Category: Weight Loss Surgery
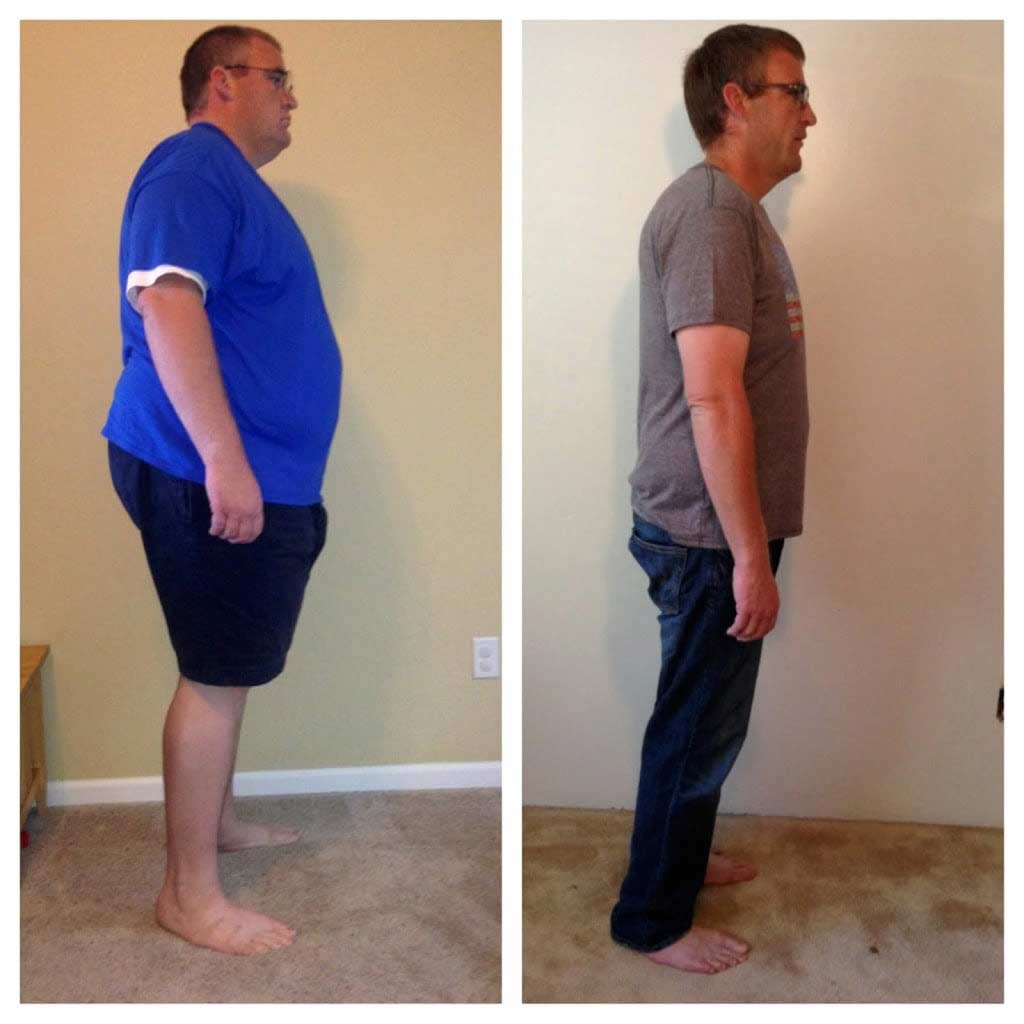
Shared Success Story- Brad P.
January 29, 2015 9:53 pm
Congratulations Brad on all your success and weight loss! You have accomplished a remarkable transformation!
2015 Back on Track or A New Start after Weight Loss SurgeryExclusive Member Content
January 08, 2015 8:37 pm
Hernia Repair And Weight loss surgery
December 22, 2014 3:35 pm
Patients having weight loss surgery (WLS) either primary or revision are sometimes also diagnosed with having a hernia. Whether a hernia can be repaired concurrently with WLS or not, depends on the type of the hernia and also type of weight loss surgery.
The 2 most common hernias encountered in weight loss surgical patient’s are 1.Ventral (incisional), or 2. Hiatal hernias. Ventral hernia refers to defects or weaknesses of the abdominal wall. If this involves a previous midline incision then an incisional hernia is diagnosed. These hernias may present with any or all of the following findings; protrusions or bulging of the anterior abdominal wall tissue through the abdominal muscle cavity, abdominal pain, and nausea and/or vomiting.
Hiatal hernias are located inside the abdominal cavity at the junction of the esophagus and the stomach at the level of the diaphragm. This condition is where the upper portion of the stomach this is usually located in the abdominal cavity has migrated through the esophageal hiatus into the chest cavity. These hernia’s usually present with reflux, episodes of nausea and are quite frequently seen in patients with experienced complications of the LAP-BAND.
The surgical treatment of these hernias are very different:
Ventral hernia repairs may require mesh placement. There are different mesh products that are available. Some are made with non absorbable material and other are absorbable- biologic material that last long enough to allow incorporation by the patients own tissue. In general, when a mesh is used, the incidence of hernia recurrence goes down significantly. However, there is an increase in complications associated with the use of mesh. These may include infection of the mesh, indications of synthetic material, and serum and rejection indications of non synthetic material. To add another layer of complexity, when the hernia is encountered at the time of weight loss surgery, especially when the GI track has to be opened ( in the case of duodenal switch, revision from a failed gastric bypass with a duodenal switch) then it is recommended that no mesh be placed because of the high incidence of mesh infection or the associated complications. In extreme cases where the abdominal wall cannot be closed, biologic meshes may be used with the understanding that a repeat hernia repair may be required at a later date.
In my practice, Hiatal hernias are always repaired at the time of the weight loss surgical procedures. Depending on the type of the weight loss surgery the patient has had previously, the type of the hernia repair, and whether or not a mesh needs to be utilized, and the amount of stomach and fundus remains for the repair, will dictate how the Hiatal hernia is repaired.
Additional information regarding hernias in a newsletter.
Holiday Survival Tips by: Marylin Calzadilla, Psy.D.
November 17, 2014 8:23 pm
REFLECT
SUPPORT, SUPPORT, SUPPORT
ALLOWANCES
KEEP ACTIVE
CREATE
PLAN ACTIVITES
Marylin Calzadilla, Psy.D
Laboratory Blood Specimen Collection Change
October 30, 2014 5:20 pm

No one likes surprises at the lab when you are about to get your blood drawn. The picture above is of the older vacutainers blood specimen tubes and a new type of tube that is being introduced. There is currently a change over of blood specimen tubes in laboratories across the country. Locally we are seeing the use of SARSTEDT tubes/syringes. This change over is for several reasons. First and foremost is to reduce blood bourne pathogen exposure due to needle sticks and tube breakage. However, these blood specimen tubes offer some additional benefits, especially to people who frequently have lab draws. One of which is the ability to use aspiration of the specimen to decrease the incidence of hemolysis. Hemolysis skews laboratory studies and damages the red blood cells in the collected specimen causing the need for repeated testing. Aspiration is also easier on fragile veins due to the decrease pressure versus vacuum. The SARSTEDT tubes are versatile in that they can also be used as a vacuum tube if needed.
Weight Loss before Weight Loss Surgery?
October 19, 2014 2:54 pm
I am frequently confronted by the question “Are you going to make me lose weight before I have weight loss surgery”? My answer is no, for several reasons, it makes little or no sense and there is scant scientific data to support it.
1-Anatomical and 2-psychological-behavior related variables have been suggested as the reasoning for the recommendations for diet before weight loss surgery.
Let’s see what the scientific evidence says about this.
1-Liver can be divided into two anatomical lobes. The tail end of the left lobe may extend all the way to the upper left side of the abdomen covering the upper 1/3 of the stomach, the gastro-esophageal junction (GEJ) and the esophageal hiatus. It was suggested that the access to the GEJ could be made easier, if the left lobe of the liver was smaller.
“A decrease in the size of the liver by 18% was shown in patients who were subjected to a very low-energy diet for 12- weeks.” This was published by Colles et.al in a small study of 39 subjects.
It is important to appreciate that this reduction in liver size meant that a patient would have to tolerate an ultra low caloric diet (less than 500/day) for 12 weeks. The interesting observation was that even with this reduction in the size of the liver there was “… no difference shown in morbidity, mortality, hospital stay, and decrease in morbidity- associated diseases whether there is preoperative weight loss or not.”
2-Behavior modifications have been entertained as a necessary element to the success of adjustable gastric banding. Numerous studies have shown that there is no predictive value of preoperative weight loss in relation to the weight loss after surgery.
The overwhelming scientific data suggest that there is no value to subjecting a weight loss surgical patient to a pre-surgical ultra low caloric diet.
“The California Department of Managed Health Care recently conducted a review of weight loss prior to bariatric surgery and concluded that “there is no literature presented by any authority that mandated weight loss, once a patient has been identified as a candidate for bariatric surgery, is indicated. This comprehensive review states that mandated weight loss prior to indicated bariatric surgery is without evidence-based support, is not medically necessary, and that the risks of delaying bariatric surgery are real and measurable.” Published by the American Society for Metabolic and Bariatric Surgery in March 2011.
Telogen Effluvium: Hair Loss After WLS (Weight Loss Surgery)
September 14, 2014 12:56 pm
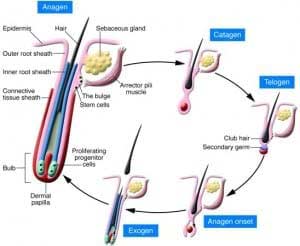
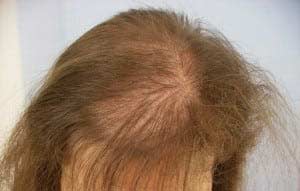
Telogen Effluvium is the premature pushing of the hair root into a resting state and can be chronic or acute. It is usually brought on by a shock to your body such as high fevers, childbirth, severe infections, severe chronic illness, severe psychological stress, major surgery or illnesses, over or under active thyroid gland, crash diets with inadequate protein, and a variety of medications. Most hair loss from medications, is this type of hair loss, and the related medications include retinoids, beta blockers, calcium channel blockers, antidepressants, and NSAIDS (including ibuprofen). Supplements that can also cause or increase telogen effluvium are higher doses of iron and Vitamin A.
The hair begins to fall out in differing amounts and can start weeks to months after the initial shock to the body or medication initiation. The hair loss can continue up to 6 weeks and typically slows at 8 weeks after the start of the hair loss.
Weight loss surgical patients experience this due to the stress of surgery and the low protein state directly after surgery. Although there is no specific treatment for Telogen Effluvium, there are steps that can be taken to potentially slow the hair loss and help support the new hair growth.
The most important steps to take are to maintain your protein supplementation at a minimum of 80-100 grams of protein daily and hydration (at least 64 ounces daily) after weight loss surgery.
Protein, particularly L-lysine, are the building blocks of hair and nails, without adequate protein your body will forgo making hair and nails to maintain critical muscle mass. Also hydration is important to flush the body of toxins, due to fat breakdown in the liver during the rapid weight loss phase, that will prevent further new hair growth.
Vitamin B6 and B12 deficits can also contribute to hair loss. Multivitamin supplementation is essential to maintaining the required levels of these vitamins. The recommended multivitamin supplementation is two multivitamins daily that are equivalent to Centrum brand multivitamin.
Some people add Zinc supplements to increase hair production. However, if you are adding Zinc it is advised to also add a Copper supplement as they compete with each other for absorption. Copper is important for red blood cell production and a copper deficiency can exacerbate iron deficiency anemia. Inactivity can also decrease zinc levels, therefore exercise/activity will naturally maintain zinc levels.
Biotin is also a B vitamin that can be helpful in new hair growth.
Folicure is a supplement tablet that contains many vitamins and minerals that some people find helpful for hair re-growth. They also manufacture a shampoo that can be used.
There are many shampoos and topical treatments that people use and report satisfaction in their results. However, it is important to note that a topical treatment may make your hair appear thicker but the hair regrowth will only be supported by internal nutritional maintenance. Minoxidil is a liquid vasodilator medication applied to the scalp that is the exception to this rule and can help with hair regrowth. However, Minoxidil will not work to it’s optimal level in the absence of adequate nutritional status.
We always go back to our basics after weight loss surgery of hydration, protein and exercise to maintain health of body and hair.
Orthostatic Hypotension/Intolerance
August 26, 2014 4:02 pm
One of the possible side effects of rapid weight loss after undergoing weight loss surgery is orthostatic hypotension or orthostatic intolerance. These terms describe a significant drop in blood pressure upon standing from a seated or reclined position. Drip in blood pressure causes a decrease in blood flow to the brain. There are several studies discussing this after RNY gastric bypass and sleeve gastrectomy. However, this can also be an issue post Duodenal Switch. The process is still not completely understood but can be due to several factors. Rapid weight loss, sympathetic nervous system dysfunction, dehydration, electrolyte imbalance, malnutrition, thyroid issues, cardiac issues, post prandial hypotension (blood pressure lowering after meals due to blood flow shifting to the gut) or medications are all suspected as possible causefor orthostatic hypotension.
Symptoms can include dizziness, lightheadedness, nausea, blurry vision, weakness, fatigue, palpitations, headache, exercise intolerance, intermittent confusion and can culminate to passing out. This can be diagnoses with blood pressure monitoring while positioning change, ECG, laboratory studies, echocardiogram, tilt table test and possibly Valsalva maneuver.
There is a direct link between obesity and hypertension. A large number of patients undergoing weight loss surgery are on anti-hypertension medications. Patients need to be followed closely in the hospital and in the rapid weight loss phase post surgery for medication changes and eventually termination of anti-hypertensive medications. Follow up and monitoring with a primary care physician is crucial due to these rapid changes.
Dehydration, anemia, and low protein intake need close surveillance after weight loss surgery. The patient may require laboratory studies to investigate these causes.
Treatments may include increasing hydration, protein intake, changing medications and treating anemia. Also, allowing time for the body to adjust to the rapid weight loss if all the underlying issues are within normal limits. If symptoms persist, after all underlying issues are investigated, the patient will need to be diligent with hydration, protein intake, supplements and other treatments. Things that may also help is to slow down in moving from one position to the other, take a moment to adjust to your new position. Compression stocking and increasing salt intake can also help if all other causes are investigated. Post prandial hypotension can be avoided with low carbohydrate and small meals. Also, moderately increasing salt intake can improve symptoms.
Vitamin D Metabolism, Deficiency and Treatment
August 23, 2014 4:17 am
Vitamin D and Weight Loss Surgery
Probiotics, C. diff & Enteric HyperoxaluriaExclusive Member Content
July 26, 2014 3:21 pm