One of the potential complications of any abdominal surgery is bowel obstruction. This can occur with open or laparoscopic operation. It can also occur within days or years of the operation. The over all incidence of bowel obstruction is relatively low.
The text book diagnostic criteria for bowel obstruction is the presence of a set of physical findings additional to the diagnostic supporting evidence. A typical patient may present with cramping abdominal pain, nausea, vomiting, absence of any flatus, and not bowel movements. The pain may be dull and could be any where on the abdomen. The White count may be elevated, and a plain abdominal Xray may show “airfluid” levels. All of these finding point to a patient that has bowel obstruction. Depending on the age and the history of the patient, the a common cause may he adhesions (scar tissue) that has cause a blockage of the bowel.
Unfortunately, these physical and radiological findings may not all be present in patients that have had the Duodenal Switch or the Gastric Bypass operation. The patients may complain of nausea but no vomiting. They may still pass gas and have bowel movements, but have cramping abdominal pain. The plain abdominal xray may not show air-fluid levels, yet have complete obstruction. The presence or lack of these findings can be explained.
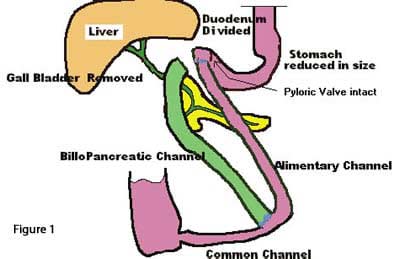
In both the DS and the RNY operations, there are two parallel limbs (figure 1). One of them is connected to the esophagus, thus it can have air in it. The other limb is not connected to the outside on the proximal end (green limb in figure one only drain the bilio-pancreatic secretions and is not connected on the proximal end to the esophagus). This major anatomical difference explains why there may be air fluid level in a bowel obstruction patient with no DS or RNY, and no such finding in a DS or RNY patient.
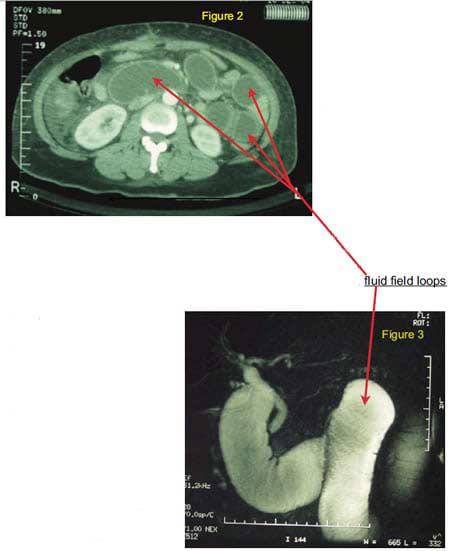
The most important diagnostic tool is a very high degree of clinical suspicion. The absence of vomiting, or air fluid levels on an abdominal xray, or the presence of flatus and bowel movements does NOT rule out a complete bowel obstruction. The more reliable way to diagnose a bowel obstruction after DS or RNY is by CT scan or and MRI (figure 2, 3).
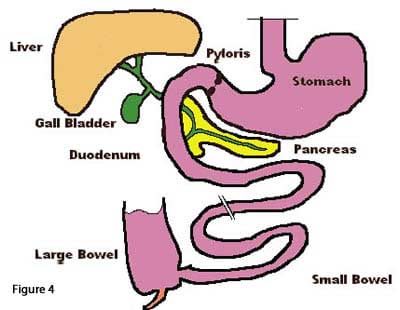
A finding of fluid field loops of bowel is highly specific for bowel obstruction and warrants a surgical intervention since it can not be corrected by a naso-gastric tube (tube inserted thru the nose into the stomach to decompress the stomach and the proximal small bowel). This is because as mentioned earlier, there is a parallel segment of bowel that is not in continuum with the esophagus. In pre DS or RNY anatomy, the entire GI track is a long tube (figure 4).
An example of a bowel obstruction caused by scar tissue is noted in the following pictures.

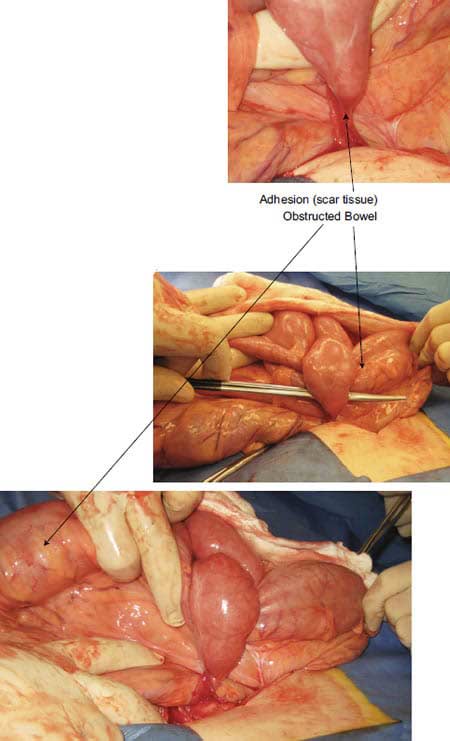
I had stomach surgery at 3 weeks old in the 60’s I had esophagus and herni surgery a year after surgery had pain and noticed a shape like a round ball in my lower stomach I feel pretty good now is there anything I can do moving forward.