Sleeve Gastrectomy in Adolescent patients
September 23, 2020 5:44 am
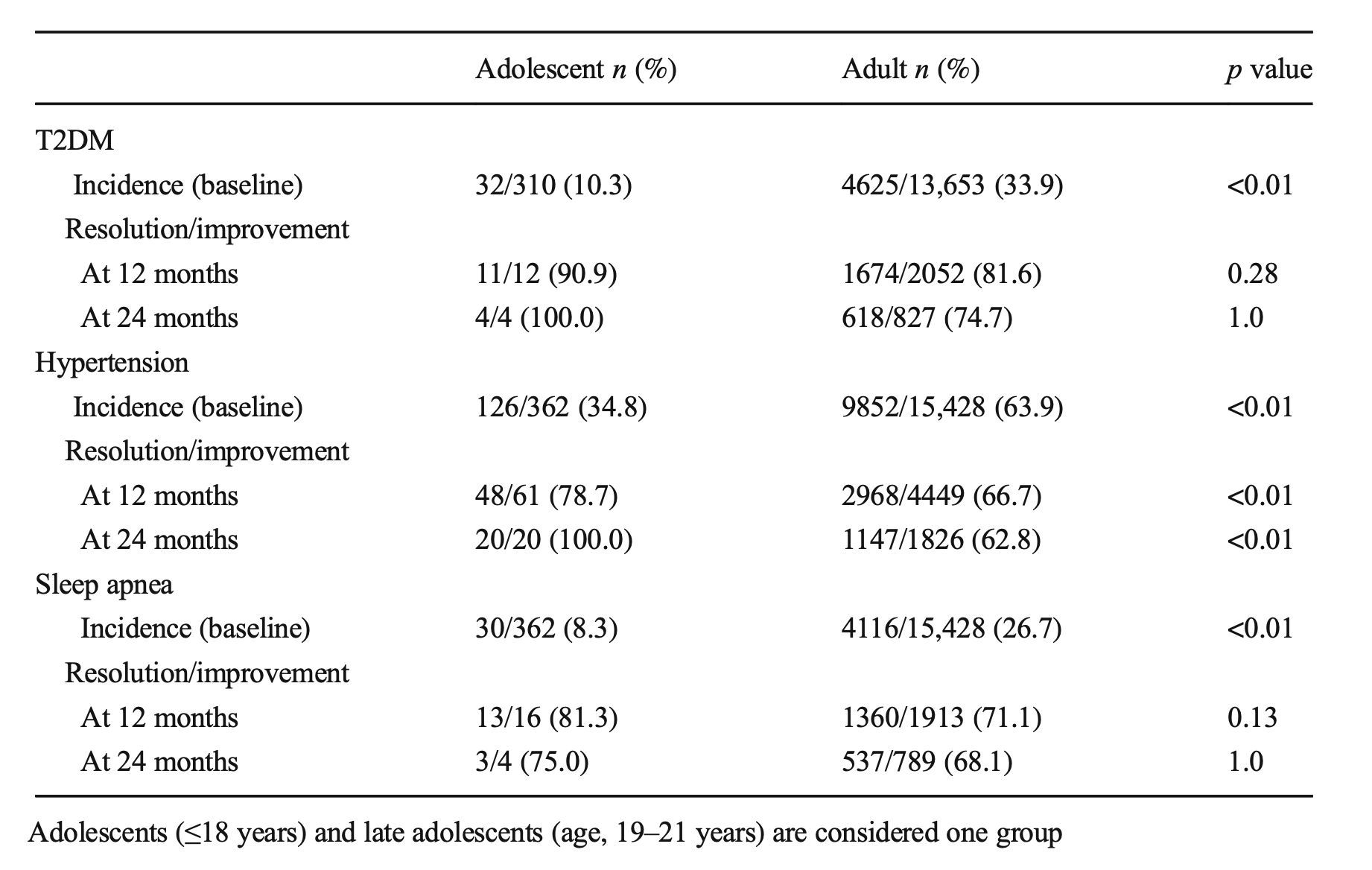 Sleep apnea resolved at the same rate. These early interventions can mean there may be lower long-term risk and associated conditions for these teens as they age.
A recent article was written from several adolescent weight loss surgical patients’ perspectives: This included their feelings of hope for their futures and health.
Sleep apnea resolved at the same rate. These early interventions can mean there may be lower long-term risk and associated conditions for these teens as they age.
A recent article was written from several adolescent weight loss surgical patients’ perspectives: This included their feelings of hope for their futures and health.
Zoom Group Meeting
September 21, 2020 7:10 am
We are excited to announce we will be having a Zoom group meeting Tuesday, September 22, 2020 at 7:00 PM PST. We hope to see you online!
Registration is required. Please follow the link to the meeting registration.
What is Corona Virus?
September 17, 2020 1:37 pm
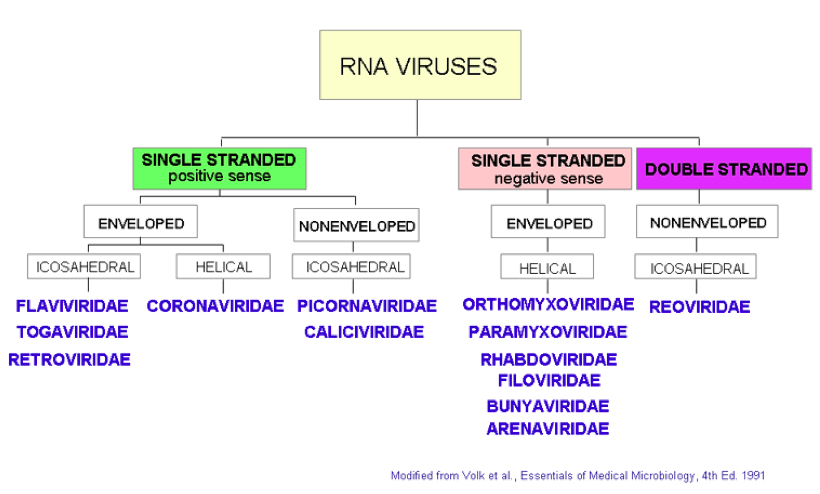 At a highly technical level Viruses are considered non-living materials. Viruses can not replicate and reproduce by themselves. Therfore, they need to attach themselves and penetrate a living organism to allow multiplication.
Double Stranded Viruses include smallpox, Chickenpox and Herpes simplex.
Single Strand Sositive Sense Virus in varies groups include HIV, and Corona Virus. Specifically, Corona virus is a Single Strand, Enveloped Helical Virus. The classifications of the viruses are based on their shape and the mechanism of attachment to the host cell.
There are differnt classification of virusrs described.
Viruses have cuased more death in the human history than any other diseases. However with vaccination, and public health policies we have been able to eliminate certain deadly viruses.
At a highly technical level Viruses are considered non-living materials. Viruses can not replicate and reproduce by themselves. Therfore, they need to attach themselves and penetrate a living organism to allow multiplication.
Double Stranded Viruses include smallpox, Chickenpox and Herpes simplex.
Single Strand Sositive Sense Virus in varies groups include HIV, and Corona Virus. Specifically, Corona virus is a Single Strand, Enveloped Helical Virus. The classifications of the viruses are based on their shape and the mechanism of attachment to the host cell.
There are differnt classification of virusrs described.
Viruses have cuased more death in the human history than any other diseases. However with vaccination, and public health policies we have been able to eliminate certain deadly viruses.
Duodenal Switch Post-op One year
August 28, 2020 1:12 pm

Will Weight Loss Surgery Resolve All Common Co-Morbid Conditions?
August 28, 2020 1:07 pm
 This is an article that I wrote for Obesity Help.
You can find the article at the following link.
This is an article that I wrote for Obesity Help.
You can find the article at the following link.
Covid-19 Mutation – Please physically distance and Wear Masks
August 18, 2020 1:16 pm
Introduction:
There is evidence emerging of Covid-19 mutation. This may explain the difference between the severity and intesity of the disease presented in the those geographical locations where the disease first.
Scientists from The Scripps Research Institute, Jupiter, Florida have identified changes in the Spike protein. This protein is used to bind the virus to host membranes. As we now know Florida is one of the few hot spots of the Covid-19 pandemic.
This has significant implications for the long term strategy needed to control transmission and manage resurrgence.
Until there is effective vaccination or effective treatment available for everyone, prevention by wearing face mask is the most efficient form to avoid transmistion.
Prevention:
The facts are that the most consistent effective preventive measures are wearing face masks and physical distancing.
There are those who may feel invincible and think that you will 1. either not get the disease or even if you get it it will 2-not affect your health. Lets first remind ourselves that wearing a mask is more to prevent passing the virus that getting it. We should all assume that someone that we come in contact with may already have it. Would you like them to breath the virus toward you ? This then brings the second issue: We do not know what the long term health effect of the virus is for those who develop significant symptoms and those who are asymtphomatic.
The unkown:
Let’s look at other viral infections that provide either no or minimal disease condition at the time of initial exposure only to result in long term health conditions that may result in death. These include hepatitis and HIV exposures and infections. Admitedly Coronavirus is a differnt family of virus. I am not suggesting that this will behave like other family of the viruses. We just do not have enough information to know what happens to those exposed to the virus (regardless of being asymptotic or not). Could the virus become dormant and over time result in organ injury (lung) like in the case of hepatitis (liver). Or make a home in our body and have recurrent debilitating infections and symptoms as it is seen with Varicella-zoster virus (VZV) which causes chickenpox and the time of the initial infection and makes residence in our body to reappear later on as herpes zoster (shingles). Will we need a new strain of vaccine every year similar to the flu vaccine?
That is the crux. We do not know because the COVID virus is new and we do not know the long term effects.
Vitamin D and COVID 19
June 13, 2020 4:40 pm
There has been extensive discussion on the importance of Vitamin D published over the last few years in regards to bone health, immune health and Calcium physiology. The importance of vitmain D and bone structure has been discussed extensively. It is also important in the absorption of Calcium. It further plays role in immune modulation.
What is new is the possible correlation of Vitamin D and COVID 19. Recently it is been shown that low vitamin D may increase the risk of a poor outcome with Covid-19 exposure and infection.
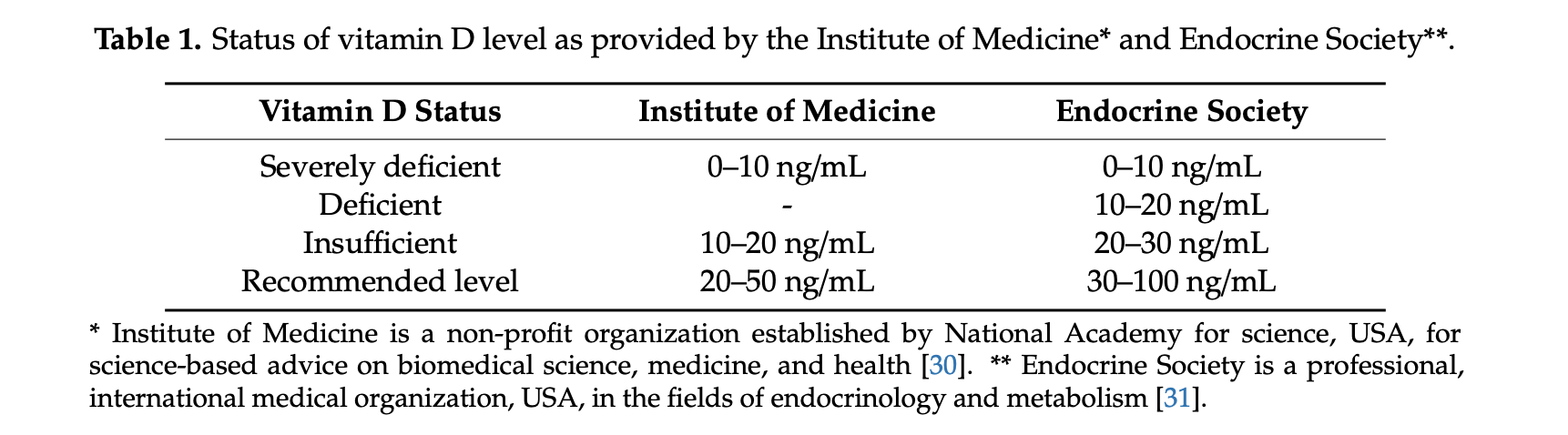
There are different standard recommendation for the Vitamin D levels.
In our practice we aim to maintain a Vitamin D level of 0ver 60 in post weight loss surgical patients.
There are a number of theories as to how the Vitamin D deficiency may play a role in this. An emerging observation is that low Vitamin D may cause abnormal and excessive blood clot formation. Mohammad et. al. in 2019 published a study on the association of low vitamin D and “…Pathogenesis of Thrombosis”
This pathologic blood clot formation in COVID-19 patients may explain the extensive lung injury and multi system organ failure in some patient. It is also one of the reason that some COVID-19 patients have loss limbs or appendages.
Please follow all supplement recommendations based on your laboratory studies and all COVID-19 recommendations. We would recommend frequent hand washing, surface cleaning, social distancing, and wearing face masks as the most basic precautions and increase precautions based on your health status.
Vitamin D and Covid -19
May 07, 2020 9:24 am
We are all aware of the many roles that Vitamin D plays in our bodies. This includes immune function in addition to all the regulatory roles that Vitamin D plays in several physiologic reactions. There may be a correlation of low Vitamin D and COVID-19 infection increasing death risk as looked at in research articles.
Covid -19 in a subset of patience causes significant lung injury. These patients require mechanical ventilation.
Previously reported publications have suggested a possible correlation between ace inhibitors and increased risk of pulmonary complications of Covid -19. Some researchers suspect that the Covid-19 may be able to enter lung cells by the ACE receptors.
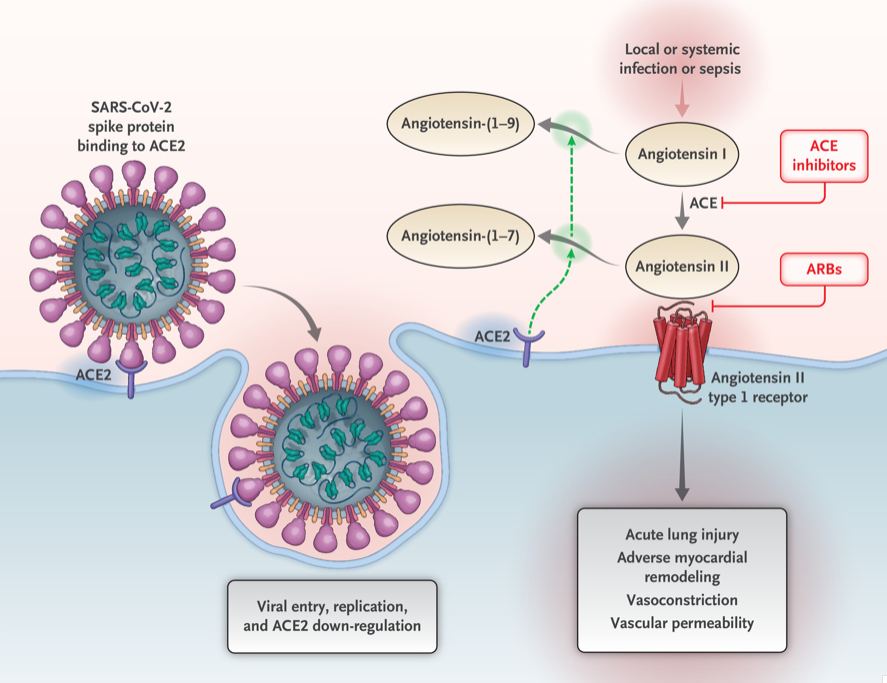
Vitamin D may positively implact the receptor ACE2. This study, report clear correlation between the high death rate with low vitamin D levels in Covid infected patients. There are limitation to this study that the attached abstract outlines.
Our take home message would be to please make sure you have updated labs and that you are all taking the recommended Vitamin D based on your surgical anatomy and laboratory values, not just an average non-bariatric person recommended dose.
https://www.dssurgery.com/wp-content/uploads/2020/05/manuscript.pdf
Copper Metabolims And Weight Loss Surgery
May 01, 2020 12:31 am
Written By: Osheen Abnous, Maria Vardapetyan, Eric Baghdasaryan
Copper is an essential element to all organisms, and it is a contributor in several enzymes vital to the function of hematopoietic, vascular, and skeletal tissues, as well as the structure and function of the nervous system.
As a crucial metal, copper plays an important role in chemical reactions throughout the human body; this includes the central nervous system. Enzymes are substances that facilitate chemical reactions. There are many copper-dependent reactions in the human body. In humans, the major site of absorption of dietary copper is still unclear. Copper in humans is absorbed in the proximal small bowel, duodenum, and ileum. This is after it has passed the acidic environment of the stomach.
Copper deficiency can be caused by malnutrition, prematurity, parenteral or enteral feeding without copper supplementation, gastrectomy, and excessive zinc therapy. The common causes of copper deficiency have been zinc supplementation, and changes to the PH (acidity) of the stomach. This can be the result of the alteration of the stomach anatomy, and by chronic acid suppression by proton pump inhibitors (antacids), and similar medications. Physicians need to be alert with patients who show signs of copper deficiency or are at a high risk of developing a copper deficiency.
It is important to raise greater awareness about copper deficiency because there is a growing number of patients undergoing surgeries for obesity, as the occurrence of copper deficiency will increase in the future.
Studies of patients who have had weight loss surgery in the past experience common symptoms such as pain involving the feet, gait abnormality (unusual walking), lower limb weakness, and recurrent falls. Common lab results include unusually low serum copper and serum ceruloplasmin levels. In some cases, elevated zinc levels are also present. Treatment includes cupric sulfate infusion until normal copper levels are reached, which then need to be maintained for the future. Vitamin B-12 deficiency has also been reported as a possible cause of myelopathy, which is a nervous system disorder that affects the spinal cord. As stated earlier, neurological damages are often irreversible and cause permanent damage to patients. Early diagnosis from physicians is crucial for patients who have undergone gastric bypass surgery, and the sooner they are diagnosed, the less permanent damage the patient will endure.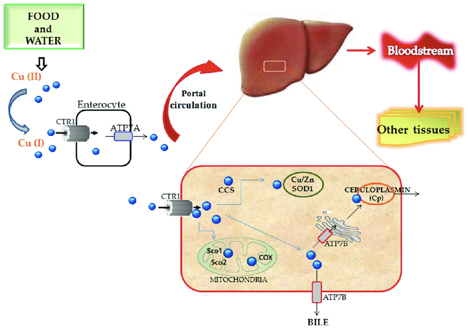
Case Discussions:
A 49-year-old woman had gastric bypass surgery for obesity 24 years age. She presetend with increasing lower limb stiffness and numbness. Additionally she reported tingling of the feet. As her pain continued to increase, she began using a walker, and her symptoms continued to worsen. After undergoing a neurological examination, results showed that the patient had increased lower limb tone and an absent perception of vibration at the toes and ankles. Laboratory results showed that the patient had copper levels barely detectable. This included serum copper and serum ceruloplasmin levels. In addition, the patient had reduced serum carotene (vitamin A) levels.
The patient received cupric sulfate intravenously daily through an 8-week period. After each daily infusion of cupric sulfate, the patient reported to have slight decreases in numbness and an increased tingling sensation. After the 8-week period, lab results showed that serum copper levels were normal and are needed to be maintained. Her night blindness was corrected by vitamin A injections.
In another case, a 53-year-old woman had symptoms of abnormal gait (abnormal walking) and anemia (lack of healthy red blood cells), and was seen for evaluation. The patient complained of pain in the lower legs, which would worsen over time and move up towards her thighs. As her ability to walk continued to worsen, the patient resorted to using a wheelchair. Her medical history consisted of an RYGB surgery for obesity. The only significant supplementation she received was 1000 μg vitamin B12 subcutaneously for several years. She had absent positional and vibratory sensation in the lower extremities to the knee. In addition, touch sensation was decreased. Laboratory examination revealed an elevated serum zinc level, and extremely low serum copper and ceruloplasmin levels.
For treatment, the patient received intravenous copper over a 6-day period, was discharged home, and then received weekly intravenous copper infusions thereafter. After a month of receiving intravenous copper, serum copper levels returned to normal. In addition, the patient’s pain in the lower leg improved, but vibratory sensation remained absent in the same area. Four months after being discharged from the hospital, the patient began walking with a cane.
Fat Soluble Vitamins
April 26, 2020 10:20 am
Written By: Maria Vardapetyan, Eric Baghdasaryan, Osheen Abnous
Vitamins are chemicals that facilitate many processes in the human body such as blood clot formation, good vision, fight infections etc. There are two classes of vitamins. Water soluble vitamins and fat soluble vitamins. Water soluble vitamins dissolve in water. This makes it possible for them to be absorbed through all mucous membranes. Fat soluble vitamins on the other hand do not dissolve or pass through mucous membranes. Fat-soluble vitamins are absorbed in the intestine along with fats in the diet. These vitamins have the ability to be stored in the fat tissues of the human body. Water-soluble vitamins are not stored in the body and have to be taken in daily with the food and dietary supplements. Solubility of a vitamin is not a function of its physical state. There are fat soluble vitamins that have a liquid form and almost all of the water soluble vitamins come in form of pills or powders.
In this article, we are going to focus on fat soluble vitamins. They are all complex molecules made of carbon, hydrogen, and oxygen in different arrangements (see figures 1, 2, 3 and 4). These fat soluble vitamins are vitamin A, D, E and K.
Vitamin A
Vitamin A has a major role in vision, immune function, cell growth, and maintenance of organs such as heart, kidneys, lungs, etc. It plays a pivotal role in the health of our eyes, specifically the retina1. Rhodopsin protein, a major protein that has the leading role in the process of vision, is found in the retina where it allows us to perceive light. This protein requires vitamin A to function properly. Without vitamin A, rhodopsin cannot sense light and thus cannot initiate the process by which vision occurs.
Figure 1: Chemical structure of Vitamin A molecule
Vitamin D
Vitamin D regulates different chemical reactions that are associated with bones, muscles, and the immune system. The simplified way it does this regulation is it helps absorb calcium from dietary nutrients which in turn strengthens the bones, helps neurons exchange signals to move muscles and helps the immune system to fight against viruses and bacteria2.
Figure 2: Chemical structure of Vitamin D molecule
Vitamin E
Vitamin E acts as an antioxidant. Antioxidants are naturally occurring chemicals that neutralize toxic byproducts of many chemical reactions in the human body. When food is consumed and digested, the human body converts it into energy. As a result of metabolism free radicals (toxic byproducts) are formed and are neutralized with the help of vitamin E. In addition, free radicals are also in the environment. Furthermore, vitamin E stimulates the immune system to fight against bacteria and viruses3.
Figure 3: Chemical structure of Vitamin E molecule
Vitamin K
Vitamin K can be obtained from food and dietary supplements. There are two forms of vitamin K: phylloquinone (Vitamin K1), which is found in spinach, kale and other greens and menaquinone-4 (Vitamin K2), which is found in animal products. Vitamin K1 is involved in blood clotting, and Vitamin K2 is involved in bone tissue building. Vitamin K1 is the main Vitamin K in human diet (75-90% of all vitamin K consumed), however, it is poorly absorbed in the body4,5.
Figure 4: Chemical structures of Vitamin K1 and K2 molecules
Absorption of fat soluble vitamins
Polarity describes the inherent charge(positive or negative) or lack of charge for any given substance or molecule. Molecules that are charged are referred to as “polar”, while those that lack charge are “nonpolar”. When discussing solubility, it is important to remember the phrase “like dissolves like”. That means polar (charged) substances like to interact with a polar environment like water, since water contains a slight negative charge. Hence, charged substances are water-soluble. Nonpolar substances on the other hand readily interact with nonpolar environments such as fat, which contains no charge. Therefore, molecules that lack a charge such as vitamins A, D, E, and K are referred to as fat soluble.
Due to their water fearing nature, these fat soluble vitamins cannot simply be absorbed directly into the bloodstream (which is mostly water) like the sugars and amino acids in our diet. As their name suggests, these fat soluble vitamins like to be embedded in fatty droplets, which facilitate their absorption in the following way. Fat soluble vitamins group together with other fat molecules to form fatty droplets, effectively reducing the amount of interaction with the watery environment of the intestines. Therefore, without an adequate amount of fat in your diet, your body is unable to effectively absorb these fat-soluble vitamins. This may be true in an intact anatomy, however, post weight loss surgical patients can not increase their fat soluble vitamin levels by increasing their fat intake. This is due to the fact that a high fat diet causes excessive bowel movement which in turn washes away any vitamins taken by mouth. DS limits fat absorption (thus the great weight loss) which can cause vitamin A and D deficiency that can not be easily corrected with oral supplementation.
As mentioned before, fat soluble vitamins are hydrophobic and nonpolar, which means they are also fat loving or lipophilic. Excess fat soluble vitamins can be stored in the liver and fat tissue. Therefore, these vitamins do not need to be eaten every single day since stores of these vitamins can sustain a person for some time. It may take several weeks or months for our body to deplete these stores of fat soluble vitamins which is why it generally takes a longer amount of time for fat soluble vitamin deficiencies to manifest themselves. The ability to store these fat soluble vitamins in tissues can also lead to vitamin toxicity – marked by an excess of vitamin stores in our body.
Clinical manifestations of A, D, E, K deficiency
| Vitamin | Clinical Deficiency manifestations |
| Vitamin A | Vision Problems
Dryness of the eye |
| Vitamin D | Softening and weakening of the bones
Bone shape distortion Bowed legs (generally in children) Hypocalcemia |
| Vitamin E | Damage to red blood cells
Tissue/organ damage due to inability to supply enough blood Vision problems Nervous tissue malfunction |
| Vitamin K1 | Excessive bruising
Increased bleeding time Small blood clots under nails Increased bleeding in mucous membrane |
| Vitamin K2 | Weak bones
Increased plaque deposits along gumline Arterial calcification |
References
- Office of Dietary Supplements – Vitamin A. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminA-HealthProfessional/#. Accessed April 26, 2020.
- Office of Dietary Supplements – Vitamin D. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminD-Consumer/. Accessed April 26, 2020.
- Office of Dietary Supplements – Vitamin E. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminE-Consumer/. Accessed April 26, 2020.
- Vitamin K. The Nutrition Source. https://www.hsph.harvard.edu/nutritionsource/vitamin-k/. Published July 2, 2019. Accessed April 26, 2020.
- Beulens JWJ, Booth SL, van den Heuvel EGHM, Stoecklin E, Baka A, Vermeer C. The role of menaquinones (vitamin K₂) in human health. The British journal of nutrition. https://www.ncbi.nlm.nih.gov/pubmed/23590754. Published October 2013. Accessed April 26, 2020.


