Tag: Crohn’s Disease
Crohn’s Disease and Ulcerative Colitis
June 07, 2016 6:33 am
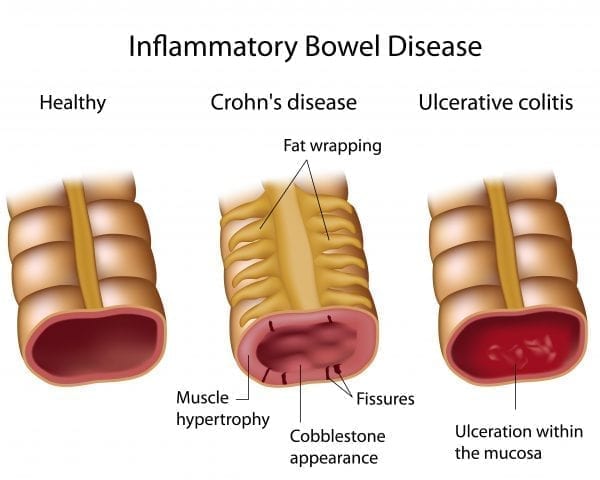
Crohn’s Disease and Ulcerative Colitis are two disease processes that effect the large intestine to varying degrees and in the case of Crohn’s possibly part of the small intestines. Both fall under the category of Inflammatory Bowel Disease however there are differences between Crohn’s Disease and Ulcerative Colitis even though they may share some symptomatology.
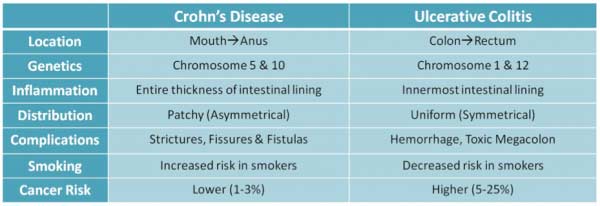
Crohn’s Disease (CD) is an inflammatory bowel disease (IBD) that causes deep tissue inflammation of the digestive lining tract. It affects the gastrointestinal (GI) tract, extending from the mouth to the rectum. CD has an asymmetrical progression, where it does not affect the entire tract uniformly (1). It is commonly found at the end of the small bowel (ileum) to the start of the large bowel (colon).
Complex interactions between three factors contribute to the occurrence of CD:
- Immune Response: Foreign environmental substances may elicit an overactive immune response. T-cell mediated immune response identifies threatening affluences and works to protect the body. This stimulates inflammation, often times without control, in the body as the body’s natural defense mechanism (2,3).
- Inherited Genes: Variation in genes that produce proteins involved in immune function may disrupt intestinal cell’s ability to respond normally to bacteria. Studies also show genetic deviation in chromosomes 5 and 10, which contain IBD loci. Alterations at this locus may lead to the increased risk of CD.
- Environmental Factors: Factors such as smoking, those between the ages of 10-40 yrs. (commonly diagnosed before 30 yrs.), diets high in sugar/sweeteners, fats/oils, and total fat may lead to the increased risk of developing CD.
Common symptoms of CD include frequent diarrhea, rectal bleeding, fatigue, fever, weight loss, reduced appetite, abdominal pain/cramps, and fever. Inflammation in CD is unevenly widespread throughout the GI tract. Inflammation in the mouth, esophagus, and stomach can lead to ulcers. However, they are rather uncommon. Inflammation in the small intestine, colon, and rectum may lead to ulcers as the severity increases (5). The complications in CD are due to chronic inflammation, which may lead to:
- Intestinal narrowing (stricture)
- Abscess: collection of pus
- Fistula: abnormal connection or tract
- Colon Cancer
- Other disorders such as anemia, osteoporosis, gallbladder/liver disease, etc.
Antibiotics, anti-inflammatories, corticosteroids, and immunomodulators have been proven to regulate the mechanisms of CD. Surgical treatment may also benefit the patient. There are several surgical options that may be performed depending on the symptoms and findings.
- Strictureplasty
- Resection
- Proctocolectomy or Colectomy
There is no known cure for Crohn’s Disease; however these treatment options may control it.
Ulcerative Colitis (UC) is an inflammatory bowel disease (IBD), which results in damaging inflammation of the colon and rectum. It effects 700,000 men and women in the United States. As opposed to Crohn’s Disease, UC spreads evenly throughout the colon and rectum only (9). It does not affect the entire GI tract.
Like CD, Ulcerative Colitis occurs through a complex interaction of three factors:
- Immune Response: T cells (lymphocyte) mature and function in identifying foreign substances to then defend the body against infection.
- Inherited Genes: Variation in genes that protect intestinal function are more likely to respond abnormally to bacteria. Studies show genetic deviation in chromosomes 1 and 12 (11).
- Environmental Factors: Factors such as those between the ages of 1-30 yrs. or exposure to isotrentinoin (vitamin A derivative) may be at risk for UC.
Common symptoms of UC include bloody diarrhea, abdominal pain, weight loss, reduced appetite, fatigue, and fever. Inflammation in UC is evenly spread, yet restricted between the colon and rectum (10). Inflammation in the right (ascending), transverse, left (descending), sigmoid colons, and rectum can lead to ulcers that vary in size and depth (red, bloody, swollen). The complications of UC are due to prolonged inflammation, which can lead to:
- Increased risk of blood clots
- Colon Cancer
- Other disorders such as osteoporosis, liver disease, etc.
Antibiotics, anti-inflammatories, corticosteroids, and immunomodulators have been proven to normalize the mechanisms of UC. There is no cure for Ulcerative Colitis, but these treatment options may help regulate it.
It is important to have a coordinated team of medical professionals to develop an ongoing and dynamic treatment plan as well as surveillance for side effects of CD and UC. Patients can lead a productive life regardless of the challenges of CD and UC with appropriate medical treatment.
References
- Westall, F. C. (2006). Integrating theories of the etiology of Crohn’s disease on the etiology of Crohn’s disease: questioning the hypotheses. William M. Chamberlin, Saleh A. Naser Med Sci Monit, 2006; 12 (2): RA27-33. Medical Science Monitor, 12(5), LE5-LE6.
- Folwaczny, C., Glas, J., & Török, H. P. (2003). Crohn’s disease: an immunodeficiency?. European journal of gastroenterology & hepatology, 15(6), 621-626.
- Braat, H., Peppelenbosch, M. P., & Hommes, D. W. (2006). Immunology of Crohn’s disease. Annals of the New York Academy of Sciences, 1072(1), 135-154.
- Canavan, C., Abrams, K. R., Hawthorne, B., Drossman, D., & Mayberry, J. F. (2006). Long‐term prognosis in Crohn’s disease: factors that affect quality of life. Alimentary pharmacology & therapeutics, 23(3), 377-385.
- Talbot, R. W., Heppell, J., Dozois, R. R., & Beart, R. W. (1986, February). Vascular complications of inflammatory bowel disease. In Mayo Clinic Proceedings (Vol. 61, No. 2, pp. 140-145). Elsevier.
- Eaden, J. A., Abrams, K. R., & Mayberry, J. F. (2001). The risk of colorectal cancer in ulcerative colitis: a meta-analysis. Gut, 48(4), 526-535.
- Colitis–Pathophysiology, U. (2003). Inflammatory bowel disease part I: ulcerative colitis–pathophysiology and conventional and alternative treatment options. Alternative medicine review, 8(3), 247-283.
- Greenstein, A. J., Janowitz, H. D., & Sachar, D. B. (1976). The extra-intestinal complications of Crohn’s disease and ulcerative colitis: a study of 700 patients. Medicine, 55(5), 401-412.
- Lennard-Jones, J. E. (1989). Classification of inflammatory bowel disease. Scandinavian Journal of Gastroenterology, 24(sup170), 2-6.
- Gillen, C. D., Walmsley, R. S., Prior, P., Andrews, H. A., & Allan, R. N. (1994). Ulcerative colitis and Crohn’s disease: a comparison of the colorectal cancer risk in extensive colitis. Gut, 35(11), 1590-1592.
- Silverberg, M. S., Cho, J. H., Rioux, J. D., McGovern, D. P., Wu, J., Annese, V., … & Barmada, M. M. (2009). Ulcerative colitis–risk loci on chromosomes 1p36 and 12q15 found by genome-wide association study. Nature genetics, 41(2), 216-220.