The re-shaping of the stomach for weight loss with a Sleeve Gastrectomy can be a technically challenging procedure. There are complications such as stricture, cork-screw stomach, GERD, nausea and vomiting that can lead to further health issues and possibly nutritional issues.
Upper GI pictures of Sleeved Stomach
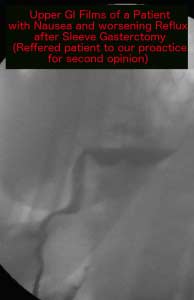
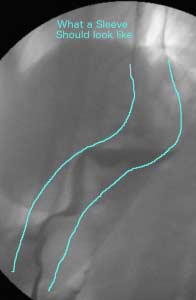
In the following series of pictures you can visualize that the Sleeve Gastrectomy in the first picture is a hard angled S shape with two stricture points. The second picture points out the two stricture points and the outline the sleeve gastrectomy of a patient referred to our practice for complications of stricture and GERD post sleeve gastrectomy in need of revision. Surgical revision of gastric stricture is highly technical and challenging. It also takes experience in identifying possible options available to the patient.
The outline in light blue depicts the shape a sleeve gastrectomy should follow.
Why are strictures bad? What is the problem with having and living with a stricture? Strictures caused by Sleeve gastrectomy or Duodenal Switch, SIPS/SADI procedure can have detrimental effects. The long-term complications may include, irreversible injury to the esophagus and the stomach above the stricture, Teeth and gum damage, aspiration in addition to nutritional deficits because of the inability to tolerate healthy meals. Additional information regarding complications that can arise from stricture, nausea and vomiting here.
Strictures can not be repaired by dilation in most cases since on one side of the narrowed section is formed by the sample line. These should be addressed surgical by an experienced surgeon. Ideally a a stricture would be avoided at all cost by assuring that the sleeves are not done too tight and narrowed and that there are no sharp angles created when the stomach is divided during these procedures. The repair of these strictures of the stomach in the duodenal switch, sleeve and the SADI/SIPS procedures are complicated since the remnant stomach is removed and the options are limited. Additional information regarding stricture complications and pictures of other stricture types here.


My wife is currently suffering from a stricture resulting from a gastric sleeve procedure done about 7 years ago. Apparently, the problem was there for quite awhile but was fully exposed after a successful hiatal hernia surgery in August, according to the surgeon. The bariatric surgeon argues that her current problem didn’t come on until after the hernia repair so the problem lies there. After the back-and-forth, the bottom line is scar tissue from the sleeve surgery is the cause of the stricture which gives her nausea, pain and vomiting.
Here’s the timeline:
August: Hiatal hernia surgery. 3 weeks later complaints of abdominal pain, nausea, vomiting.
September: Stricture discovered by endoscopy.
Dilation of stricture. Improvement for 2 weeks before symptoms returned. Repeat dilation of stricture. Improvement for about 1 week before symptoms returned with daily visits to the ER for pain, nausea and vomiting.
November: stents placed at site of stricture to help in allowing food to pass. It did not help. In fact, there was rejection of any clear liquids and increased pain, nausea and vomiting foam/dry heaves. Started TPN feed thru picc line. Stents removed after 3 weeks of stent-related pain, nausea and vomiting. After removal, the stents acted like dilators as her appetite returned. Diet improved from clear to full liquids to soft foods, small amounts. This lasted for about 3 weeks before symptoms returned.
December: referred to bariatric specialist. He has dilated her twice already with the same results but this time the symptoms returned in just a few days. His plan is to do a bypass after the holidays. He said the surgery would be relatively ‘easy’ due to the location of the stricture. I’ve read a little about stricturoplasty which seems like a simpler procedure. What is your opinion on these procedures? Given my wife’s situation what would you recommend? I’m asking because her bariatric doctor is currently unavailable until after the holidays.
Hello
I can not make any recommendations. MY decision needs to be made based not he films, endoscopy results etc. In general however there are a lot of alternatives such as stricturoplasty before a conversion to and RNY which has a whole lot of other problems associated with it.
Ara