Category: AGB
Stricture with Lap Band
May 31, 2015 6:44 am
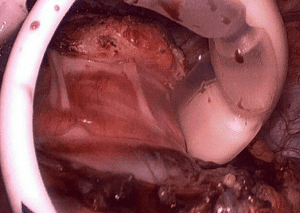
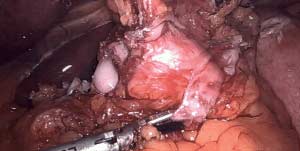
One of the most common findings with patients seeking revision of the Lap band is the persistent and continuos nausea, vomiting and reflux, even though the band is emptied. The typical presentation is that of a patient who had an adjustable gastric band placed and adjusted. When the weight loss stops any attempt to adjust and tighten the band results in reflux, nausea and vomiting. Unfortunately, there is lack of recognition that even when the band is completely empty, and even if removed, then a patient can still have the symptoms present, if the scar capsule that forms between the band and the tissue is not removed.
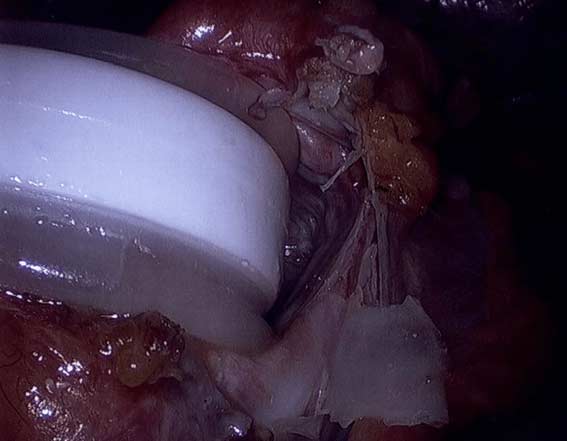
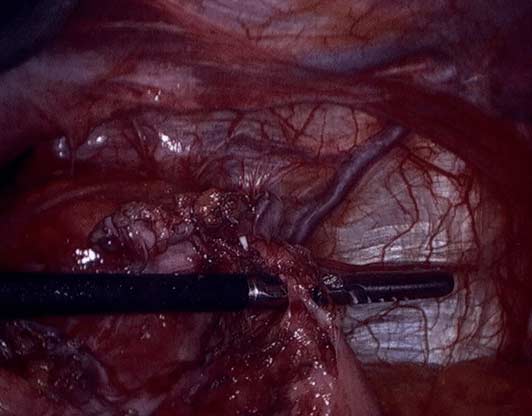
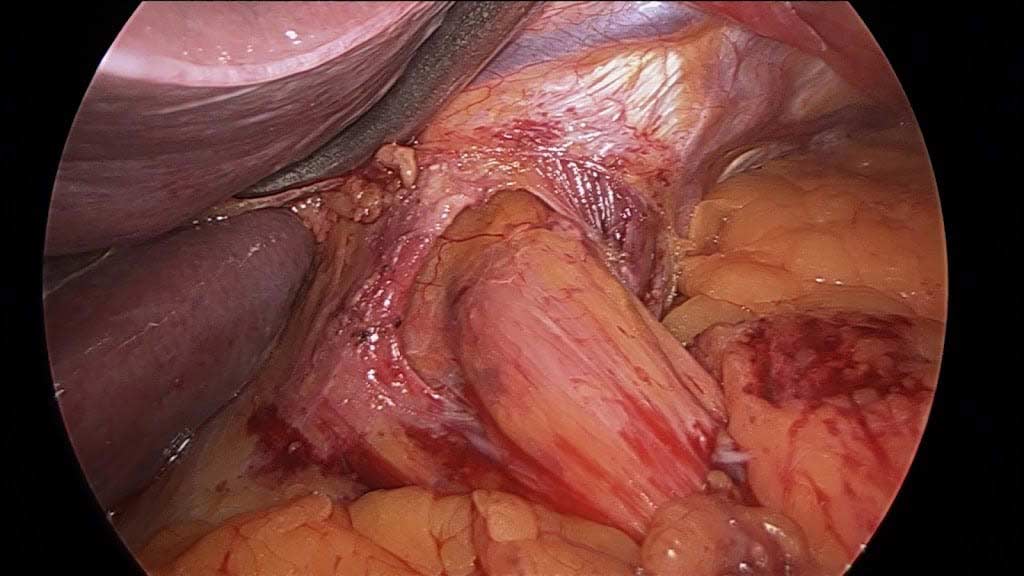
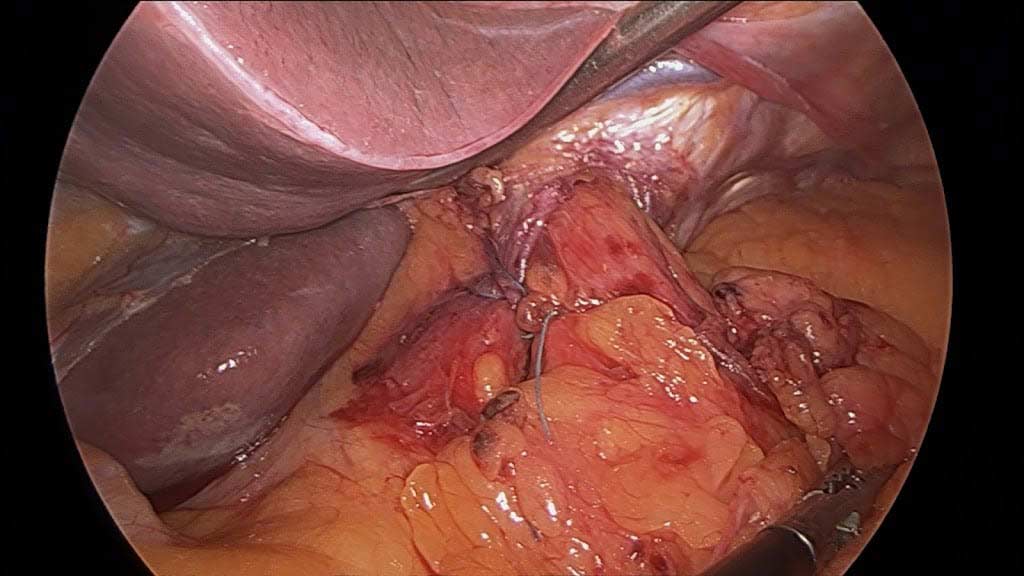
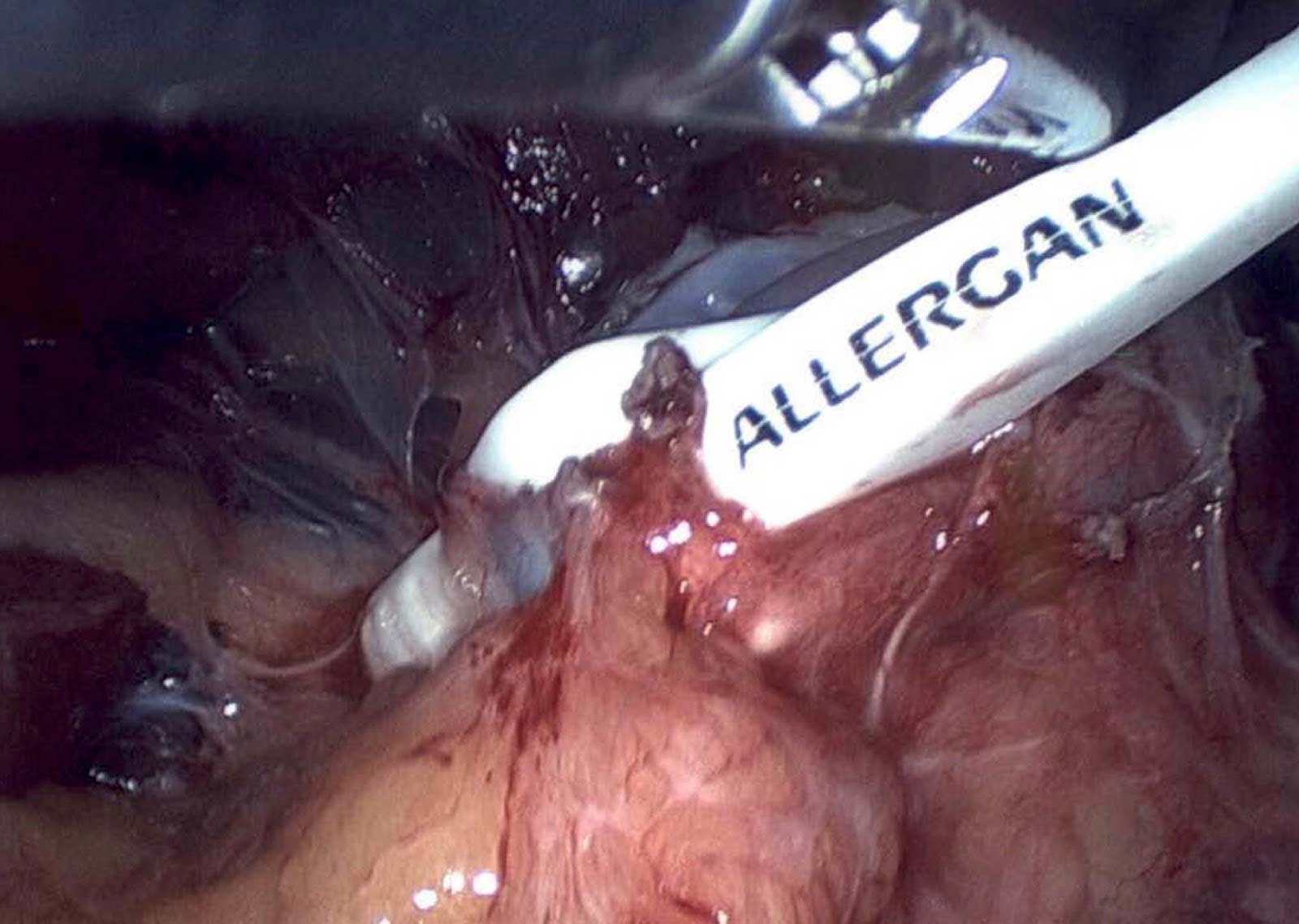
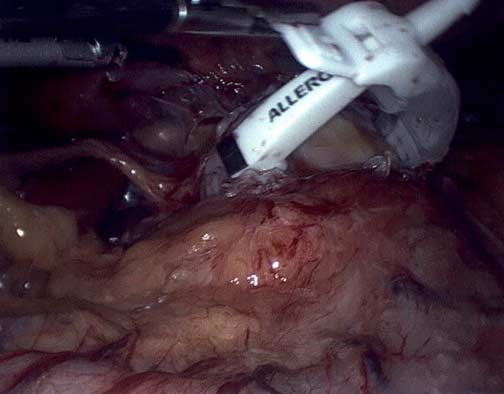
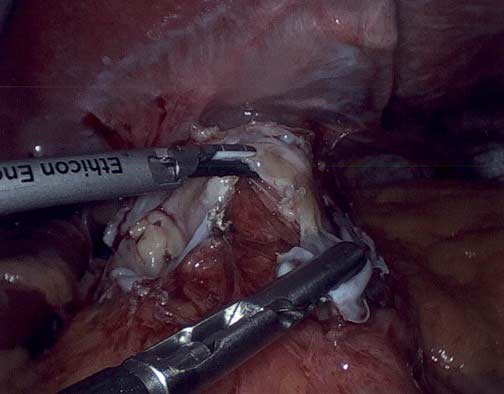
It is critical that when a Lap band is removed that time is spent excising the capsule that is present to allow for the tissue beneath the band to return to its normal caliber.
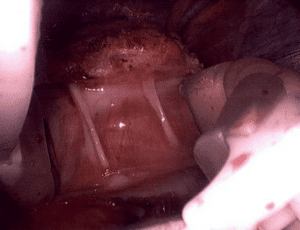
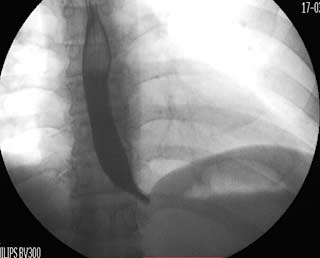
Note in these images how with the Lap band completely open the tissue underneath is “restricted” by the capsule that has formed under the band. In this case the capsule was also excised and removed along with the band.
Rebanding- A Bad Idea In My Opinion
May 12, 2015 3:42 pm
There is a wide discrepancy of outcomes for patients who have decided to have weight loss surgery and are experiencing different weight loss, regain and complications primary related to their choice of the procedure. In our practice we see quite a few revisions cases on weekly basis. More recently there have been a few “Rebanding” patients seeking revision to the Duodenal Switch.
The typical scenario is of a patient who had an adjustable gastric band placed, and after the initial weight loss (mostly because of the persistent nausea and vomiting) the weight stabilized. The weight loss was never close to a healthy weight and in most cases their co-morbidities did not resolve but now have added complications of reflux and abdominal pain developed. These patients were then recommended to have the band repositioned to resolve a slipped band causing the above complications.
The scientific evidence for rebranding is not justifiable. I think there continues to be an element of denial that the adjustable gastric banding procedures do not work for the vast majority of the people. In fact, AGB in the long term will result in some complications that may not be revisable. The scientific literature shows that there is no benefit to rebranding when it comes to weight loss.
In my opinion when a patient encounters problem with the adjustable gastric band, Duodenal Switch operation represent the best option because it has the best long term outcome of all weight loss surgical procedures.
GERD, Nausea and Vomiting- Don’t ignore it!
April 28, 2015 11:30 am
Gastroesophageal Reflux Disease is a serious matter and should not be left untreated. It is know as heartburn or reflux and if you are experiencing more than twice a week you should be evaluated by a physician to investigate the cause. Listed below are some of the causes and end results of not treating GERD.
Esophagitis – An irritant that can be acid, bile, food and digestive enzymes coming back up the esophagus can cause irritation and swelling in the esophagus. If left untreated, it can damage the lining of the esophagus to the point of erosion and scarring. Bile Reflux may also be a cause of esophagitis and Duodenogastroesphogeal reflux (DGER). Bile Reflux information here.
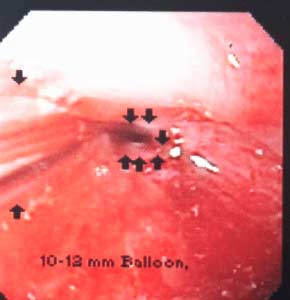
Esophageal Stricture – Scar tissue can cause the lumen of the esophagus to become smaller and narrow. This stricture makes it difficult or painful to swallow foods. If a stricture is narrow enough food may become stuck and require intervention for removal and treatment. This can also put a person at risk for choking. The treatment includes ballon dilation with an endoscope and in cases where it recurs surgery may be required.
Esophageal Ulceration– If GERD is left untreated it can progress to actual ulcerations in the esophagus. Patients may cough up or vomit blood or see it in their stool as dark tarry or coffee ground type stool.
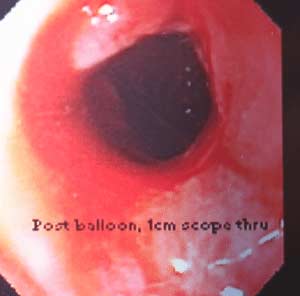
Gastric Stricture– After weight loss surgery such as sleeve gastrectomy, RNY Gastric Bypass, Duodenal Switch, SADI/Loop, Adjustable Gastric Banding, or other gastric surgeries a narrowing of the inner opening of the stomach can result from scar tissue forming. This will require a surgical procedure to rectify. The symptoms can be food intolerance, full feeling, nausea and/or vomiting. (See pictures below)
Hiatal Hernia– An anatomical weakening or enlargement of the opening of the diaphragm muscle where the esophagus meets the stomach. This defect can allow a portion of the stomach to slide or roll into the chest cavity. This then causes reflux of gastric juice and content. Hiatal Hernia’s can also form on weight loss surgical patients. There are several examples within this blog here.
Breathing Difficulties– The acid aspiration while sleeping can make asthma and other breathing difficulties worst and can cause coughing and other issues.
Dental Issues – The acid, food, digestive enzymes backing up into the esophagus and mouth can cause dental issues such as erosion and tooth decay. In regards to dental issues after weight loss surgery there are also other vitamin and mineral deficiencies that can cause oral health issues. Dental Issues after WLS here.
Lower Quality of Life– GERD can affect a person’s quality of life. If you are in discomfort from acid reflux or having food intolerance it can make life difficult. It can also alter food choices and impact nutrition.
Barrets Esophagus– Pre-cancerous changes in the bottom portion of the esophagus due to long term acid exposure from gastric reflux. Diagnosis requires and endoscopic procedure (EGD) and biopsy.
Esophageal Cancer– There is a significant rise in the western world in esophageal adenocarcinoma. The main risk factors are alcohol use, smoking, untreated GERD, and poor diet.
Reflux and difficulty with swallowing caused by stricture is not normal. These problems are quite frequently encountered as complication of Adjustable gastric banding, with slipped band or a band that is too tight and scarred in placed resulting is belt effect. This results in the esophagus not being able to empty and propel the food down. The end result is significant reflux, with difficulty swallowing, nausea, vomiting etc. Similar problems are seen with Gastric bypass where the anastomosis between the stomach pouch and the small bowel RNY limb is too narrow. In Gastric Sleeve and Duodenal Switch operations, is the sleeve is made too narrow, or misshaped (hour glass, funnel, cork screw) it will result in the patient having reflux and symptoms of stricture. One specific problem with the new operation of SADI is the concern for risk of bile reflux, similar to the BillRoth I procedure.
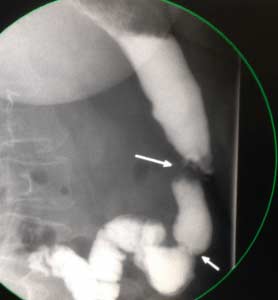
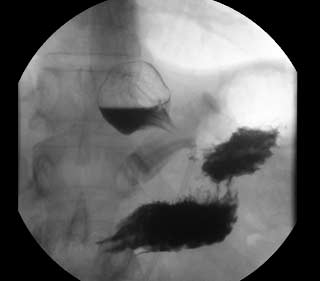
Gastric bypass patient with stricture at the gastro-jejunostomy before and after balloon dilation. Fig A
After balloon dilation. Fig B
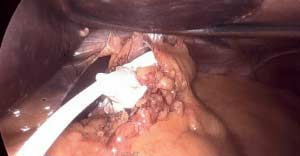
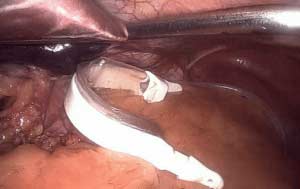
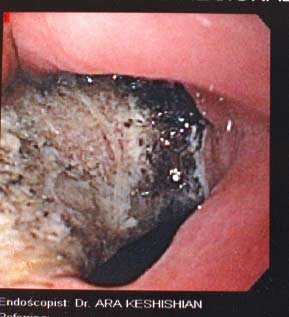
Fig. C : Lap band Patient with stricture where the band as removed at another facility and the scar tissue formed around the GE junction was not taken down. The patient had to be taken back to the operation room after his symptoms persisted even though the band had been removed 3 months prior.
A corkscrew stomach of a Duodenal Switch done at another facility, with the patient presented with persistent reflux, nausea and vomiting for years after surgery. Fig. D
This is not an inclusive discussion of GERD and the treatment. Please see your healthcare providers if you are experiencing any symptoms pertaining to GERD or any other health care issue.
Adjustable Gastric Band Removal & Hiatal Hernia Repair
April 21, 2015 6:30 pm
The band in place and after being taken down
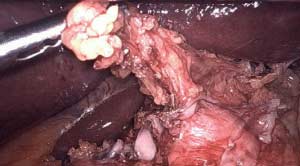
The dissection of the wrap over the band that shows erosion
Shared Success Story- Odessa D.
April 07, 2015 10:20 am
My name is Odessa D. I am going to talk about my weight loss journey with the lap band which started in 2006. At my heaviest I weighed 270 pounds and was a size 24 waist. I had high blood pressure, was a border line diabetic, had lower back pain, I had no energy, I was tired all the time, and I had sleep apnea.
My family doctor had suggested weight loss surgery but I was hesitant because I was afraid of surgery. Until one night my 8 year old daughter found me not breathing in my sleep. I made the decision to go through with the surgery.
Prior to surgery I did as much research as I could about the lap band. At the time I felt it was the right decision. On the day of the surgery everything went well. The first few months were great. I was losing weight, feeling good, feeling happy, and healthier then I have in years.
Then it began, all the symptoms of a slipped band. I started vomiting, nausea, acid reflux, and I was having trouble drinking and eating on a daily basis. My doctor confirmed it was a slipped band. We decided to replace the band because I was still overweight. On day of surgery I weighed 210 lbs.
After a month I started having symptoms of a slipped band. My doctor performed x-rays but everything looked fine. After 2 years with these symptoms and numerous doctor visits and x-rays I just gave up and learned to live with it. In 2 years I lost 4 lbs. My high blood pressure and sleep apnea came back. I finally decided to get the lap band removed. I wanted my life back and if that meant gaining the weight back that I lost then I was willing to make that sacrifice.
Dr. Keshishian was referred to me by 2 of his past patients. From the moment I walked into his office I was already at ease. When I first met Dr. Keshishian, I knew I was in good hands and I knew he could help me. He confirmed I had another slipped band and a detached port. At this point we discussed removing the lap band and switching to the Sleeve Gastrectomy. Finally everything was going to be fixed and everything was going to be right.
I can’t express how much my life has improved since removing the second band and switching to the sleeve. I have lost 46 pounds in 9 months. I now weigh 160 pounds and wear a size 8 waist. Now I look forward to each and every day with joy and pleasure knowing I don’t have to deal with a bad band and all the horrible symptoms that came with it.
Since the surgery and losing more weight I have been very active. I go hiking almost every weekend. I have literally climbed a mountain! I did my first 5k mud obstacle course in which my second 5k is in October. I even have a purple Mohawk! I have 100% confidence in myself and in everything that I do. My life has greatly improved since the sleeve. All thanks to Dr. Keshishian. It has been a very bumpy road with my weight loss journey but Dr. Keshishian has smoothed out the bumps and I plan on traveling the distance with many adventures along the way.
I would like to leave a huge “Thank You” to Dr. Keshishian and his staff. Thank you for making me feel welcomed, being friendly, making me feel comfortable, and especially for giving my life back to me. I can’t wait to see what the future holds for me and my family!
Thank you Dr. Keshishian and staff!
Odessa D.
Erosion of Adjustable Gastric Band
February 17, 2015 8:22 pm
Adjustable gastric band has been promoted as a minimally invasive procedure. The long term data has proven this not to be the case. One of the complications is erosion of Adjustable Gastric Band. The adjustable gastric band results in the least amount of weight loss, as well as the lowest rate of resolution of the co-morbidities of all weight loss surgical procedures. As for the minimally invasive claim of the AGB, one has to also consider all the adjustments, the radiation exposure related to the upper GI and X-rays, as well as the upper endoscopies that are necessary to maintain a band. I would argue that an average band is much more invasive when one accounts for the total number of procedure that are done on a band patient.
Other complications arise, when, not if, a band needs to be surgical revised or removed. Band removal requires an extensive amount of scar tissue dissection to expose the band before it can be removed. This is an example of a patient with erosion of the band.
Note the very thick scar tissue that is formed around the band (the white tissue on the left lower corner)
Hiatal Hernia Repair- Reflux and Adjustable Gastric Band Revision
January 14, 2015 3:47 pm
Hiatal Hernia is an anatomical weakening or enlargement of the opening in the diaphragm where the esophagus meets the stomach. The defect can allow a section of stomach to slide or roll into the chest cavity. This causes the reflux of stomach content back to the esophagus. Esophageal Reflux may also be occur without the presences of a Hiatal hernia. It is reported that approximately 60% of people over 50 have a Hiatal hernia with about 9% being symptomatic.
However, over the years we have also noticed a significant increase in reflux disease in patients who have had adjustable gastric band placed. Quite frequently the reflux symptoms after the band is ” blamed” on the patient’s eating habit. Most of the time all studies are reported as “normal” and the complaints are discounted. Other symptoms of Hiatal hernia may or may not include shortness of breath, heart palpitations, or a feeling of food being stuck.
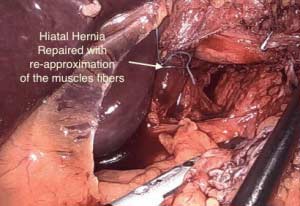
It is important to confirm the presence or absence of a hiatal hernia when considering revision from an adjustable gastric band procedure. Any hiatal hernia identified either before surgery or at the time of the operation will need to be repaired surgically.
With a hiatal hernia repair, the opening is made smaller, and the esophagus, stomach and the junction between them is returned to the proper location to minimize-eliminate reflux.
Erosion of Gastric Band
November 30, 2014 5:03 pm
Gastric bands are restrictive rings placed around the top part of the stomach, close to the junction of the esophagus. Their mechanism of action is to create a small tight band to restrict the flow of the food into the stomach. The theory has been that the band will decrease the time food travels down past the narrowing thereby eating less with the end result of weight loss. One of the many complications from the band is erosion of the band into the lumen of the stomach. This results in the patient presenting with nausea, vomiting and some patients develop abdominal accesses. This may present itself with symptoms of abdominal pain, fever, and redness at the port site under the skin.
The treatment for this is urgent removal of the band and repair of the erosion/ulceration. Patients who are contemplating a revision to another weight loss surgical procedure are best advised to stage the procedure because of the potential for leak from the repair site. Almost all of these procedures can be done laparoscopically.
Adjustable Gastric Band Easily Reversible?
November 24, 2014 3:25 pm
The Adjustable Gastric Band (AGB) procedures have been advertised as “easily reversible” minimally invasive procedures. A point of interest is why doesn’t anyone ask the question, “Why would a successful device and/or procedure need to be revised or removed?”
The long term success data shows that the AGB procedure is the most inferior of all bariatric procedures. It is important, that when looking at the published data, special attention is given to the definitions in that particular study. An example would be that if a study defines “successful outcomes as weight loss for 30 days!” then all procedure will be successful.
The following is an example of a patient who had the Lap Band (R) a several years ago in another institution. She was seen for surgical follow up with minimal weight loss over a short period of time. She then developed the typical complications of the band, namely the upper abdominal pain, reflux, inability to swallow solids, persistent nausea and vomiting. Her symptoms were all “worked up” and was told that all the studies were normal. All of her symptoms were contributed to her eating habits, even though they persisted after the Lap Band (R) was completely empty.
The patient then presented n our office for a second opinion. After being seen in our office and having a full work up, she had the Lap Band removed and was revised to a Laparoscopic Sleeve Gastrectomy. She had complete resolution of all of her prior presenting symptoms.
“Normal” Lap Band placement!
April 23, 2013 9:39 pm
One of the most common problems that we see are patients who have been told that their band is in correct placement, and yet they are still having nausea, vomiting, reflux etc. These patients are frequently blamed for their symptoms as if properly placed band completely eliminates the problems being associated with the band.