Tag: revisional weight loss surgery
Success Story: Hasmik
January 13, 2016 2:47 pm
Failed Band: My earliest memory of feeling ashamed of being “too heavy” is from kindergarten. For over 30+ years I have struggled with gaining weight, trying to lose weight, or going mad maintaining my weight. There is no shortcut that does not come back to bite you in the butt. There is no diet that effectively changes you permanently. For me exercise is a mindful struggle I sometimes successfully commit to over small periods of time.
I was desperate and ready for a real change. I wanted a genuine difference in the way I consumed and related to food and decided the lap band was the way to go. It was marketed as a “non intrusive, non permanent, easily reversible weight loss tool” and that is EXACTLY what I thought I needed and wanted. I was so very wrong, after my surgery I was considered a “success”. In fact up until the removal of my second slipped failed band, esophagus damage, and poor nutrition; I was considered a success. I look back and think how troubling this was/is. How very damaging to the person struggling and dealing with weight issues. Truly, it messed with my mind and my ability to speak up, admit to myself and out loud the band was NOT working for me. In fact, if I’m completely truthful, it was dangerous and turned me into a residue of the person I once was. I was not able to eat comfortably or eat out any place I happen to be. With the Band, I would need to consider how long I was going to be away from home because I could only eat small bites in small quantities to ensure I did not get stuck or worse vomit what I put inside my mouth. Yes, I had lost almost 100 lbs, but I had given my quality of life as payment. My guilt ensured I would never speak up or complain since I felt “fortunate” and grateful to have had this second chance at life. In my mind, speaking up meant possibly losing the tool (lap band) that allowed me to change my life and reality. Because for the first time in memory, I was the same weight at the start, middle, and end of the year. I did not have to buy different sizes of clothing or underclothing. I could predict what I might wear since my size was stable and my clothes fit. The reality is and was far from this corrupted self truth. I was unhealthy with the restrictive nature of how the lap band worked. In fact my band slipped twice after a severe stomach virus. I later learned of many other symptoms I was making excuses for and quite frankly straight out ignored.
I met Dr. Keshishian (Dr. K) at my lowest weight and at the lowest point in my health. I finally realized, the lap band needed to come out after it had slipped again. It was clear I needed a doctor who would be straight with me and cared for my health and not his/her “success” rates and have the expertise to deal with my failed band. I researched and called several bariatric surgeons then attempted to make appointments with each to discuss the urgent band removal surgery I needed (not as simple as you would think). I was also hopeful I might have the option to undergo the bariatric sleeve surgery because I knew I would not be able to keep my weight under control on my own. I was unwilling to undergo the emotional and mental torment of gaining and losing weight for the rest of my days. I succeeded in making three appointments and truthfully after meeting and speaking to Dr. K and his office staff I canceled them immediately. Let me start with the staff as that REALLY is important; they help you feel comfortable with the doctor, the procedure, and overall experience. They represent and reflect how the doctor you’re about to see will treat his patients. The expected standard within Dr. Keshishian’s office immediately made me feel like I called the right place. I was taken by the knowledgable, kind tone and efficient manner in which they requested the necessary information to effectively help me get from the starting point to the end goal. When I got to my appointment, Dr. Keshishian BLEW MY MIND. He not only presented himself as an approachable person I immediately felt at ease with but also reveal my concerns and questions. He treated me like a person. This may sound strange but this doctor made me feel like a human being with real concerns. He listened to me, asked questions rather than talked at me, and explained how and what was happening to my body and mind. He spent 3 hours with me to answer all my questions (even if I repeated them), draw diagrams, show me video to better help me understand what was happening, and then just sat with me while I cried for a moment. I cried because my 30+ years journey of ups and downs, crazy and insanity finally led me to the door of a man who understood and knew how to help without judgment. WHICH DOCTOR DOES THIS! None that I know.
My life post surgery is what I always hoped it would be. I am able to eat vegetables, leafy greens, fruit, grains and basically a well rounded diet. What’s amazing is that I naturally do not crave sweets, heavy creamy dressings, sauces and fill up quickly. There is after all a difference between the restriction of a lap band and the feeling of being full with the sleeve which Dr. K patiently explained. Today I am able to go any where, at any time, enjoy the moment and the company rather than worry about what I’m not able to consume. My days of scanning to locate the nearest bathroom in case I need to dash to it are over.
As I write this today, I feel like a real person, not some transient hoping to savor my life at glimpses. I am a person that is balanced in my heart with the average person’s anxiety and mindful eating habits. The sleeve is not a magic end to weight gain, it does give you the fighting chance to make choices in life leading up to results you’re willing to work for.
~ Grateful and Mindful, Hasmik (September 2015 Sleeve Op Patient)
2015 ASMBS Summary
November 11, 2015 7:31 am
The 2015 ASMBS meeting was held November 2-6, 2015. It was combined with TOS (The Obesity Society) and had more than 5,600 attendees from all over the world in every aspect of obesity treatment. There were some interesting additions and deletions from this meeting compared to the past.
The one sentence that comes to my mind is “I told you so”.
One important addition was a DS course for Surgeons and Allied Health. This was very exciting, except the content and questions seemed to gravitate to SADI/SIPS/Loop rather than DS. Dr. Cottam was one of the moderators of the course. It seems that they have found the value in preserving the pyloric valve. It was clear that the discussion was driven by the need to come legitimize the single anastomosis procedures at this early stage with almost no data to prove long term outcome. With many of the Vertical Sleeve Gastrectomies having re-gain and the they are looking for a surgery that the “masses” can perform. This was actually the term used by one of the presenters, implying that the duodenal switch needed to be simplified so that all surgeons, those who have pushed all other procedures can not offer Duodenal Switch to their patients with less than desirable outcome. Several surgeons also voiced their concern and dissatisfaction with the issues and complication of the RNY and want an alternative. There was much discussion regarding SADI/SIPS/Loop being investigational and that it shouldn’t be as it is a Sleeve Gastrectomy with a Billroth II. Dr. Roslin and Dr. Cottam discussed their SIPS nomenclature saying they wanted to stay away from something that had Ileostomy, suggesting bowel issues, or the word “SAD”i due to negative connotations. The point to be made is that the SADI and SIPS and the loop are all the same. I have also noticed other surgeons using SADS (Single Anastomosis Duodenal Switch). There is a great deal of industry behind these procedures and many surgeons being trained in courses funded by industry. One surgeon stood up and informed the entire course that they need to be clear with their patients about the surgery they are performing, as he had been in Bariatric chat rooms and there is upset within the community about SADI/SIPS/Loop being toted as “the same or similar to Duodenal Switch”.
There was also presenter who said “We are doing something new about every five years.” No, “we” are not. Some of us have stood by the surgery and techniques with the best long term outcomes and not gone with every “new” thing out there. The process of Duodenal Switch may have changes, open Vs. Lap, drains, location of incisions, post operative care and stay, but the tested procedure with the best outcome has been the duodenal switch operation and not the shortcut versions. Although, those of us that are standing by long term results seems to be in the minority. Why do I stand by Duodenal Switch? Because it works, when done correctly by making the length of the bowel proportional to the patient total bowel length, and height, and not just cookie cutter length for all patients, with the right follow-up, patient education, vitamin and mineral regime and eating habits.
A new addition was the Gastric Balloon, which in the research presented had a 60-70% re-gain rate and a no more than 10-15% weight loss one year only. This data represents more than 70% weight regain when the balloon is taken out. The Gastric Balloons can be left in between 4-6 months depending on the brand or type of balloon. The Gastric Balloon is not new to the Bariatrics and was first introduced in 1985. After 20 years and 3,608 patients the results were and average of 17.6% excess weight loss. It seems that we are re-gurgiating old procedures. There are many new medications that were front and center in this meeting.
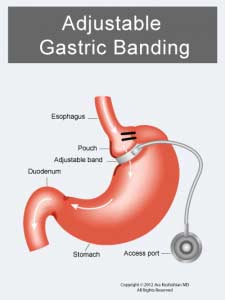
The Adjustable Gastric Bands were missing from the exhibit hall this year. It is my hope and feeling from the other attendees that we may be seeing the era of the Adjustable Gastric Band being placed in patients come to an end. Although there are some still holding out that there are some patients that can do well with the Band.
Attending the 2015 ASMBS meeting this year, as it has every year, only reemphasized the importance of avoiding what has become the norm of chasing a simple solution that is fashionable and easy now. We stay convinced that the duodenal switch operation with the common channel and the alimentary length measured as a percentage of the total length is by far the best procedure with the proven track record. The patient should avoid the temptation of settling for an unproven procedure or device, because if history holds true, there will be a need for revision surgeries in the future.
Revision of a Sleeve Gastrectomy or RNY
August 31, 2015 6:32 am
These are examples of two types of patients referred to us for revision surgery.
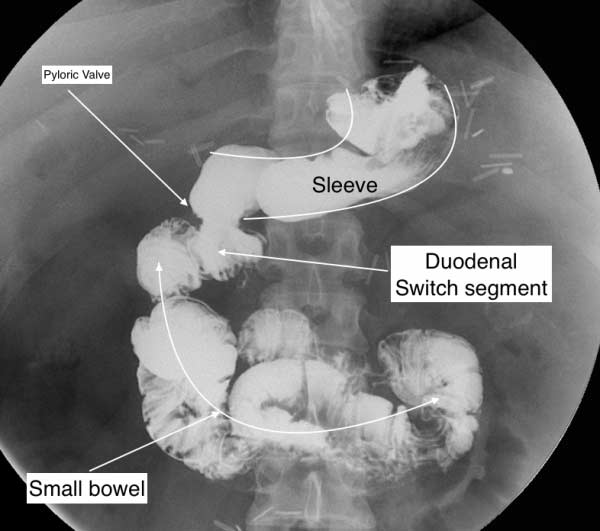
The first example is a gastric bypass that we revise to the duodenal switch operation. The upper GI series after the revision, shows a “banana shaped” stomach, the pyloric valve and the duodo-ilesotomy anatomosis component of the duodenal switch.
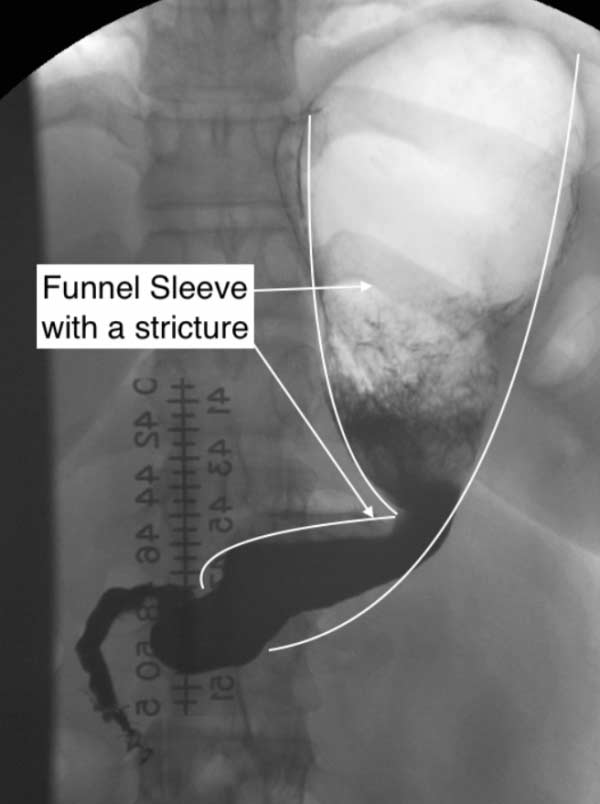
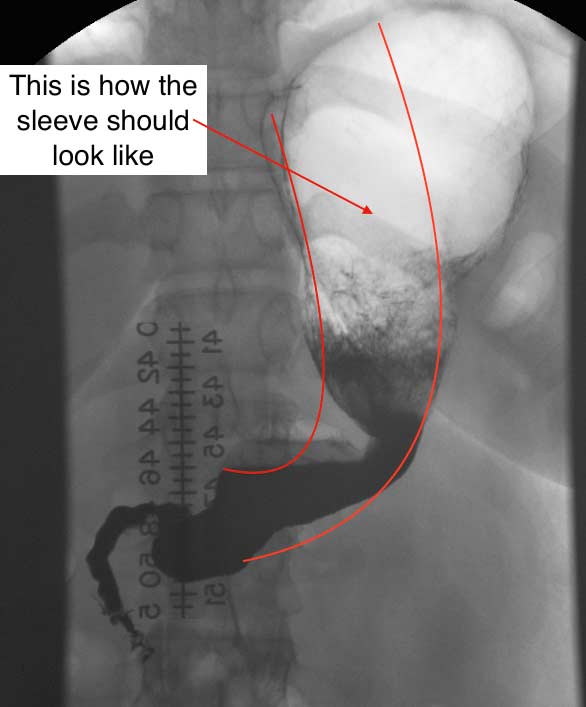
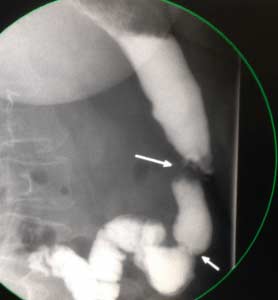
The second example, images noted below, is that of a sleeve revised to the duodenal switch – both operations done at different institution. Note how the stomach is not a “banana shaped” and more like a funnel with a narrowing at the bottom of the stomach- a stricture.
Surgical Treatment of Gastric Fistula
August 05, 2015 7:45 pm
Iron Deficiency & Anemia July 15, 2015 Webinar RecordingExclusive Member Content
July 16, 2015 1:52 pm
Vena Cava Filter
July 06, 2015 7:09 am
Example of a Vena Cava Filter Video:
Shared Success- Whitney a RNY to DS revision
June 09, 2015 7:43 am
I was always the big girl, pleasingly plump, chubby. I was put on my first diet at age 12. By the time I graduated High School I had yo-yoed up to 200 pounds at College graduation I was up to close to 300 pounds. In 2002 I had RNY Gastric Bypass surgery. I was 39 and weighted 280 pounds. I was told it was the Gold Standard. The Band was still considered experimental and the Duodenal Switch was never mentioned as an option. In fact, I did not even know it existed.
I lost 110 pounds and was considered a WLS success. I did not have any food restrictions and I felt great and maintained the loss for five years. Then I started to slowly gain weight. In little under 5 years I gained 70 pounds. I developed Dumping Syndrome and my Stoma was stretched out. I joined Weight Watchers and lost 5 pounds in a year. Nothing worked. I developed ulcers, osteoarthritis, planter fasciitis and could barley walk a couple of blocks without pain. I was miserable. I felt like a failure
In 2012 started to research surgical options. A local surgeon wanted to “revamp” my already tiny stomach, put a band around my stoma, and “clean up my intestines”. I asked about revision to Duodenal Switch and was strongly discouraged, but I wasn’t going to settle because that was what he was only capable of doing.
I wanted the best. I wanted long term success. So I travelled from Northern CA to Southern CA for a consult with Dr. Keshishian. The only choice for me was to revise to DS. In December of 2012, I had revision surgery of my RNY to Duodenal Switch. One week after surgery, still in the hospital, I went in for a second surgery. Dr. Keshishian found a small leak. I spent an additional two weeks in the hospital. My experience was not the norm and a leak can happen in any surgery involving the stomach.
Recovery was slow but steady. The first 2 weeks Dr. Keshishian called me every three days to make sure I was doing ok. I still have his cell number in my phone. I was back to work 14 weeks after surgery. I could have gone back sooner.
Over the past year I have lost 115 pounds. My BMI is 20, and I feel great. I have my life back. All pre-op issues have been resolved and I am going to start training for a 5K.
My advice for anyone contemplating Weight Loss Surgery is to research all of the options available. Do not settle for a substandard surgery. Get a second or even third opinion. It’s not a decision to be taken lightly. It’s your life fight for it!
Whitney B.
Stricture with Lap Band
May 31, 2015 6:44 am
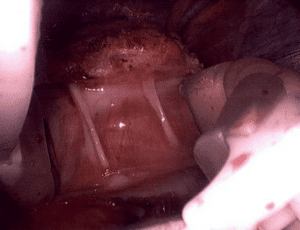
One of the most common findings with patients seeking revision of the Lap band is the persistent and continuos nausea, vomiting and reflux, even though the band is emptied. The typical presentation is that of a patient who had an adjustable gastric band placed and adjusted. When the weight loss stops any attempt to adjust and tighten the band results in reflux, nausea and vomiting. Unfortunately, there is lack of recognition that even when the band is completely empty, and even if removed, then a patient can still have the symptoms present, if the scar capsule that forms between the band and the tissue is not removed.
It is critical that when a Lap band is removed that time is spent excising the capsule that is present to allow for the tissue beneath the band to return to its normal caliber.
Note in these images how with the Lap band completely open the tissue underneath is “restricted” by the capsule that has formed under the band. In this case the capsule was also excised and removed along with the band.
Rebanding- A Bad Idea In My Opinion
May 12, 2015 3:42 pm
There is a wide discrepancy of outcomes for patients who have decided to have weight loss surgery and are experiencing different weight loss, regain and complications primary related to their choice of the procedure. In our practice we see quite a few revisions cases on weekly basis. More recently there have been a few “Rebanding” patients seeking revision to the Duodenal Switch.
The typical scenario is of a patient who had an adjustable gastric band placed, and after the initial weight loss (mostly because of the persistent nausea and vomiting) the weight stabilized. The weight loss was never close to a healthy weight and in most cases their co-morbidities did not resolve but now have added complications of reflux and abdominal pain developed. These patients were then recommended to have the band repositioned to resolve a slipped band causing the above complications.
The scientific evidence for rebranding is not justifiable. I think there continues to be an element of denial that the adjustable gastric banding procedures do not work for the vast majority of the people. In fact, AGB in the long term will result in some complications that may not be revisable. The scientific literature shows that there is no benefit to rebranding when it comes to weight loss.
In my opinion when a patient encounters problem with the adjustable gastric band, Duodenal Switch operation represent the best option because it has the best long term outcome of all weight loss surgical procedures.
GERD, Nausea and Vomiting- Don’t ignore it!
April 28, 2015 11:30 am
Gastroesophageal Reflux Disease is a serious matter and should not be left untreated. It is know as heartburn or reflux and if you are experiencing more than twice a week you should be evaluated by a physician to investigate the cause. Listed below are some of the causes and end results of not treating GERD.
Esophagitis – An irritant that can be acid, bile, food and digestive enzymes coming back up the esophagus can cause irritation and swelling in the esophagus. If left untreated, it can damage the lining of the esophagus to the point of erosion and scarring. Bile Reflux may also be a cause of esophagitis and Duodenogastroesphogeal reflux (DGER). Bile Reflux information here.
Esophageal Stricture – Scar tissue can cause the lumen of the esophagus to become smaller and narrow. This stricture makes it difficult or painful to swallow foods. If a stricture is narrow enough food may become stuck and require intervention for removal and treatment. This can also put a person at risk for choking. The treatment includes ballon dilation with an endoscope and in cases where it recurs surgery may be required.
Esophageal Ulceration– If GERD is left untreated it can progress to actual ulcerations in the esophagus. Patients may cough up or vomit blood or see it in their stool as dark tarry or coffee ground type stool.
Gastric Stricture– After weight loss surgery such as sleeve gastrectomy, RNY Gastric Bypass, Duodenal Switch, SADI/Loop, Adjustable Gastric Banding, or other gastric surgeries a narrowing of the inner opening of the stomach can result from scar tissue forming. This will require a surgical procedure to rectify. The symptoms can be food intolerance, full feeling, nausea and/or vomiting. (See pictures below)
Hiatal Hernia– An anatomical weakening or enlargement of the opening of the diaphragm muscle where the esophagus meets the stomach. This defect can allow a portion of the stomach to slide or roll into the chest cavity. This then causes reflux of gastric juice and content. Hiatal Hernia’s can also form on weight loss surgical patients. There are several examples within this blog here.
Breathing Difficulties– The acid aspiration while sleeping can make asthma and other breathing difficulties worst and can cause coughing and other issues.
Dental Issues – The acid, food, digestive enzymes backing up into the esophagus and mouth can cause dental issues such as erosion and tooth decay. In regards to dental issues after weight loss surgery there are also other vitamin and mineral deficiencies that can cause oral health issues. Dental Issues after WLS here.
Lower Quality of Life– GERD can affect a person’s quality of life. If you are in discomfort from acid reflux or having food intolerance it can make life difficult. It can also alter food choices and impact nutrition.
Barrets Esophagus– Pre-cancerous changes in the bottom portion of the esophagus due to long term acid exposure from gastric reflux. Diagnosis requires and endoscopic procedure (EGD) and biopsy.
Esophageal Cancer– There is a significant rise in the western world in esophageal adenocarcinoma. The main risk factors are alcohol use, smoking, untreated GERD, and poor diet.
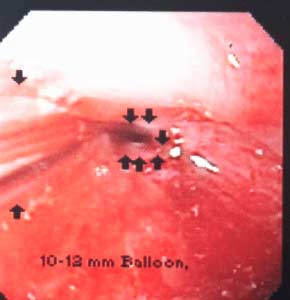
Reflux and difficulty with swallowing caused by stricture is not normal. These problems are quite frequently encountered as complication of Adjustable gastric banding, with slipped band or a band that is too tight and scarred in placed resulting is belt effect. This results in the esophagus not being able to empty and propel the food down. The end result is significant reflux, with difficulty swallowing, nausea, vomiting etc. Similar problems are seen with Gastric bypass where the anastomosis between the stomach pouch and the small bowel RNY limb is too narrow. In Gastric Sleeve and Duodenal Switch operations, is the sleeve is made too narrow, or misshaped (hour glass, funnel, cork screw) it will result in the patient having reflux and symptoms of stricture. One specific problem with the new operation of SADI is the concern for risk of bile reflux, similar to the BillRoth I procedure.
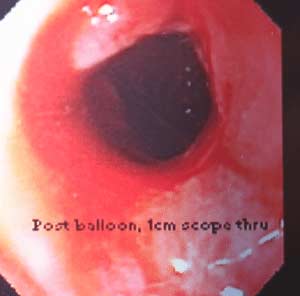
Gastric bypass patient with stricture at the gastro-jejunostomy before and after balloon dilation. Fig A
After balloon dilation. Fig B
Fig. C : Lap band Patient with stricture where the band as removed at another facility and the scar tissue formed around the GE junction was not taken down. The patient had to be taken back to the operation room after his symptoms persisted even though the band had been removed 3 months prior.
A corkscrew stomach of a Duodenal Switch done at another facility, with the patient presented with persistent reflux, nausea and vomiting for years after surgery. Fig. D
This is not an inclusive discussion of GERD and the treatment. Please see your healthcare providers if you are experiencing any symptoms pertaining to GERD or any other health care issue.