in diabetes improvement following metabolic surgery.

There are a number of overlapping and sequential layers for possible reasons why diabetes resolves after weight loss/metabolic surgery. These may be directly related to surgery and the reduction of the calorie intake or absorption. It may also involve the neuroendocrine modulators.
What can be said definitively is that early surgical intervention is best and most likely the only permanent solution to type II diabetic resolution. There is no medical justification in not considering metabolic surgery in diabetic patients who may also have difficulty with meaning a BMI< 35.
Medication Absorption After Weight Loss Surgery
March 30, 2020 8:01 am
Weight loss surgical procedures, in one form or another, achieve the desired effect of weight loss by altering absorption of fat, protein, and carbohydrates. This results in decreased total absorption of required calories.
An unintended consequence is the altered absorption of medications. Frequently I am asked about the specific medication. Usually the answer is vague since the information is limited on specific medications. If the desired effect is not achieved, then it is probably not being absorbed well. Specially, if the same dose of the same medication working well before surgery.
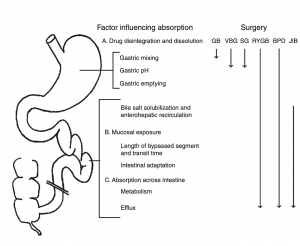
There is a summary article about the Theoretical absorption pattern of different weight loss surgical procedures.
Osteoporosis Medications
March 28, 2020 7:22 pm
There are a number of lectures, posting that we have done over the years on this topic. However the questions of osteoporosis medications and their benefits and risks comes up often.
The links are attached:
Here is an updated list of medication that I had previously published. I made some clarification to explain how the medications work. There are different classes of medications and the detail of the action and soda effects were described earlier at a blog post.
List of medications that effect bone health.
The table is obtained from https://www.nof.org site.
Pregnancy FileExclusive Member Content
March 28, 2020 9:08 am
Vitamin D Metabolism and Deficiency file
March 28, 2020 8:17 am
It’s important to understand Vitamin D metabolism and deficiency potential following weight loss surgery Vitamins after DS need to be followed via laboratory blood studies. There are basic vitamin needs but individual needs should be based on medical history, genetics, alimentary limb length, common channel length and other surgical and physiologic determinations. Vitamins after DS are a life long commitment as well as protein needs and hydration. Duodenal Switch is a malabsorptive procedure which requires at least yearly laboratory blood studies, daily vitamins/minerals, daily high protein and daily hydration intake. There is not an all in one vitamin that is adequate for a DS patient or tailored to your individual needs. (example: you may need more Vitamin D and less Vitamin A if you are taking a all-in-one vitamin you can’t get more of one and less of another vitamin)
DS patients are recommended to take Dry forms (water miscible form) of Vitamin A, D3, E, K due to the fat malabsorption after DS. Dry formulations by Biotech are processed so they can be absorbed by a water soluble method after the DS procedure. Vitamin D seems to be the vitamin that can become deficient the easiest, followed by Vitamin A. Take these vitamins away from dietary fat.
In some cases, patients may need injectable Vitamin A or D to improve vitamin levels.
Click the links to view the information below and within the comments of this file:
Vitamin D3 50 by Biotech: Amazon
directly from BioTech:
Many DS surgeon’s do not recommend Children’s vitamins or chewable vitamins unless there is a specific reason or need for them.
DS Surgeon Blog on Vitamin D:
Webinar on Vitamin D metabolism:
Medications that effect Bone health:
This does not constitute medical advice, diagnosis or prescribing. It is simply a compiled list of gathered information. If you are in doubt or have questions please contact your medical healthcare professional.